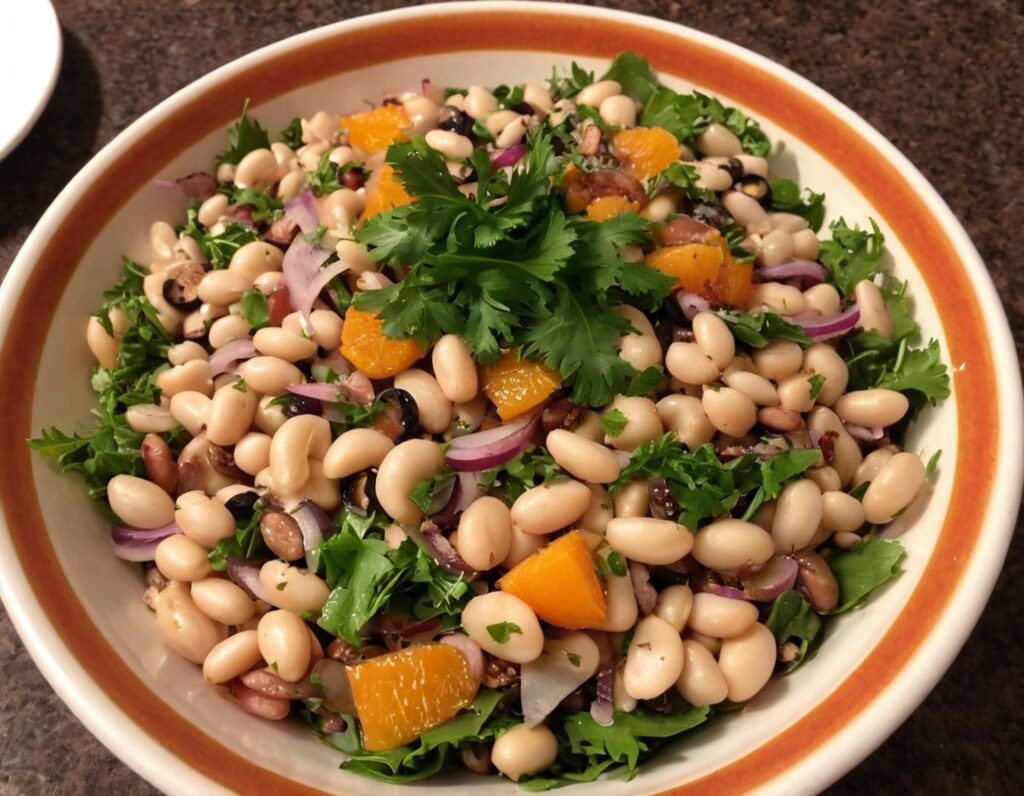As the U.S. Struggles With a Stillbirth Crisis, Australia Offers a Model for How to Do Better
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
ProPublica is a Pulitzer Prize-winning investigative newsroom. Sign up for The Big Story newsletter to receive stories like this one in your inbox.
Series: Stillbirths:When Babies Die Before Taking Their First Breath
The U.S. has not prioritized stillbirth prevention, and American parents are losing babies even as other countries make larger strides to reduce deaths late in pregnancy.
The stillbirth of her daughter in 1999 cleaved Kristina Keneally’s life into a before and an after. It later became a catalyst for transforming how an entire country approaches stillbirths.
In a world where preventing stillbirths is typically far down the list of health care priorities, Australia — where Keneally was elected as a senator — has emerged as a global leader in the effort to lower the number of babies that die before taking their first breaths. Stillbirth prevention is embedded in the nation’s health care system, supported by its doctors, midwives and nurses, and touted by its politicians.
In 2017, funding from the Australian government established a groundbreaking center for research into stillbirths. The next year, its Senate established a committee on stillbirth research and education. By 2020, the country had adopted a national stillbirth plan, which combines the efforts of health care providers and researchers, bereaved families and advocacy groups, and lawmakers and government officials, all in the name of reducing stillbirths and supporting families. As part of that plan, researchers and advocates teamed up to launch a public awareness campaign. All told, the government has invested more than $40 million.
Meanwhile, the United States, which has a far larger population, has no national stillbirth plan, no public awareness campaign and no government-funded stillbirth research center. Indeed, the U.S. has long lagged behind Australia and other wealthy countries in a crucial measure: how fast the stillbirth rate drops each year.
According to the latest UNICEF report, the U.S. was worse than 151 countries in reducing its stillbirth rate between 2000 and 2021, cutting it by just 0.9%. That figure lands the U.S. in the company of South Sudan in Africa and doing slightly better than Turkmenistan in central Asia. During that period, Australia’s reduction rate was more than double that.
Definitions of stillbirth vary by country, and though both Australia and the U.S. mark stillbirths as the death of a fetus at 20 weeks or more of pregnancy, to fairly compare countries globally, international standards call for the use of the World Health Organization definition that defines stillbirth as a loss after 28 weeks. That puts the U.S. stillbirth rate in 2021 at 2.7 per 1,000 total births, compared with 2.4 in Australia the same year.
Every year in the United States, more than 20,000 pregnancies end in a stillbirth. Each day, roughly 60 babies are stillborn. Australia experiences six stillbirths a day.
Over the past two years, ProPublica has revealed systemic failures at the federal and local levels, including not prioritizing research, awareness and data collection, conducting too few autopsies after stillbirths and doing little to combat stark racial disparities. And while efforts are starting to surface in the U.S. — including two stillbirth-prevention bills that are pending in Congress — they lack the scope and urgency seen in Australia.
“If you ask which parts of the work in Australia can be done in or should be done in the U.S., the answer is all of it,” said Susannah Hopkins Leisher, a stillbirth parent, epidemiologist and assistant professor in the stillbirth research program at the University of Utah Health. “There’s no physical reason why we cannot do exactly what Australia has done.”
Australia’s goal, which has been complicated by the pandemic, is to, by 2025, reduce the country’s rate of stillbirths after 28 weeks by 20% from its 2020 rate. The national plan laid out the target, and it is up to each jurisdiction to determine how to implement it based on their local needs.
The most significant development came in 2019, when the Stillbirth Centre of Research Excellence — the headquarters for Australia’s stillbirth-prevention efforts — launched the core of its strategy, a checklist of five evidence-based priorities known as the Safer Baby Bundle. They include supporting pregnant patients to stop smoking; regular monitoring for signs that the fetus is not growing as expected, which is known as fetal growth restriction; explaining the importance of acting quickly if fetal movement changes or decreases; advising pregnant patients to go to sleep on their side after 28 weeks; and encouraging patients to talk to their doctors about when to deliver because in some cases that may be before their due date.
Officials estimate that at least half of all births in the country are covered by maternity services that have adopted the bundle, which focuses on preventing stillbirths after 28 weeks.
“These are babies whose lives you would expect to save because they would survive if they were born alive,” said Dr. David Ellwood, a professor of obstetrics and gynecology at Griffith University, director of maternal-fetal medicine at Gold Coast University Hospital and a co-director of the Stillbirth Centre of Research Excellence.
Australia wasn’t always a leader in stillbirth prevention.
In 2000, when the stillbirth rate in the U.S. was 3.3 per 1,000 total births, Australia’s was 3.7. A group of doctors, midwives and parents recognized the need to do more and began working on improving their data classification and collection to better understand the problem areas. By 2014, Australia published its first in-depth national report on stillbirth. Two years later, the medical journal The Lancet published the second report in a landmark series on stillbirths, and Australian researchers applied for the first grant from the government to create the stillbirth research center.
But full federal buy-in remained elusive.
As parent advocates, researchers, doctors and midwives worked to gain national support, they didn’t yet know they would find a champion in Keneally.
Keneally’s improbable journey began when she was born in Nevada to an American father and Australian mother. She grew up in Ohio, graduating from the University of Dayton before meeting the man who would become her husband and moving to Australia.
When she learned that her daughter, who she named Caroline, would be stillborn, she remembers thinking, “I’m smart. I’m educated. How did I let this happen? And why did nobody tell me this was a possible outcome?”
A few years later, in 2003, Keneally decided to enter politics. She was elected to the lower house of state parliament in New South Wales, of which Sydney is the capital. In Australia, newly elected members are expected to give a “first speech.” She was able to get through just one sentence about Caroline before starting to tear up.
As a legislator, Keneally didn’t think of tackling stillbirth as part of her job. There wasn’t any public discourse about preventing stillbirths or supporting families who’d had one. When Caroline was born still, all Keneally got was a book titled “When a Baby Dies.”
In 2009, Keneally became New South Wales’ first woman premier, a role similar to that of an American governor. Another woman who had suffered her own stillbirth and was starting a stillbirth foundation learned of Keneally’s experience. She wrote to Keneally and asked the premier to be the foundation’s patron.
What’s the point of being the first female premier, Keneally thought, if I can’t support this group?
Like the U.S., Australia had previously launched an awareness campaign that contributed to a staggering reduction in sudden infant death syndrome, or SIDS. But there was no similar push for stillbirths.
“If we can figure out ways to reduce SIDS,” Keneally said, “surely it’s not beyond us to figure out ways to reduce stillbirth.”
She lost her seat after two years and took a break from politics, only to return six years later. In 2018, she was selected to serve as a senator at Australia’s federal level.
Keneally saw this as her second chance to fight for stillbirth prevention. In the short period between her election and her inaugural speech, she had put everything in place for a Senate inquiry into stillbirth.
In her address, Keneally declared stillbirth a national public health crisis. This time, she spoke at length about Caroline.
“When it comes to stillbirth prevention,” she said, “there are things that we know that we’re not telling parents, and there are things we don’t know, but we could, if we changed how we collected data and how we funded research.”
The day of her speech, March 27, 2018, she and her fellow senators established the Select Committee on Stillbirth Research and Education.
Things moved quickly over the next nine months. Keneally and other lawmakers traveled the country holding hearings, listening to testimony from grieving parents and writing up their findings in a report released that December.
“The culture of silence around stillbirth means that parents and families who experience it are less likely to be prepared to deal with the personal, social and financial consequences,” the report said. “This failure to regard stillbirth as a public health issue also has significant consequences for the level of funding available for research and education, and for public awareness of the social and economic costs to the community as a whole.”
It would be easy to swap the U.S. for Australia in many places throughout the report. Women of Aboriginal and Torres Strait Islander backgrounds experienced double the rate of stillbirth of other Australian women; Black women in America are more than twice as likely as white women to have a stillbirth. Both countries faced a lack of coordinated research and corresponding funding, low autopsy rates following a stillbirth and poor public awareness of the problem.
The day after the report’s release, the Australian government announced that it would develop a national plan and pledged $7.2 million in funding for prevention. Nearly half was to go to education and awareness programs for women and their health care providers.
In the following months, government officials rolled out the Safer Baby Bundle and pledged another $26 million to support parents’ mental health after a loss.
Many in Australia see Keneally’s first speech as senator, in 2018, as the turning point for the country’s fight for stillbirth prevention. Her words forced the federal government to acknowledge the stillbirth crisis and launch the national action plan with bipartisan support.
Australia’s assistant minister for health and aged care, Ged Kearney, cited Keneally’s speech in an email to ProPublica where she noted that Australia has become a world leader in stillbirth awareness, prevention and supporting families after a loss.
“Kristina highlighted the power of women telling their story for positive change,” Kearney said, adding, “As a Labor Senator Kristina Keneally bravely shared her deeply personal story of her daughter Caroline who was stillborn in 1999. Like so many mothers, she helped pave the way for creating a more compassionate and inclusive society.”
Keneally, who is now CEO of Sydney Children’s Hospitals Foundation, said the number of stillbirths a day in Australia spurred the movement for change.
“Six babies a day,” Keneally said. “Once you hear that fact, you can’t unhear it.”
Australia’s leading stillbirth experts watched closely as the country moved closer to a unified effort. This was the moment for which they had been waiting.
“We had all the information needed, but that’s really what made it happen.” said Vicki Flenady, a perinatal epidemiologist, co-director of the Stillbirth Centre of Research Excellence based at the Mater Research Institute at the University of Queensland, and a lead author on The Lancet’s stillbirth series. “I don’t think there’s a person who could dispute that.”
Flenady and her co-director Ellwood had spent more than two decades focused on stillbirths. After establishing the center in 2017, they were now able to expand their team. As part of their work with the International Stillbirth Alliance, they reached out to other countries with a track record of innovation and evidence-based research: the United Kingdom, the Netherlands, Ireland. They modeled the Safer Baby Bundle after a similar one in the U.K., though they added some elements.
In 2019, the state of Victoria, home to Melbourne, was the first to implement the Safer Baby Bundle. But 10 months into the program, the effort had to be paused for several months because of the pandemic, which forced other states to cancel their launches altogether.
“COVID was a major disruption. We stopped and started,” Flenady said.
Still, between 2019 and 2021, participating hospitals across Victoria were able to reduce their stillbirth rate by 21%. That improvement has yet to be seen at the national level.
A number of areas are still working on implementing the bundle. Westmead Hospital, one of Australia’s largest hospitals, planned to wrap that phase up last month. Like many hospitals, Westmead prominently displays the bundle’s key messages in the colorful posters and flyers hanging in patient rooms and in the hallways. They include easy-to-understand slogans such as, “Big or small. Your baby’s growth matters,” and, “Sleep on your side when baby’s inside.”
As patients at Westmead wait for their names to be called, a TV in the waiting room plays a video on stillbirth prevention, highlighting the importance of fetal movement. If a patient is concerned their baby’s movements have slowed down, they are instructed to come in to be seen within two hours. The patient’s chart gets a colorful sticker with a 16-point checklist of stillbirth risk factors.
Susan Heath, a senior clinical midwife at Westmead, came up with the idea for the stickers. Her office is tucked inside the hospital’s maternity wing, down a maze of hallways. As she makes the familiar walk to her desk, with her faded hospital badge bouncing against her navy blue scrubs, it’s clear she is a woman on a mission. The bundle gives doctors and midwives structure and uniform guidance, she said, and takes stillbirth out of the shadows. She reminds her staff of how making the practices a routine part of their job has the power to change their patients’ lives.
“You’re trying,” she said, “to help them prevent having the worst day of their life.”
Christine Andrews, a senior researcher at the Stillbirth Centre who is leading an evaluation of the program’s effectiveness, said the national stillbirth rate beyond 28 weeks has continued to slowly improve.
“It is going to take a while until we see the stillbirth rate across the whole entire country go down,” Andrews said. “We are anticipating that we’re going to start to see a shift in that rate soon.”
As officials wait to receive and standardize the data from hospitals and states, they are encouraged by a number of indicators.
For example, several states are reporting increases in the detection of babies that aren’t growing as they should, a major factor in many late-gestation stillbirths. Many also have seen an increase in the number of pregnant patients who stopped smoking. Health care providers also are more consistently offering post-stillbirth investigations, such as autopsies.
In addition to the Safer Baby Bundle, the national plan also calls for raising awareness and reducing racial disparities. The improvements it recommends for bereavement care are already gaining global attention.
To fulfill those directives, Australia has launched a “Still Six Lives” public awareness campaign, has implemented a national stillbirth clinical care standard and has spent two years developing a culturally inclusive version of the Safer Baby Bundle for First Nations, migrant and refugee communities. Those resources, which were recently released, incorporated cultural traditions and used terms like Stronger Bubba Born for the bundle and “sorry business babies,” which is how some Aboriginal and Torres Strait Islander women refer to stillbirth. There are also audio versions for those who can’t or prefer not to read the information.
In May, nearly 50 people from the state of Queensland met in a large hotel conference room. Midwives, doctors and nurses sat at round tables with government officials, hospital administrators and maternal and infant health advocates. Some even wore their bright blue Safer Baby T-shirts.
One by one, they discussed their experiences implementing the Safer Baby Bundle. One midwifery group was able to get more than a third of its patients to stop smoking between their first visit and giving birth.
Officials from a hospital in one of the fastest-growing areas in the state discussed how they carefully monitored for fetal growth restriction.
And staff from another hospital, which serves many low-income and immigrant patients, described how 97% of pregnant patients who said their baby’s movements had decreased were seen for additional monitoring within two hours of voicing their concern.
As the midwives, nurses and doctors ticked off the progress they were seeing, they also discussed the fear of unintended consequences: higher rates of premature births or increased admissions to neonatal intensive care units. But neither, they said, has materialized.
“The bundle isn’t causing any harm and may be improving other outcomes, like reducing early-term birth,” Flenady said. “I think it really shows a lot of positive impact.”
As far behind as the U.S. is in prioritizing stillbirth prevention, there is still hope.
Dr. Bob Silver, who co-authored a study that estimated that nearly 1 in 4 stillbirths are potentially preventable, has looked to the international community as a model. Now, he and Leisher — the University of Utah epidemiologist and stillbirth parent — are working to create one of the first stillbirth research and prevention centers in the U.S. in partnership with stillbirth leaders from Australia and other countries. They hope to launch next year.
“There’s no question that Australia has done a better job than we have,” said Silver, who is also chair of the University of Utah Health obstetrics and gynecology department. “Part of it is just highlighting it and paying attention to it.”
It’s hard to know what parts of Australia’s strategy are making a difference — the bundle as a whole, just certain elements of it, the increased stillbirth awareness across the country, or some combination of those things. Not every component has been proven to decrease stillbirth.
The lack of U.S. research on the issue has made some cautious to adopt the bundle, Silver said, but it is clear the U.S. can and should do more.
There comes a point when an issue is so critical, Silver said, that people have to do the best they can with the information that they have. The U.S. has done that with other problems, such as maternal mortality, he said, though many of the tactics used to combat that problem have not been proven scientifically.
“But we’ve decided this problem is so bad, we’re going to try the things that we think are most likely to be helpful,” Silver said.
After more than 30 years of working on stillbirth prevention, Silver said the U.S. may be at a turning point. Parents’ voices are getting louder and starting to reach lawmakers. More doctors are affirming that stillbirths are not inevitable. And pressure is mounting on federal institutions to do more.
Of the two stillbirth prevention bills in Congress, one already sailed through the Senate. The second bill, the Stillbirth Health Improvement and Education for Autumn Act, includes features that also appeared in Australia’s plan, such as improving data, increasing awareness and providing support for autopsies.
And after many years, the National Institutes of Health has turned its focus back to stillbirths. In March, it released a report with a series of recommendations to reduce the nation’s stillbirth rate that mirror ProPublica’s reporting about some of the causes of the crisis. Since then, it has launched additional groups to begin to tackle three critical angles: prevention, data and bereavement. Silver co-chairs the prevention group.
In November, more than 100 doctors, parents and advocates gathered for a symposium in New York City to discuss everything from improving bereavement care in the U.S to tackling racial disparities in stillbirth. In 2022, after taking a page out of the U.K.’s book, the city’s Mount Sinai Hospital opened the first Rainbow Clinic in the U.S., which employs specific protocols to care for people who have had a stillbirth.
But given the financial resources in the U.S. and the academic capacity at American universities and research institutions, Leisher and others said federal and state governments aren’t doing nearly enough.
“The U.S. is not pulling its weight in relation either to our burden or to the resources that we have at our disposal,” she said. “We’ve got a lot of babies dying, and we’ve got a really bad imbalance of who those babies are as well. And yet we look at a country with a much smaller number of stillbirths who is leading the world.”
“We can do more. Much more. We’re just not,” she added. “It’s unacceptable.”
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
21 Most Beneficial Polyphenols & What Foods Have Them
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We often write about polyphenols here at 10almonds; sometimes mentioning that a certain food is good because it has them, or else occasionally an entire article about a particular polyphenol. But what about a birds-eye view of polyphenols as a whole?
Well, there are many, but we’ve picked 21 particularly beneficial for human health, and what foods contain them.
We’ll be working from this fantastic database, by the way:
❝Phenol-Explorer is the first comprehensive database on polyphenol content in foods. The database contains more than 35,000 content values for 500 different polyphenols in over 400 foods. These data are derived from the systematic collection of more than 60,000 original content values found in more than 1,300 scientific publications. Each of these publications has been critically evaluated before inclusion in the database. The whole data on the polyphenol composition of foods is available for download.❞
Source: Phenol-Explorer.EU | Database on polyphenol content in foods
We use this database at least several times per week while writing 10almonds; it’s a truly invaluable resource!
However, 500 is a lot, so here’s a rundown of 21 especially impactful ones; we’ve sorted them per the categories used in the explorer, and in some cases we’ve aggregated several very similar polyphenols typically found together in the same foods, into one item (so for example we just list “quercetin” instead of quercetin 3-O-rutinoside + quercetin 4′-O-glucoside + quercetin 3,4′-O-diglucoside, etc etc). We’ve also broadly grouped some particularly populous ones such as “anthocyanins”, “catechins”, and so forth.
Without further ado, here’s what you ideally want to be getting plenty of in your diet:
Flavonoids
- Quercetin
- Foods: onions, apples, berries, kale, broccoli, capers.
- Benefits: anti-inflammatory, reduces allergy symptoms, supports heart and brain health, and may lower blood pressure.
- See also: Fight Inflammation & Protect Your Brain, With Quercetin
- Kaempferol
- Foods: spinach, kale, tea (green and black), capers, brussels sprouts.
- Benefits: antioxidant, may reduce the risk of cancer, supports cardiovascular health, and has anti-inflammatory properties.
- Epigallocatechin gallate (EGCG)
- Foods: green tea, matcha.
- Benefits: potent antioxidant, promotes weight loss, supports brain health, and may reduce the risk of heart disease.
- Anthocyanins
- Foods: blueberries, blackberries, raspberries, red cabbage, cherries.
- Benefits: improve brain health, support eye health, and reduce the risk of cardiovascular diseases.
- Apigenin
- Foods: parsley, celery, chamomile tea.
- Benefits: anti-inflammatory, reduces anxiety, and supports brain and immune system health.
- Luteolin
- Foods: peppers, thyme, celery, carrots.
- Benefits: anti-inflammatory, supports brain health, and may help reduce the growth of cancer cells.
- Catechins (aside from EGCG)
- Foods: green tea, dark chocolate, apples
- Benefits: boosts metabolism, supports cardiovascular health, and reduces oxidative stress.
- Hesperidin
- Foods: oranges, lemons, limes, grapefruits.
- Benefits: supports vascular health, reduces inflammation, and may help manage diabetes.
- Naringenin
- Foods: oranges, grapefruits, tomatoes.
- Benefits: antioxidant, supports liver health, and may improve cholesterol levels.
For more on epigallocatechin gallate and other catechins, see: Which Tea Is Best, By Science?
Phenolic Acids
- Chlorogenic acid
- Foods: coffee, artichokes, apples, pears.
- Benefits: supports weight management, improves blood sugar regulation, and reduces inflammation.
- See also: Green Coffee Bean Extract: Coffee Benefits Without The Coffee?
- Caffeic acid
- Foods: coffee, thyme, sage, basil.
- Benefits: antioxidant, anti-inflammatory, and supports skin health.
- See also: The Bitter Truth About Coffee (or is it?)
- Ferulic acid
- Foods: whole grains, rice bran, oats, flaxseeds, spinach.
- Benefits: protects skin from UV damage, reduces inflammation, and supports cardiovascular health.
- Gallic acid
- Foods: green tea, berries, walnuts.
- Benefits: antioxidant, may reduce the risk of cancer, and supports brain health.
Stilbenes
- Resveratrol
- Foods: red currants, blueberries, peanuts.
- Benefits: anti-aging properties, supports heart health, and reduces inflammation.
- See also: Resveratrol & Healthy Aging ← and no, you can’t usefully get it from red wine; here’s why!
Lignans
- Secoisolariciresinol
- Foods: flaxseeds, sesame seeds, whole grains.
- Benefits: supports hormone balance, reduces the risk of hormone-related cancers, and promotes gut health.
- Matairesinol
- Foods: rye, oats, barley, sesame seeds.
- Benefits: hormonal support, antioxidant, and may reduce the risk of cardiovascular diseases.
See also: Sprout Your Seeds, Grains, Beans, Etc ← for maximum nutritional availability!
Tannins
- Ellagic acid
- Foods: pomegranates, raspberries, walnuts.
- Benefits: anti-cancer properties, supports skin health, and reduces inflammation.
- Proanthocyanidins
- Foods: cranberries, apples, grapes, dark chocolate.
- Benefits: supports urinary tract health, reduces inflammation, and improves blood vessel health.
See also: Enjoy Bitter Foods For Your Heart & Brain
Curcuminoids
- Curcumin
- Foods: turmeric.
- Benefits: potent anti-inflammatory, supports joint health, and may reduce the risk of chronic diseases.
- See also: Why Curcumin (Turmeric) Is Worth Its Weight In Gold
Isoflavones
- Genistein
- Foods: soybeans, chickpeas.
- Benefits: supports bone health, reduces the risk of hormone-related cancers, and promotes heart health.
- Daidzein
- Foods: soybeans, legumes.
- Benefits: hormonal balance, supports bone health, and may help alleviate menopausal symptoms.
See also: What Does “Balance Your Hormones” Even Mean?
Well, that’s a lot of things to remember!
If you want to make it easier for yourself, you can simply make sure to get at least 30 different kinds of plant into your diet per week, and by doing so, statistically, you should cover most of these!
Read more: What’s Your Plant Diversity Score?
Alternatively, for a middle-ground approach of targetting 16 most polyphenol delivering foods, check out this super-dense arrangement:
Mediterranean Diet… In A Pill? ← it’s about plant extracts from 16 specific foods, and the polyphenols they deliver
Enjoy!
Share This Post
- Quercetin
-
We looked at genetic clues to depression in more than 14,000 people. What we found may surprise you
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The core experiences of depression – changes in energy, activity, thinking and mood – have been described for more than 10,000 years. The word “depression” has been used for about 350 years.
Given this long history, it may surprise you that experts don’t agree about what depression is, how to define it or what causes it.
But many experts do agree that depression is not one thing. It’s a large family of illnesses with different causes and mechanisms. This makes choosing the best treatment for each person challenging.
Reactive vs endogenous depression
One strategy is to search for sub-types of depression and see whether they might do better with different kinds of treatments. One example is contrasting “reactive” depression with “endogenous” depression.
Reactive depression (also thought of as social or psychological depression) is presented as being triggered by exposure to stressful life events. These might be being assaulted or losing a loved one – an understandable reaction to an outside trigger.
Endogenous depression (also thought of as biological or genetic depression) is proposed to be caused by something inside, such as genes or brain chemistry.
Many people working clinically in mental health accept this sub-typing. You might have read about this online.
But we think this approach is way too simple.
While stressful life events and genes may, individually, contribute to causing depression, they also interact to increase the risk of someone developing depression. And evidence shows that there is a genetic component to being exposed to stressors. Some genes affect things such as personality. Some affect how we interact with our environments.
What we did and what we found
Our team set out to look at the role of genes and stressors to see if classifying depression as reactive or endogenous was valid.
In the Australian Genetics of Depression Study, people with depression answered surveys about exposure to stressful life events. We analysed DNA from their saliva samples to calculate their genetic risk for mental disorders.
Our question was simple. Does genetic risk for depression, bipolar disorder, schizophrenia, ADHD, anxiety and neuroticism (a personality trait) influence people’s reported exposure to stressful life events?
We looked at the genetic risk of mental illness to see how that was linked to stressful life events, such as childhood abuse and neglect. Kamira/Shutterstock You may be wondering why we bothered calculating the genetic risk for mental disorders in people who already have depression. Every person has genetic variants linked to mental disorders. Some people have more, some less. Even people who already have depression might have a low genetic risk for it. These people may have developed their particular depression from some other constellation of causes.
We looked at the genetic risk of conditions other than depression for a couple of reasons. First, genetic variants linked to depression overlap with those linked to other mental disorders. Second, two people with depression may have completely different genetic variants. So we wanted to cast a wide net to look at a wider spectrum of genetic variants linked to mental disorders.
If reactive and endogenous depression sub-types are valid, we’d expect people with a lower genetic component to their depression (the reactive group) would report more stressful life events. And we’d expect those with a higher genetic component (the endogenous group) would report fewer stressful life events.
But after studying more than 14,000 people with depression we found the opposite.
We found people at higher genetic risk for depression, anxiety, ADHD or schizophrenia say they’ve been exposed to more stressors.
Assault with a weapon, sexual assault, accidents, legal and financial troubles, and childhood abuse and neglect, were all more common in people with a higher genetic risk of depression, anxiety, ADHD or schizophrenia.
These associations were not strongly influenced by people’s age, sex or relationships with family. We didn’t look at other factors that may influence these associations, such as socioeconomic status. We also relied on people’s memory of past events, which may not be accurate.
How do genes play a role?
Genetic risk for mental disorders changes people’s sensitivity to the environment.
Imagine two people, one with a high genetic risk for depression, one with a low risk. They both lose their jobs. The genetically vulnerable person experiences the job loss as a threat to their self-worth and social status. There is a sense of shame and despair. They can’t bring themselves to look for another job for fear of losing it too. For the other, the job loss feels less about them and more about the company. These two people internalise the event differently and remember it differently.
Genetic risk for mental disorders also might make it more likely people find themselves in environments where bad things happen. For example, a higher genetic risk for depression might affect self-worth, making people more likely to get into dysfunctional relationships which then go badly.
If two people lose their jobs, one with a high genetic risk of depression the other at low risk, both will experience and remember the event differently. Inside Creative House/Shutterstock What does our study mean for depression?
First, it confirms genes and environments are not independent. Genes influence the environments we end up in, and what then happens. Genes also influence how we react to those events.
Second, our study doesn’t support a distinction between reactive and endogenous depression. Genes and environments have a complex interplay. Most cases of depression are a mix of genetics, biology and stressors.
Third, people with depression who appear to have a stronger genetic component to their depression report their lives are punctuated by more serious stressors.
So clinically, people with higher genetic vulnerability might benefit from learning specific techniques to manage their stress. This might help some people reduce their chance of developing depression in the first place. It might also help some people with depression reduce their ongoing exposure to stressors.
If this article has raised issues for you, or if you’re concerned about someone you know, call Lifeline on 13 11 14.
Jacob Crouse, Research Fellow in Youth Mental Health, Brain and Mind Centre, University of Sydney and Ian Hickie, Co-Director, Health and Policy, Brain and Mind Centre, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Beyond “Make Your Bed”—life lessons from experience
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Beyond “Make Your Bed”—life lessons from experience
This is Admiral William H. McRaven, a former United States Navy four-star admiral who served as the ninth commander of the United States Special Operations Command.
So, for those of us whose day-to-day lives don’t involve coordinating military operations, what does he have to offer?
Quick note: 10almonds’ mission statement is “to make health and productivity crazy simple”.
We tend to focus on the health side of this, and in the category of productivity, it’s often what most benefits our mental health.
We’re writing less for career-driven technopreneurs in the 25–35 age bracket and more for people with a more holistic view of productivity and “a good life well-lived”.
So today’s main feature is more in that vein!
Start each day with an accomplishment
McRaven famously gave a speech (and wrote a book) that began with the advice, “make your bed”. The idea here doesn’t have to be literal (if you’ll pardon the pun). Indeed, if you’re partnered, then depending on schedules and habits, it could be you can’t (sensibly) make your bed first thing because your partner is still in it. But! What you can do is start the day with an accomplishment—however small. A short exercise routine is a great example!
Success in life requires teamwork
We’re none of us an island (except in the bathtub). The point is… Nobody can do everything alone. Self-sufficiency is an illusion. You can make your own coffee, but could you have made the coffee machine, or even the cup? How about, grown the coffee? Transported it? So don’t be afraid to reach out for (and acknowledge!) help from others. Teamwork really does make the dream work.
It’s what’s inside that counts
It’s a common trap to fall into, getting caught up the outside appearance of success, rather than what actually matters the most. We need to remember this when it comes to our own choices, as well as assessing what others might bring to the table!
A setback is only permanent if you let it be
No, a positive attitude won’t reverse a lifelong degenerative illness, for example. But what we can do, is take life as comes, and press on with the reality, rather than getting caught up in the “should be”.
Use failure to your advantage
Learn. That’s all. Learn, and improve.
Be daring in life
To borrow from another military force, the SAS has the motto “Who dares, wins”. Caution has it place, but if we’ve made reasonable preparations*, sometimes being bold is the best (or only!) way forward.
*Meanwhile the Parachute Regiment, from which come 80% of all SAS soldiers, has the motto “Utrinque paratus”, “prepared on all sides”.
Keep courage close
This is about not backing down when we know what’s right and we know what we need to do. Life can be scary! But if we don’t overcome our fears, they can become self-realizing.
Writer’s note: a good example of this is an advice I sometimes gave during my much more exciting (military) life of some decades ago, and it pertains to getting into a knife-fight (top advice for civilians: don’t).
But, if you’re in one, you need to not be afraid of getting cut.
Because if you’re not afraid of getting cut, you will probably get cut.
But if you are afraid of getting cut, you will definitely get cut.
Hopefully your life doesn’t involve knives outside of the kitchen (mine doesn’t, these days, and I like it), but the lesson applies to other things too.
Sometimes the only way out is through.
Be your best at your worst
Sometimes life is really, really hard. But if we allow those moments to drive us forwards, they’re also a place we can find more strength than we ever knew we had.
Keep on swimming
It’s said that the majority in life is about showing up—and often it is. But you have to keep showing up, day after day. So make what you’re doing sustainable for you, and keep on keeping on.
Share This Post
Related Posts
-
Mung Beans vs Black Beans – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing mung beans to black beans, we picked the black beans.
Why?
Both are great! But…
In terms of macros, black beans have more protein, carbs, and fiber, as well as the lower glycemic index (although both are already low). So, a clear win for black beans here.
In the category of vitamins, mung beans have more of vitamins A, B5, B9, and C, while black beans have more of vitamins B1, B6, E, K, and choline. Thus, a slight win for black beans this time.
When it comes to minerals, mung beans have more selenium and zinc, while black beans have more calcium, copper, iron, magnesium, manganese, phosphorus, and potassium. An easy win for black beans.
Of course, enjoy either or both—but if you’re going to pick one, we say black beans win the day.
Want to learn more?
You might like to read:
Plant vs Animal Protein: Head-to-Head
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The “Yes I Can” Salad
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sometimes, we are given to ask ourselves: “Can I produce a healthy and tasty salad out of what I have in?” and today we show how, with a well-stocked pantry, the answer is “yes I can”, regardless of what is (or isn’t) in the fridge.
You will need
- 1 can cannellini beans, drained
- 1 can sardines (if vegetarian/vegan, substitute ½ can chickpeas, drained)
- 1 can mandarin segments
- 1 handful pitted black olives, from a jar (or from a can, if you want to keep the “yes I can” theme going)
- ½ red onion, thinly sliced (this can be from frozen, defrosted—sliced/chopped onion is always a good thing to have in your freezer, by the way; your writer here always has 1–6 lbs of chopped onions in hers, divided into 1lb bags)
- 1 oz lemon juice
- 1 tbsp chopped parsley (this can be freeze-dried, but fresh is good if you have it)
- 1 tbsp extra virgin olive oil
- 1 tbsp chia seeds
- 1 tsp miso paste
- 1 tsp honey (omit if you don’t care for sweetness; substitute with agave nectar if you do like sweetness but don’t want to use honey specifically)
- 1 tsp red chili flakes
Method
(we suggest you read everything at least once before doing anything)
1) Combine the onion and the lemon juice in a small bowl, massaging gently
2) Mix (in another bowl) the miso paste with the chili flakes, chia seeds, honey, olive oil, and the spare juice from the can of mandarin segments, and whisk it to make a dressing.
3) Add the cannellini beans, sardines (break them into bite-size chunks), mandarin segments, olives, and parsley, tossing them thoroughly (but gently) in the dressing.
4) Top with the sliced onion, discarding the excess lemon juice, and serve:
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Three Daily Servings of Beans?
- We Are Such Stuff As Fish Are Made Of
- Chia: The Tiniest Seeds With The Most Value
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Taurine: An Anti-Aging Powerhouse? Exploring Its Unexpected Benefits
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Mark Rosenberg explains:
Not a stimulant, but…
- Its presence in energy drinks often causes people to assume it’s a stimulant, but it’s not. In fact, it’s a GABA-agonist, thus having a calming effect.
- The real reason it’s in energy drinks is because it helps increase mitochondrial ATP production (ATP = adenosine triphosphate = how cells store energy that’s ready to use; mitochondria take glucose and make ATP)
- Taurine is also anti-inflammatory, antioxidant, and anticancer.
- In the category of aging, human studies are slow to give results for obvious reasons, but mouse studies show that supplementing taurine in middle-aged mice increased their lifespan by 10–12%, as well as improving various physiological markers of aging.
- Taking a closer look at aging—literally; looking at cellular aging—taurine reduces cellular senescence and protects telomeres, thus decreasing DNA mutations.
For more on the science of these, plus Dr. Rosenberg’s personal experience, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
- Taurine’s Benefits For Heart Health And More
- Dr. Greger’s Anti-Aging Eight
- Age & Aging: What Can (And Can’t) We Do About It?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: