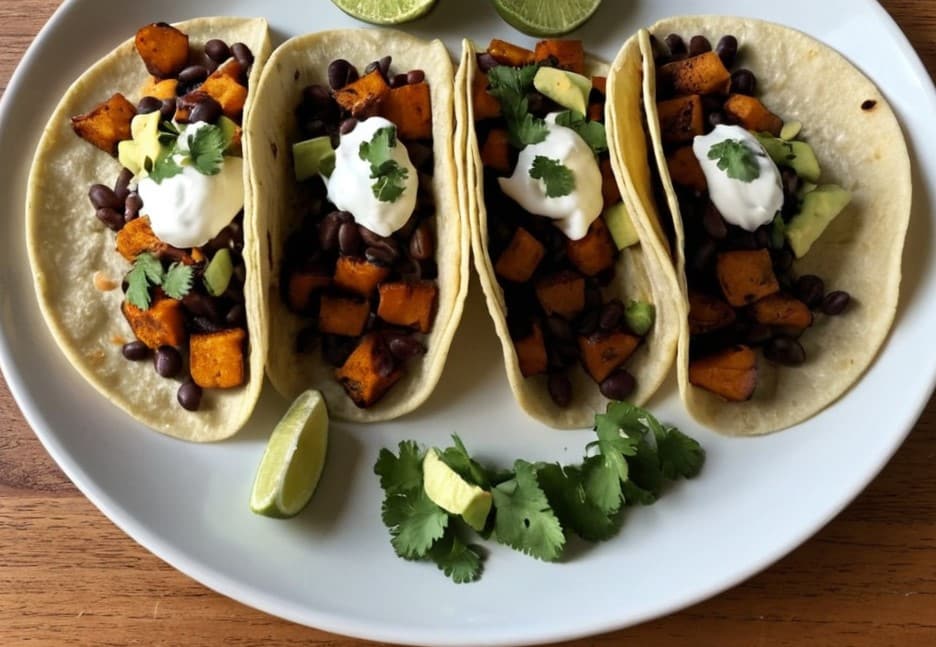Two Things You Can Do To Improve Stroke Survival Chances
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Andrew’s Stroke Survival Guide

This is Dr. Nadine Andrew. She’s a Senior Research Fellow in the Department of Medicine at Monash University. She’s the Research Data Lead for the National Center of Healthy Aging. She is lead investigator on the NHMRC-funded PRECISE project… The most comprehensive stroke data linkage study to date! In short, she knows her stuff.
We’ve talked before about how sample size is important when it comes to scientific studies. It’s frustrating; sometimes we see what looks like a great study until we notice it has a sample size of 17 or something.
Dr. Andrew didn’t mess around in this regard, and the 12,386 participants in her Australian study of stroke patients provided a huge amount of data!
With a 95% confidence interval because of the huge dataset, she found that there was one factor that reduced mortality by 26%.
And the difference was…
Whether or not patients had a chronic disease management plan set up with their GP (General Practitioner, or “family doctor”, in US terms), after their initial stroke treatment.
45% of patients had this; the other 55% did not, so again the sample size was big for both groups.
Why this is important:
After a stroke, often a patient is discharged as early as it seems safe to do so, and there’s a common view that “it just takes time” and “now we wait”. After all, no medical technology we currently have can outright repair that damage—the body must repair itself! Medications—while critical*—can only support that and help avoid recurrence.
*How critical? VERY critical. Critical critical. Dr. Andrew found, some years previously, that greater levels of medication adherence (ie, taking the correct dose on time and not missing any) significantly improved survival outcomes. No surprise, right? But what may surprise is that this held true even for patients with near-perfect adherence. In other words: miss a dose at your peril. It’s that important.
But, as Dr. Andrew’s critical research shows, that’s no reason to simply prescribe ongoing meds and otherwise cut a patient loose… or, if you or a loved one are the patient, to allow yourself/them to be left without a doctor’s ongoing active support in the form of a chronic disease management plan.
What does a chronic disease management plan look like?
First, what it’s not:
- “Yes yes, I’m here if you need me, just make an appointment if something changes”
- “Let’s pencil in a check-up in three months”
- Etc
What it actually looks like:
It looks like a plan. A personal care plan, built around that person’s individual needs, risks, liabilities… and potential complications.
Because who amongst us, especially at the age where strokes are more likely, has an uncomplicated medical record? There will always be comorbidities and confounding factors, so a one-size-fits-all plan will not do.
Dr. Andrew’s work took place in Australia, so she had the Australian healthcare system in mind… We know many of our subscribers are from North America and other places. But read this, and you’ll see how this could go just as much for the US or Canada:
❝The evidence shows the importance of Medicare financially supporting primary care physicians to provide structured chronic disease management after a stroke.
We also provide a strong case for the ongoing provision of these plans within a universal healthcare system. Strategies to improve uptake at the GP level could include greater financial incentives and mandates, education for patients and healthcare professionals.❞
See her groundbreaking study for yourself here!
The Bottom Line:
If you or a loved one has a stroke, be prepared to make sure you get a chronic health management plan in place. Note that if it’s you who has the stroke, you might forget this or be unable to advocate for yourself. So, we recommend to discuss this with a partner or close friend sooner rather than later!
“But I’m quite young and healthy and a stroke is very unlikely for me”
Good for you! And the median age of Dr. Andrew’s gargantuan study was 70 years. But:
- do you have older relatives? Be aware for them, too.
- strokes can happen earlier in life too! You don’t want to be an interesting statistic.
Some stroke-related quick facts:
Stroke is the No. 5 cause of death and a leading cause of disability in the U.S.
Stroke can happen to anyone—any age, any time—and everyone needs to know the warning signs.
On average, 1.9 million brain cells die every minute that a stroke goes untreated.
Stroke is an EMERGENCY. Call 911 immediately.
Early treatment leads to higher survival rates and lower disability rates. Calling 911 lets first responders start treatment on someone experiencing stroke symptoms before arriving at the hospital.
Source: https://www.stroke.org/en/about-stroke
What are the warning signs for stroke?
Use the letters F.A.S.T. to spot a stroke and act quickly:
- F = Face Drooping—does one side of the face droop or is it numb? Ask the person to smile. Is the person’s smile uneven?
- A = Arm Weakness—is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward?
- S = Speech Difficulty—is speech slurred?
- T = Time to call 911
Source: https://www.stroke.org/en/about-stroke/stroke-symptoms
Last but not least, while we’re sharing resources:
Download the PDF Checklist: 8 Ways To Help Prevent a Second Stroke
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Increase Your Muscle Mass Boost By 26% (No Extra Effort, No Supplements)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You’ve probably seen this technology advertised, but the trick is in how it’s used (which is not how most people use it).
It’s about neuromuscular electrical stimulation (NMES), also called electrical muscle stimulation (EMS); in other words, those squid-like electrode kits that promise “six-pack abs without exercise”, by stimulating the muscles for you—using the exact same tech as for transcutaneous electrical nerve stimulation (TENS), for pain relief.
Do they work for pain relief? Yes, for many people in any case. But that’s beyond the scope of today’s article.
Do they work for building muscles as advertised? No. The limiting factor is that they can’t fully exert the muscles in the same way actual exercise can, because of the limitations to how much electrical current can safely be applied.
However…
The cyborgization of your regular workout
A meta-analysis of 13 studies compared two [meta-]groups of exercisers:
- Group 1 doing conventional resistance training
- Group 2 doing the same resistance training, plus NMES at the same time (specifically: NMES of the same muscles being used in the workout)
The analysis had two output variables: strength and muscle mass
What they found: group 2 enjoyed more than 31% greater strength gains, and 26% greater muscle mass gains, from the same training over the same period of time.
Of course, one of the biggest challenges to strength gain and muscle mass gain is hitting a plateau, so it’s worth noting that when they looked at training periods ranging from 2 weeks to 16 weeks, longer durations yielded better results—it is, it seems, the gift that keeps on giving.
You can find the paper here (which also explains how they analysed data from 13 different studies to get one coherent set of results):
How it works and why it matters
While the paper itself does not go into how it works, a reasonable hypothesis is that it works by “confusing” the muscles—because they are receiving mixed signals (one set from your brain, one set from the electrodes), with fast- and slow-twitch muscle fibers both working at the same time.
Another way to “confuse” the muscles is by High Intensity [Interval] Resistance Training (HIRT)—which is basically High Intensity Interval Training (HIIT), but for resistance training specifically.
See: How To Do HIIT (Without Wrecking Your Body) and HIIT, But Make It HIRT
Now, we want to confuse our muscles, not our readers, so if that’s all too much to juggle at once, just pick one and go with it. But today’s article is about the RT+NEMS combination, so perhaps you’ll pick that.
Why it matters: as we get older, sarcopenia (the loss of muscle mass) becomes more of an issue, and even if we’re not inclined to a career in bodybuilding, we do still need to at least maintain a healthy muscle mass because:
- Strong muscles improve our stability and make us less likely to fall
- Strong muscles force the body to build strong bones to hold them on, which means lower risk of fractures or worse
- Muscle mass itself improves the body’s basal metabolic rate, which means systemic benefits to the whole body (including against metabolic diseases especially)
See also: Resistance Is Useful! (Especially As We Get Older)
Want to try it?
If you don’t already have a NMES/EMS/TENS kit lying around the house, here’s an example product on Amazon—remember to use it simultaneously with your regular resistance training workout, on the same muscles at the same time, to get the benefit we talked about! 😎
Enjoy!
Share This Post
-
Rainbow Roasted Potato Salad
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This salad has potatoes in it, but it’s not a potato salad as most people know it. The potatoes are roasted, but in a non-oily-dressing, that nevertheless leaves them with an amazing texture—healthy and delicious; the best of both worlds. And the rest? We’ve got colorful vegetables, we’ve got protein, we’ve got seasonings full of healthy spices, and more.
You will need
- 1½ lbs new potatoes (or any waxy potatoes; sweet potato is also a great option; don’t peel them, whichever you choose) cut into 1″ chunks
- 1 can / 1 cup cooked cannellini beans (or your preferred salad beans)
- 1 carrot, grated
- 2 celery stalks, finely chopped
- 3 spring onions, finely chopped
- ½ small red onion, finely sliced
- 2 tbsp white wine vinegar
- 1 tbsp balsamic vinegar
- 1 tbsp lemon juice
- 1 tbsp nutritional yeast
- 1 tsp garlic powder
- 1 tsp black pepper
- ½ tsp red chili powder
- We didn’t forget salt; it’s just that with the natural sodium content of the potatoes plus the savory flavor-enhancing properties of the nutritional yeast, it’s really not needed here. Add if you feel strongly about it, opting for low-sodium salt, or MSG (which has even less sodium).
- To serve: 1 cup basil pesto (we’ll do a recipe one of these days; meanwhile, store-bought is fine, or you can use the chermoula we made the other day, ignoring the rest of that day’s recipe and just making the chermoula component)
Method
(we suggest you read everything at least once before doing anything)
1) Preheat the oven as hot as it goes!
2) Combine the potatoes, white wine vinegar, nutritional yeast, garlic powder, black pepper, and red chili powder, mixing thoroughly (but gently!) to coat.
3) Spread the potatoes on a baking tray, and roast in the middle of the oven (for best evenness of cooking); because of the small size of the potato chunks, this should only take about 25 minutes (±5mins depending on your oven); it’s good to turn them halfway through, or at least jiggle them if you don’t want to do all that turning.
4) Allow to cool while still on the baking tray (this allows the steam to escape immediately, rather than the steam steaming the other potatoes, as it would if you put them in a bowl).
5) Now put them in a serving bowl, and mix in the beans, vegetables, balsamic vinegar, and lemon juice, mixing thoroughly but gently
6) Add generous lashings of the pesto to serve; it should be gently mixed a little too, so that it’s not all on top.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- White Potato vs Sweet Potato – Which is Healthier?
- Eat More (Of This) For Lower Blood Pressure
- Our Top 5 Spices: How Much Is Enough For Benefits?
Take care!
Share This Post
-
4 things ancient Greeks and Romans got right about mental health
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
According to the World Health Organization, about 280 million people worldwide have depression and about one billion have a mental health problem of any kind.
People living in the ancient world also had mental health problems. So, how did they deal with them?
As we’ll see, some of their insights about mental health are still relevant today, even though we might question some of their methods.
Jr Morty/Shutterstock 1. Our mental state is important
Mental health problems such as depression were familiar to people in the ancient world. Homer, the poet famous for the Iliad and Odyssey who lived around the eighth century BC, apparently died after wasting away from depression.
Already in the late fifth century BC, ancient Greek doctors recognised that our health partly depends on the state of our thoughts.
In the Epidemics, a medical text written in around 400BC, an anonymous doctor wrote that our habits about our thinking (as well as our lifestyle, clothing and housing, physical activity and sex) are the main determinants of our health.
Homer, the ancient Greek poet, had depression. Thirasia/Shutterstock 2. Mental health problems can make us ill
Also writing in the Epidemics, an anonymous doctor described one of his patients, Parmeniscus, whose mental state became so bad he grew delirious, and eventually could not speak. He stayed in bed for 14 days before he was cured. We’re not told how.
Later, the famous doctor Galen of Pergamum (129-216AD) observed that people often become sick because of a bad mental state:
It may be that under certain circumstances ‘thinking’ is one of the causes that bring about health or disease because people who get angry about everything and become confused, distressed and frightened for the slightest reason often fall ill for this reason and have a hard time getting over these illnesses.
Galen also described some of his patients who suffered with their mental health, including some who became seriously ill and died. One man had lost money:
He developed a fever that stayed with him for a long time. In his sleep he scolded himself for his loss, regretted it and was agitated until he woke up. While he was awake he continued to waste away from grief. He then became delirious and developed brain fever. He finally fell into a delirium that was obvious from what he said, and he remained in this state until he died.
3. Mental illness can be prevented and treated
In the ancient world, people had many different ways to prevent or treat mental illness.
The philosopher Aristippus, who lived in the fifth century BC, used to advise people to focus on the present to avoid mental disturbance:
concentrate one’s mind on the day, and indeed on that part of the day in which one is acting or thinking. Only the present belongs to us, not the past nor what is anticipated. The former has ceased to exist, and it is uncertain if the latter will exist.
The philosopher Clinias, who lived in the fourth century BC, said that whenever he realised he was becoming angry, he would go and play music on his lyre to calm himself.
Doctors had their own approaches to dealing with mental health problems. Many recommended patients change their lifestyles to adjust their mental states. They advised people to take up a new regime of exercise, adopt a different diet, go travelling by sea, listen to the lectures of philosophers, play games (such as draughts/checkers), and do mental exercises equivalent to the modern crossword or sudoku.
Galen, a famous doctor, believed mental problems were caused by some idea that had taken hold of the mind. Pierre Roche Vigneron/Wikimedia For instance, the physician Caelius Aurelianus (fifth century AD) thought patients suffering from insanity could benefit from a varied diet including fruit and mild wine.
Doctors also advised people to take plant-based medications. For example, the herb hellebore was given to people suffering from paranoia. However, ancient doctors recognised that hellebore could be dangerous as it sometimes induced toxic spasms, killing patients.
Other doctors, such as Galen, had a slightly different view. He believed mental problems were caused by some idea that had taken hold of the mind. He believed mental problems could be cured if this idea was removed from the mind and wrote:
a person whose illness is caused by thinking is only cured by taking care of the false idea that has taken over his mind, not by foods, drinks, [clothing, housing], baths, walking and other such (measures).
Galen thought it was best to deflect his patients’ thoughts away from these false ideas by putting new ideas and emotions in their minds:
I put fear of losing money, political intrigue, drinking poison or other such things in the hearts of others to deflect their thoughts to these things […] In others one should arouse indignation about an injustice, love of rivalry, and the desire to beat others depending on each person’s interest.
4. Addressing mental health needs effort
Generally speaking, the ancients believed keeping our mental state healthy required effort. If we were anxious or angry or despondent, then we needed to do something that brought us the opposite of those emotions.
Watch some comedy, said physician Caelius Aurelianus. VCU Tompkins-McCaw Library/Flickr, CC BY-NC-SA This can be achieved, they thought, by doing some activity that directly countered the emotions we are experiencing.
For example, Caelius Aurelianus said people suffering from depression should do activities that caused them to laugh and be happy, such as going to see a comedy at the theatre.
However, the ancients did not believe any single activity was enough to make our mental state become healthy. The important thing was to make a wholesale change to one’s way of living and thinking.
When it comes to experiencing mental health problems, we clearly have a lot in common with our ancient ancestors. Much of what they said seems as relevant now as it did 2,000 years ago, even if we use different methods and medicines today.
If this article has raised issues for you, or if you’re concerned about someone you know, call Lifeline on 13 11 14.
Konstantine Panegyres, McKenzie Postdoctoral Fellow, researching Greco-Roman antiquity, The University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Sweet Potato & Black Bean Tacos
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fiber, protein, and polyphenols! What more could one ask for? Well, great taste and warm healthy goodness, which these deliver:
You will need
For the sweet potatoes:
- 2 medium sweet potatoes, cubed (we recommend leaving the skin on, but you can peel them if you really want to)
- 1 tbsp extra virgin olive oil
- 2 tsp garlic powder
- 2 tsp smoked paprika
- 1 tsp chili powder
- 1 tsp black pepper
- 1 tsp ground cumin
- 1 tsp ground turmeric
- ½ tsp MSG or 1 tsp low-sodium salt
For the black beans:
- 2 cans black beans, drained and rinsed (or 2 cups black beans that you cooked yourself)
- ¼ bulb garlic, minced
- 1 fresh jalapeño finely chopped (or ¼ cup jalapeños from a jar, finely chopped) ← adjust quantities per your preference and per the quality of the pepper(s) you’re using; we can’t judge that from here without tasting them, so we give a good basic starting suggestion.
- 2 tsp black pepper
- 1 tsp red chili flakes
- ½ tsp MSG or 1 tsp low-sodium salt
For serving:
- 8 small corn tortillas, or your preference if substituting
- 1 avocado, pitted, peeled, cubed, and tossed in lime juice ← we’re mentioning this here because you want to do this as soon as you cut it, to avoid oxidation
- Any other salad you’d like to include; fresh parsley is also a good option when it comes to greenery, or cilantro if you don’t have the soap gene
- Tomato salsa (quantity and spice level per your preference)
Method
(we suggest you read everything at least once before doing anything)
1) Preheat the oven to 400°F / 200°C.
2) Toss the sweet potato cubes in a large bowl with the rest of the ingredients from the sweet potato section above, ensuring they are evenly coated.
3) Bake them in the oven, on a baking tray lined with baking paper, for about 30 minutes or until tender inside and crispy at the edges. Turn them over halfway through.
4) While that’s happening, mix the black beans in a bowl with the other ingredients from the black bean section above, and heat them gently. You could do this in a saucepan, but honestly, while it’s not glamorous, the microwave is actually better for this. Note: many people find the microwave cooks food unevenly, but there are two reasons for this and they’re both easily fixable:
- instead of using high power for x minutes, use medium power for 2x minutes; this will produce better results
- instead of putting the food just in a bowl, jug, or similar, use a wide bowl or similar container, and then inside that, place a small empty microwave-safe glass jar or similar upturned in the middle, and then add the food around it, so that the food is arranged in a donut shape rather than a wide cylinder shape. This means there is no “middle bit” to go underheated while the edges are heated excessively; instead, it will heat through evenly.
If you really don’t want to do that though, use a saucepan on a very low heat, add a small amount of liquid (or tomato salsa), and stir constantly.
5) Heat the tortillas in a dry skillet for about 30 seconds each on each side, when ready to serve.
6) Assemble the tacos; you can do this how you like but a good order of operations is: tortilla, leafy salad (if using), potato, beans, non-leafy salad including avocado, salsa or other topping per your preference.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- White Potato vs Sweet Potato – Which is Healthier?
- Kidney Beans or Black Beans – Which is Healthier?
- Coconut vs Avocado – Which is Healthier?
- Glutathione: More Than An Antioxidant
- Our Top 5 Spices: How Much Is Enough For Benefits? ← we hit 4/5 today!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What’s the difference between period pain and endometriosis pain?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
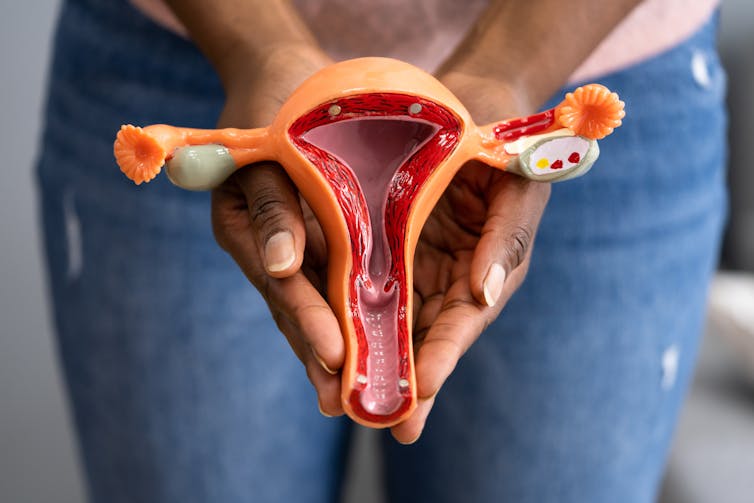
Menstruation, or a period, is the bleeding that occurs about monthly in healthy people born with a uterus, from puberty to menopause. This happens when the endometrium, the tissue that lines the inside of the uterus, is shed.
Endometriosis is a condition that occurs when endometrium-like tissue is found outside the uterus, usually within the pelvic cavity. It is often considered a major cause of pelvic pain.
Pelvic pain significantly impacts quality of life. But how can you tell the difference between period pain and endometriosis?
Polina Zimmerman/Pexels Periods and period pain
Periods involve shedding the 4-6 millimetre-thick endometrial lining from the inside of the uterus.
As the lining detaches from the wall of the uterus, the blood vessels which previously supplied the lining bleed. The uterine muscles contract, expelling the blood and crumbled endometrium.
The crumbled endometrium and blood mostly pass through the cervix and vagina. But almost everyone back-bleeds via their fallopian tubes into their pelvic cavity. This is known as “retrograde menstruation”.
Most of the lining is shed through the vagina. Andrey_Popov/Shutterstock The process of menstrual shedding is caused by inflammatory substances, which also cause nausea, vomiting, diarrhoea, headaches, aches, pains, dizziness, feeling faint, as well as stimulating pain receptors.
These inflammatory substances are responsible for the pain and symptoms in the week before a period and the first few days.
For women with heavy periods, their worst days of pain are usually the heaviest days of their period, coinciding with more cramps to expel clots and more retrograde bleeding.
Many women also have pain when they are releasing an egg from their ovary at the time of ovulation. Ovulation or mid-cycle pain can be worse in those who bleed more, as those women are more likely to bleed into the ovulation follicle.
Around 90% of adolescents experience period pain. Among these adolescents, 20% will experience such severe period pain they need time off from school and miss activities. These symptoms are too often normalised, without validation or acknowledgement.
What about endometriosis?
Many symptoms have been attributed to endometriosis, including painful periods, pain with sex, bladder and bowel-related pain, low back pain and thigh pain.
Other pain-related conditions such migraines and chronic fatigue have also been linked to endometriosis. But these other pain-related symptoms occur equally often in people with pelvic pain who don’t have endometriosis.
One in five adolescents who menstrate experience severe symptoms. CGN089/Shutterstock Repeated, significant period and ovulation pain can eventually lead some people to develop persistent or chronic pelvic pain, which lasts longer than six months. This appears to occur through a process known as central sensitisation, where the brain becomes more sensitive to pain and other sensory stimuli.
Central sensitisation can occur in people with persistent pain, independent of the presence or absence of endometriosis.
Eventually, many people with period and/or persistent pelvic pain will have an operation called a laparoscopy, which allows surgeons to examine organs in the pelvis and abdomen, and diagnose and treat endometriosis.
Yet only 50% of those with identical pain symptoms who undergo a laparoscopy will end up having endometriosis.
Endometriosis is also found in pain-free women. So we cannot predict who does and doesn’t have endometriosis from symptoms alone.
How is this pain managed?
Endometriosis surgery usually involves removing lesions and adhesions. But at least 30% of people return to pre-surgery pain levels within six months or have more pain than before.
After surgery, emergency department presentations for pain are unchanged and 50% have repeat surgery within a few years.
Suppressing periods using hormonal therapies (such as continuous oral contraceptive pills or progesterone-only approaches) can suppress endometriosis and reduce or eliminate pain, independent of the presence or absence of endometriosis.
Not every type or dose of hormonal medications suits everyone, so medications need to be individualised.
The current gold-standard approach to manage persistent pelvic pain involves a multidisciplinary team approach, with the aim of achieving sustained remission and improving quality of life. This may include:
- physiotherapy for pelvic floor and other musculoskeletal problems
- management of bladder and bowel symptoms
- support for self-managing pain
- lifestyle changes including diet and exercise
- psychological or group therapy, as our moods, stress levels and childhood events can affect how we feel and experience pain.
Whether you have period pain, chronic pelvic pain or pain you think is associated with endometriosis, if you feel pain, it’s real. If it’s disrupting your life, you deserve to be taken seriously and treated as the whole person you are.
Sonia R. Grover, Senior Research Fellow, Murdoch Children’s Research Institute; Clinical Professor of Gynaecology, The University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Radical Remission – by Dr. Kelly Turner
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
First, what this is not:an autobiographical account of the “I beat cancer and you can too” pep-talk style.
What it is: a very readable pop-science book based on the author’s own PhD research into radical remission.
She knew that a very small percentage of people experience spontaneous radical remission (or quasi-spontaneous, if the remission is attributed to lifestyle changes, and/or some alternative therapy), but a small percentage of people means a large number worldwide, so she travelled the world studying over 1,000 cases of people with late-stage cancer who had either not gone for conventional anticancer drugs, or had and then stopped, and lived to tell the tale.
While she doesn’t advocate for any particular alternative therapy, she does report on what things came to her attention. She does advocate for some lifestyle changes.
Perhaps the biggest value this book offers is in its promised “9 key factors that can make a real difference”, which are essentially her conclusions from her PhD dissertation.
There isn’t room to talk about them here in a way that wouldn’t be misleading/unhelpful for a paucity of space, so perhaps we’ll do a main feature one of these days.
Bottom line: if you have (or a loved one has) cancer, this is an incredibly sensible book to read. If you don’t, then it’s an interesting and thought-provoking book to read.
Click here to check out Radical Remission, and learn about the factors at hand!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: