Wondering how to spot the signs of postpartum depression?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Postpartum depression, or PPD, is a debilitating, potentially life-threatening mental health condition that impacts about one in eight people who give birth in the U.S. While it’s normal to feel worried or stressed after becoming a parent, PPD can cause feelings of extreme sadness or anxiety that may lead to suicidal thoughts.
Read on to learn what PPD is, what causes it, how it’s treated, and more.
What is the difference between the baby blues and postpartum depression?
Postpartum blues, or the “baby blues,” impact up to 80 percent of new parents. The baby blues may cause bouts of crying, mood swings, anxiety, sadness, reduced concentration, irritability, changes in appetite, and trouble sleeping, but symptoms are fleeting.
“Baby blues are a transient period—hours to a few days—of emotionality that does not impair one’s functioning or cause severe symptoms like suicidality,” says Dr. Jennifer L. Payne, a professor of psychiatry and neurobehavioral sciences at the University of Virginia. “[Postpartum depression] can cause severe symptoms, including suicidality.”
In addition to causing more debilitating symptoms, PPD can last for months.
Some new parents also experience postpartum psychosis, which can cause hallucinations and delusions. However, unlike PPD, postpartum psychosis is rare.
What are the symptoms of postpartum depression?
PPD symptoms may include:
- Feeling depressed, irritable, angry, or hopeless
- Severe mood swings
- Difficulty bonding with your baby
- Withdrawing from family and friends
- Changes in appetite or sleeping patterns
- Extreme fatigue
- Difficulty concentrating
- Anxiety and panic attacks
- Thoughts of harming yourself or your baby
- Thoughts of death or suicide
If you are experiencing symptoms of PPD, Payne recommends seeking help from a primary care provider or obstetrician right away.
“It’s really important—not just for you, but for your baby,” Payne explains. “Babies exposed to significant PPD have slower language development, lower IQs, and more behavioral problems.”
Your health care provider will ask you a series of screening questions to determine if you are experiencing PPD.
What causes postpartum depression?
Research suggests that the drop in hormones that occurs after birth, genetics, and sleep deprivation may contribute to PPD.
You may be at higher risk of developing PPD if you have a history of mental health conditions like depression or bipolar disorder, have relatives who’ve experienced PPD, or experienced stressful events during or after pregnancy.
How is postpartum depression treated?
“PPD is usually treated with antidepressant medications—typically SSRIs and now with the new FDA-approved medication, zuranolone,” says Payne. Therapy has also been shown to help people manage PPD.
Your health care provider can help determine the best treatment options for you and can outline the risks and benefits of taking certain medications while breastfeeding.
For referrals to care, information about local support groups, and other mental health resources for new parents, call the National Maternal Mental Health Hotline or Postpartum Support International. If you are experiencing a mental health emergency, call or text the 988 Suicide & Crisis Lifeline.
Can non-birthing parents have postpartum depression?
New parents who did not give birth, including cisgender men, may experience anxiety, depression, irritability, fatigue, and changes in appetite or sleeping patterns after a partner gives birth.
“Everyone knows that mothers’ hormones change a lot during and after pregnancy,” psychologist Scott Bea said in a 2019 Cleveland Clinic article. “But there’s evidence that fathers also experience real changes in their hormone levels after a baby is born.”
Adoptive parents may also show similar symptoms.
If you or anyone you know is considering suicide or self-harm or is anxious, depressed, upset, or needs to talk, call the Suicide & Crisis Lifeline at 988 or text the Crisis Text Line at 741-741. For international resources, here is a good place to begin.
This article first appeared on Public Good News and is republished here under a Creative Commons license.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Top 10 Causes Of High Blood Pressure
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
As Dr. Frita Fisher explains, these are actually the top 10 known causes of high blood pressure. Number zero on the list would be “primary hypertension”, which means high blood pressure with no clear underlying cause.
Superficially, this feels a little like the sometime practice of writing the catch-all “heart failure” as the cause of death on a death certificate, because yes, that heart sure did stop beating. But in reality, primary hypertension is most likely often caused by such things as unmanaged chronic stress—something that doesn’t show up on most health screenings.
Dr. Fisher’s Top 10
- Thyroid disease: both hyperthyroidism and hypothyroidism can cause high blood pressure.
- Obstructive sleep apnea: characterized by snoring, daytime sleepiness, and headaches, this condition can lead to hypertension.
- Chronic kidney disease: diseases ranging from diabetic nephropathy to renal vascular disease can cause high blood pressure.
- Elevated cortisol levels: conditions like Cushing’s syndrome or disease, which involve high cortisol levels, can lead to hypertension—as can a lifestyle with a lot of chronic stress, but that’s less readily diagnosed as such than something one can tell from a blood test.
- Elevated aldosterone levels: excess aldosterone from the adrenal glands causes the body to retain salt and water, increasing blood pressure, because more stuff = more pressure.
- Brain tumor: tumors that increase intracranial pressure can cause a rise in blood pressure to ensure adequate brain perfusion. In these cases, the hypertension is keeping you alive—unless it kills you first. If this seems like a strange bodily response, remember that our bodily response to an infection is often fever, to kill off the infection which can’t survive at such high temperatures (but neither can we, so it becomes a game of chicken with our life on the line), so sometimes our body does kill us with one thing while trying to save us from another.
- Coarctation of the aorta: this congenital heart defect results in narrowing of the aorta, leading to hypertension, especially in the upper body.
- Pregnancy: pregnancy can either induce or worsen existing hypertension.
- Obesity: excess weight increases blood flow and pressure on arteries, raising the risk of hypertension and associated conditions, e.g. diabetes etc.
- Drugs: certain medications and recreational drugs (including, counterintuitively, alcohol!) can elevate blood pressure.
For more information on each of these, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Hypertension: Factors Far More Relevant Than Salt
Take care!
Share This Post
-
Radishes vs Endives – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing radishes to endives, we picked the endives.
Why?
These are both great, but there’s a clear winner here in every category!
In terms of macros, radishes have more carbs while endives have more fiber and protein.
In the category of vitamins, radishes have more of vitamins B6 and C, while endives have more of vitamins A, B1, B2, B4, B5, B7, B9, E, K, and choline.
When it comes to minerals, things are not less one-sided: radishes have more selenium, while endives have more calcium, copper, iron, magnesium, manganese, phosphorus, potassium, and zinc.
You may be thinking: but what about radishes’ shiny red bit? Doesn’t that usually mean more of something important, like carotenoids or anthocyanins or something? And the answer is that the red pigment in radishes is so thinly-distributed on the exterior that it’s barely there and if we’re looking at values per 100g, it’s a tiny fraction of a tiny fraction.
In both cases, their bitter taste comes mostly from flavonols, of which mostly kaempferol, of which endives have about 20x what radishes have, on average.
All in all, an overwhelming win for endives.
Want to learn more?
You might like to read:
Enjoy Bitter Foods For Your Heart & Brain
Take care!
Share This Post
-
The Brain-Gut Highway: A Two-Way Street
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The Brain-Gut Two-Way Highway
This is Dr. Emeran Mayer. He has the rather niche dual specialty of being a gastroenterologist and a neurologist. He has published over 353 peer reviewed scientific articles, and he’s a professor in the Departments of Medicine, Physiology, and Psychiatry at UCLA. Much of his work has been pioneering medical research into gut-brain interactions.
We know the brain and gut are connected. What else does he want us to know?
First, that it is a two-way interaction. It’s about 90% “gut tells the brain things”, but it’s also 10% “brain tells the gut things”, and that 10% can make more like a 20% difference, if for example we look at the swing between “brain using that 10% communication to tell gut to do things worse” or “brain using that 10% communication to tell gut to do things better”, vs the midpoint null hypothesis of “what the gut would be doing with no direction from the brain”.
For example, if we are experiencing unmanaged chronic stress, that is going to tell our gut to do things that had an evolutionary advantage 20,000–200,000 years ago. Those things will not help us now. We do not need cortisol highs and adrenal dumping because we ate a piece of bread while stressed.
Read more (by Dr. Mayer): The Stress That Evolution Has Not Prepared Us For
With this in mind, if we want to look after our gut, then we can start before we even put anything in our mouths. Dr. Mayer recommends managing stress, anxiety, and depression from the head downwards as well as from the gut upwards.
Here’s what we at 10almonds have written previously on how to manage those things:
- No-Frills, Evidence-Based Mindfulness
- How To Set Anxiety Aside
- The Mental Health First-Aid You’ll Hopefully Never Need
Do eat for gut health! Yes, even if…
Unsurprisingly, Dr. Mayer advocates for a gut-friendly, anti-inflammatory diet. We’ve written about these things before:
…but there’s just one problem:
For some people, such as with IBS, Crohn’s, and colitis, the Mediterranean diet that we (10almonds and Dr. Mayer) generally advocate for, is inaccessible. If you (if you have those conditions) eat as we describe, a combination of the fiber in many vegetables and the FODMAPs* in many fruits, will give you a very bad time indeed.
*Fermentable Oligo-, Di-, Monosaccharides And Polyols
Dr. Mayer has the answer to this riddle, and he’s not just guessing; he and his team did science to it. In a study with hundreds of participants, he measured what happened with adherence (or not) to the Mediterranean diet (or modified Mediterranean diet) (or not), in participants with IBS (or not).
The results and conclusions from that study included:
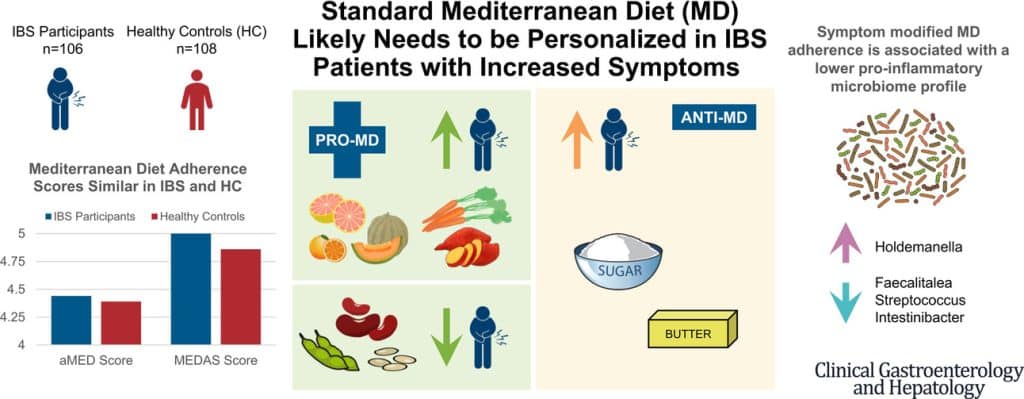
❝Among IBS participants, a higher consumption of fruits, vegetables, sugar, and butter was associated with a greater severity of IBS symptoms. Multivariate analysis identified several Mediterranean Diet foods to be associated with increased IBS symptoms.
A higher adherence to symptom-modified Mediterranean Diet was associated with a lower abundance of potentially harmful Faecalitalea, Streptococcus, and Intestinibacter, and higher abundance of potentially beneficial Holdemanella from the Firmicutes phylum.
A standard Mediterranean Diet was not associated with IBS symptom severity, although certain Mediterranean Diet foods were associated with increased IBS symptoms. Our study suggests that standard Mediterranean Diet may not be suitable for all patients with IBS and likely needs to be personalized in those with increased symptoms.❞
In graphical form:
And if you’d like to read more about this (along with more details on which specific foods to include or exclude to get these results), you can do so…
- The study itself (full article): The Association Between a Mediterranean Diet and Symptoms of Irritable Bowel Syndrome
- Dr. Mayer’s blog (lay explanation): The Benefits of a Modified Mediterranean Diet for Irritable Bowel Syndrome
Want to know more?
Dr. Mayer offers many resources, including a blog, books, recipes, podcasts, and even a YouTube channel:
Share This Post
Related Posts
-
My dance school is closed for the summer, how can I keep up my fitness?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Once the end-of-year dance concert and term wrap up for the year it is important to take a break. Both physical and mental rest are important and taking a few weeks off can help your body repair and have a mental break from dance.
If your mind and body are in need of an extended break (such as more than a few weeks), then it’s more than OK to take longer off, especially if you are training at a competitive or pre-professional level.
There is benefit in enjoying other aspects of your life outside of dance such as spending time with family, friends and enjoying hobbies.
Tatyana Vyc/Shutterstock A safe, fulfilling dancing life
Creating meaning and value in life outside of dance and expanding sense of self can make it easier to lean into other aspects when experiencing change or difficult times during dance training such as being injured.
Taking an extended break from dance training will, however, mean losing some fitness and physical capacity. When you return to dance your body will take time to return to full capacity again.
Approaches such as being “whipped back into shape” can promote sudden spikes in training load (hours and intensity of training) which can increase the risk of injury. It is advised to gradually and progressively increase training load over time to allow the body to adapt and return to full capacity safely.
A four-to-six week period of gradually progressing training load and introducing jumping has been suggested in dance settings.
For dancers wanting to maintain fitness over the summer holidays, a great place to start is focusing on building a physical foundation.
Exercise like running can help build a physical foundation. Jacek Chabraszewski/Shutterstock Building a physical foundation means focusing on targeted areas of fitness such as full body strength, cardiovascular fitness or stamina (such as skipping, cycling walking, running, swimming), flexibility, and some dance-specific conditioning (for example, calf rises for ballet).
A good physical foundation will mean an improved capacity and fitness level so your body is ready to take on more challenging dance movements and routines once you return to the studio.
Building full body strength at home or at the park
A great place to start is by choosing movements that require your muscles to work to support your own body weight.
Fundamental movements such as crawling (moving on the floor on hands and feet) and locomotion (travelling movements such as lunging, hopping, sliding) are great for developing body control, arm and leg stability and coordinated movement patterns.
Below is a sequence that can be used as a warm up and even as a workout itself. The ten minute sequence is based on gross motor and fundamental movement patterns. It includes exercises that work through a range of joint movements and in multiple planes (forwards, sideways, rotating).
This fundamental movement sequence can be used as a warm-up or a workout. Joanna Nicholas, CC BY Once feeling comfortable with the above fundamental movements, it is time to introduce body weight resistance exercises.
Body weight resistance exercises can be beneficial for developing a strong foundation for dance movements such as jumping, landing, floorwork, partnering and aerial work.
Exercises from the above sequence can be used to form a safe and effective neuromuscular warm up.
Aim to include one exercise from each of the below movement categories (squat, horizontal push etc) to build your own workout.
Aim to complete two to three sets (or rounds) of each exercise with about one minute rest between sets. An alternative is to complete one set of each exercise with minimal rest between, then complete a second or third time.
If training with friends, you could set a timer and do each exercise for up to 50 seconds (instead of counting reps) and take ten seconds to transition to the next exercise.
Depending on your level of strength you may need to do fewer repetitions and build up sets and repetitions overtime. After you have completed the body weight exercises complete a cool down including stretches for the upper and lower body muscles. Be sure to use a sturdy bar (such as an outdoor fitness station) for horizontal row and overhead hold.
Exercises may need to be modified depending on fitness level and physical limitations such as injury.
You can build your own full body strength workout using these movements. Joanna Nicholas, CC BY How often should I train?
A common misconception in dance is that “more is better”. This belief can lead to dancers training long hours on most or all days of the week which can lead to overtraining, plateauing and increased risk of injury.
Our bodies require sufficient time between training sessions to adapt and get stronger and fitter. The time between sessions is when our muscles and tissues repair and training gains are made.
By incorporating adequate recovery (including sleep and downtime) and including rest days throughout the week, our bodies can gain the most benefits from training.
Rest days are important, too. Manop Boonpeng/Shutterstock Muscles can take up to 48–72 hours to recover from most types of strength-based exercises (the more intense the longer they’ll need to recover).
Aerobic activity at low intensity, such as a brisk walk, can be done most days (24-hour recovery) while high stress anaerobic exercise such as high intensity intervals or sprints can take three days or more to recover from.
Aim to spread training sessions out over the week and allow time to recover between sessions.
Below is an example weekly schedule based on incorporating adequate recovery between sessions, and incorporating polarised training where some days are harder and others are easier.
Seek guidance from your healthcare provider and/or an exercise professional prior to undertaking a new exercise program.
Joanna Nicholas, Lecturer in Dance and Performance Science, Edith Cowan University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Longevity… Simplified – by Dr. Howard Luks
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In the spirit of the book itself, we’ll keep this one simple:
The information in this book will not be new to regular readers of 10almonds, or at least, not if you’ve been with us for a while (because we can only cover so much per day, so long-time readers will have accumulated more knowledge).
On the other hand, the information is clear, correct, and very much stripped down to the most important basics. Not the very simplest basics, which would be an oversimplification to the point of inutility, but the most important basics.
To take an example, when it comes to exercise, he doesn’t say “exercise more” but rather that “a complete exercise program has four pillars: aerobic training, resistance training, balance training, and high-intensity interval training (HIIT)”, and then he goes about explaining, in clear and simple terms, how to do those.
The style is similar when it comes to diet, sleep, and body-part-specific chapters such as about heart health, brain health, and so forth.
Bottom line: if you’re a long-time 10almonds reader, you probably don’t need this one, but it’d be a great book for someone else who has expressed an interest in getting healthier, as it really is a top-tier “primer” in increasing health and healthspan.
Click here to check out Longevity… Simplified, and enjoy simplified longevity!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How do I handle it if my parent is refusing aged care? 4 things to consider
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s a shock when we realise our parents aren’t managing well at home.
Perhaps the house and garden are looking more chaotic, and Mum or Dad are relying more on snacks than nutritious meals. Maybe their grooming or hygiene has declined markedly, they are socially isolated or not doing the things they used to enjoy. They may be losing weight, have had a fall, aren’t managing their medications correctly, and are at risk of getting scammed.
You’re worried and you want them to be safe and healthy. You’ve tried to talk to them about aged care but been met with swift refusal and an indignant declaration “I don’t need help – everything is fine!” Now what?
Here are four things to consider.
1. Start with more help at home
Getting help and support at home can help keep Mum or Dad well and comfortable without them needing to move.
Consider drawing up a roster of family and friends visiting to help with shopping, cleaning and outings. You can also use home aged care services – or a combination of both.
Government subsidised home care services provide from one to 13 hours of care a week. You can get more help if you are a veteran or are able to pay privately. You can take advantage of things like rehabilitation, fall risk-reduction programs, personal alarms, stove automatic switch-offs and other technology aimed at increasing safety.
Call My Aged Care to discuss your options.
Is Mum or Dad OK at home?
Nadino/Shutterstock2. Be prepared for multiple conversations
Getting Mum or Dad to accept paid help can be tricky. Many families often have multiple conversations around aged care before a decision is made.
Ideally, the older person feels supported rather than attacked during these conversations.
Some families have a meeting, so everyone is coming together to help. In other families, certain family members or friends might be better placed to have these conversations – perhaps the daughter with the health background, or the auntie or GP who Mum trusts more to provide good advice.
Mum or Dad’s main emotional support person should try to maintain their relationship. It’s OK to get someone else (like the GP, the hospital or an adult child) to play “bad cop”, while a different person (such as the older person’s spouse, or a different adult child) plays “good cop”.
3. Understand the options when help at home isn’t enough
If you have maximised home support and it’s not enough, or if the hospital won’t discharge Mum or Dad without extensive supports, then you may be considering a nursing home (also known as residential aged care in Australia).
Every person has a legal right to choose where we live (unless they have lost capacity to make that decision).
This means families can’t put Mum or Dad into residential aged care against their will. Every person also has the right to choose to take risks. People can choose to continue to live at home, even if it means they might not get help immediately if they fall, or eat poorly. We should respect Mum or Dad’s decisions, even if we disagree with them. Researchers call this “dignity of risk”.
It’s important to understand Mum or Dad’s point of view. Listen to them. Try to figure out what they are feeling, and what they are worried might happen (which might not be rational).
Try to understand what’s really important to their quality of life. Is it the dog, having privacy in their safe space, seeing grandchildren and friends, or something else?
Older people are often understandably concerned about losing independence, losing control, and having strangers in their personal space.
Sometimes families prioritise physical health over psychological wellbeing. But we need to consider both when considering nursing home admission.
Research suggests going into a nursing home temporarily increases loneliness, risk of depression and anxiety, and sense of losing control.
Mum and Dad should be involved in the decision-making process about where they live, and when they might move.
Some families start looking “just in case” as it often takes some time to find the right nursing home and there can be a wait.
After you have your top two or three choices, take Mum or Dad to visit them. If this is not possible, take pictures of the rooms, the public areas in the nursing home, the menu and the activities schedule.
We should give Mum or Dad information about their options and risks so they can make informed (and hopefully better) decisions.
For instance, if they visit a nursing home and the manager says they can go on outings whenever they want, this might dispel a belief they are “locked up”.
Having one or two weeks “respite” in a home may let them try it out before making the big decision about staying permanently. And if they find the place unacceptable, they can try another nursing home instead.
You might need to have multiple conversations about aged care.
CGN089/Shutterstock4. Understand the options if a parent has lost capacity to make decisions
If Mum or Dad have lost capacity to choose where they live, family may be able to make that decision in their best interests.
If it’s not clear whether a person has capacity to make a particular decision, a medical practitioner can assess for that capacity.
Mum or Dad may have appointed an enduring guardian to make decisions about their health and lifestyle decisions when they are not able to.
An enduring guardian can make the decision that the person should live in residential aged care, if the person no longer has the capacity to make that decision themselves.
If Mum or Dad didn’t appoint an enduring guardian, and have lost capacity, then a court or tribunal can appoint that person a private guardian (usually a family member, close friend or unpaid carer).
If no such person is available to act as private guardian, a public official may be appointed as public guardian.
Deal with your own feelings
Families often feel guilt and grief during the decision-making and transition process.
Families need to act in the best interest of Mum or Dad, but also balance other caring responsibilities, financial priorities and their own wellbeing.
Lee-Fay Low, Professor in Ageing and Health, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: