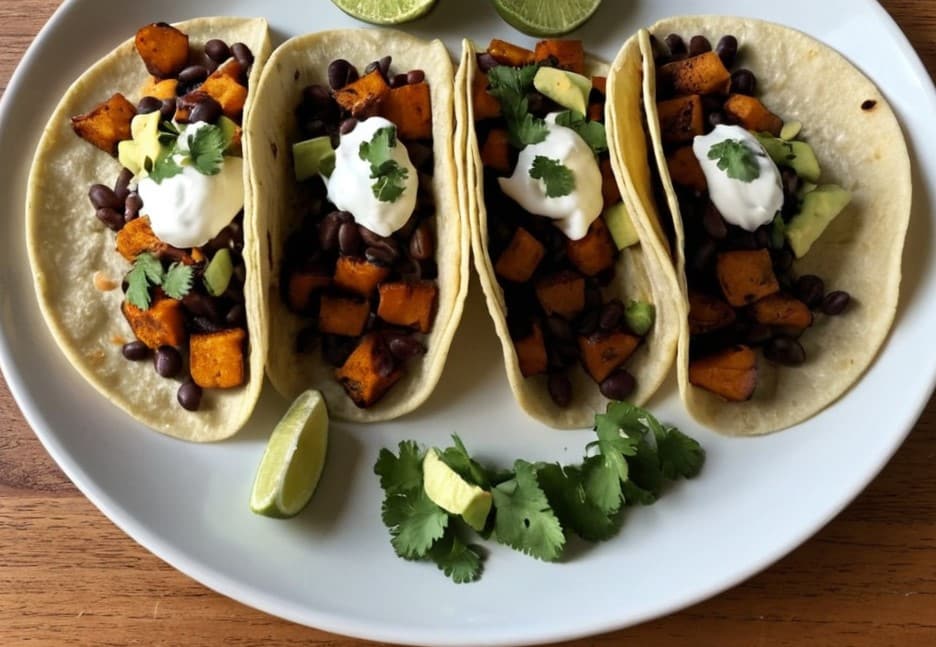A Hospital Kept a Brain-Damaged Patient on Life Support to Boost Statistics. His Sister Is Now Suing for Malpractice.
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
ProPublica is a Pulitzer Prize-winning investigative newsroom. Sign up for The Big Story newsletter to receive stories like this one in your inbox.
In 2018, Darryl Young was hoping for a new lease on life when he received a heart transplant at a New Jersey hospital after years of congestive heart failure. But he suffered brain damage during the procedure and never woke up.
The following year, a ProPublica investigation revealed that Young’s case was part of a pattern of heart transplants that had gone awry at Newark Beth Israel Medical Center in 2018. The spate of bad outcomes had pushed the center’s percentage of patients still alive one year after surgery — a key benchmark — below the national average. Medical staff were under pressure to boost that metric. ProPublica published audio recordings from meetings in which staff discussed the need to keep Young alive for a year, because they feared another hit to the program’s survival rate would attract scrutiny from regulators. On the recordings, the transplant program’s director, Dr. Mark Zucker, cautioned his team against offering Young’s family the option of switching from aggressive care to comfort care, in which no lifesaving efforts would be made. He acknowledged these actions were “very unethical.”
ProPublica’s revelations horrified Young’s sister Andrea Young, who said she was never given the full picture of her brother’s condition, as did the findings of a subsequent federal regulator’s probe that determined that the hospital was putting patients in “immediate jeopardy.” Last month, she filed a medical malpractice lawsuit against the hospital and members of her brother’s medical team.
The lawsuit alleges that Newark Beth Israel staff were “negligent and deviated from accepted standards of practice,” leading to Young’s tragic medical outcome.
Defendants in the lawsuit haven’t yet filed responses to the complaint in court documents. But spokesperson Linda Kamateh said in an email that “Newark Beth Israel Medical Center is one of the top heart transplant programs in the nation and we are committed to serving our patients with the highest quality of care. As this case is in active litigation, we are unable to provide further detail.” Zucker, who is no longer on staff at Newark Beth Israel, didn’t respond to requests for comment. His attorney also didn’t respond to calls and emails requesting comment.
Zucker also didn’t respond to requests for comment from ProPublica in 2018; Newark Beth Israel at the time said in a statement, made on behalf of Zucker and other staff, that “disclosures of select portions of lengthy and highly complex medical discussions, when taken out of context, may distort the intent of conversations.”
The lawsuit alleges that Young suffered brain damage as a result of severely low blood pressure during the transplant surgery. In 2019, when the federal Centers for Medicare and Medicaid Services scrutinized the heart transplant program following ProPublica’s investigation, the regulators found that the hospital had failed to implement corrective measures even after patients suffered, leading to further harm. For example, one patient’s kidneys failed after a transplant procedure in August 2018, and medical staff made recommendations internally to increase the frequency of blood pressure measurement during the procedure, according to the lawsuit. The lawsuit alleges that the hospital didn’t implement its own recommendations and that one month later, “these failures were repeated” in Young’s surgery, leading to brain damage.
The lawsuit also alleges that Young wasn’t asked whether he had an advance directive, such as a preference for a do-not-resuscitate order, despite a hospital policy stating that patients should be asked at the time of admission. The lawsuit also noted that CMS’ investigation found that Andrea Young was not informed of her brother’s condition.
Andrea Young said she understands that mistakes can happen during medical procedures, “however, it’s their duty and their responsibility to be honest and let the family know exactly what went wrong.” Young said she had to fight to find out what was going on with her brother, at one point going to the library and trying to study medical books so she could ask the right questions. “I remember as clear as if it were yesterday, being so desperate for answers,” she said.
Andrea Young said that she was motivated to file the lawsuit because she wants accountability. “Especially with the doctors never, from the outset, being forthcoming and truthful about the circumstances of my brother’s condition, not only is that wrong and unethical, but it took a lot away from our entire family,” she said. “The most important thing to me is that those responsible be held accountable.”
ProPublica’s revelation of “a facility putting its existence over that of a patient is a scary concept,” said attorney Jonathan Lomurro, who’s representing Andrea Young in this case with co-counsel Christian LoPiano. Besides seeking damages for Darryl Young’s children, “we want to call attention to this so it doesn’t happen again,” Lomurro said.
The lawsuit further alleges that medical staff at Newark Beth Israel invaded Young’s privacy and violated the Health Insurance Portability and Accountability Act, more commonly known as HIPAA, by sharing details of his case with the media without his permission. “We want people to be whistleblowers and want information out,” but that information should be told to patients and their family members directly, Lomurro said.
The 2019 CMS investigation determined that Newark Beth Israel’s program placed patients in “immediate jeopardy,” the most serious level of violation, and required the hospital to implement corrective plans. Newark Beth Israel did not agree with all of the regulator’s findings and in a statement at the time said that the CMS team lacked the “evidence, expertise and experience” to assess and diagnose patient outcomes.
The hospital did carry out the corrective plans and continues to operate a heart transplant program today. The most recent federal data, based on procedures from January 2021 through June 2023, shows that the one year probability of survival for a patient at Newark Beth is lower than the national average. It also shows that the number of graft failures, including deaths, in that time period was higher than the expected number of deaths for the program.
Andrea Young said she’s struggled with a feeling of emptiness in the years after her brother’s surgery. They were close and called each other daily. “There’s nothing in the world that can bring my brother back, so the only solace I will have is for the ones responsible to be held accountable,” she said. Darryl Young died on Sept 12, 2022, having never woken up after the transplant surgery.
A separate medical malpractice lawsuit filed in 2020 by the wife of another Newark Beth Israel heart transplant patient who died after receiving an organ infected with a parasitic disease is ongoing. The hospital has denied the allegations in court filing. The state of New Jersey, employer of the pathologists named in the case, settled for $1.7 million this month, according to the plaintiff’s attorney Christian LoPiano. The rest of the case is ongoing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Sweet Potato & Black Bean Tacos
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fiber, protein, and polyphenols! What more could one ask for? Well, great taste and warm healthy goodness, which these deliver:
You will need
For the sweet potatoes:
- 2 medium sweet potatoes, cubed (we recommend leaving the skin on, but you can peel them if you really want to)
- 1 tbsp extra virgin olive oil
- 2 tsp garlic powder
- 2 tsp smoked paprika
- 1 tsp chili powder
- 1 tsp black pepper
- 1 tsp ground cumin
- 1 tsp ground turmeric
- ½ tsp MSG or 1 tsp low-sodium salt
For the black beans:
- 2 cans black beans, drained and rinsed (or 2 cups black beans that you cooked yourself)
- ¼ bulb garlic, minced
- 1 fresh jalapeño finely chopped (or ¼ cup jalapeños from a jar, finely chopped) ← adjust quantities per your preference and per the quality of the pepper(s) you’re using; we can’t judge that from here without tasting them, so we give a good basic starting suggestion.
- 2 tsp black pepper
- 1 tsp red chili flakes
- ½ tsp MSG or 1 tsp low-sodium salt
For serving:
- 8 small corn tortillas, or your preference if substituting
- 1 avocado, pitted, peeled, cubed, and tossed in lime juice ← we’re mentioning this here because you want to do this as soon as you cut it, to avoid oxidation
- Any other salad you’d like to include; fresh parsley is also a good option when it comes to greenery, or cilantro if you don’t have the soap gene
- Tomato salsa (quantity and spice level per your preference)
Method
(we suggest you read everything at least once before doing anything)
1) Preheat the oven to 400°F / 200°C.
2) Toss the sweet potato cubes in a large bowl with the rest of the ingredients from the sweet potato section above, ensuring they are evenly coated.
3) Bake them in the oven, on a baking tray lined with baking paper, for about 30 minutes or until tender inside and crispy at the edges. Turn them over halfway through.
4) While that’s happening, mix the black beans in a bowl with the other ingredients from the black bean section above, and heat them gently. You could do this in a saucepan, but honestly, while it’s not glamorous, the microwave is actually better for this. Note: many people find the microwave cooks food unevenly, but there are two reasons for this and they’re both easily fixable:
- instead of using high power for x minutes, use medium power for 2x minutes; this will produce better results
- instead of putting the food just in a bowl, jug, or similar, use a wide bowl or similar container, and then inside that, place a small empty microwave-safe glass jar or similar upturned in the middle, and then add the food around it, so that the food is arranged in a donut shape rather than a wide cylinder shape. This means there is no “middle bit” to go underheated while the edges are heated excessively; instead, it will heat through evenly.
If you really don’t want to do that though, use a saucepan on a very low heat, add a small amount of liquid (or tomato salsa), and stir constantly.
5) Heat the tortillas in a dry skillet for about 30 seconds each on each side, when ready to serve.
6) Assemble the tacos; you can do this how you like but a good order of operations is: tortilla, leafy salad (if using), potato, beans, non-leafy salad including avocado, salsa or other topping per your preference.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- White Potato vs Sweet Potato – Which is Healthier?
- Kidney Beans or Black Beans – Which is Healthier?
- Coconut vs Avocado – Which is Healthier?
- Glutathione: More Than An Antioxidant
- Our Top 5 Spices: How Much Is Enough For Benefits? ← we hit 4/5 today!
Take care!
Share This Post
-
Are You Taking PIMs?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Getting Off The Overmedication Train
The older we get, the more likely we are to be on more medications. It’s easy to assume that this is because, much like the ailments they treat, we accumulate them over time. And superficially at least, that’s what happens.
And yet, almost half of people over 65 in Canada are taking “potentially inappropriate medications”, or PIMs—in other words, medications that are not needed and perhaps harmful. This categorization includes medications where the iatrogenic harms (side effects, risks) outweigh the benefits, and/or there’s a safer more effective medication available to do the job.
You may be wondering: what does this mean for the US?
Well, we don’t have the figures for the US because we’re working from Canadian research today, but given the differences between the two country’s healthcare systems (mostly socialized in Canada and mostly private in the US), it seems a fair hypothesis that if it’s almost half in Canada, it’s probably more than half in the US. Socialized healthcare systems are generally quite thrifty and seek to spend less on healthcare, while private healthcare systems are generally keen to upsell to new products/services.
The three top categories of PIMs according to the above study:
- Gabapentinoids (anticonvulsants also used to treat neuropathic pain)
- Proton pump inhibitors (PPIs)
- Antipsychotics (especially, to people without psychosis)
…but those are just the top of the list; there are many many more.
The list continues: opioids, anticholinergics, sulfonlyurea, NSAIDs, benzodiazepines and related rugs, and cholinesterase inhibitors. That’s where the Canadian study cuts off (although it also includes “others” just before NSAIDs), but still, you guessed it, there are more (we’re willing to bet statins weigh heavily in the “others” section, for a start).
There are two likely main causes of overmedication:
The side effect train
This is where a patient has a condition and is prescribed drug A, which has some undesired side effects, so the patient is prescribed drug B to treat those. However, that drug also has some unwanted side effects of its own, so the patient is prescribed drug C to treat those. And so on.
For a real-life rundown of how this can play out, check out the case study in:
The Hidden Complexities of Statins and Cardiovascular Disease (CVD)
The convenience factor
No, not convenient for you. Convenient for others. Convenient for the doctor if it gets you out of their office (socialized healthcare) or because it was easy to sell (private healthcare). Convenient for the staff in a hospital or other care facility.
This latter is what happens when, for example, a patient is being too much trouble, so the staff give them promazine “to help them settle down”, notwithstanding that promazine is, besides being a sedative, also an antipsychotic whose common side effects include amenorrhea, arrhythmias, constipation, drowsiness and dizziness, dry mouth, impotence, tiredness, galactorrhoea, gynecomastia, hyperglycemia, insomnia, hypotension, seizures, tremor, vomiting and weight gain.
This kind of thing (and worse) happens more often towards the end of a patient’s life; indeed, sometimes precipitating that end, whether you want it or not:
Mortality, Palliative Care, & Euthanasia
How to avoid it
Good practice is to be “open-mindedly skeptical” about any medication. By this we mean, don’t reject it out of hand, but do ask questions about it.
Ask your prescriber not only what it’s for and what it’ll do, but also what the side effects and risks are, and an important question that many people don’t think to ask, and for which doctors thus don’t often have a well-prepared smooth-selling reply, “what will happen if I don’t take this?”
And look up unbiased neutral information about it, from reliable sources (Drugs.com and The BNF are good reference guides for this—and if it’s important to you, check both, in case of any disagreement, as they function under completely different regulatory bodies, the former being American and the latter being British. So if they both agree, it’s surely accurate, according to best current science).
Also: when you are on a medication, keep a journal of your symptoms, as well as a log of your vitals (heart rate, blood pressure, weight, sleep etc) so you know what the medication seems to be helping or harming, and be sure to have a regular meds review with your doctor to check everything’s still right for you. And don’t be afraid to seek a second opinion if you still have doubts.
Want to know more?
For a more in-depth exploration than we have room for here, check out this book that we reviewed not long back:
To Medicate or Not? That is the Question! – by Dr. Asha Bohannon
Take care!
Share This Post
-
Laugh Often, To Laugh Longest!
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Putting The Abs Into Absurdity
We’ve talked before about the health benefits of a broadly positive outlook on life:
Optimism Seriously Increases Longevity!
…and we’re very serious about it, but that’s about optimistic life views in general, and today we’re about not just keeping good humor in questionable circumstances, but actively finding good humor in the those moments—even when the moments in question might not be generally described as good!
After all, laughter really can be the best medicine, for example:
From the roots
First a quick recap on de-toothing the psychological aspect of threats, no matter how menacing they may be:
Hello, Emotions: Time For Radical Acceptance!
…which we can then take a step further:
What’s The Worst That Could Happen?
Choose your frame
Do you remember when that hacker hacked and publicized the US Federal no-fly list, after already hacking a nationwide cloud-based security camera company, getting access to more than 150,000 companies’ and private individuals’ security cameras, amongst various other cyber crimes, mostly various kinds of fraud and data theft?
Imagine how she (age 21) must have felt, when being indicted. What do you suppose this hacker had to say for itself under such circumstances?
❝congress is investigating now 🙂
but i stay silly :3 ❞
…the latter half of which, usually rendered “but I stay silly” or “but we stay silly” has since entered popular Gen-Z parlance, usually after expressing some negative thing, often in a state of powerlessness.
Which is an important life skill if powerlessness is something that is often likely.
It’s important for many Gen-Zs with negligible life prospects economically; it’s equally important for 60-somethings getting cancer diagnoses (statistically the most likely decade to find out one has cancer, by the way), and many other kinds of people younger, older, and in between.
Because at the end of the day, we all start powerless and we all end powerless.
Learned helplessness (two kinds)
In psychology, “learned helplessness” occurs when a person or creature gives up after learning that all and any attempts to resist a Bad Thing™ fail, perhaps even badly. A lab rat may just shut down and sit there getting electroshocked, for example. A person subjected to abuse may stop trying to improve their situation, and just go with the path of least resistance.
But, there’s another kind, wherein someone in a position of absolute powerlessness not only makes their peace with that, but also, decides that the one thing the outside world can’t control, is how they take it. Like the hacker we mentioned earlier.
Sometimes the gallows humor is even more literal, laughing at one’s own impending death. Not as a matter of bravado, but genuinely seeing the funny side.
But how?
Unfortunately, fortunately
The trick here is to “find a silver lining” that is nowhere near enough to compensate for the bad thing—and it may even be worse! But that’s fine:
“Unfortunately, I didn’t have time to do the dishes before leaving for my vacation. Fortunately, I also forgot to turn the oven off, so the house burning down covered up my messy kitchen”
Writer’s personal less drastic example: today I set my espresso machine to press me an espresso; it doesn’t have an auto-off and I got distracted and it overflowed everywhere; my immediate reaction was “Oh! I have been blessed with an abundance of coffee!”
This kind of silly little thing, on a daily basis, builds a very solid habit for life that allows one to see the funny side in even the most absurd situations, even matters of life and death (can confirm: been there enough times personally—so far so good, still alive to find the remembered absurdity silly).
The point is not to genuinely value the “silver lining”, because half the time it isn’t even one, really, and it is useless to pretend, in seriousness.
But to pretend in silliness? Now we’re onto something, and the real benefit is in the laughs we had along the way.
Because those worst moments? Are probably when we need it the most, so it’s good to get some practice in!
Want more ways to find the funny and make it a life habit?
We reviewed a good book recently:
The Humor Habit: Rewire Your Brain To Stress Less, Laugh More, And Achieve More’er – by Paul Osincup
Stay silly!
Share This Post
Related Posts
-
I’m a medical forensic examiner. Here’s what people can expect from a health response after a sexual assault
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
An estimated one in five women and one in 16 men in Australia have experienced sexual violence.
After such a traumatic experience, it’s understandable many are unsure if they want to report it to the police. In fact, less than 10% of Australian women who experience sexual assault ever make a police report.
In Australia there is no time limit on reporting sexual assault to police. However, there are tight time frames for collecting forensic evidence, which can sometimes be an important part of the police investigation, whether it’s commenced at the time or later.
This means the decision of whether or not to undergo a medical forensic examination needs to be made quite quickly after an assault.
I work as a medical forensic examiner. Here’s what you can expect if you present for a medical forensic examination after a sexual assault.
fizkes/Shutterstock A team of specialists
There are about 100 sexual assault services throughout Australia providing 24-hour care. As with other areas of health care, there are extra challenges in regional and rural areas, where there are often further distances to travel and staff shortages.
Sexual assault services in Australia are free regardless of Medicare status. To find your nearest service you can call 1800 RESPECT (1800 737 732) or Full Stop Australia (1800 385 578) who can also provide immediate telephone counselling support.
It’s important to call the local sexual assault service before turning up. They can provide the victim-survivor with information and advice to prevent delays and make the process as helpful as possible.
The consultation usually occurs in a hospital emergency department which has a designated forensic suite, or in a specialised forensic service.
The victim-survivor is seen by a doctor or nurse trained in medical and forensic care. There’s a sexual assault counsellor, crisis worker or social worker present to support the patient and offer counselling advice. This is called an “integrated response” with medical and psychosocial staff working together.
In most cases the victim-survivor can have their own support person present too.
Depending on what the victim-survivor wants, the doctor or nurse will take a history of the assault to guide any medical care which may be needed (such as emergency contraception) and to guide the examination.
Sexual assault services are always very aware of giving victim-survivors a choice about having a medical forensic examination. If a person presents to a sexual assault service, they can receive counselling and medical care without undergoing a forensic examination if they do not wish to. https://www.youtube.com/embed/CGlbTgia0Ek?wmode=transparent&start=0 Sexual assault services are inclusive of all genders.
Collecting forensic samples
Samples collected during a medical forensic examination can sometimes identify the perpetrator’s DNA or intoxicating substances (alcohol or drugs that might be relevant to the investigation). The window of opportunity to collect these samples can be as short as 12 hours, or up to 5–7 days, depending on the nature of the sexual assault.
In most of Australia, an adult who has experienced a recent sexual assault can be offered a medical forensic examination without making a report to police.
Depending on the state or territory, the forensic samples can usually be stored for 3 to 12 months (up to 100 years in Tasmania). This allows the victim-survivor time to decide if they want to release them to police for processing.
The doctor or nurse will collect the samples using a sexual assault investigation kit, or a “rape kit”.
Collecting these samples might involve taking swabs to try to detect DNA from external and internal genital areas and anywhere there may have been DNA transfer. This can be from skin cells, where the perpetrator touched the victim-survivor, or from bodily fluids including semen or saliva.
The doctor or nurse carrying out the examination do their best to minimise re-traumatisation, by providing the victim-survivor information, choices and control at every step of the process.
The victim-survivor can usually have a support person with them. Monkey Business Images/Shutterstock How about STIs and pregnancy?
During the consultation, the doctor or nurse will address any concerns about sexually transmitted infections (STIs) and pregnancy, if applicable.
In most cases the risk of STIs is small. But follow-up testing at 1–2 weeks for infections such as chlamydia and gonorrhoea, and at 6–12 weeks for infections such as syphilis and HIV, is usually recommended.
Emergency contraception (sometimes called the “morning after pill”) can be provided to prevent pregnancy. It can be taken up to five days after sexual assault (but the sooner the better) with follow-up pregnancy testing recommended at 2–3 weeks.
Things have improved over time
When I was a junior doctor in the late 90s, taking forensic swabs was usually the responsibility of the busy obstetrics and gynaecology trainee in the emergency department, who was often managing multiple patients and had little training in forensics. There was also usually no supportive counsellor.
Anecdotally, both the doctor and the patient were traumatised by this experience. Research shows that when specialised, integrated services are not provided, victim-survivors’ feelings of powerlessness are magnified.
But the way we carry out medical forensic examinations after sexual assault in Australia has improved over the years.
With patient-centred practices, and designated forensic and counselling staff, the experience for the patient is thought to be empowering rather than re-traumatising.
Our research
In new research published in the Australian Journal of General Practice, my colleagues and I explored the experience of the medical forensic examination from the victim-survivor’s perspective.
We surveyed 291 patients presenting to a sexual assault service in New South Wales (where I work) over four years.
Some 75% of patients reported the examination was reassuring and another 20% reported it was OK. Only 2% reported that it was traumatising. The majority (98%) said they would recommend a friend present to a sexual assault service if they were in a similar situation.
While patients spoke positively about the care they received, many commented that the sexual assault service was not visible enough. They didn’t know how to find it or even that it existed.
We know many victim-survivors don’t present to a sexual assault service or undergo a medical forensic examination after a sexual assault. So we need to do more to increase the visibility of these services.
The National Sexual Assault, Family and Domestic Violence Counselling Line – 1800 RESPECT (1800 737 732) – is available 24 hours a day, seven days a week for any Australian who has experienced, or is at risk of, family and domestic violence and/or sexual assault.
Mary Louise Stewart, Senior Career Medical Officer, Northern Sydney Local Health District; PhD Candidate, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Kidney Beans or Black Beans – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing kidney beans to black beans, we picked the black beans.
Why?
First, do note that black beans are also known as turtle beans, or if one wants to hedge one’s bets, black turtle beans. It’s all the same bean. As a small linguistic note, kidney beans are known as “red beans” in many languages, so we could have called this “red beans vs black beans”, but that wouldn’t have landed so well with our largely anglophone readership. So, kidney beans vs black beans it is!
They’re certainly both great, and this is a close one today…
In terms of macros, they’re equal on protein and black beans have more carbs and/but also more fiber. So far, so equal—or rather, if one pulls ahead of the other here, it’s a matter of subjective priorities.
In the category of vitamins, they’re equal on vitamins B2, B3, and choline, while kidney beans have more of vitamins B6, B9, C, and K, and black beans have more of vitamins A, B1, B5, and E. In other words, the two beans are still tied with a 4:4 split, unless we want to take into account that that vitamin E difference is that black beans have 29x more vitamin E, in which case, black beans move ahead.
When it comes to minerals, finally the winner becomes apparent; while kidney beans have a little more manganese and zinc, on the other hand black beans have more calcium, copper, iron, magnesium, phosphorus, potassium, and selenium. However, it should be noted that honestly, the margins aren’t huge here and kidney beans are almost as good for all of these minerals.
In short, black beans win the day, but kidney beans are very close behind, so enjoy whichever you prefer, or better yet, both! They go great together in tacos, burritos, or similar, by the way.
Want to learn more?
You might like to read:
- Kidney Beans vs Fava Beans – Which is Healthier?
- Chickpeas vs Black Beans – Which is Healthier?
- Bold Beans – by Amelia Christie-Miller ← this is a recipe book; if you’re looking to incorporate more beans into your diet and want to make it good, this cookbook can lead the way!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Jumping Rope Changes The Human Body
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Most popularly enjoyed by professional boxers and six-year-old girls, jumping rope is one of the most metabolism-boosting exercises around:
Just a hop, skip, and a jump away from good health
Maybe you haven’t tried it since your age was in single digits, so, if you do…
What benefits can you expect?
- Improves cardiovascular fitness, equivalent to 30 minutes of running with just 10 minutes of jumping.
- Increases bone density and boosts immunity by aiding the lymphatic system.
- Enhances explosiveness in the lower body, agility, and stamina.
- Improves shoulder endurance, coordination, and spatial awareness.
What kind of rope is best for you?
- Beginner ropes: licorice ropes (nylon/vinyl), beaded ropes for rhythm and durability.
- Advanced ropes: speed ropes (denser, faster materials) for higher speeds and more difficult skills.
- Weighted ropes: build upper body muscles (forearms, shoulders, chest, back).
What length should you get?
- Recommended rope length varies by height (8 ft for 5’0″–5’4″, 9 ft for 5’5″–5’11”, 10 ft for 6’0″ and above).
- Beginners should start with longer ropes for clearance.
What should you learn?
- Initial jump rope skills: start with manageable daily jump totals, gradually increasing as ankles, calves, and feet adapt.
- Further skills: learn the two-foot jump and then the boxer’s skip for efficient, longer sessions and advanced skills. Keep arms close and hands at waist level for a smooth swing.
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
How To Do High Intensity Interval Training (Without Wrecking Your Body)
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: