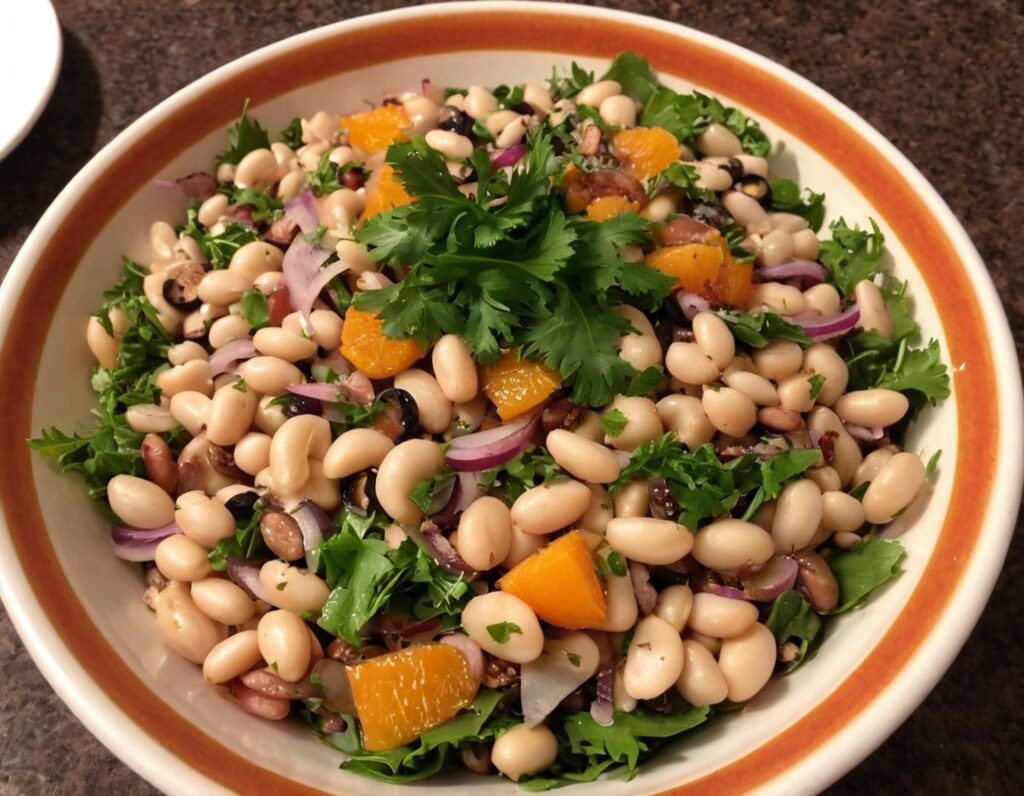Savory Protein Crêpe
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Pancakes have a bad reputation healthwise, but they don’t have to be so. Here’s a very healthy crêpe recipe, with around 20g of protein per serving (which is about how much protein most people’s body’s can use at one sitting) and a healthy dose of fiber too:
You will need
Per crêpe:
- ½ cup milk (your preference what kind; we recommend oat milk for this)
- 2 oz chickpea flour (also called garbanzo bean flour, or gram flour)
- 1 tsp nutritional yeast
- 1 tsp ras el-hanout (optional but tasty and contains an array of beneficial phytochemicals)
- 1 tsp dried mixed herbs
- ⅛ tsp MSG or ¼ tsp low-sodium salt
For the filling (also per crêpe):
- 6 cherry tomatoes, halved
- Small handful baby spinach
- Extra virgin olive oil
Method
(we suggest you read everything at least once before doing anything)
1) Mix the dry crêpe ingredients in a bowl, and then stir in the milk, whisking to mix thoroughly. Leave to stand for at least 5 minutes.
2) Meanwhile, heat a little olive oil in a skillet, add the tomatoes and fry for 1 minute, before adding the spinach, stirring, and turning off the heat. As soon as the spinach begins to wilt, set it aside.
3) Heat a little olive oil either in the same skillet (having been carefully wiped clean) or a crêpe pan if you have one, and pour in a little of the batter you made, tipping the pan so that it coats the pan evenly and thinly. Once the top is set, jiggle the pan to see that it’s not stuck, and then flip your crêpe to finish on the other side.
If you’re not confident of your pancake-tossing skills, or your pan isn’t good enough quality to permit this, you can slide it out onto a heatproof chopping board, and use that to carefully turn it back into the pan to finish the other side.
4) Add the filling to one half of the crêpe, and fold it over, pushing down at the edges with a spatula to make a seal, cooking for another 30 seconds or so. Alternatively, you can just serve a stack of crêpes and add the filling at the table, folding or rolling per personal preference:

Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Level-Up Your Fiber Intake! (Without Difficulty Or Discomfort)
- Three Daily Servings of Beans?
- Lycopene’s Benefits For The Gut, Heart, Brain, & More
- Our Top 5 Spices: How Much Is Enough For Benefits?
- Sea Salt vs MSG – Which is Healthier?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What are ‘Ozempic babies’? Can the drug really increase your chance of pregnancy?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Hundreds of thousands of people worldwide are taking drugs like Ozempic to lose weight. But what do we actually know about them? This month, The Conversation’s experts explore their rise, impact and potential consequences.
We’ve heard a lot about the impacts of Ozempic recently, from rapid weight loss and lowered blood pressure, to persistent vomiting and “Ozempic face”.
Now we’re seeing a rise in stories about “Ozempic babies”, where women who use drugs like Ozempic (semaglutide) report unexpected pregnancies.
But does semaglutide (also sold as Wegovy) improve fertility? And if so, how? Here’s what we know so far.
Remind me, what is Ozempic?
Ozempic and related drugs (glucagon-like peptide-1 receptor agonists or GLP-1-RAs) were developed to help control blood glucose levels in people with type 2 diabetes.
But the reason for Ozempic’s huge popularity worldwide is that it promotes weight loss by slowing stomach emptying and reducing appetite.
Ozempic is prescribed in Australia as a diabetes treatment. It’s not currently approved to treat obesity but some doctors prescribe it “off label” to help people lose weight. Wegovy (a higher dose of semaglutide) is approved for use in Australia to treat obesity but it’s not yet available.
How does obesity affect fertility?
Obesity affects the fine-tuned hormonal balance that regulates the menstrual cycle.
Women with a body mass index (BMI) above 27 are three times more likely than women in the normal weight range to be unable to conceive because they are less likely to ovulate.
The metabolic conditions of type 2 diabetes and polycystic ovary syndrome (PCOS) are both linked to obesity and fertility difficulties.
Women with type 2 diabetes are more likely than other women to have obesity and to experience fertility difficulties and miscarriage.
Similarly, women with PCOS are more likely to have obesity and trouble conceiving than other women because of hormonal imbalances that cause irregular menstrual cycles.
In men, obesity, diabetes and metabolic syndrome (a cluster of conditions that increase the risk of heart disease and stroke) have negative effects on fertility.
Low testosterone levels caused by obesity or type 2 diabetes can affect the quality of sperm.
So how might Ozempic affect fertility?
Weight loss is recommended for people with obesity to reduce the risk of health problems. As weight loss can improve menstrual irregularities, it may also increase the chance of pregnancy in women with obesity.
This is why weight loss and metabolic improvement are the most likely reasons why women who use Ozempic report unexpected pregnancies.
But unexpected pregnancies have also been reported by women who use Ozempic and the contraceptive pill. This has led some experts to suggest that some GLP-1-RAs might affect the absorption of the pill and make it less effective. However, it’s uncertain whether there is a connection between Ozempic and contraceptive failure.
Some women have reported getting pregnant while taking the contraceptive pill and Ozempic. Cottonbro Studio/Pexels In men with type 2 diabetes, obesity and low testosterone, drugs like Ozempic have shown promising results for weight loss and increasing testosterone levels.
Avoid Ozempic if you’re trying to conceive
It’s unclear if semaglutide can be harmful in pregnancy. But data from animal studies suggest it should not be used in pregnancy due to potential risks of fetal abnormalities.
That’s why the Therapeutic Goods Administration recommends women of childbearing potential use contraception when taking semaglutide.
Similarly, PCOS guidelines state health professionals should ensure women with PCOS who use Ozempic have effective contraception.
Guidelines recommended stopping semaglutide at least two months before planning pregnancy.
For women who use Ozempic to manage diabetes, it’s important to seek advice on other options to control blood glucose levels when trying for pregnancy.
What if you get pregnant while taking Ozempic?
For those who conceive while using Ozempic, deciding what to do can be difficult. This decision may be even more complicated considering the unknown potential effects of the drug on the fetus.
While there is little scientific data available, the findings of an observational study of pregnant women with type 2 diabetes who were on diabetes medication, including GLP-1-RAs, are reassuring. This study did not indicate a large increased risk of major congenital malformations in the babies born.
Women considering or currently using semaglutide before, during, or after pregnancy should consult with a health provider about how to best manage their condition.
When pregnancies are planned, women can take steps to improve their baby’s health, such as taking folic acid before conception to reduce the risk of neural tube defects, and stopping smoking and consuming alcohol.
While unexpected pregnancies and “Ozempic babies” may be welcomed, their mothers have not had the opportunity to take these steps and give them the best start in life.
Read the other articles in The Conversation’s Ozempic series here.
Karin Hammarberg, Senior Research Fellow, Global and Women’s Health, School of Public Health & Preventive Medicine, Monash University and Robert Norman, Emeritus Professor of Reproductive and Periconceptual Medicine, The Robinson Research Institute, University of Adelaide
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Clean – by Dr. James Hamblin
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our skin is our largest organ, and it’s easy to forget that, and how much it does for us. All things considered, it’s good to take good care of it! But what if we sometimes take too much “care” of it?
Dr. James Hamblin, a medical doctor-turned-writer, has explored this a lot both personally and in research. Through such, he has come to the conclusion there’s definitely a “sweet spot” of personal hygiene:
- Too little, and the Bubonic plague sweeps through Europe, or other plagues sweep through other places when European invaders came.
- Too much, and we strip our skin of one of its greatest qualities: the ability to protect us.
Dr. Hamblin asks (and answers) such questions as:
- What is good hygiene, and what is neurotically doing ourselves multiple levels of harm because advertising companies shamed us into doing so?
- Is it good or bad to use a series of products, each to undo the problem caused by the previous?
- What the difference between a 5-step skincare routine, and a series of gratuitous iatrogenic damage?
- Which products clean us most helpfully, and which clean us most harmfully?
- How often should we bathe/shower, really?
If the book has a weak point, it’s that it’s written mostly with his body in mind. That makes a difference when it comes to hairwashing, for example. He’s a white guy with short hair. If you’re black and/or have long hair, for example, your haircare needs will be quite different. Similarly, many women engage in shaving/depilation in places that most men don’t, and the consequences of that choice (and implications for any extra washing needs/harms) aren’t covered.
Bottom line: notwithstanding the aforementioned blind-spots, this book will help readers reduce the amount of harm we are doing to our bodies with our washing routines, without sacrificing actual hygiene.
Click here to check out Clean and help your skin to help you!
Share This Post
-
The “Yes I Can” Salad
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sometimes, we are given to ask ourselves: “Can I produce a healthy and tasty salad out of what I have in?” and today we show how, with a well-stocked pantry, the answer is “yes I can”, regardless of what is (or isn’t) in the fridge.
You will need
- 1 can cannellini beans, drained
- 1 can sardines (if vegetarian/vegan, substitute ½ can chickpeas, drained)
- 1 can mandarin segments
- 1 handful pitted black olives, from a jar (or from a can, if you want to keep the “yes I can” theme going)
- ½ red onion, thinly sliced (this can be from frozen, defrosted—sliced/chopped onion is always a good thing to have in your freezer, by the way; your writer here always has 1–6 lbs of chopped onions in hers, divided into 1lb bags)
- 1 oz lemon juice
- 1 tbsp chopped parsley (this can be freeze-dried, but fresh is good if you have it)
- 1 tbsp extra virgin olive oil
- 1 tbsp chia seeds
- 1 tsp miso paste
- 1 tsp honey (omit if you don’t care for sweetness; substitute with agave nectar if you do like sweetness but don’t want to use honey specifically)
- 1 tsp red chili flakes
Method
(we suggest you read everything at least once before doing anything)
1) Combine the onion and the lemon juice in a small bowl, massaging gently
2) Mix (in another bowl) the miso paste with the chili flakes, chia seeds, honey, olive oil, and the spare juice from the can of mandarin segments, and whisk it to make a dressing.
3) Add the cannellini beans, sardines (break them into bite-size chunks), mandarin segments, olives, and parsley, tossing them thoroughly (but gently) in the dressing.
4) Top with the sliced onion, discarding the excess lemon juice, and serve:
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Three Daily Servings of Beans?
- We Are Such Stuff As Fish Are Made Of
- Chia: The Tiniest Seeds With The Most Value
Take care!
Share This Post
Related Posts
-
Life Lessons From A Brain Surgeon – by Dr. Rahul Jandial
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In the category of surgeons with a “what to put on your table to stay off mine” angle, this book packs an extra punch. As well as being an experienced brain surgeon, Dr. Jandial also does a lot of cutting edge lab research too. What does this mean for us?
This book gives, as the subtitle promises, “practical strategies for peak health and performance”—with a brain-centric bias, of course.
From diet and nootropic supplements, to exercise and brain-training, we get a good science-based view of which ones actually work, and which don’t. The style is also very readable; Dr. Jandial is a great educator, presenting genuine scientific content with very accessible language.
Bottom line: if you’d indeed like to look after your most important organ optimally, this book gives a lot of key pointers, without unnecessary fluff.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Is It Possible To Lose Weight Quickly?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In Victorian England, weight-loss trends like the dangerous tapeworm diet were popular. While modern fad diets can seem less extreme, they often promise similarly fast results. However, these quick fixes can have similarly harmful consequences:
Not so fast
To illustrate the difference between gradual and extreme dieting, the video bids us consider two identical twins, Sam and Felix:
- Sam adopts a gradual approach, slowly reducing calorie intake and exercising regularly. This causes his body to burn glycogen stores before transitioning to fat as an energy source. Regular exercise helps Sam maintain muscle mass, which boosts his metabolism and supports sustained weight loss.
- Felix drastically cuts calories, forcing his body into starvation mode. He quickly depletes glycogen stores, loses muscle mass, and burns fewer calories, making long-term weight loss more difficult. Although Felix might initially lose water weight, this is temporary and unsustainable.
You cannot “just lose it quickly now, and then worry about healthiness once the weight’s gone”, because you will lose health much more quickly than you will lose fat, and that will sabotage, rather than help, your fat loss journey.Healthy weight loss requires gradual, balanced changes in diet and exercise tailored to individual needs. Extreme diets, whether through calorie restriction or things like elimination of carbs or fats, are unsustainable and shock the body. It’s important to prioritize long-term health over societal pressures for quick weight loss and focus on developing a sustainable, healthy lifestyle.
In short, the quickest way to lose weight and keep it off (without dying), is to lose it slowly.
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
How To Lose Weight (Healthily)
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Beneficial Is MCT Oil, Really?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Often derived from coconuts (though it doesn’t have to be), medium-chain triglycerides (MCTs) are trendy… But does the science back the hype?
First, the principle
MCTs are commonly enjoyed because unlike short- or long-chain fatty acids, they can be quickly broken down and either immediately converted quickly and easily into energy, or turned into ketones in the case of a surplus (in the case of true excess, however, it’ll simply be stored as fat).
Most of that involves the liver, so for anyone who wants a refresher on liver health:
How To Unfatty A Fatty Liver ← notwithstanding the title, this is also important knowledge even if your liver is healthy now—if you’d like it to stay healthy, anyway!
You can also read about the ins and outs of glycogen metabolism and the body’s energy-based metabolic processes in general (including the body’s energy processes that go on in the liver), here:
From Apples to Bees, and High-Fructose Cs: Which Sugars Are Healthier, And Which Are Just The Same?
If the liver turns the MCTs into ketones, those ketones will then be used for energy if there is insufficient glucose available (as the body will always use glucose from the blood first, if available, before moving to alternative energy sources such as ketones and/or fat reserves.)
Thus, many people look to ketones as a solution for having enough energy to function while on a very low-carb diet such as the ketogenic diet:
Ketogenic Diet: Burning Fat Or Burning Out?
…which as you’ll recall, does work for short-term weight loss, but brings long-term health risks, so should not be undertaken for long periods of time.
So, does MCT Oil help?
With regard to weight loss, the research is weak and mixed:
- Weak, because often the methodology was shoddy, often there are many factors not controlled-for, and often the sample sizes were small (and also, RCTs by their very nature tend to be quite short-term (often 6, 8, or 12 weeks), whereas heavy reliance on ketones from MCTs may fall into the same long-term problems as the ketogenic diet in general).
- Mixed, because the results varied widely (probably because of the aforementioned problems).
Rather than pick at individual studies, let’s look at this review and meta-analysis of 13 studies, with a combined sample size of 749 people (so you can imagine how small the individual RCTs were):
❝Compared with LCTs, MCTs decreased body weight (-0.51 kg [95% CI-0.80 to -0.23 kg]; P<0.001; I(2)=35%); waist circumference (-1.46 cm [95% CI -2.04 to -0.87 cm]; P<0.001; I(2)=0%), hip circumference (-0.79 cm [95% CI -1.27 to -0.30 cm]; P=0.002; I(2)=0%), total body fat (standard mean difference -0.39 [95% CI -0.57 to -0.22]; P<0.001; I(2)=0%), total subcutaneous fat (standard mean difference -0.46 [95% CI -0.64 to -0.27]; P<0.001; I(2)=20%), and visceral fat (standard mean difference -0.55 [95% CI -0.75 to -0.34]; P<0.001; I(2)=0%).
No differences were seen in blood lipid levels.
Many trials lacked sufficient information for a complete quality assessment, and commercial bias was detected.❞
So, if we’re going to take those numbers at face value, that means a net weight loss, over the course of the trial period, was…
*drumroll*
0.51kg (that’s about 1 lb).
To put that into perspective, if you did nothing else but pee 1 cup of urine before getting weighed, you’d register as having lost 0.25kg (or about ½ lb) by virtue of the bathroom trip alone.
Here’s the paper:
What about cholesterol and heart health?
With regard to cholesterol, MCT oil is touted as improving blood lipids, which means lowering LDL and increasing HDL (within a safe range, anyway).
You’ll remember that the above review concluded “No differences were seen in blood lipid levels”.
It may again be a case of individual studies cancelling each other out. For example…
This study found that it improved lipids in 40 young women as part of a calorie-controlled interventional diet:
This study found that it worsened lipids in 17 young men, worse even than taking an equivalent amount of sunflower oil:
In short, it’s a gamble.
It may be good for insulin sensitivity, though
This one seems to be specific to people with type 2 diabetes. The paper heading says it all, but we include the link in case you want to know the details (the short version is, it improved insulin sensitivity in diabetic subjects only (not others), and didn’t affect anything else that was measured:
The sample size was small (20 people total, of whom 10 had diabetes), and the next study was with 40 people, this time moderately overweight and all with type 2 diabetes:
Want to try some?
We don’t sell it, but here for your convenience is an example product on Amazon 😎
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: