How Aging Changes At 44 And Again At 60 (And What To Do About It)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
As it turns out, aging is not linear. Or rather: chronological aging may be, but biological aging isn’t, and there are parts of our life where it kicks into a different gear. This study looked at 108 people (65 of whom women) between the ages of 25 and 75, as part of a longitudinal cohort study, tracked for around 2–8 years (imprecise as not all follow-up durations were the same). They took frequent blood and urine samples, and tested them for thousands of different molecules and analyzing changes in gene expression, proteomic, blood biomarkers, and more. All things that are indicators of various kinds of health/disease, and which might seem more simple but it isn’t: aging.
Here’s what they found:
Landmark waypoints
At 44, significant changes occur in the metabolism, including notably the metabolism of carbs, caffeine, and alcohol. A large portion of this may be hormone related, as that’s a time of change not just for those undergoing the menopause, but also the andropause (not entirely analogous to the menopause, but it does usually entail a significant reduction in sex hormone production; in this case, testosterone).
However, the study authors also hypothesize that lifestyle factors may be relevant, as one’s 40s are often a stressful time, and an increase in alcohol consumption often occurs around the same time as one’s ability to metabolize it drops, resulting in further dysfunctional alcohol metabolism.
At 60, carb metabolism slows again, with big changes in glucose metabolism specifically, as well as an increased risk of cardiovascular disease, and a decline in kidney function. In case that wasn’t enough: also an increase free radical pathology, meaning a greatly increased risk of cancer. Immune function drops too.
What to do about this: the recommendation is of course to be proactive, and look after various aspects of your health before it becomes readily apparent that you need to. For example, good advice for anyone approaching 44 might be to quit alcohol, go easy on caffeine, and eat a diet that is conducive to good glucose metabolism. Similarly, good advice for anyone approaching 60 might be to do the same, and also pay close attention to keeping your kidneys healthy. Getting regular tests done is also key, including optional extras that your doctor might not suggest but you should ask for, such as blood urea nitrogen levels (biomarkers of kidney function). The more we look after each part of our body, the more they can look after us in turn, and the fewer/smaller problems we’ll have down the line.
If you, dear reader, are approaching the age 44 or 60… Be neither despondent nor complacent. We must avoid falling into the dual traps of “Well, that’s it, bad health is around the corner, nothing I can do about it; that’s nature”, vs “I’ll be fine, statistics are for other people, and don’t apply to me”.
Those are averages, and we do not have to be average. Every population has statistical outliers. But it would be hubris to think none of this will apply to us and we can just carry on regardless. So, for those of us who are approaching one of those two ages… It’s time to saddle up, knuckle down, and do our best!
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Also, if you’d like to read the actual paper by Dr. Xiaotao Shen et al., here it is:
Nonlinear dynamics of multi-omics profiles during human aging ← honestly, it’s a lot clearer and more informative than the video, and also obviously discusses things in a lot more detail than we have room to here
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Tofu vs Seitan – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing tofu to seitan, we picked the tofu.
Why?
This one is not close!
In terms of macros, seitan does have about 2x the protein, but it also has 6x the carbs and 6x the sodium of tofu, as well as less fiber than tofu.. So we’ll call it a tie on macros. But…
Seitan is also much more processed than tofu, as tofu has usually just been fermented and possibly pressed (depending on kind). Seitan, in contrast, is processed gluten that has been extracted from wheat and usually had lots of things happen to it on the way (depending on kind).
About that protein… Tofu is a complete protein, meaning it has all of the essential amino acids. Seitain, meanwhile, is lacking in lysine.
When it comes to vitamins and minerals, again tofu easily comes out on top; tofu has 5x the calcium, similar iron, more magnesium, 2x the phosphorous, 150% of the potassium, and contains several other nutrients that seitan doesn’t, such as folate and choline.
So, easy winning for tofu across the board on micronutrients.
Tofu is also rich in isoflavones, antioxidant phytonutrients, while seitan has no such benefits.
So, another win for tofu.
There are two reasons you might choose seitan:
- prioritizing bulk protein above all other health considerations
- you are allergic to soy and not allergic to gluten
If neither of those things are the case, then tofu is the healthier choice!
Want to learn more?
You might like to read:
- Tempeh vs Tofu – Which is Healthier? ← tempeh is, nutritionally speaking, tofu but better. Of course on a culinary level, there are many recipes where tofu will work and tempeh wouldn’t, though.
- Gluten: What’s The Truth?
Take care!
Share This Post
-
Artichoke vs Cabbage – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing artichoke to cabbage, we picked the artichoke.
Why?
Looking at the macros first of all, artichoke has more than 2x the protein; it also has nearly 2x the carbs, but to more than counterbalance that, it has more than 2x the fiber. An easy win for artichoke in the macros category.
In the category of vitamins, both are very respectable; artichoke has more of vitamins B1, B2, B3, B5, B9, E, and choline, while cabbage has more of vitamins A, C, and K. Superficially, that’s a 7:3 win for artichoke, but the margins of difference for artichoke’s vitamins are very small (meaning cabbage is hot on its heels for those vitamins), whereas cabbage’s A, C, and K are with big margins of difference (3–7x more), and arguably those vitamins are higher priority in the sense that B-vitamins of various kinds are found in most foods, whereas A, C, and K aren’t, and while E isn’t either, artichoke had a tiny margin of difference for that. All in all, we’re calling this category a tie, as an equally fair argument could be made for either vegetable here.
When it comes to minerals, there’s a much clearer winner: artichoke has a lot more copper, iron, magnesium, manganese, phosphorus, potassium, and zinc, while cabbage has a tiny bit more selenium. The two vegetables are equal on calcium.
Adding up two clear artichoke wins and a tie, makes for an overall clear win for artichoke. Of course, enjoy both though; diversity is almost always best of all!
Want to learn more?
You might like to read:
What’s Your Plant Diversity Score?
Take care!
Share This Post
-
Missing Microbes – by Dr. Martin Blaser
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You probably know that antibiotic resistance is a problem, but you might not realize just what a many-headed beast antibiotic overuse is.
From growing antibiotic superbugs, to killing the friendly bacteria that normally keep pathogens down to harmless numbers (resulting in death of the host, as the pathogens multiply unopposed), to multiple levels of dangers in antibiotic overuse in the farming of animals, this book is scary enough that you might want to save it for Halloween.
But, Dr. Blaser does not argue against antibiotic use when it’s necessary; many people are alive because of antibiotics—he himself recovered from typhoid because of such.
The style of the book is narrative, but information-dense. It does not succumb to undue sensationalization, but it’s also far from being a dry textbook.
Bottom line: if you’d like to understand the real problems caused by antibiotics, and how we can combat that beyond merely “try not to take them unnecessarily”, this book is very worthy reading.
Click here to check out Missing Microbes, and learn more about yours!
Share This Post
Related Posts
-
Eye Drops: Safety & Alternatives
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? You can always hit “reply” to any of our emails, or use the feedback widget at the bottom!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝Before important business meetings my father used to use eye drops to add a “sparkle” to his eyes. I think that is a step too far, but what, short of eye drops, can we do to keep our eyes bright throughout the day?❞
Firstly, we’d indeed not recommend eye drops unless advised to do so by your doctor to treat a specific health condition:
- Infections from over-the-counter artificial tears
- Are my eye drops safe to use?
- More eye drops recalled due to infection danger
Those eye drops that “add sparkle” are often based on astringents such as witch hazel. This means that the capillaries in the eye undergo vasoconstriction, becoming much less visible and the eye thus appears much whiter and thus brighter.
There isn’t a way to do the same thing from the inside, as taking a vasoconstrictor will simply increase your general blood pressure, making the capillaries of your eyes more, rather than less, visible.
However, what you can do is…
- look after your general vasculature (cardiovascular health)
- in particular, reduce hypertension
- that includes limiting salt
- stay away from vasoconstrictors (including caffeine)
- reduce your resting cortisol levels
- that certainly also means reducing alcohol consumption
- maintain good hydration
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Modern Art and Science of Mobility – by Aurélien Broussal-Derval
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve reviewed mobility books before, so what makes this one stand out?
We’ll be honest: the illustrations are lovely.
The science, the information, the exercises, the routines, the programs… All these things are excellent too, but these can be found in many a book.
What can’t usually be found is very beautiful (yet no less clear) watercolor paintings and charcoal sketches as anatomical illustrations.
There are photos too (also of high quality), but the artistry of the paintings and sketches is what makes the reader want to spend time perusing the books.
At least, that’s what this reviewer found! Because it’s all very well having access to a lot of information (and indeed, I read so much), but making it enjoyable increases the chances of rereading it much more often.
As for the rest of the content, the book’s information is divided in categories:
- Pain (what causes it, what it means, and how to manage it)
- Breathing (yes, a whole section devoted to this, and it is aligned heavily to posture also, as well as psychological state and the effect of stress on tension, inflammation, and more)
- Movement (this is mostly about kinds of movement and ranges of movement)
- Mobility (this is about aggregating movements as a fully mobile human)
So, each builds on from the previous because any pain needs addressing before anything else, breathing (and with it, posture) comes next, then we learn about movement, then we bring it all together for mobility.
Bottom line: this is a beautiful and comprehensive book that will make learning a joy
Click here to check out The Modern Art and Science of Mobility, and learn and thrive!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Debate over tongue tie procedures in babies continues. Here’s why it can be beneficial for some infants
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
There is increasing media interest about surgical procedures on new babies for tongue tie. Some hail it as a miracle cure, others view it as barbaric treatment, though adverse outcomes are rare.
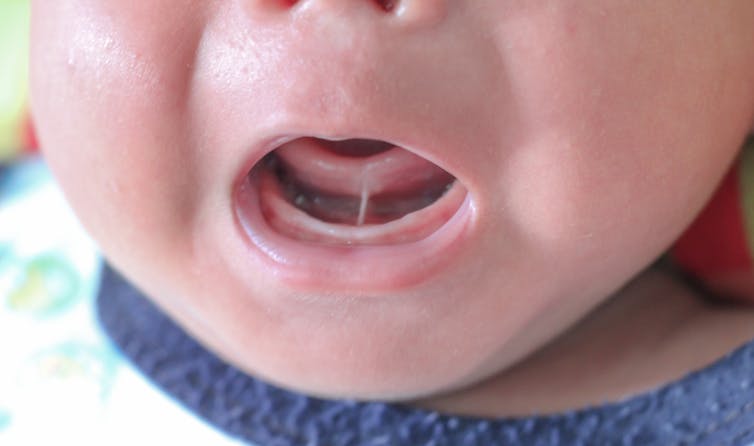
Tongue tie occurs when the tissue under the tongue is attached to the lower gum or floor of the mouth in a way that can restrict the movement or range of the tongue. This can impact early breastfeeding in babies. It affects an estimated 8% of children under one year of age.
While there has been an increase in tongue tie releases (also called division or frenotomy), it’s important to keep this in perspective relative to the increase in breastfeeding rates.
The World Health Organization recommends exclusive breastfeeding for the first six months of life, with breastfeeding recommended into the second year of life and beyond for the health of mother and baby as well as optimal growth. Global rates of breastfeeding infants for the first six months have increased from 38% to 48% over the past decade. So, it is not surprising there is also an increase in the number of babies being referred globally with breastfeeding challenges and potential tongue tie.
An Australian study published in 2023 showed that despite a 25% increase in referrals for tongue tie division between 2014 and 2018, there was no increase in the number of tongue tie divisions performed. Tongue tie surgery rates increased in Australia in the decade from 2006 to 2016 (from 1.22 per 1,000 population to 6.35) for 0 to 4 year olds. There is no data on surgery rates in Australia over the last eight years.
Tongue tie division isn’t always appropriate but it can make a big difference to the babies who need it. More referrals doesn’t necessarily mean more procedures are performed.
chomplearn/Shutterstock How tongue tie can affect babies
When tongue tie (ankyloglossia) restricts the movement of the tongue, it can make it more difficult for a baby to latch onto the mother’s breast and painlessly breastfeed.
Earlier this month, the International Consortium of oral Ankylofrenula Professionals released a tongue tie position statement and practice guideline. Written by a range of health professionals, the guidelines define tongue tie as a functional diagnosis that can impact breastfeeding, eating, drinking and speech. The guidelines provide health professionals and families with information on the assessment and management of tongue tie.
Tongue tie release has been shown to improve latch during breastfeeding, reduce nipple pain and improve breast and bottle feeding. Early assessment and treatment are important to help mothers breastfeed for longer and address any potential functional problems.
The frenulum is a band of tissue under the tongue that is attached to the gumline base of the mouth. Akkalak Aiempradit/Shutterstock Where to get advice
If feeding isn’t going well, it may cause pain for the mother or there may be signs the baby isn’t attaching properly to the breast or not getting enough milk. Parents can seek skilled help and assessment from a certified lactation consultant or International Board-Certified Lactation Consultant who can be found via online registry.
Alternatively, a health professional with training and skills in tongue tie assessment and division can assist families. This may include a doctor, midwife, speech pathologist or dentist with extended skills, training and experience in treating babies with tongue tie.
When access to advice or treatment is delayed, it can lead to unnecessary supplementation with bottle feeds, early weaning from breastfeeding and increased parental anxiety.
Getting a tongue tie assessment
During assessment, a qualified health professional will collect a thorough case history, including pregnancy and birth details, do a structural and functional assessment, and conduct a comprehensive breastfeeding or feeding assessment.
They will view and thoroughly examine the mouth, including the tongue’s movement and lift. The appearance of where the tissue attaches to the underside of the tongue, the ability of the tongue to move and how the baby can suck also needs to be properly assessed.
Treatment decisions should focus on the concerns of the mother and baby and the impact of current feeding issues. Tongue tie division as a baby is not recommended for the sole purpose of avoiding speech problems in later life if there are no feeding concerns for the baby.
A properly qualified lactation consultant can help with positioning and attachment. HarryKiiM Stock/Shutterstock Treatment options
The Australian Dental Association’s 2020 guidelines provide a management pathway for babies diagnosed with tongue tie.
Once feeding issues are identified and if a tongue tie is diagnosed, non-surgical management to optimise positioning, latch and education for parents should be the first-line approach.
If feeding issues persist during follow-up assessment after non-surgical management, a tongue tie division may be considered. Tongue tie release may be one option to address functional challenges associated with breastfeeding problems in babies.
There are risks associated with any procedure, including tongue tie release, such as bleeding. These risks should be discussed with the treating practitioner before conducting any laser, scissor or scalpel tongue tie procedure.
Post-release support by a certified lactation consultant or feeding specialist is necessary after a tongue tie division. A post-release treatment plan should be developed by a team of health professionals including advice and support for breastfeeding to address both the mother and baby’s individual needs.
We would like to acknowledge the contribution of Raymond J. Tseng, DDS, PhD, (Paediatric Dentist) to the writing of this article.
Sharon Smart, Lecturer and Researcher (Speech Pathology) – School of Allied Health, Curtin University; David Todd, Associate Professor, Neonatology, ANU Medical School, Australian National University, and Monica J. Hogan, PhD student, ANU School of Medicine and Psychology, Australian National University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: