Unfuck Your Brain – by Dr. Faith Harper
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This book takes a trauma-informed care approach, which is relatively novel in the mental health field and it’s quickly becoming the industry standard because of its effectiveness.
The basic premise of trauma-informed care is that you had a bad experience (possibly even more than one—what a thought!) and that things that remind you of that will tend to prompt reactivity from you in a way that probably isn’t healthy. By identifying each part of that process, we can then interrupt it, much like we might with CBT (the main difference being that CBT, for all its effectiveness, tends to assume that the things that are bothering you are not true, while TIC acknowledges that they might well be, and that especially historically, they probably were).
A word of warning: if something that triggers a trauma-based reactivity response in you is people swearing, then this book will either cure you by exposure therapy or leave you a nervous wreck, because it’s not just the title; Dr. Harper barely gets through a sentence without swearing. It’s a lot, even by this (European) reviewer’s standards (we’re a lot more relaxed about swearing over here, than people tend to be in America).
On the other hand, something that Dr. Harper excels at is actually explaining stuff very well. So while it sometimes seems like she’s “trying too hard” style-wise in terms of being “not like other therapists”, in her defence she’s nevertheless a very good writer; she knows her stuff, and knows how to communicate it clearly.
Bottom line: if you don’t mind a writer who swears more than 99% of soldiers, then this book is an excellent how-to guide for self-administered trauma-informed care.
Click here to check out Unfuck Your Brain, and indeed unfuck it!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
100,000 People, 30 Years, One Clear Winner vs Aging
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Generally speaking, the scientific community most highly lauds the Mediterranean diet as being best for general health:
The Mediterranean Diet: What Is It Good For? ← what isn’t it good for?!
However, even this can be tweaked with specific health considerations in mind, for example:
Four Ways To Upgrade The Mediterranean Diet ← these tweaks offer adjusted versions of the Mediterranean diet, optimized for anti-inflammation, gut health, heart health, or brain health
And today we present to you some very good research into…
The best diet for aging well
Let’s be clear on terms first: by “aging well”, this means reaching age 70 without chronic diseases and maintaining good cognitive, physical, and mental health.
105,015 participants (of whom, 66% women, average age 53 at the start of the study) were followed for up to 30 years. Not in the stalkery way, but in the longitudinal study way. We say “up to”, because as with any sizeable longitudinal study, some died before the end of the study.
9,771 of them were deemed, at the end of the study, to have achieved “healthy aging”.
So, how did those participants achieve that, in terms of diet?
The dietary patterns that had the strongest positive impact were:
- AHEI (Alternative Healthy Eating Index): best for mental and physical function, overall healthy aging.
- PHDI (Planetary Health Diet Index): best for cognitive health and survival to age 70.
- DASH (Dietary Approaches to Stop Hypertension): strongest general impact.
- MIND (Mediterranean-DASH Intervention for Neurodegenerative Delay): best for brain health.
- rEDIH (Reversed Empirical Dietary Index for Hyperinsulinemia): most effective for chronic disease prevention.
In contrast:
- EIDP (Empirically Inflammatory Dietary Pattern): shocking nobody, performed least well in all areas
You are probably wondering what those dietary patterns actually consist of, so click here to see a chart of what’s included or excluded in each dietary pattern.
As you can see, the AHEI diet that was “best for mental and physical function, overall healthy aging” is essentially the Mediterranean diet with three small tweaks:
- no seafood, but long-chain omega-3 fatty acids include to compensate
- no sugar-sweetened beverages or fruit juices
- “no” sodium (in other words, minimal sodium, since almost everything contains trace amounts)
The PHDI diet, which was “best for cognitive health and survival to age 70” is essentially a whole-foods plant-based diet. Which in turn is very consistent with the Mediterranean, except that it excludes animal products, of which the Mediterranean diet uses small amounts.
You can read the paper in its entirety here:
Optimal dietary patterns for healthy aging
Want to know more?
A panel of 69 doctors and nutritionists examined the evidence for 38 diets (including Mediterranean, MIND, DASH, Vegan, Keto, Slimfast, WeightWatchers, Nutrisystem, and more) and scored them in 21 categories (e.g. best for general health, best for weight loss, best for heart, best against diabetes, etc):
Which Diet? Top Diets Ranked By Experts
Enjoy!
Share This Post
-
Getting to Neutral – by Trevor Moawad
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We all know that a pessimistic outlook is self-defeating… And yet, toxic positivity can also be a set-up for failure! At some point, reckless faith in the kindly nature of the universe will get crushed, badly. Sometimes that point is a low point in life… sometimes it’s six times a day. But one thing’s for sure: we can’t “just decide everything will go great!” because the world just doesn’t work that way.
That’s where Trevor Moawad comes in. “Getting to neutral” is not a popular selling point. Everyone wants joy, abundance, and high after high. And neutrality itself is often associated with boredom and soullessness. But, Moawad argues, it doesn’t have to be that way.
This book’s goal—which it accomplishes well—is to provide a framework for being a genuine realist. What does that mean?
“I’m not a pessimist; I’m a realist” – every pessimist ever.
^Not that. That’s not what it means. What it means instead is:
- Hope for the best
- Prepare for the worst
- Adapt as you go
…taking care to use past experiences to inform future decisions, but without falling into the trap of thinking that because something happened a certain way before, it always will in the future.
To be rational, in short. Consciously and actively rational.
Feel the highs! Feel the lows! But keep your baseline when actually making decisions.
Bottom line: this book is as much an antidote to pessimism and self-defeat, as it is to reckless optimism and resultant fragility. Highly recommendable.
Click here to check out “Getting to Neutral” and start creating your best, most reason-based life!
PS: in this book, Moawad draws heavily from his own experiences of battling adversity in the form of cancer—of which he died, before this book’s publication. A poignant reminder that he was right: we won’t always get the most positive outcome of any given situation, so what matters the most is making the best use of the time we have.
Share This Post
-
Do Try This At Home: The 12-Week Brain Fitness Program
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
12 Weeks To Measurably Boost Your Brain
This is Dr. Majid Fotuhi. From humble beginnings (being smuggled out of Iran in 1980 to avoid death in the war), he went on (after teaching himself English, French, and German, hedging his bets as he didn’t know for sure where life would lead him) to get his MD from Harvard Medical School and his PhD in neuroscience from Johns Hopkins University. Since then, he’s had a decades-long illustrious career in neurology and neurophysiology.
What does he want us to know?
The Brain Fitness Program
This is not, by the way, something he’s selling. Rather, it was a landmark 12-week study in which 127 people aged 60–80, of which 63% female, all with a diagnosis of mild cognitive impairment, underwent an interventional trial—in other words, a 12-week brain fitness course.
After it, 84% of the participants showed statistically significant improvements in cognitive function.
Not only that, but of those who underwent MRI testing before and after (not possible for everyone due to practical limitations), 71% showed either no further deterioration of the hippocampus, or actual growth above the baseline volume of the hippocampus (that’s good, and it means functionally the memory center of the brain has been rejuvenated).
You can read a little more about the study here:
As for what the program consisted of, and what Dr. Fotuhi thus recommends for everyone…
Cognitive stimulation
This is critical, so we’re going to spend most time on this one—the others we can give just a quick note and a pointer.
In the study this came in several forms and had the benefit of neurofeedback technology, but he says we can replicate most of the effects by simply doing something cognitively stimulating. Whatever challenges your brain is good, but for maximum effect, it should involve the language faculties of the brain, since these are what tend to get hit most by age-related cognitive decline, and are also what tends to have the biggest impact on life when lost.
If you lose your keys, that’s an inconvenience, but if you can’t communicate what is distressing you, or understand what someone is explaining to you, that’s many times worse—and that kind of thing is a common reality for many people with dementia.
To keep the lights brightly lit in that part of the brain: language-learning is good, at whatever level suits you personally. In other words: there’s a difference between entry-level Duolingo Spanish, and critically analysing Rumi’s poetry in the original Persian, so go with whatever is challenging and/but accessible for you—just like you wouldn’t go to the gym for the first time and try to deadlift 500lbs, but you also probably wouldn’t do curls with the same 1lb weights every day for 10 years.
In other words: progressive overloading is key, for the brain as well as for muscles. Start easy, but if you’re breezing through everything, it’s time to step it up.
If for some reason you’re really set against the idea of learning another language, though, check out:
Reading As A Cognitive Exercise ← there are specific tips here for ensuring your reading is (and remains) cognitively beneficial
Mediterranean diet
Shocking nobody, this is once again recommended. You might like to check out the brain-healthy “MIND” tweak to it, here:
Four Ways To Upgrade The Mediterranean Diet ← it’s the fourth one
Omega-3 supplementation
Nothing complicated here. The brain needs a healthy balance of these fatty acids to function properly, and most people have an incorrect balance (too little omega-3 for the omega-6 present):
What Omega-3 Fatty Acids Really Do For Us ← scroll to “against cognitive decline”
Increasing fitness
There’s a good rule of thumb: what’s healthy for your heart, is healthy for your brain. This is because, like every other organ in your body, the brain does not function well without good circulation bringing plenty of oxygen and nutrients, which means good cardiovascular health is necessary. The brain is extra sensitive to this because it’s a demanding organ in terms of how much stuff it needs delivering via blood, and also because of the (necessary; we’d die quickly and horribly without it) impediment of the blood-brain barrier, and the possibility of beta-amyloid plaques and similar woes (they will build up if circulation isn’t good).
How To Reduce Your Alzheimer’s Risk ← number two on the list here
Practising mindfulness medication
This is also straightforward, but not to be underestimated or skipped over:
No-Frills, Evidence-Based Mindfulness
Want to step it up? Check out:
Meditation Games That You’ll Actually Enjoy
Lastly…
Dr. Fotuhi wants us to consider looking after our brain the same way we look after our teeth. No, he doesn’t want us to brush our brain, but he does want us to take small measurable actions multiple times per day, every day.
You can’t just spend the day doing nothing but brushing your teeth for the entirety of January the 1st and then expect them to be healthy for the rest of the year; it doesn’t work like that—and it doesn’t work like that for the brain, either.
So, make the habits, and keep them going
Take care!
Share This Post
Related Posts
-
Traveling To Die: The Latest Form of Medical Tourism
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In the 18 months after Francine Milano was diagnosed with a recurrence of the ovarian cancer she thought she’d beaten 20 years ago, she traveled twice from her home in Pennsylvania to Vermont. She went not to ski, hike, or leaf-peep, but to arrange to die.
“I really wanted to take control over how I left this world,” said the 61-year-old who lives in Lancaster. “I decided that this was an option for me.”
Dying with medical assistance wasn’t an option when Milano learned in early 2023 that her disease was incurable. At that point, she would have had to travel to Switzerland — or live in the District of Columbia or one of the 10 states where medical aid in dying was legal.
But Vermont lifted its residency requirement in May 2023, followed by Oregon two months later. (Montana effectively allows aid in dying through a 2009 court decision, but that ruling doesn’t spell out rules around residency. And though New York and California recently considered legislation that would allow out-of-staters to secure aid in dying, neither provision passed.)
Despite the limited options and the challenges — such as finding doctors in a new state, figuring out where to die, and traveling when too sick to walk to the next room, let alone climb into a car — dozens have made the trek to the two states that have opened their doors to terminally ill nonresidents seeking aid in dying.
At least 26 people have traveled to Vermont to die, representing nearly 25% of the reported assisted deaths in the state from May 2023 through this June, according to the Vermont Department of Health. In Oregon, 23 out-of-state residents died using medical assistance in 2023, just over 6% of the state total, according to the Oregon Health Authority.
Oncologist Charles Blanke, whose clinic in Portland is devoted to end-of-life care, said he thinks that Oregon’s total is likely an undercount and he expects the numbers to grow. Over the past year, he said, he’s seen two to four out-of-state patients a week — about one-quarter of his practice — and fielded calls from across the U.S., including New York, the Carolinas, Florida, and “tons from Texas.” But just because patients are willing to travel doesn’t mean it’s easy or that they get their desired outcome.
“The law is pretty strict about what has to be done,” Blanke said.
As in other states that allow what some call physician-assisted death or assisted suicide, Oregon and Vermont require patients to be assessed by two doctors. Patients must have less than six months to live, be mentally and cognitively sound, and be physically able to ingest the drugs to end their lives. Charts and records must be reviewed in the state; neglecting to do so constitutes practicing medicine out of state, which violates medical licensing requirements. For the same reason, the patients must be in the state for the initial exam, when they request the drugs, and when they ingest them.
State legislatures impose those restrictions as safeguards — to balance the rights of patients seeking aid in dying with a legislative imperative not to pass laws that are harmful to anyone, said Peg Sandeen, CEO of the group Death With Dignity. Like many aid-in-dying advocates, however, she said such rules create undue burdens for people who are already suffering.
Diana Barnard, a Vermont palliative care physician, said some patients cannot even come for their appointments. “They end up being sick or not feeling like traveling, so there’s rescheduling involved,” she said. “It’s asking people to use a significant part of their energy to come here when they really deserve to have the option closer to home.”
Those opposed to aid in dying include religious groups that say taking a life is immoral, and medical practitioners who argue their job is to make people more comfortable at the end of life, not to end the life itself.
Anthropologist Anita Hannig, who interviewed dozens of terminally ill patients while researching her 2022 book, “The Day I Die: The Untold Story of Assisted Dying in America,” said she doesn’t expect federal legislation to settle the issue anytime soon. As the Supreme Court did with abortion in 2022, it ruled assisted dying to be a states’ rights issue in 1997.
During the 2023-24 legislative sessions, 19 states (including Milano’s home state of Pennsylvania) considered aid-in-dying legislation, according to the advocacy group Compassion & Choices. Delaware was the sole state to pass it, but the governor has yet to act on it.
Sandeen said that many states initially pass restrictive laws — requiring 21-day wait times and psychiatric evaluations, for instance — only to eventually repeal provisions that prove unduly onerous. That makes her optimistic that more states will eventually follow Vermont and Oregon, she said.
Milano would have preferred to travel to neighboring New Jersey, where aid in dying has been legal since 2019, but its residency requirement made that a nonstarter. And though Oregon has more providers than the largely rural state of Vermont, Milano opted for the nine-hour car ride to Burlington because it was less physically and financially draining than a cross-country trip.
The logistics were key because Milano knew she’d have to return. When she traveled to Vermont in May 2023 with her husband and her brother, she wasn’t near death. She figured that the next time she was in Vermont, it would be to request the medication. Then she’d have to wait 15 days to receive it.
The waiting period is standard to ensure that a person has what Barnard calls “thoughtful time to contemplate the decision,” although she said most have done that long before. Some states have shortened the period or, like Oregon, have a waiver option.
That waiting period can be hard on patients, on top of being away from their health care team, home, and family. Blanke said he has seen as many as 25 relatives attend the death of an Oregon resident, but out-of-staters usually bring only one person. And while finding a place to die can be a problem for Oregonians who are in care homes or hospitals that prohibit aid in dying, it’s especially challenging for nonresidents.
When Oregon lifted its residency requirement, Blanke advertised on Craigslist and used the results to compile a list of short-term accommodations, including Airbnbs, willing to allow patients to die there. Nonprofits in states with aid-in-dying laws also maintain such lists, Sandeen said.
Milano hasn’t gotten to the point where she needs to find a place to take the meds and end her life. In fact, because she had a relatively healthy year after her first trip to Vermont, she let her six-month approval period lapse.
In June, though, she headed back to open another six-month window. This time, she went with a girlfriend who has a camper van. They drove six hours to cross the state border, stopping at a playground and gift shop before sitting in a parking lot where Milano had a Zoom appointment with her doctors rather than driving three more hours to Burlington to meet in person.
“I don’t know if they do GPS tracking or IP address kind of stuff, but I would have been afraid not to be honest,” she said.
That’s not all that scares her. She worries she’ll be too sick to return to Vermont when she is ready to die. And, even if she can get there, she wonders whether she’ll have the courage to take the medication. About one-third of people approved for assisted death don’t follow through, Blanke said. For them, it’s often enough to know they have the meds — the control — to end their lives when they want.
Milano said she is grateful she has that power now while she’s still healthy enough to travel and enjoy life. “I just wish more people had the option,” she said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Long-acting contraceptives seem to be as safe as the pill when it comes to cancer risk
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
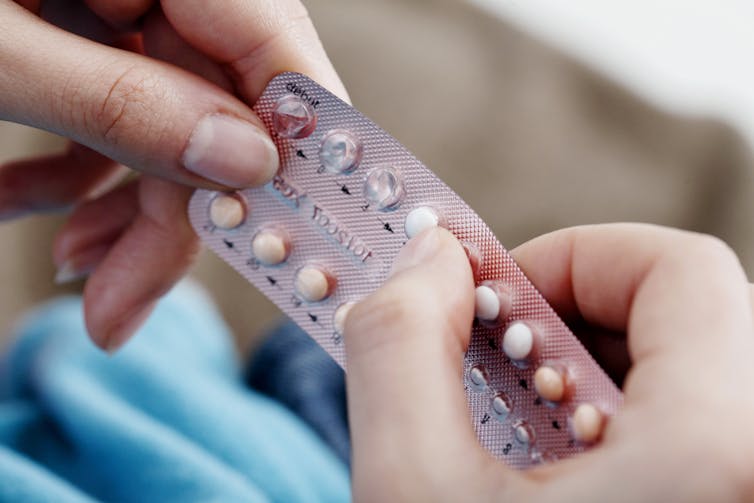
Many women worry hormonal contraceptives have dangerous side-effects including increased cancer risk. But this perception is often out of proportion with the actual risks.
So, what does the research actually say about cancer risk for contraceptive users?
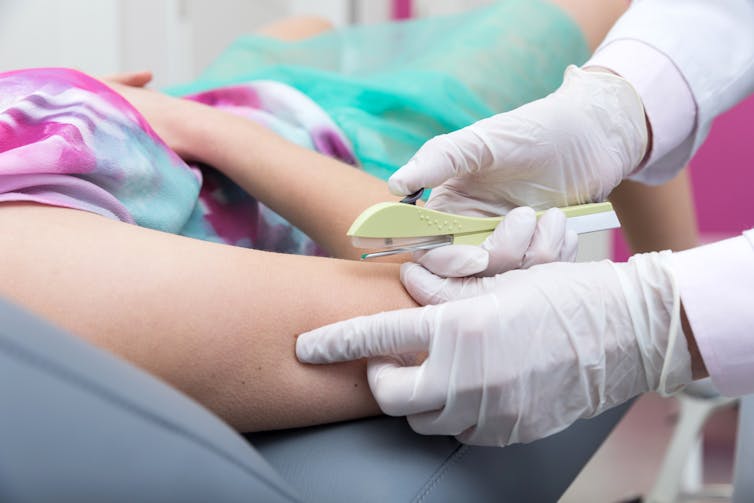
And is your cancer risk different if, instead of the pill, you use long-acting reversible contraceptives? These include intrauterine devices or IUDs (such as Mirena), implants under the skin (such as Implanon), and injections (such as Depo Provera).
Our new study, conducted by the University of Queensland and QIMR Berghofer Medical Research Institute and published by the Journal of the National Cancer Institute, looked at this question.
We found long-acting contraceptives seem to be as safe as the pill when it comes to cancer risk (which is good news) but not necessarily any safer than the pill.
Peakstock/Shutterstock Some hormonal contraceptives take the form of implants under the skin. WiP-Studio/Shutterstock How does the contraceptive pill affect cancer risk?
The International Agency for Research on Cancer, which compiles evidence on cancer causes, has concluded that oral contraceptives have mixed effects on cancer risk.
Using the oral contraceptive pill:
- slightly increases your risk of breast and cervical cancer in the short term, but
- substantially reduces your risk of cancers of the uterus and ovaries in the longer term.
Our earlier work showed the pill was responsible for preventing far more cancers overall than it contributed to.
In previous research we estimated that in 2010, oral contraceptive pill use prevented over 1,300 cases of endometrial and ovarian cancers in Australian women.
It also prevented almost 500 deaths from these cancers in 2013. This is a reduction of around 25% in the deaths that could have occurred that year if women hadn’t taken the pill.
In contrast, we calculated the pill may have contributed to around 15 deaths from breast cancer in 2013, which is less than 0.5% of all breast cancer deaths in that year.
Previous work showed the pill was responsible for preventing far more cancers overall than it contributed to. Image Point Fr What about long-acting reversible contraceptives and cancer risk?
Long-acting reversible contraceptives – which include intrauterine devices or IUDs, implants under the skin, and injections – release progesterone-like hormones.
These are very effective contraceptives that can last from a few months (injections) up to seven years (intrauterine devices).
Notably, they don’t contain the hormone oestrogen, which may be responsible for some of the side-effects of the pill (including perhaps contributing to a higher risk of breast cancer).
Use of these long-acting contraceptives has doubled over the past decade, while the use of the pill has declined. So it’s important to know whether this change could affect cancer risk for Australian women.
Our new study of more than 1 million Australian women investigated whether long-acting, reversible contraceptives affect risk of invasive cancers. We compared the results to the oral contraceptive pill.
We used de-identified health records for Australian women aged 55 and under in 2002.
Among this group, about 176,000 were diagnosed with cancer between 2004 and 2013 when the oldest women were aged 67. We compared hormonal contraceptive use among these women who got cancer to women without cancer.
We found that long-term users of all types of hormonal contraception had around a 70% lower risk of developing endometrial cancer in the years after use. In other words, the risk of developing endometrial cancer is substantially lower among women who took hormonal contraception compared to those who didn’t.
For ovarian cancer, we saw a 50% reduced risk (compared to those who took no hormonal contraception) for women who were long-term users of the hormone-containing IUD.
The risk reduction was not as marked for the implants or injections, however few long-term users of these products developed these cancers in our study.
As the risk of endometrial and ovarian cancers increases with age, it will be important to look at cancer risk in these women as they get older.
What about breast cancer risk?
Our findings suggest that the risk of breast cancer for current users of long-acting contraceptives is similar to users of the pill.
However, the contraceptive injection was only associated with an increase in breast cancer risk after five years of use and there was no longer a higher risk once women stopped using them.
Our results suggested that the risk of breast cancer also reduces after stopping use of the contraceptive implants.
We will need to follow-up the women for longer to determine whether this is also the case for the IUD.
It is worth emphasising that the breast cancer risk associated with all hormonal contraceptives is very small.
About 30 in every 100,000 women aged 20 to 39 years develop breast cancer each year, and any hormonal contraceptive use would only increase this to around 36 cases per 100,000.
What about other cancers?
Our study did not show any consistent relationships between contraceptive use and other cancers types. However, we only at looked at invasive cancers (meaning those that start at a primary site but have the potential to spread to other parts of the body).
A recent French study found that prolonged use of the contraceptive injection increased the risk of meningioma (a type of benign brain tumour).
However, meningiomas are rare, especially in young women. There are around two cases in every 100,000 in women aged 20–39, so the extra number of cases linked to contraceptive injection use was small.
The French study found the hormonal IUD did not increase meningioma risk (and they did not investigate contraceptive implants).
Benefits and side-effects
There are benefits and side-effects for all medicines, including contraceptives, but it is important to know most very serious side-effects are rare.
A conversation with your doctor about the balance of benefits and side-effects for you is always a good place to start.
Susan Jordan, Professor of Epidemiology, The University of Queensland; Karen Tuesley, Postdoctoral Research Fellow, School of Public Health, The University of Queensland, and Penny Webb, Distinguished Scientist, Gynaecological Cancers Group, QIMR Berghofer Medical Research Institute
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Lower Your Cortisol! (Here’s Why & How)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Cortisol, or “the stress hormone” to its friends, is produced by your adrenal glands, and is generally considered “not fun”.
It does serve a purpose, of course, just like almost everything else our body does. It serves as part of the “fight or flight” response, for example, and helps you to wake up in the morning.
While you do need some cortisol (and a small percentage of people have too little), most of us have too much.
Why? Simply put, modern life is not what 200,000* years of human evolution prepared us for:
- Agriculture (which allowed us to settle down and cease being nomadic) happened during the last 6% of those 200,000 years.
- The Industrial Revolution and the onset of modern capitalism happened during only during the last 0.1% of those 200,000 years.
*the 200,000 years figure is conservative and doesn’t take into account the 200,000,000 years of pre-hominid mammalian evolution. Doing so, on the basis of the mammalian brain & physiology being what’s important here, means our modern stressors have been around for <0.0001% of the time we have.
So guess what, our bodies haven’t caught up. As far as our bodies are concerned, we are supposed to be enjoying the sunshine of grassy plains and the shade of woodland while eating fruit.
- When the alarm clock goes off, our body panics and prepares us to either flee or help fight the predator, because why else would we have been woken so?
- When we have a pressing deadline for work, our brain processes this as “if we don’t do this, we will literally starve and die”.
- When people are upset or angry with us, there’s a part of our brain that fears exile from the tribe and resultant death.
…and so on.
Health Risks of High Cortisol
The long-term stressors are the biggest issue for health. Unless you have a heart condition or other relevant health problem, almost anyone can weather a brief unpleasant surprise. But if something persists? That prompts the body to try to protect you, bless it. The body’s attempts backfire, because…
- One way it does this by making sure to save as much food as possible in the form of body fat
- It’ll also increase your appetite, to make sure you eat anything you can while you still can
- It additionally tries to protect you by keeping you on the brink of fight-or-flight readiness, e.g:
- High blood pressure
- High blood sugar levels
- Rapid mood changes—gotta be able to do those heel-turns as necessary and react quickly to any possible threat!
Suffice it to say, these things are not good for your long-term health.
That’s the “Why”—now here’s the “How”:
Lowering your cortisol levels mostly means lowering your stress and/or lowering your stress response. We previously gave some powerful tools for lowering anxiety, which for these purposes amounts to the same thing.
However, we can also make nutritional and lifestyle changes that will reduce our cortisol levels, for example:
- Reduce (ideally: eliminate from your lifestyle) caffeine
- Reduce (ideally: eliminate from your lifestyle) alcohol
- Yes, really. While many understandably turn to alcohol specifically to help manage stress, it only makes it worse long-term.
- Additionally, alcohol directly stimulates cortisol production, counterintuitive as that may be.
Read: Alcohol, Aging, and the Stress Response ← full article (with 37 sources of its own) from the NYMC covering how alcohol stimulates cortisol production and what that means for us
As well as reductions/eliminations, are some things you can add into your lifestyle that will help!
We’ve written previously about some:
Read: Ashwagandha / Read: L-Theanine / Read: CBD Oil
Other things include, no surprises here:
- The Mediterranean diet (nutritious and delicious): https://10almonds.com/mediterranean-diet
- Get 7–9 hours (good quality!) sleep per night: https://10almonds.com/time-pillow-talk
- Get regular exercise (the regularity matters most!): https://10almonds.com/keep-on-keeping-on
Progressive Relaxation
We’ll give this one its own section because we’ve not talked about it before. Maybe you’re familiar. If not, then in a nutshell: progressive relaxation means progressively tensing and then relaxing each part of your body in turn.
Why does this work? Part of it is just a physical trick involving biofeedback and the natural function of muscles to contract and relax in turn, but the other part is even cleverer:
It basically tricks the most primitive part of your brain, the limbic system, into thinking you had a fight and won, telling it “thank you very much for the cortisol but we don’t need it anymore”.
Take a Hike! Or a Stroll… You Do You!
Last but not least: go connect with your roots. Spend time in the park, or at least the garden. Have a picnic, if the weather suits. Go somewhere you can spend time around leafy green things under a blue sky (we realize the blue sky may be subject to availability in some locations, but do what you can!).
Remember also: just as your body’s responses will be tricked by the alarm clock or the housework, they will also be easily tricked by blue and green stuff around you. If a sunny garden isn’t available in your location, a picture of one as your desktop background is the next best thing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: