52 Ways to Walk – by Annabel Streets
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Most of us learned to walk at a very young age and probably haven’t thought much about it since, except perhaps in a case where some injury made it difficult.
Annabel Streets provides a wonderful guide to not just taking up (or perhaps reclaiming) the joy of walking, but also the science of it in more aspects than most of us have considered:
- The physical mechanics of walking—what’s best?
- Boots or shoes? Barefoot?
- Roads, grass, rougher vegetation… Mud?
- Flora & fauna down to the microbiota that affect us
- How much walking is needed, to be healthy?
- Is there such a thing as too much walking?
- What are the health benefits (or risks) of various kinds of weather?
- Is it better to walk quickly or to walk far?
- What about if we’re carrying some injury?
- What’s going on physiologically when we walk?
- And so much more…
Streets writes with a captivating blend of poetic joie-de-vivre coupled with scientific references.
One moment the book is talking about neuroradiology reports of NO-levels in our blood, the impact of Mycobacterium vaccae, and the studied relationship between daily steps taken and production of oligosaccharide 3′-sialyllactose, and the next it’s all:
“As if the newfound lightness in our limbs has crept into our minds, loosening our everyday cares and constraints…”
And all in all, this book helps remind us that sometimes, science and a sense of wonder can and do (and should!) walk hand-in-hand.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Night School – by Dr. Richard Wiseman
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sleep is a largely neglected part of health for most people. Compared to factors like food and exercise, it’s something that experientially we’re mostly not present for! Little wonder then that we also often feel like it’s outside of our control.
While Dr. Wiseman does cover the usual advices with regard to getting good sleep, this book has a lot more than that.
Assuming that they go beyond the above, resources about sleep can usually be divided into one of two categories:
- Hard science: lots about brainwaves, sleep phases, circadian rhythms, melatonin production, etc… But nothing very inspiring!
- Fantastical whimsy: lots about dreams, spiritualism, and not a scientific source to be found… Nothing very concrete!
This book does better.
We get the science and the wonder. When it comes to lucid dreaming, sleep-learning, sleep hypnosis, or a miraculously reduced need for sleep, everything comes with copious scientific sources or not at all. Dr. Wiseman is well-known in his field for brining scientific skepticism to paranormal claims, by the way—so it’s nice to read how he can do this without losing his sense of wonder. Think of him as the Carl Sagan of sleep, perhaps.
Style-wise, the book is pop-science and easy-reading. Unsurprising, for a professional public educator and science-popularizer.
Structurally, the main part of the book is divided into lessons. Each of these come with background science and principles first, then a problem that we might want to solve, then exercises to do, to get the thing we want. It’s at once a textbook and an instruction manual.
Bottom line: this is a very inspiring book with a lot of science. Whether you’re looking to measurably boost your working memory or heal trauma through dreams, this book has everything.
Click here to check out Night School and learn what your brain can do!
Share This Post
-
7 Signs of Undiagnosed Autism in Adults
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
When it comes to adults and autism, there are two kinds of person in the popular view: those who resemble the Rain Man, and those who are making it up. But, it’s not so, as Paul Micallef explains:
The signs
We’ll not keep them a mystery; they are:
- Social interaction difficulties: such a person may struggle with understanding social cues, leading to awkwardness, isolation, or appearing eccentric.
- Need for structure and routine: either highly structured or disorganized, both of which stem from executive function challenges. The former, of course, is a coping mechanism, while the latter is the absence of same.
- Sensory sensitivities: can include sensitivities or insensitivities to light, sound, temperature, smells, tastes, and so forth.
- Spiky skillset: extreme strengths in certain areas, coupled with significant difficulties in others, leading to uneven abilities. May be able to dismantle and rebuild a PC, while not knowing how to arrange an Über.
- Emotional regulation issues: experiences of meltdowns, shutdowns, or withdrawal as coping mechanisms when overwhelmed. Not that this is “or”, not necessarily “and”. The latter goes especially unnoticed as an emotional regulation issue, because for everyone else, it’s something that’s not there to see.
- Unusual associations: making mental connections or associations that seem random or uncommon compared to others. The mind went to 17 places quickly and while everyone else got from idea A to idea B, this person is already at idea Q.
- Being “just different”: a general sense of being the odd one out, standing out in subtle or distinct ways. This is rather a catch-all, but if there’s someone who fits this, there’s a good chance, the other things apply too.
For more on all of these, whether pertaining to yourself or a loved one (or both!), enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
- 16 Overlooked Autistic Traits In Women
- What is AuDHD? 5 important things to know when someone has both autism and ADHD
Take care!
Share This Post
-
Fix Tight Hamstrings In Just 3 Steps
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
There’s a better way to increase your flexibility than just stretching and stretching and hoping for the best. Here’s a 3-step method that will transform your flexibility:
As easy as 1-2-3
Only one part actually involves stretching:
Step 1: reciprocal inhibition
- Concept: when one muscle contracts, the opposing muscle relaxes—which is what we need.
- Goal: engage hip flexors to encourage hamstring relaxation.
- Method:
- Kneeling hamstring stretch position with one leg forward.
- Support with yoga blocks or a chair; use a cushion for comfort.
- Maintain a slight arch in the lower back and hinge forward slightly.
- Attempt to lift the foot off the floor, even if it doesn’t move.
- Hold for around 10 seconds.
Step 2: engaging more muscle fibers
- Concept: our muscles contain a lot of fibers, and often not all of them come along for the ride when we do something (exercising, stretching, etc), and those fibers that weren’t engaged will hold back the whole process.
- Goal: activate more fibers in the hamstring for a deeper stretch.
- Method:
- Same kneeling position, slight back arch, and forward hinge.
- Drive the heel into the floor as if trying to dent it.
- Apply significant effort but hold for only 10 seconds.
- A small bend in the knee is acceptable.
Step 3: manipulating the nervous system
- Concept: the nervous system often limits flexibility due to safety signals (causing sensations of discomfort to tell us to stop a lot sooner than we really need to).
- Goal: passive stretching to reduce nervous system resistance.
- Method:
- Avoid muscle engagement or movement—stay completely relaxed.
- Focus on calmness, with slow, steady breaths.
- Avoid signs of tension (e.g. clenched fists, short/sharp breathing). While your nervous system is trying to communicate to you that you are in danger, you need to communicate to your nervous system that this is fine actually, so in order to reassure your nervous system you need to avoid signs that will tip it off that you’re worried too.
- Don’t overstretch; prioritize a relaxed, safe feeling.
For more on all of this, plus visual demonstrations, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like:
Tight Hamstrings? Here’s A Test To Know If It’s Actually Your Sciatic Nerve
Take care!
Share This Post
Related Posts
-
Pomegranate vs Cherries – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing pomegranate to cherries, we picked the pomegranate.
Why?
In terms of macros, pomegranate is slightly higher in carbs, and/but 4x higher in fiber. That’s already a good start for pomegranates. Lest we be accused of cherry-picking, though, we’ll mention that pomegranate is also slightly higher in protein and fat, for what it’s worth—which is not a lot. As with most fruits, the protein and fat numbers are low importance next to the carb:fiber ratio.
When it comes to vitamins, pomegranate has more of vitamins B1, B2, B5, B6, B9. E. K, and choline. On the other hand, cherries have more of vitamins A and B3. The two fruits are equal in vitamin C. This all makes for a clear win for pomegranate.
In the category of minerals, pomegranate boasts more copper, magnesium, phosphorus, potassium, selenium, and zinc. In contrast, cherries have slightly more calcium. Another win for pomegranate.
Both of these fruits have beneficial polyphenols, each with a slightly different profile, but neither pressingly better than the other.
In short: as ever with healthy foods, enjoy both—diversity is good! But if you’re going to pick on, we recommend the pomegranate.
Want to learn more?
You might like to read:
- Pomegranate Peel’s Potent Potential ← so don’t throw it away!
- Cherries’ Very Healthy Wealth Of Benefits!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Spermidine For Longevity
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small 😎
❝How much evidence is there behind the longevity-related benefit related to spermidine, and more specifically, does it cause autophagy?❞
A short and simple answer to the latter question: yes, it does:
Spermidine: a physiological autophagy inducer acting as an anti-aging vitamin in humans?
For anyone wondering what autophagy is: it’s when old cells are broken down and consumed by the body to make new ones. Doing this earlier rather than later means that the genetic material is not yet so degraded when it is copied, and so the resultant new cell(s) will be “younger” than if the previous cell(s) had been broken down and recycled when older.
Indeed, we have written previously about senolytic supplements such as fisetin, which specialize in killing senescent (aging) cells earlier:
Fisetin: The Anti-Aging Assassin
As for spermidine and longevity, because of its autophagy-inducing properties, it’s considered a caloric restriction mimetic, that is to say, it has the same effect on a cellular level as caloric restriction. And yes, while it’s not an approach we regularly recommend here (usually preferring intermittent fasting as a CR-mimetic), caloric restriction is a way to fight aging:
Is Cutting Calories The Key To Healthy Long Life?
As for how spermidine achieves similarly:
Spermidine delays aging in humans
However! Both of the scientific papers on spermidine use in humans that we’ve cited so far today have conflict of interests statements made with regard to the funding of the studies, which means there could be some publication bias.
To that end, let’s look at a less glamorous study (e.g. no “in humans” in the title because, like most longevity studies, it’s with non-human animals with naturally short lifespans such as mice and rats), like this one that finds it to be both cardioprotective and neuroprotective and having many anti-aging benefits mediated by inducing autophagy:
A review on polyamines as promising next-generation neuroprotective and anti-aging therapy
(the polyamines in question are spermidine and putrescine, which latter is a similar polyamine)
Lastly, let’s answer a few likely related questions, so that you don’t have to Google them:
Does spermidine come from sperm?
Amongst other places (including some foods, which we’ll come to in a moment), yes, spermidine is normally found in semen (in fact, it’s partly responsible for the normal smell, though other factors influence the overall scent, such as diet, hormones, and other lifestyle factors such as smoking, alcohol use etc) and that is how/where it was first identified.
Does that mean that consuming semen is good for longevity?
Aside from the health benefits of a healthy sex life… No, not really. Semen does contain spermidine (as discussed) as well as some important minerals, but you’d need to consume approximately 1 cup of semen to get the equivalent spermidine you’d get from 1 tbsp of edamame (young soy) beans.
Unless your lifestyle is rather more exciting than this writer’s, it’s a lot easier to get 1 tbsp of edamame beans than 1 cup of semen.
Here are how some top foods stack up, by the way—we admittedly cherry-picked from the near top of the list, but wheatgerm is an even better source, with cheddar cheese and mushrooms (it was shiitake in the study) coming after soy:
Frontiers in Nutrition | Polyamines in Food
Alternatively, if you prefer to just take it in supplement form, here’s an example product on Amazon, giving 5mg per capsule (which is almost as much as the 1 cup of semen or 1 tbsp of edamame that we mentioned earlier).
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
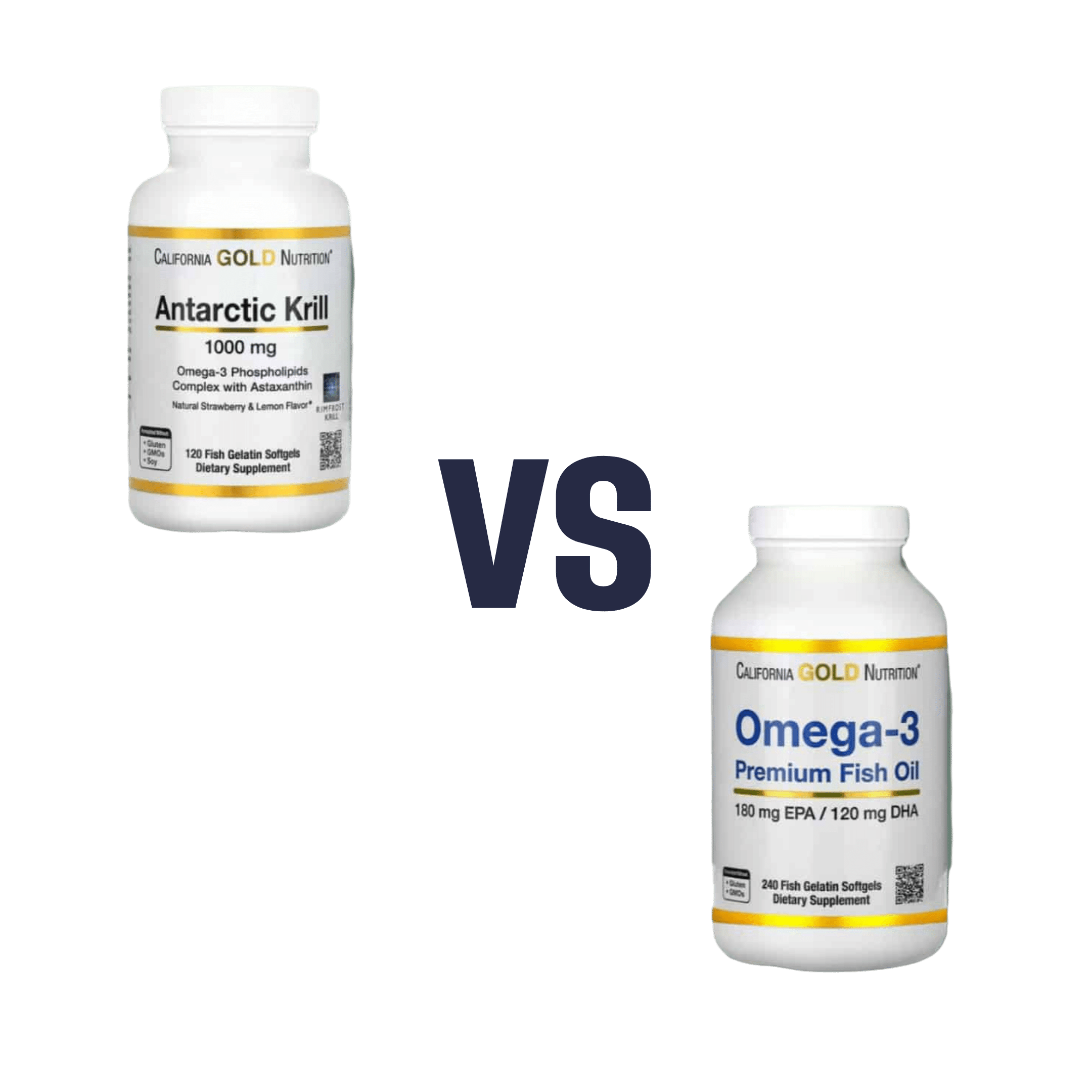
Krill Oil vs Fish Oil – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing krill oil to fish oil, we picked the krill oil.
Why?
Both of these products are good sources of omega-3 fatty acids EPA and DHA, and for the specific brand depicted above, in both cases 2 softgels will give you the recommended daily amount (which is generally held to be 250–500mg combined omega-3s per day).
This brand’s fish oil gives more (640mg combined omega-3s per 2 softgels, to the same brand’s krill oil’s 480mg per 2 softgels), but since the krill oil is already in the high end of RDA territory, the excess beyond the RDA is not helpful, and not a huge factor. More quantity is not always better, when the body can only process so much at a time.
However, the krill oil gives some extra things that the fish oil doesn’t:
- Astaxanthin, a “super-antioxidant”
- and neuroprotectant, heart-healthy phospholipids
Additional considerations
We have declared “the winner” based on health considerations only. That’s a sticking point for us in all our writings; we’ll occasionally look at and mention other factors, but we know that health is what you’re here for, so that’s what we’ll always treat as most critical.
However, in case these factors may interest you and/or influence you to one or the other:
• The fish oil is about 30% cheaper financially
• The krill oil is a lot more sustainable environmentallyBack to the health science…
Read more:
• What Omega-3 Fatty Acids Really Do For Us
• Astaxanthin: Super-Antioxidant & NeuroprotectantWant some? Here for your convenience are some example products on Amazon:
(brands available will vary per region, but now you know what to look out for on the labels!)
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: