Brown Rice Protein: Strengths & Weaknesses
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝I had a friend mention that recent research showed Brown Rice Protein Powder can be bad for you, possibly impacting your nutrient absorption. Is this true? I’ve been using it given it’s one of the few plant-based proteins with a full essential amino acid profile!❞
Firstly: we couldn’t find anything to corroborate the “brown rice protein powder [adversely] impacts nutrient absorption” idea, but we suspect that the reason for this belief is: brown rice (not brown rice protein powder) contains phytic acid, which is something of an antinutrient, in that it indeed reduces absorption of various other nutrients.
However, two things are important to note here:
- the phytic acid is found in whole grains, not in protein isolates as found in brown rice protein powder. The protein isolates contain protein… Isolated. No phytates!
- even in the case of eating whole grain rice, the phytic acid content is greatly reduced by two things: soaking and heating (especially if those two things are combined) ← doing this the way described results in bioavailability of nutrients that’s even better than if there were just no phytic acid, albeit it requires you having the time to soak, and do so at temperature.
tl;dr = no, it’s not true, unless there truly is some groundbreaking new research we couldn’t find—it was almost certainly a case of an understandable confusion about phytic acid.
Your question does give us one other thing to mention though:
Brown rice indeed technically contains all 9 essential amino acids, but it’s very low in several of them, most notably lysine.
However, if you use our Tasty Versatile Rice Recipe, the chia seeds we added to the rice have 100x the lysine that brown rice does, and the black pepper also boosts nutrient absorption.
Because your brown rice protein powder is a rice protein powder and not simply rice, it’s possible that they’ve tweaked it to overcome rice’s amino acid deficiencies. But, if you’re looking for a plant-based protein powder that is definitely a complete protein, soy is a very good option assuming you’re not allergic to that:
Amino Acid Compositions Of Soy Protein Isolate
If you’re wondering where to get it, you can see examples of them next to each other on Amazon here:
Brown Rice Protein Powder | Soy Protein Isolate Powder
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Covering obesity: 6 tips for dispelling myths and avoiding stigmatizing news coverage
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
When researchers looked at news coverage of obesity in the United States and the United Kingdom a few years ago, they found that images in news articles often portrayed people with larger bodies “in a stigmatizing manner” — they emphasized people’s abdomens, for example, or showed them eating junk food, wearing tight clothes or lounging in front of a TV.
When people with larger bodies were featured in photos and videos, nearly half were shown only from their necks down or with part of their heads missing, according to the analysis, published in November 2023. The researchers examined a total of 445 images posted to the websites of four U.S. news outlets and four U.K. news outlets between August 2018 and August 2019.
The findings underscore the need for dramatic changes in the way journalists report on obesity and people who weigh more than what medical authorities generally consider healthy, Rebecca Puhl, one of the paper’s authors, told The Journalist’s Resource in an email interview.
“Using images of ‘headless stomachs’ is dehumanizing and stigmatizing, as are images that depict people with larger bodies in stereotypical ways (e.g., eating junk food or being sedentary),” wrote Puhl, deputy director of the Rudd Center for Food Policy and Health at the University of Connecticut and a leading scholar on weight stigma.
She noted that news images influence how the public views and interacts with people with obesity, a complicated and often misunderstood condition that the American Medical Association considers a disease.
In the U.S., an estimated 42% of adults aged 20 years and older have obesity, a number researchers predict will rise to 50% over the next six years. While the disease isn’t as common in other parts of the planet, the World Obesity Federation projects that by 2035, more than half the global population will have obesity or overweight.
Several other studies Puhl has conducted demonstrate that biased new images can have damaging consequences for individuals affected by obesity.
“Our research has found that seeing the stigmatizing image worsens people’s attitudes and weight bias, leading them to attribute obesity to laziness, increasing their dislike of people with higher weight, and increasing desire for social distance from them,” Puhl explained.
Dozens of studies spotlight problems in news coverage of obesity in the U.S. and abroad. In addition to stigmatizing images, journalists use stigmatizing language, according to a 2022 research review in eClinicalMedicine, a journal published by The Lancet.
The research also suggests people with higher weights feel excluded and ridiculed by news outlets.
“Overt or covert discourses in news media, social media, and public health campaigns included depictions of people with overweight or obesity as being lazy, greedy, undisciplined, unhappy, unattractive, and stupid,” write the authors of the review, which examines 113 academic studies completed before Dec. 2, 2021.
To help journalists reflect on and improve their work, The Journalist’s Resource asked for advice from experts in obesity, weight stigma, health communication and sociolinguistics. They shared their thoughts and opinions, which we distilled into the six tips that appear below.
In addition to Puhl, we interviewed these six experts:
Jamy Ard, a professor of epidemiology and prevention at Wake Forest University School of Medicine and co-director of the Wake Forest Baptist Health Weight Management Center. He’s also president of The Obesity Society, a professional organization of researchers, health care providers and other obesity specialists.
Leslie Cofie, an assistant professor of health education and promotion at East Carolina University’s College of Health and Human Performance. He has studied obesity among immigrants and military veterans.
Leslie Heinberg, director of Enterprise Weight Management at the Cleveland Clinic, an academic medical center. She’s also vice chair for psychology in the Cleveland Clinic’s Center for Behavioral Health Department of Psychiatry and Psychology.
Monu Khanna, a physician in Missouri who is board certified in obesity medicine.
Jenn Lonzer, manager of the Cleveland Clinic Health Library and the co-author of several academic papers on health communication.
Cindi SturtzSreetharan, an anthropologist and professor at the Arizona State University School of Human Evolution and Social Change. She studies the language people of different cultures use to describe human bodies.
1. Familiarize yourself with recent research on what causes obesity and how obesity can affect a person’s health. Many long-held beliefs about the disease are wrong.
Journalists often report incorrect or misleading information about obesity, possibly because they’re unaware that research published in recent decades dispels many long-held beliefs about the disease, the experts say. Obesity isn’t simply the result of eating too many calories and doing too little exercise. A wide range of factors drive weight gain and prevent weight loss, many of which have nothing to do with willpower or personal choices.
Scholars have learned that stress, gut health, sleep duration and quality, genetics, medication, personal income, access to healthy foods and even climate can affect weight regulation. Prenatal and early life experiences also play a role. For example, childhood trauma such as child abuse can become “biologically embedded,” altering children’s brain structures and influencing their long-term physical and mental health, according to a 2020 research review published in the journal Physiology & Behavior.
“The causes of obesity are numerous and each individual with obesity will have a unique set of contributors to their excess weight gain,” Jamy Ard, president of The Obesity Society, wrote to The Journalist’s Resource.
The experts urge journalists to help dispel myths, correct misinformation and share new research findings. News outlets should examine their own work, which often “ignores the science and sets up situation blaming,” says Leslie Heinberg, director of Enterprise Weight Management at the Cleveland Clinic.
“So much of the media portrayal is simply ‘This is a person who eats too much and the cure is simply to eat less or cut out that food’ or something overly, overly simplistic,” Heinberg says.
Journalists need to build their knowledge of the problem before they can explain it to their audiences. Experts point out that educating policymakers, health care providers and the public about obesity is key to eliminating the stigma associated with having a larger body.
Weight stigma alone is so physically and emotionally damaging that 36 international experts issued a consensus statement in 2020 to raise awareness about it. The document, endorsed by dozens of medical and academic organizations, outlines 13 recommendations for eliminating weight bias and stigma.
Recommendation No. 5: “We call on the media to produce fair, accurate, and non-stigmatizing portrayals of obesity. A commitment from the media is needed to shift the narrative around obesity.”
2. Use person-first language — the standard among health and medical professionals for communicating about people with chronic diseases.
The experts we interviewed encourage journalists to ditch the adjectives “obese” and “overweight” because they are dehumanizing. Use person-first language, which avoids labeling people as their disease by putting the person before the disease.
Instead of saying “an obese teenager,” say “a teenager who has obesity” or “a teenager affected by obesity.” Instead of writing “overweight men,” write “men who have overweight.”
Jenn Lonzer, manager of the Cleveland Clinic Health Library, says using “overweight” as a noun might look and sound awkward at first. But it makes sense considering other diseases are treated as nouns, she notes. Journalists would not typically refer to someone in a news story as “a cancerous person,” for example. They would report that the individual has cancer.
It’s appropriate to refer to people with overweight or obesity using neutral weight terminology. Puhl wrote that she uses “people with higher body weight” or “people with high weight” and, sometimes, “people with larger bodies” in her own writing.
While the Associated Press stylebook offers no specific guidance on the use of terms such as “obese” or “overweight,” it advises against “general and often dehumanizing ‘the’ labels such as the poor, the mentally ill, the disabled, the college-educated.”
The Association of Health Care Journalists recommends person-first language when reporting on obesity. But it also advises journalists to ask sources how they would like to be characterized, provided their weight or body size is relevant to the news story.
Anthropologist Cindi SturtzSreetharan, who studies language and culture, says sources’ responses to that question should be part of the story. Some individuals might prefer to be called “fat,” “thick” or “plus-sized.”
“I would include that as a sentence in the article — to signal you’ve asked and that’s how they want to be referred to,” SturtzSreetharan says.
She encourages journalists to read how authors describe themselves in their own writing. Two books she recommends: Thick by Tressie McMillan Cottom and Heavy: An American Memoir by Kiese Laymon.
3. Carefully plan and choose the images that will accompany news stories about obesity.
Journalists need to educate themselves about stigma and screen for it when selecting images, Puhl noted. She shared these four questions that journalists should ask themselves when deciding how to show people with higher weights in photos and video.
- Does the image imply or reinforce negative stereotypes?
- Does it provide a respectful portrayal of the person?
- Who might be offended, and why?
- Can an alternative image convey the same message and eliminate possible bias?
“Even if your written piece is balanced, accurate, and respectful, a stigmatizing image can undermine your message and promote negative societal attitudes,” Puhl wrote via email.
Lonzer says newsrooms also need to do a better job incorporating images of people who have different careers, interests, education levels and lifestyles into their coverage of overweight and obesity.
“We are diverse,” says Lonzer, who has overweight. “We also have diversity in body shape and size. It’s good to have images that reflect what Americans look like.”
If you’re looking for images and b-roll videos that portray people with obesity in non-stigmatizing ways, check out the Rudd Center Media Gallery. It’s a collection of original images of people from various demographic groups that journalists can use for free in their coverage.
The Obesity Action Coalition, a nonprofit advocacy organization, also provides images. But journalists must sign up to use the OAC Bias-Free Image Gallery.
Other places to find free images: The World Obesity Image Bank, a project of the World Obesity Federation, and the Flickr account of Obesity Canada.
4. Make sure your story does not reinforce stereotypes or insinuate that overcoming obesity is simply a matter of cutting calories and doing more exercise.
“Think about the kinds of language used in the context of eating habits or physical activity, as some can reinforce shame or stereotypes,” Puhl wrote.
She suggested journalists avoid phrases such as “resisting temptations,” “cheating on a diet,” “making excuses,” “increasing self-discipline” and “lacking self-control” because they perpetuate the myth that individuals can control their weight and that the key to losing weight is eating less and moving more.
Lonzer offers this advice: As you work on stories about obesity or weight-related issues, ask yourself if you would use the same language and framing if you were reporting on someone you love.
Here are other questions for journalists to contemplate:
“Am I treating this as a complex medical condition or am I treating it as ‘Hey, lay off the French fries?’” Lonzer adds. “Am I treating someone with obesity differently than someone with another disease?”
It’s important to also keep in mind that having excess body fat does not, by itself, mean a person is unhealthy. And don’t assume everyone who has a higher weight is unhappy about it.
“Remember, not everyone with obesity is suffering,” physician Monu Khanna wrote to The Journalist’s Resource.
5. To help audiences understand how difficult it is to prevent and reduce obesity, explain that even the places people live can affect their waistlines.
When news outlets report on obesity, they often focus on weight-loss programs, surgical procedures and anti-obesity medications. But there are other important issues to cover. Experts stress the need to help the public understand how factors not ordinarily associated with weight gain or loss can influence body size.
For example, a paper published in 2018 in the American Journal of Preventive Medicine indicates adults who are regularly exposed to loud noise have a higher waist circumference than adults who are not. Research also finds that people who live in neighborhoods with sidewalks and parks are more active.
“One important suggestion I would offer to journalists is that they need to critically explore environmental factors (e.g., built environment, food deserts, neighborhood safety, etc.) that lead to disproportionately high rates of obesity among certain groups, such as low-income individuals and racial/ethnic minorities,” Leslie Cofie, an assistant professor at East Carolina University, wrote to The Journalist’s Resource.
Cofie added that moving to a new area can prompt weight changes.
“We know that immigrants generally have lower rates of obesity when they first migrate to the U.S.,” he wrote. “However, over time, their obesity rates resemble that of their U.S.-born counterparts. Hence, it is critical for journalists to learn about how the sociocultural experiences of immigrants change as they adapt to life in the U.S. For example, cultural perspectives about food, physical activities, gender roles, etc. may provide unique insights into how the pre- and post-migration experiences of immigrants ultimately contribute to the unfavorable trends in their excessive weight gain.”
Other community characteristics have been linked to larger body sizes for adults or children: air pollution, lower altitudes, higher temperatures, lower neighborhood socioeconomic status, perceived neighborhood safety, an absence of local parks and closer proximity to fast-food restaurants.
6. Forge relationships with organizations that study obesity and advocate on behalf of people living with the disease.
Several organizations are working to educate journalists about obesity and help them improve their coverage. Five of the most prominent ones collaborated on a 10-page guide book, “Guidelines for Media Portrayals of Individuals Affected by Obesity.”
- The Rudd Center for Food Policy and Health, based at the University of Connecticut, “promotes solutions to food insecurity, poor diet quality, and weight bias through research and policy,” according to its website. Research topics include food and beverage marketing, weight-related bullying and taxes on sugary drinks.
- The Obesity Society helps journalists arrange interviews with obesity specialists. It also offers journalists free access to its academic journal, Obesity, and free registration to ObesityWeek, an international conference of researchers and health care professionals held every fall. This year’s conference is Nov. 2-6 in San Antonio, Texas.
- The Obesity Medicine Association represents health care providers who specialize in obesity treatment and care. It also helps journalists connect with obesity experts and offers, on an individual basis, free access to its events, including conferences and Obesity Medicine Fundamentals courses.
- The Obesity Action Coalition offers free access to its magazine, Weight Matters, and guides on weight bias at work and in health care.
- The American Society for Metabolic and Bariatric Surgery represents surgeons and other health care professionals who work in the field of metabolic and bariatric surgery. It provides the public with resources such as fact sheets and brief explanations of procedures such as the Roux-en-Y Gastric Bypass.
For further reading
Weight Stigma in Online News Images: A Visual Content Analysis of Stigma Communication in the Depictions of Individuals with Obesity in U.S. and U.K. News
Aditi Rao, Rebecca Puhl and Kirstie Farrar. Journal of Health Communication, November 2023.Influence and Effects of Weight Stigmatization in Media: A Systematic Review
James Kite; et al. eClinicalMedicine, June 2022.Has the Prevalence of Overweight, Obesity and Central Obesity Leveled Off in the United States? Trends, Patterns, Disparities, and Future Projections for the Obesity Epidemic
Youfa Wang; et al. International Journal of Epidemiology, June 2020.This article first appeared on The Journalist’s Resource and is republished here under a Creative Commons license.
Share This Post
-
Reporting on psychedelics research or legislation? Proceed with caution
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
More cities and states are introducing bills to decriminalize and regulate access to psychedelic drugs, which could potentially become another option to treat mental health conditions and substance use disorders. But the substances remain illegal under U.S. federal law and scientific evidence about their effectiveness is still far from conclusive.
This month alone, California lawmakers introduced a bill to allow people 21 and older to consume psychedelic mushrooms under medical supervision. In Massachusetts, lawmakers are working on a bill that would legalize psilocybin, the active ingredient of psychedelic mushrooms. And Arizona legislators have also introduced a bill that would make psychedelic mushrooms available as a mental health treatment option.
Last December, Congress passed legislation that included funding for psychedelic clinical trials for active-duty service members. And in January this year, the Department of Veterans Affairs announced that it will begin funding research on MDMA, also known as ecstasy, and psilocybin, to treat veterans with post-traumatic stress disorder and depression. This is the first time since the 1960s that the VA is funding research on such compounds, according to the department.
The rise of proposed and passed legislation in recent years necessitates more journalistic coverage. But it’s important for journalists to go beyond what the bills and lawmakers say and include research studies about psychedelics and note the limitations of those studies.
Major medical organizations, including the American Psychiatric Association, have not yet endorsed psychedelics to treat psychiatric disorders, except in clinical trials, due to inadequate scientific evidence.
The authors of a 2023 study published in the journal Therapeutic Advances in Psychopharmacology, also advise “strong caution” regarding the hype around the potential medical use of psychedelics. “There is not enough robust evidence to draw any firm conclusions about the safety and efficacy of psychedelic therapy,” they write.
Scientists are still trying to better understand how psychedelics work, what’s the best dose for treating different mental health conditions and how to reduce the risk of potential side effects such as intense emotional experiences or increased heart rate and blood pressure, the authors of a February 2024 study published in the journal Progress in Neuro-Psychopharmacology and Biological Psychiatry write.
In a 2022 study published in JAMA Psychiatry, Dr. Joshua Siegel and his colleagues at Washington University in St. Louis write that while legislative reform for psychedelic drugs is moving forward rapidly, several issues have not been addressed, including:
- A mechanism for verifying the chemical content of drugs that are obtained from outside the medical establishment.
- Licensure and training criteria for practitioners who wish to provide psychedelic treatment.
- Clinical and billing infrastructure.
- Assessing potential interactions with other drugs.
- How the drugs should be used in populations such as youths, older adults and pregnant people.
“Despite the relative rapidity with which some have embraced psychedelics as legitimate medical treatments, critical questions about the mechanism of action, dose and dose frequency, durability of response to repeated treatments, drug-drug interactions, and the role that psychotherapy plays in therapeutic efficacy remain unanswered,” Siegel and colleagues write.
What are psychedelics?
Psychedelics are among the oldest class of mind-altering substances, used by humans for thousands of years in traditional or religious rituals.
In 2021, 74 million people 12 years and older reported using hallucinogens, according to the National Survey on Drug Use and Health.
The terms “psychedelics” and “hallucinogens” are used interchangeably in public discourse, but scientifically, hallucinogens fall into three groups based on chemical structure and mechanism of action, according to NIH’s National Institute on Drug Abuse:
- Psychedelic drugs, also called “classic psychedelics” or simply “psychedelics,” mainly affect the way the brain processes serotonin, a chemical that carries messages between nerve cells in the brain and the body. These drugs can bring on vivid visions and affect a person’s sense of self, according to NIDA. Drugs in this category include:
- Psilocybin is the active ingredient in psychedelic mushrooms, also known as “magic” mushrooms or shrooms. It’s a Schedule 1 drug in the U.S. under the Controlled Substances Act, which means it has a high potential for abuse and has no accepted medical use. However, some states have decriminalized it, according to NIDA. The drug has also been given the Breakthrough Therapy designation from the FDA, a process to speed up the development and review of drugs, for the treatment of major depressive disorder.
- LSD, or lysergic acid diethylamide, is a synthetic chemical made from a fungus that infects rye. It’s a Schedule 1 drug.
- DMT, or dimethyltryptamine, found in certain plants native to the Amazon rainforest, has been used in religious practices and rituals. The plants are sometimes used to make a tea called ayahuasca. DMT can also be made in the lab as a white powder. DMT is generally smoked or consumed in brews like ayahuasca. It’s a Schedule 1 drug.
- Mescaline, a chemical compound found in a small cactus called peyote, has been used by Indigenous people in northern Mexico and the southwestern U.S. in religious rituals. Mescaline can also be produced in the lab. Mescaline and peyote are Schedule 1 drugs.
- Dissociative drugs affect how the brain processes glutamate, an abundant chemical released by nerve cells in the brain that plays an important role in learning and memory. These drugs can make people feel disconnected from their bodies and surroundings. Drugs in this category include:
- PCP, or phencyclidine, was developed in the 1950s as an injectable anesthetic but was discontinued because patients became agitated and delusional. Today it is an illegal street drug. It’s a Schedule 2 drug, which means it has a high potential for abuse, but lower compared to Schedule 1 drugs.
- Ketamine, a drug developed in the 1960s and used as an anesthetic in the Vietnam War, is approved by the FDA as an anesthetic. It has been shown to play a role in pain management and treatment of depression. It is also illegally used for its hallucinogenic effects. It is a Schedule 3 drug, which means it has a moderate to low potential for physical and psychological dependence. A chemically-similar drug called esketamine is approved by the FDA for the treatment of depression that doesn’t respond to standard treatment.
- Other hallucinogens, which affect different brain functions and can cause psychedelic and potentially dissociative effects, include:
- MDMA, or ecstasy, is a synthetic drug that’s a stimulant and hallucinogen. It is a Schedule 1 drug. It has been given the Breakthrough Therapy designation from the FDA for the treatment of PTSD.
- Salvia is an herb in the mint family that has hallucinogenic effects. It is not a federally controlled drug, but it is controlled in some states, according to the DEA.
- Ibogaine is derived from the root bark of a West African shrub and is a stimulant and hallucinogen. It is a Schedule 1 drug.
Research on psychedelics
There was a wave of studies on psychedelics, particularly LSD, in the 1950s and 1960s, but they came to a halt when the U.S. declared a “War on Drugs” in 1971 and tightened pharmaceutical regulations. There was little research activity until the early 1990s when studies on drugs such as MDMA and DMT began to emerge.
In 2006, researchers at Johns Hopkins University published a seminal double-blind study in which two-thirds of participants — who had never taken psychedelics previously — said their psychedelic sessions were among the most meaningful experiences of their lives.
“These studies, among others, renewed scientific interest in psychedelics and, accordingly, research into their effects has continued to grow since,” Jacob S. Aday and colleagues write in a 2019 study published in Drug Science, Policy and Law.
In their paper, Aday and colleagues argue that 2018 may be remembered as the true turning point in psychedelic research due to “advances within science, increased public interest, and regulatory changes,” such as psilocybin receiving the “breakthrough therapy” status from the FDA.
Today, there are numerous ongoing clinical trials on the therapeutic potential of psychedelics for different conditions, including substance use disorders and mental health conditions such as depression, anxiety and post-traumatic stress disorder.
Given the growing number of studies on psychedelics, the Food and Drug Administration issued a draft guidance in June 2023 for clinical trials with psychedelic drugs, aiming to help researchers design studies that will yield more reliable results for drug development.
The systematic reviews highlighted below show that there’s a lack of robust study designs in many psychedelic clinical trials. Some have small sample sizes. Some include participants who have used psychedelics before, so when they participate in a randomized controlled clinical trial, they know whether they are receiving psychedelic treatment or a placebo. Or, some include participants who may have certain expectations due to positive coverage in the lay media, hence creating bias in the results.
If you’re covering a study about psychedelics…
It’s important for journalists to pay close attention to study design and speak with an expert who is not involved in the study.
In a February 2024 blog post from Harvard Law School’s Petrie-Flom Center, Leiden University professors Eiko I. Fried and Michiel van Elk share several challenges in psychedelic research:
- “Conclusions are dramatically overstated in many studies. This ranges from conclusions in the results sections, abstracts, and even titles of papers not consistent with the reported results.”
- “There is emerging evidence that adverse events resulting from psychedelic substances are both common and underreported.”
- Some studies don’t have control groups, which can create problems for interpreting results, “because treatments like psychedelics need to be compared against a placebo or other treatment to conclude that they work beyond the placebo effect or already existing, readily available treatments.”
- “Participants in psychedelic studies usually know if they are in the treatment or control group, which artificially increases the apparent efficacies of psychedelics in clinical studies.”
- Small sample sizes can affect the statistical power and generalizability of the findings. “Small samples also mean that results are not representative. For example, participants with severe or comorbid mental health problems are commonly excluded from psychedelic studies, and therefore results may look better in these studies than in real-world psychiatric settings.”
- Many studies do not include long-term follow-ups of participants. “Studying how these people are feeling a few days or weeks after they receive treatment is not sufficient to establish that they are indeed cured from depression.”
Fried and van Elk also have a useful checklist for assessing the quality and scientific rigor of psychedelic research in their 2023 study “History Repeating: Guidelines to Address Common Problems in Psychedelic Science,” published in the journal Therapeutic Advances in Psychopharmacology.
Journalists should also remind their audiences that the drugs are still illegal under federal law and can pose a danger to health.
In California, the number of emergency room visits involving the use of hallucinogens increased by 54% between 2016 and 2022, according to a January 2024 study published in Addiction. Meanwhile, the law enforcement seizure of psychedelic mushrooms has risen dramatically, increasing nearly four-fold between 2017 and 2022, according to a February 2024 study published in the journal Drug and Alcohol Dependence.
Below, we have curated and summarized five recent studies, mostly systematic reviews and meta-analyses, which examine various aspects of psychedelic drugs, including legislative reform; long-term effects; efficacy and safety for the treatment of anxiety, depression and PTSD; and participation of older adults in clinical trials. The research summaries are followed by recommended reading.
Research roundup
Psychedelic Drug Legislative Reform and Legalization in the US
Joshua S. Siegel, James E. Daily, Demetrius A. Perry and Ginger E. Nicol. JAMA Psychiatry, December 2022.The study: Most psychedelics are Schedule I drugs federally, but state legislative reforms are changing the prospects of the drugs’ availability for treatment and their illegal status. For a better understanding of the legislative reform landscape around Schedule I psychedelic drugs, researchers collected all bills and ballot initiatives related to psychedelic drugs that were introduced into state legislatures between 2019 and September 2022. They used publicly available sources, including BillTrack50, Ballotpedia and LexisNexis.
The findings: In total, 25 states considered 74 bills, although the bills varied widely in their framework. A majority proposed decriminalization but only a few would require medical oversight and some would not even require training or licensure, the authors write. Ten of those bills became law in seven states — Colorado, Connecticut, Hawaii, New Jersey, Oregon, Texas and Washington. As of August 1, 2022, 32 bills were dead and 32 remained active.
The majority of the bills — 67 of them — referred to psilocybin; 27 included both psilocybin and MDMA; 43 proposed decriminalization of psychedelic drugs.
To predict the future legalization of psychedelics, the authors also created two models based on existing medical and recreational marijuana reform. Using 2020 as the year of the first psychedelic decriminalization in Oregon, their models predict that 26 states will legalize psychedelics between 2033 and 2037.
In the authors’ words: “Despite the relative rapidity with which some have embraced psychedelics as legitimate medical treatments, critical questions about the mechanism of action, dosing and dose frequency, durability of response to repeated treatments, drug-drug interactions, and the role psychotherapy plays in therapeutic efficacy remain unanswered. This last point is critical, as a significant safety concern associated with drugs like psilocybin, MDMA, or LSD is the suggestibility and vulnerability of the patient while under the influence of the drug. Thus, training and clinical oversight is necessary to ensure safety and also therapeutic efficacy for this divergent class of treatments.”
Who Are You After Psychedelics? A Systematic Review and a Meta-Analysis of the Magnitude of Long-Term Effects of Serotonergic Psychedelics on Cognition/Creativity, Emotional Processing and Personality
Ivana Solaja, et al. Neuroscience & Behavioral Reviews, March 2024.The study: Many anecdotal reports and observational studies have reported that psychedelics, even at microdoses, which are roughly one-tenth of a typical recreational dose, may enhance certain aspects of cognition and/or creativity, including coming up with new, useful ideas. Cognition is a “range of intellectual functions and processes involved in our ability to perceive, process, comprehend, store and react to information,” the authors explain. There are established relationships between impaired cognitive functioning and mental health disorders.
Due to limitations such as a lack of rigorous study designs, various populations in the studies and lack of documented dosage, it’s difficult to draw any conclusions about changes that last at least one week as a result of consuming psychedelics.
The authors screened 821 studies and based on the criteria they had set, found 10 to be eligible for the review and meta-analysis. The drugs in the studies include psilocybin, ayahuasca and LSD.
The findings: Overall, there was little evidence that these psychedelics have lasting effects on creativity. Also, there was not sufficient evidence to determine if this group of psychedelics enhances cognition and creativity in healthy populations or improves cognitive deficits in the study populations.
Pooled data from three studies showed lasting improvement in emotional processing — perceiving, expressing and managing emotions.
The studies offered little evidence suggesting lasting effects of psychedelics on personality traits.
In the authors’ words: “Results from this study showed very limited evidence for any lasting beneficial effects across these three psychological constructs. However, preliminary meta-analytic evidence suggested that these drugs may have the potential to cause lasting improvement in emotional recognition time. Future studies investigating these constructs should employ larger sample sizes, better control conditions, standardized and validated measures and longer-term follow-ups.”
The Impact of Psychedelics on Patients with Alcohol Use Disorder: A Systematic Review with Meta-Analysis
Dakota Sicignano, et al. Current Medical Research and Opinion, December 2023.The study: Researchers are exploring the psychedelics’ potential for the treatment of alcohol use disorder, which affected nearly 30 million Americans in 2022. The authors of this study searched PubMed from 1960 to September 2023 for studies on the use of psychedelics to treat alcohol use disorder. Out of 174 English-language studies, they selected six studies that met the criteria for their analysis.
The findings: LSD and psilocybin are promising therapies for alcohol use disorder, the authors report. However, five of the six trials were conducted in the 1960s and 1970s and may not reflect the current treatment views. Also, four of the six studies included patients who had used psychedelics before participating in the study, increasing the risk of bias.
In the authors’ words: “Despite the existence of several clinical trials showing relatively consistent benefits of psychedelic therapy in treating alcohol use disorder, there are important limitations in the dataset that must be appreciated and that preclude a conclusive determination of its value for patient care at this time.”
Older Adults in Psychedelic-Assisted Therapy Trials: A Systematic Review
Lisa Bouchet, et al. Journal of Psychopharmacology, January 2024.The study: People 65 years and older have been underrepresented in clinical trials involving psychedelics, including the use of psilocybin for the treatment of depression and anxiety. About 15% of adults older than 60 suffer from mental health issues, the authors note. They wanted to quantify the prevalence of older adults enrolled in psychedelic clinical trials and explore safety data in this population. They searched for English-language studies in peer-reviewed journals from January 1950 to September 2023. Of 4,376 studies, the authors selected 36. The studies involved psilocybin, MDMA, LSD, ayahuasca, and DPT (dipropyltryptamine), which is a less-studied synthetic hallucinogen.
The findings: Of the 1,400 patients participating in the selected studies, only 19 were 65 and older. Eighteen received psychedelics for distress related to cancer or other life-threatening illnesses. In a trial of MDMA-assisted therapy for PTSD, only one older adult was included. Adverse reactions to the drugs among older patients, including heart and gastrointestinal issues were resolved within two days and didn’t have a long-lasting impact.
In the authors’ words: “Although existing data in older adults is limited, it does provide preliminary evidence for the safety and tolerability of [psychedelic-assisted therapy] in older patients, and as such, should be more rigorously studied in future clinical trials.”
Efficacy and Safety of Four Psychedelic-Assisted Therapies for Adults with Symptoms of Depression, Anxiety, and Posttraumatic Stress Disorder: A Systematic Review and Meta-Analysis
Anees Bahji, Isis Lunsky, Gilmar Gutierrez and Gustavo Vazquez. Journal of Psychoactive Drugs, November 2023.The study: LSD, psilocybin, ayahuasca and MDMA have been approved for clinical trials on psychedelic-assisted therapy of mental health conditions in Canada and the U.S. However, major medical associations, including the American Psychiatric Association, have argued that there is insufficient scientific evidence to endorse these drugs for treating mental health disorders. To better understand the current evidence, researchers reviewed 18 blinded, randomized controlled trials, spanning 2008 through 2023. Most studies were conducted in the U.S. or Switzerland.
The findings: The studies overall suggest preliminary evidence that psychedelic drugs are mostly well-tolerated. Psilocybin and MDMA therapies may offer relief from depression and PTSD symptoms for at least a year. Most studies also used therapy and psychological support along with psychedelics.
In the authors’ words: “Despite the promising evidence presented by our study and previous reviews in the field, the evidence base remains limited and underpowered. Long-term efficacy and safety data are lacking,” the authors write. “Future steps should encourage and highlight the need for more robust larger scale randomized controlled trials with longer follow-up periods, and efforts to address regulatory and legal barriers through the collaborations between researchers, healthcare professionals, regulatory bodies, and policymakers.”
This article first appeared on The Journalist’s Resource and is republished here under a Creative Commons license.
Share This Post
-
Cavolo Nero & Sweet Potato Hash
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
🎶 Sweet potato hash? It’s a seasonal smash… Catches on in a flash… Let’s do the hash 🎶
You will need
- 6 oz cavolo nero, tough stems removed, chopped
- 1 large sweet potato, diced
- 1 large red onion, finely chopped
- 1 parsnip, grated
- 1 small red pepper, chopped
- 4 oz baby portobello mushrooms, chopped
- ½ cup fresh or thawed peas
- ¼ bulb garlic, thinly sliced
- 1 tbsp nutritional yeast
- 2 tsp black pepper, coarse ground
- 1 tsp dried rosemary
- 1 tsp dried thyme (dried for convenience; fresh is also fine if you have it)
- 1 tsp red chili flakes (dried for convenience; fresh is also fine if you have it)
- 1 tsp ground turmeric
- ½ tsp MSG or 1 tsp low-sodium salt
- Extra virgin olive oil
Method
(we suggest you read everything at least once before doing anything)
1) Preheat the oven to 425℉ / 220℃.
2) Toss the diced sweet potato in 1 tbsp olive oil, as well as the nutritional yeast, ground turmeric, black pepper, and MSG/salt, ensuring an even distribution. Roast in the oven on a lined baking tray, for 30 minutes, turning at least once to get all sides of the potato. When it is done, remove from the oven and set aside.
3) Heat a little oil in a sauté pan or large skillet (either is fine; we’re not adding liquids today), and fry the onion, parsnip, and pepper until softened, which should take about 5 minutes (this is one reason why we grated the parsnip; the other is for the variation in texture).
4) Add the garlic, mushrooms, herbs, and chili flakes, and cook for a further 1 minute, while stirring.
5) Add the cavolo nero and peas, stir until the cavolo nero begins to wilt, and then…
6) Add the roasted sweet potato; cook for about 5 more minutes, pressing down with the spatula here and there to mash the ingredients together.
7) Turn the hash over when it begins to brown on the bottom, to lightly brown the other side too.
8) Serve hot.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Brain Food? The Eyes Have It!
- Which Bell Peppers To Pick?
- Ergothioneine: “The Longevity Vitamin” (That’s Not A Vitamin)
- Our Top 5 Spices: How Much Is Enough For Benefits?
- What’s Your Plant Diversity Score?
Take care!
Share This Post
Related Posts
-
5 Things To Know About Passive Suicidal Ideation
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
If you’ve ever wanted to go to sleep and never wake up, or have some accident/incident/illness take you with no action on your part, or a loved one has ever expressed such thoughts/feelings to you… Then this video is for you. Dr. Scott Eilers explains:
Tired of living
We’ll not keep them a mystery; here are the five things that Dr. Eilers wants us to know about passive suicidal ideation:
- What it is: a desire for something to end your life without taking active steps. While it may seem all too common, it’s not necessarily inevitable or unchangeable.
- What it means in terms of severity: it isn’t a clear indicator of how severe someone’s depression is. It doesn’t necessarily mean that the person’s depression is mild; it can be severe even without active suicidal thoughts, or indeed, suicidality at all.
- What it threatens: although passive suicidal ideation doesn’t usually involve active planning, it can still be dangerous. Over time, it can evolve into active suicidal ideation or lead to risky behaviors.
- What it isn’t: passive suicidal ideation is different from intrusive thoughts, which are unwanted, distressing thoughts about death. The former involves a desire for death, while the latter does not.
- What it doesn’t have to be: passive suicidal ideation is often a symptom of underlying depression or a mood disorder, which can be treated through therapy, medication, or a combination of both. Seeking treatment is crucial and can be life-changing.
For more on all of the above, here’s Dr. Eilers with his own words:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
- The Mental Health First Aid You’ll Hopefully Never Need ← about depression generally
- How To Stay Alive (When You Really Don’t Want To) ← about suicidality specifically
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Art and Science of Connection – by Kasley Killam, MPH
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We can eat well, exercise well, and even sleep well, and we’ll still have a +53% increased all-cause mortality if we lack social connection—even if we technically have support and access to social resources, just not the real human connection itself. And as we get older, it gets increasingly easy to find ourselves isolated.
The author is a social scientist by profession, and it shows. None of what she shares in the book is wishy-washy; it has abundant scientific references coming thick and fast, and a great deal of clarity with regard to terms, something often not found in books of this genre that lean more towards the art than the science.
On which note, for the reader who may be thinking “I am indeed quite alone”, she also offers proven techniques for remedying that; not in the way that many books use the word “proven” to mean “we got some testimonials”, but rather, proven in the sense of “we did science to it and based on these 17 large population-based retrospective cohort studies, we can say with 99% confidence that this is an effective tool to mediate improved social bonds and social health outcomes”.
To this end, it’s a very practical book also, and should bestow upon any isolated reader a sense of confidence that in fact, things can be better. A particular strength is that it also looks at many different scenarios, so for the “what if I…” people with clear reasons why social connection is not abundantly available, yes, she has such cases covered too.
Bottom line: if you’d like to live more healthily for longer, social health is an underrated and oft-forgotten way of greatly increasing those things, by science.
Click here to check out The Art And Science Of Social Connection, and get connected!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Homeopathy: Evidence So Tiny That It’s Not there?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Homeopathy: Evidence So Tiny That It’s Not There?
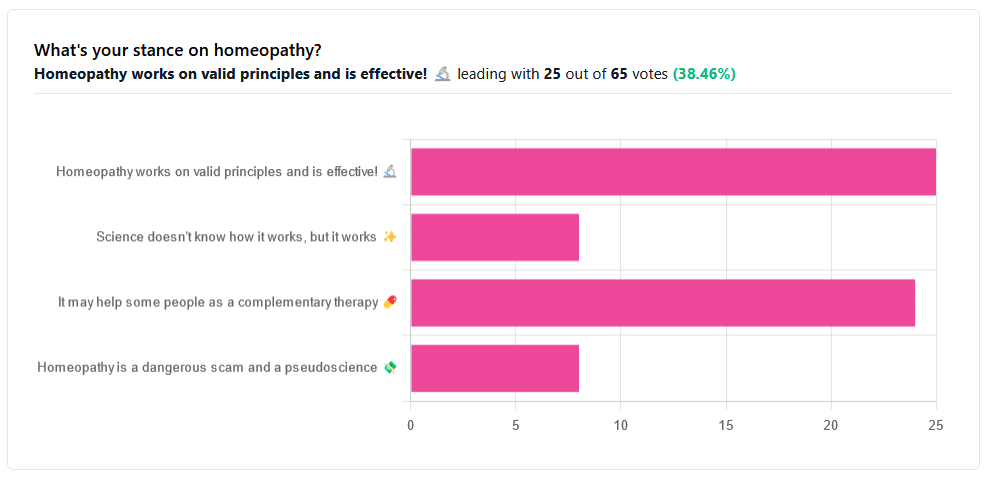
Yesterday, we asked you your opinions on homeopathy. The sample size of responses was a little lower than we usually get, but of those who did reply, there was a clear trend:
- A lot of enthusiasm for “Homeopathy works on valid principles and is effective”
- Near equal support for “It may help some people as a complementary therapy”
- Very few people voted for “Science doesn’t know how it works, but it works”; this is probably because people who considered voting for this, voted for the more flexible “It may help some people as a complementary therapy” instead.
- Very few people considered it a dangerous scam and a pseudoscience.
So, what does the science say?
Well, let us start our investigation by checking out the position of the UK’s National Health Service, an organization with a strong focus on providing the least expensive treatments that are effective.
Since homeopathy is very inexpensive to arrange, they will surely want to put it atop their list of treatments, right?
❝Homeopathy is a “treatment” based on the use of highly diluted substances, which practitioners claim can cause the body to heal itself.
There’s been extensive investigation of the effectiveness of homeopathy. There’s no good-quality evidence that homeopathy is effective as a treatment for any health condition.❞
The NHS actually has a lot more to say about that, and you can read their full statement here.
But that’s just one institution. Here’s what Australia’s National Health and Medical Research Council had to say:
❝There was no reliable evidence from research in humans that homeopathy was effective for treating the range of health conditions considered: no good-quality, well-designed studies with enough participants for a meaningful result reported either that homeopathy caused greater health improvements than placebo, or caused health improvements equal to those of another treatment❞
You can read their full statement here.
The American FDA, meanwhile, have a stronger statement:
❝Homeopathic drug products are made from a wide range of substances, including ingredients derived from plants, healthy or diseased animal or human sources, minerals and chemicals, including known poisons. These products have the potential to cause significant and even permanent harm if they are poorly manufactured, since that could lead to contaminated products or products that have potentially toxic ingredients at higher levels than are labeled and/or safe, or if they are marketed as substitute treatments for serious or life-threatening diseases and conditions, or to vulnerable populations.❞
You can read their full statement here.
Homeopathy is a dangerous scam and a pseudoscience: True or False?
False and True, respectively, mostly.
That may be a confusing answer, so let’s elaborate:
- Is it dangerous? Mostly not; it’s mostly just water. However, two possibilities for harm exist:
- Careless preparation could result in a harmful ingredient still being present in the water—and because of the “like cures like” principle, many of the ingredients used in homeopathy are harmful, ranging from heavy metals to plant-based neurotoxins. However, the process of “ultra-dilution” usually removes these so thoroughly that they are absent or otherwise scientifically undetectable.
- Placebo treatment has its place, but could result in “real” treatment going undelivered. This can cause harm if the “real” treatment was critically needed, especially if it was needed on a short timescale.
- Is it a scam? Probably mostly not; to be a scam requires malintent. Most practitioners probably believe in what they are practising.
- Is it a pseudoscience? With the exception that placebo effect has been highly studied and is a very valid complementary therapy… Yes, aside from that it is a pseudoscience. There is no scientific evidence to support homeopathy’s “like cures like” principle, and there is no scientific evidence to support homeopathy’s “water memory” idea. On the contrary, they go against the commonly understood physics of our world.
It may help some people as a complementary therapy: True or False?
True! Not only is placebo effect very well-studied, but best of all, it can still work as a placebo even if you know that you’re taking a placebo… Provided you also believe that!
Science doesn’t know how it works, but it works: True or False?
False, simply. At best, it performs as a placebo.
Placebo is most effective when it’s a remedy against subjective symptoms, like pain.
However, psychosomatic effect (the effect that our brain has on the rest of our body, to which it is very well-connected) can mean that placebo can also help against objective symptoms, like inflammation.
After all, our body, directed primarily by the brain, can “decide” what immunological defenses to deploy or hold back, for example. This is why placebo can help with conditions as diverse as arthritis (an inflammatory condition) or diabetes (an autoimmune condition, and/or a metabolic condition, depending on type).
Here’s how homeopathy measures up, for those conditions:
(the short answer is “no better than placebo”)
Homeopathy works on valid principles and is effective: True or False?
False, except insofar as placebo is a valid principle and can be effective.
The stated principles of homeopathy—”like cures like” and “water memory”—have no scientific basis.
We’d love to show the science for this, but we cannot prove a negative.
However, the ideas were conceived in 1796, and are tantamount to alchemy. A good scientific attitude means being open-minded to new ideas and testing them. In homeopathy’s case, this has been done, extensively, and more than 200 years of testing later, homeopathy has consistently performed equal to placebo.
In summary…
- If you’re enjoying homeopathic treatment and that’s working for you, great, keep at it.
- If you’re open-minded to enjoying a placebo treatment that may benefit you, be careful, but don’t let us stop you.
- If your condition is serious, please do not delay seeking evidence-based medical treatment.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: