Ozempic’s cousin drug liraglutide is about to get cheaper. But how does it stack up?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fourteen years ago, the older drug cousin of semaglutide (Ozempic and Wegovy) came onto the market. The drug, liraglutide, is sold under the brand names Victoza and Saxenda.
Patents for Victoza and Saxenda have now expried. So other drug companies are working to develop “generic” versions. These are likely be a fraction of current cost, which is around A$400 a month.
So how does liraglutide compare with semaglutide?

How do these drugs work?
Liraglutide was not originally developed as a weight-loss treatment. Like semaglutide (Ozempic), it originally treated type 2 diabetes.
The class of drugs liraglutide and semaglutide belong to are known as GLP-1 mimetics, meaning they mimic the natural hormone GLP-1. This hormone is released from your small intestines in response to food and acts in several ways to improve the way your body handles glucose (sugar).
How do they stop hunger?
Liraglutide acts in several regions of the unconscious part of your brain, specifically the hypothalamus, which controls metabolism, and parts of the brain stem responsible for communicating your body’s nutrient status to the hypothalamus.
Its actions here appear to reduce hunger in two different ways. First, it helps you to feel full earlier, making smaller meals more satisfying. Second, it alters your “motivational salience” towards food, meaning it reduces the amount of food you seek out.
Liraglutide’s original formulation, designed to treat type 2 diabetes, was marketed as Victoza. Its ability to cause weight loss was evident soon after it entered the market.
Shortly after, a stronger formulation, called Saxenda, was released, which was intended for weight loss in people with obesity.
How much weight can you lose with liraglutide?
People respond differently and will lose different amounts of weight. But here, we’ll note the average weight loss users can expect. Some will lose more (sometimes much more), others will lose less, and a small proportion won’t respond.
The first GLP-1 mimicking drug was exenatide (Bayetta). It’s still available for treating type 2 diabetes, but there are currently no generics. Exenatide does provide some weight loss, but this is quite modest, typically around 3-5% of body weight.
For liraglutide, those using the drug to treat obesity will use the stronger one (Saxenda), which typically gives about 10% weight loss.
Semaglutide, with the stronger formulation called Wegovy, typically results in 15% weight loss.
The newest GLP-1 mimicking drug on the market, tirzepatide (Mounjaro for type 2 diabetes and Zepbound for weight loss), results in weight loss of around 25% of body weight.
What happens when you stop taking them?
Despite the effectiveness of these medications in helping with weight loss, they do not appear to change people’s weight set-point.
So in many cases, when people stop taking them, they experience a rebound toward their original weight.
What is the dose and how often do you need to take it?
Liraglutide (Victoza) for type 2 diabetes is exactly the same drug as Saxenda for weight loss, but Saxenda is a higher dose.
Although the target for each formulation is the same (the GLP-1 receptor), for glucose control in type 2 diabetes, liraglutide has to (mainly) reach the pancreas.
But to achieve weight loss, it has to reach parts of the brain. This means crossing the blood-brain barrier – and not all of it makes it, meaning more has to be taken.
All the current formulations of GLP-1 mimicking drug are injectables. This won’t change when liraglutide generics hit the market.
However, they differ in how frequently they need to be injected. Liraglutide is a once-daily injection, whereas semaglutide and tirzepatide are once-weekly. (That makes semaglutide and tirzepatide much more attractive, but we won’t see semaglutide as a generic until 2033.)
What are the side effects?
Because all these medicines have the same target in the body, they mostly have the same side effects.
The most common are a range of gastrointestinal upsets including nausea, vomiting, bloating, constipation and diarrhoea. These occur, in part, because these medications slow the movement of food out of the stomach, but are generally managed by increasing the dose slowly.
Recent clinical data suggests the slowing in emptying of the stomach can be problematic for some people, and may increase the risk of of food entering the lungs during operations, so it is important to let your doctor know if you are taking any of these drugs.
Because these are injectables, they can also lead to injection-site reactions.

During clinical trials, there were some reports of thyroid disease and pancreatitis (inflammation of the pancreas). However, it is not clear that these can be attributed to GLP-1 mimicking drugs.
In animals, GLP-1 mimicking drugs drugs have been found to negatively alter the growth of the embryo. There is currently no controlled clinical trial data on their use during pregnancy, but based on animal data, these medicines should not be used during pregnancy.
Who can use them?
The GLP-1 mimicking drugs for weight loss (Wegovy, Saxenda, Zepbound/Mounjaro) are approved for use by people with obesity and are meant to only be used in conjunction with diet and exercise.
These drugs must be prescribed by a doctor and for obesity are not covered by the Pharmaceutical Benefits Scheme, which is one of the reasons why they are expensive. But in time, generic versions of liraglutide are likely to be more affordable.
Sebastian Furness, ARC Future Fellow, School of Biomedical Sciences, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Wakefulness, Cognitive Enhancement, AND Improved Mood?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Old Drug, New Tricks?
Modafinil (also known by brand names including Modalert and Provigil) is a dopamine uptake inhibitor.
What does that mean? It means it won’t put any extra dopamine in your brain, but it will slow down the rate at which your brain removes naturally-occuring dopamine.
The result is that your brain will get to make more use of the dopamine it does have.
(dopamine is a neutrotransmitter that allows you to feel wakeful and happy, and perform complex cognitive tasks)
Modafinil is prescribed for treatment of excessive daytime sleepiness. Often that’s caused by shift work sleep disorder, sleep apnea, restless leg syndrome, or narcolepsy.
Read: Overview of the Clinical Uses, Pharmacology, and Safety of Modafinil
Many studies done on humans (rather than rats) have been military experiments to reduce the effects of sleep deprivation:
Click Here To See A Military Study On Modafinil!
They’ve found modafinil to be helpful, and more effective and more long-lasting than caffeine, without the same “crash” later. This is for two reasons:
1) while caffeine works by blocking adenosine (so you don’t feel how tired you are) and by constricting blood vessels (so you feel more ready-for-action), modafinil works by allowing your brain to accumulate more dopamine (so you’re genuinely more wakeful, and you get to keep the dopamine)
2) the biological half-life of modafinil is 12–15 hours, as opposed to 4–8 hours* for caffeine.
*Note: a lot of sources quote 5–6 hours for caffeine, but this average is misleading. In reality, we are each genetically predetermined to be either a fast caffeine metabolizer (nearer 4 hours) or a slow caffeine metabolizer (nearer 8 hours).
What’s a biological half-life (also called: elimination half-life)?
A substance’s biological half-life is the time it takes for the amount in the body to be reduced by exactly half.
For example: Let’s say you’re a fast caffeine metabolizer and you have a double-espresso (containing 100mg caffeine) at 8am.
By midday, you’ll have 50mg of caffeine left in your body. So far, so simple.
By 4pm you might expect it to be gone, but instead you have 25mg remaining (because the amount halves every four hours).
By 8pm, you have 12.5mg remaining.
When midnight comes and you’re tucking yourself into bed, you still have 6.25mg of caffeine remaining from your morning coffee!
Use as a nootropic
Many healthy people who are not sleep-deprived use modafinil “off-label” as a nootropic (i.e., a cognitive enhancer).
Read: Modafinil for cognitive neuroenhancement in healthy non-sleep-deprived subjects: A systematic review
Important Note: modafinil is prescription-controlled, and only FDA-approved for sleep disorders.
To get around this, a lot of perfectly healthy biohackers describe the symptoms of sleep pattern disorder to their doctor, to get a prescription.
We do not recommend lying to your healthcare provider, and nor do we recommend turning to the online “grey market”.
Such websites often use anonymized private doctors to prescribe on an “informed consent” basis, rather than making a full examination. Those websites then dispense the prescribed medicines directly to the patient with no further questions asked (i.e. very questionable practices).
Caveat emptor!
A new mood-brightener?
Modafinil was recently tested head-to-head against Citalapram for the treatment of depression, and scored well:
See its head-to-head scores here!
How does it work? Modafinil does for dopamine what a lot of anti-depressants do for serotonin. Both dopamine and serotonin promote happiness and wakefulness.
This is very promising, especially as modafinil (in most people, at least) has fewer unwanted side-effects than a lot of common anti-depressant medications.
Share This Post
-
Building Psychological Resilience (Without Undue Hardship)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What’s The Worst That Could Happen?
When we talk about the five lifestyle factors that make the biggest difference to health, stress management would be a worthy addition as number six. We haven’t focused explicitly on that for a while, so let’s get ready to start the New Year on a good footing…
You’re not going to have a stress-free 2024
What a tender world that would be! Hopefully your stressors will be small and manageable, but rest assured, things will stress you.
And that’s key: “rest assured”. Know it now, prepare for it, and build resilience.
Sounds grim, doesn’t it? It doesn’t have to be, though.
When the forecast weather is cold and wet, you’re not afraid of it when you have a warm dry house. When the heating bill comes for that warm dry house, you’re not afraid of it when you have money to pay it. If you didn’t have the money and the warm dry house, the cold wet weather could be devastating to you.
The lesson here is: we can generally handle what we’re prepared for.
Negative visualization and the PNS
This is the opposite of what a lot of “think and grow rich”-style gurus would advise. And indeed, it’s not helpful to slide into anxious worrying.
If you do find yourself spiralling, here’s a tool for getting out of that spiral:
RAIN: an intervention for dealing with difficult emotions
For now, however, we’re going to practice Radical Acceptance.
First, some biology: you may be aware that your Central Nervous System (CNS) branches into the Sympathetic Nervous System (SNS) and the Parasympathetic Nervous System (PNS).
The PNS is the part that cues our body to relax, and suppresses our fight/flight response. We’re going to activate it.
Activating the PNS is easy for most people in comfortable circumstances (e.g., you are not currently exposed to stressful stimuli). It may well be activated already, and if it’s not, a few deep breaths is usually all it takes.
If you’d like a quick and easy Mindfulness-Based Stress Reduction (MBSR) technique, here you go:
No-Frills, Evidence-Based Mindfulness
Activating the PNS is hard for most people in difficult circumstances (e.g., you either are currently exposed to stressful stimuli, or you are in one of the emotional spirals we discussed earlier).
However, we can trick our bodies and brains by—when we are safe and unstressed—practicing imagining those stressful stimuli. Taking a moment to not just imagine it experientially, but immersively. This, in CBT and DBT, is the modern equivalent to the old samurai who simply accepted, before battle, that they were already dead—and thus went into battle with zero fear of death.
A less drastic example is the zen master who had a favorite teacup, and feared it would get broken. So he would tell himself “the cup is already broken”. One day, it actually broke, and he simply smiled ruefully and said “Of course”.
How this ties together: practice the mindfulness-based stress reduction we linked above, while imagining the things that do/would stress you the most.
Since it’s just imagination, this is a little easier than when the thing is actually happening. Practicing this way means that when and if the thing actually happens (an unfortunate diagnosis, a financial reversal, whatever it may be), our CNS is already well-trained to respond to stress with a dose of PNS-induced calm.
You can also leverage hormesis, a beneficial aspect of (in this case, optional and chosen by you) acute stress:
Dr. Elissa Epel | The Stress Prescription
Psychological resilience training
This (learned!) ability to respond to stress in an adaptive fashion (without maladaptive coping strategies such as unhelpful behavioral reactivity and/or substance use) is a key part of what in psychology is called resilience:
And yes, the CBT/DBT/MBSR methods we’ve been giving you are the evidence-based gold standard.
Only the best for 10almonds subscribers! 😎
❝That was helpful, but not cheery; can we finish the year on a cheerier note?❞
We can indeed:
How To Get Your Brain On A More Positive Track (Without Toxic Positivity)
Take care!
Share This Post
-
Corn Chips vs Potato Chips: Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing corn chips to potato chips, we picked the corn chips.
Why?
First, let it be said, this was definitely a case of “lesser evil voting” as there was no healthy choice here. But as for which is relatively least unhealthy…
Most of the macronutrient and micronutrient profile is quite similar. Both foods are high carb, moderately high fat, negligible protein, and contain some trace minerals and even some tiny amounts of vitamins. Both are unhealthily salty.
Exact numbers will of course vary from one brand’s product to another, but you can see some indicative aggregate scores here in the USDA’s “FoodData Central” database:
The biggest health-related difference that doesn’t have something to balance it out is that the glycemic index of corn chips averages around 63, whereas the glycemic index of potato chips averages around 70 (that is worse).
That’s enough to just about tip the scales in favor of corn chips.
The decision thus having been made in favor of corn chips (and the next information not having been part of that decision), we’ll mention one circumstantial extra benefit to corn chips:
Corn chips are usually eaten with some kind of dip (e.g. guacamole, sour cream, tomato salsa, etc) which can thus deliver actual nutrients. Potato chips meanwhile are generally eaten with no additional nutrients. So while we can’t claim the dip as being part of the nutritional make-up of the corn chips, we can say:
If you’re going to have a habit of eating one or the other, then corn chips are probably the least unhealthy of the two.
And yes, getting vegetables (e.g. in the dips) in ways that are not typically associated with “healthy eating” is still better than not getting vegetables at all!
Check out: Level-Up Your Fiber Intake! (Without Difficulty Or Discomfort)
Share This Post
Related Posts
-
Laziness Does Not Exist – by Dr. Devon Price
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Some cultures prize productivity as an ideal above most other things, and it’s certainly so in the US. Not only is this not great for mental health in general, but also—as Dr. Price explains—it’s based on a lie.
Generally speaking, when a person appears lazy there is something stopping them/you from doing better, and it’s not some mystical unseen force of laziness, not a set character trait, not a moral failing. Rather, the root cause may be physical, psychological, socioeconomic, or something else entirely.
Those causes can in some cases be overcome (for example, a little CBT can often set aside perfectionist anxiety that results in procrastination), and in some cases they can’t, at least on an individual level (disabilities often stubbornly remain disabling, and societal problems require societal solutions).
This matters for our mental health in areas well beyond the labor marketplace, of course, and these ideas extend to personal projects and even personal relationships. Whatever it is, if it’s leaving you exhausted, then probably something needs to be changed (even if the something is just “expectations”).
The book does offer practical solutions to all manner of such situations, improving what can be improved, making easier what can be made easier, and accepting what just needs to be accepted.
The style of this book is casual yet insightful and deep, easy-reading yet with all the acumen of an accomplished social psychologist.
Bottom line: if life leaves you exhausted, this book can be the antidote and cure
Click here to check out Laziness Does Not Exist, and break free!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What is mitochondrial donation? And how might it help people have a healthy baby one day?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Mitochondria are tiny structures in cells that convert the food we eat into the energy our cells need to function.
Mitochondrial disease (or mito for short) is a group of conditions that affect this ability to generate the energy organs require to work properly. There are many different forms of mito and depending on the form, it can disrupt one or more organs and can cause organ failure.
There is no cure for mito. But an IVF procedure called mitochondrial donation now offers hope to families affected by some forms of mito that they can have genetically related children free from mito.
After a law to allow mitochondrial donation in Australia was passed in 2022, scientists are now preparing for a clinical trial to see if mitochondrial donation is safe and works.
Jonathan Borba/Pexels What is mitochondrial disease?
There are two types of mitochondrial disease.
One is caused by faulty genes in the nuclear DNA, the DNA we inherit from both our parents and which makes us who we are.
The other is caused by faulty genes in the mitochondria’s own DNA. Mito caused by faulty mitochondrial DNA is passed down through the mother. But the risk of disease is unpredictable, so a mother who is only mildly affected can have a child who develops serious disease symptoms.
Mitochondrial disease is the most common inherited metabolic condition affecting one in 5,000 people.
Some people have mild symptoms that progress slowly, while others have severe symptoms that progress rapidly. Mito can affect any organ, but organs that need a lot of energy such as brain, muscle and heart are more often affected than other organs.
Mito that manifests in childhood often involves multiple organs, progresses rapidly, and has poor outcomes. Of all babies born each year in Australia, around 60 will develop life-threatening mitochondrial disease.
What is mitochondrial donation?
Mitochondrial donation is an experimental IVF-based technique that offers people who carry faulty mitochondrial DNA the potential to have genetically related children without passing on the faulty DNA.
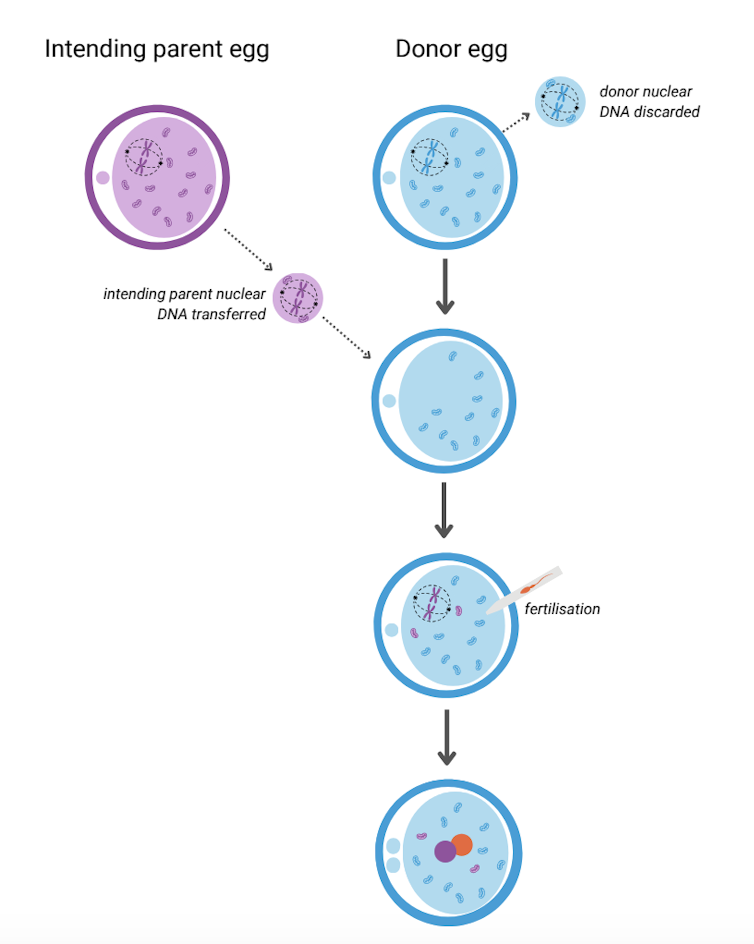
It involves removing the nuclear DNA from the egg of someone who carries faulty mitochondrial DNA and inserting it into a healthy egg donated by someone not affected by mito, which has had its nuclear DNA removed.
The donor egg (in blue) has had its nuclear DNA removed. Author provided The resulting egg has the nuclear DNA of the intending parent and functioning mitochondria from the donor. Sperm is then added and this allows the transmission of both intending parents’ nuclear DNA to the child.
A child born after mitochondrial donation will have genetic material from the three parties involved: nuclear DNA from the intending parents and mitochondrial DNA from the egg donor. As a result the child will likely have a reduced risk of mito, or no risk at all.
The procedure removes the faulty DNA to reduce the chance of it passing on to the baby. Josh Willink/Pexels This highly technical procedure requires specially trained scientists and sophisticated equipment. It also requires both the person with mito and the egg donor to have hormone injections to stimulate the ovaries to produce multiple eggs. The eggs are then retrieved in an ultrasound-guided surgical procedure.
Mitochondrial donation has been pioneered in the United Kingdom where a handful of babies have been born as a result. To date there have been no reports about whether they are free of mito.
Maeve’s Law
After three years of public consultation The Mitochondrial Donation Law Reform (Maeve’s Law) Bill 2021 was passed in the Australian Senate in 2022, making mitochondrial donation legal in a research and clinical trial setting.
Maeve’s law stipulates strict conditions including that clinics need a special licence to perform mitochondrial donation.
To make sure mitochondrial donation works and is safe before it’s introduced into Australian clinical practice, the law also specifies that initial licences will be issued for pre-clinical and clinical trial research and training.
We’re expecting one such licence to be issued for the mitoHOPE (Healthy Outcomes Pilot and Evaluation) program, which we are part of, to perfect the technique and conduct a clinical trial to make sure mitochondrial donation is safe and effective.
Before starting the trial, a preclinical research and training program will ensure embryologists are trained in “real-life” clinical conditions and existing mitochondrial donation techniques are refined and improved. To do this, many human eggs are needed.
The need for donor eggs
One of the challenges with mitochondrial donation is sourcing eggs. For the preclinical research and training program, frozen eggs can be used, but for the clinical trial “fresh” eggs will be needed.
One possible source of frozen eggs is from people who have stored eggs they don’t intend to use.
A recent study looked at data on the outcomes of eggs stored at a Melbourne clinic from 2012 to 2021. Over the ten-year period, 1,132 eggs from 128 patients were discarded. No eggs were donated to research because the clinics where the eggs were stored did not conduct research requiring donor eggs.
However, research shows that among people with stored eggs, the number one choice for what to do with eggs they don’t need is to donate them to research.
This offers hope that, given the opportunity, those who have eggs stored that they don’t intend to use might be willing to donate them to mitochondrial donation preclinical research.
As for the “fresh” eggs needed in the future clinical trial, this will require individuals to volunteer to have their ovaries stimulated and eggs retrieved to give those people impacted by mito a chance to have a healthy baby. Egg donors may be people who are friends or relatives of those who enter the trial, or it might be people who don’t know someone affected by mito but would like to help them conceive.
At this stage, the aim is to begin enrolling participants in the clinical trial in the next 12 to 18 months. However this may change depending on when the required licences and ethics approvals are granted.
Karin Hammarberg, Senior Research Fellow, Global and Women’s Health, School of Public Health & Preventive Medicine, Monash University; Catherine Mills, Professor of Bioethics, Monash University; Mary Herbert, Professor, Anatomy & Developmental Biology, Monash University, and Molly Johnston, Research fellow, Monash Bioethics Centre, Monash University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
California Is Investing $500M in Therapy Apps for Youth. Advocates Fear It Won’t Pay Off.
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
With little pomp, California launched two apps at the start of the year offering free behavioral health services to youths to help them cope with everything from living with anxiety to body acceptance.
Through their phones, young people and some caregivers can meet BrightLife Kids and Soluna coaches, some who specialize in peer support or substance use disorders, for roughly 30-minute virtual counseling sessions that are best suited to those with more mild needs, typically those without a clinical diagnosis. The apps also feature self-directed activities, such as white noise sessions, guided breathing, and videos of ocean waves to help users relax.
“We believe they’re going to have not just great impact, but wide impact across California, especially in places where maybe it’s not so easy to find an in-person behavioral health visit or the kind of coaching and supports that parents and young people need,” said Gov. Gavin Newsom’s health secretary, Mark Ghaly, during the Jan. 16 announcement.
The apps represent one of the Democratic governor’s major forays into health technology and come with four-year contracts valued at $498 million. California is believed to be the first state to offer a mental health app with free coaching to all young residents, according to the Department of Health Care Services, which operates the program.
However, the rollout has been slow. Only about 15,000 of the state’s 12.6 million children and young adults have signed up for the apps, school counselors say they’ve never heard of them, and one of the companies isn’t making its app available on Android phones until summer.
Advocates for youth question the wisdom of investing taxpayer dollars in two private companies. Social workers are concerned the companies’ coaches won’t properly identify youths who need referrals for clinical care. And the spending is drawing lawmaker scrutiny amid a state deficit pegged at as much as $73 billion.
An App for That
Newsom’s administration says the apps fill a need for young Californians and their families to access professional telehealth for free, in multiple languages, and outside of standard 9-to-5 hours. It’s part of Newsom’s sweeping $4.7 billion master plan for kids’ mental health, which was introduced in 2022 to increase access to mental health and substance use support services. In addition to launching virtual tools such as the teletherapy apps, the initiative is working to expand workforce capacity, especially in underserved areas.
“The reality is that we are rarely 6 feet away from our devices,” said Sohil Sud, director of Newsom’s Children and Youth Behavioral Health Initiative. “The question is how we can leverage technology as a resource for all California youth and families, not in place of, but in addition to, other behavioral health services that are being developed and expanded.”
The virtual platforms come amid rising depression and suicide rates among youth and a shortage of mental health providers. Nearly half of California youths from the ages of 12 to 17 report having recently struggled with mental health issues, with nearly a third experiencing serious psychological distress, according to a 2021 study by the UCLA Center for Health Policy Research. These rates are even higher for multiracial youths and those from low-income families.
But those supporting youth mental health at the local level question whether the apps will move the needle on climbing depression and suicide rates.
“It’s fair to applaud the state of California for aggressively seeking new tools,” said Alex Briscoe of California Children’s Trust, a statewide initiative that, along with more than 100 local partners, works to improve the social and emotional health of children. “We just don’t see it as fundamental. And we don’t believe the youth mental health crisis will be solved by technology projects built by a professional class who don’t share the lived experience of marginalized communities.”
The apps, BrightLife Kids and Soluna, are operated by two companies: Brightline, a 5-year-old venture capital-backed startup; and Kooth, a London-based publicly traded company that has experience in the U.K. and has also signed on some schools in Kentucky and Pennsylvania and a health plan in Illinois. In the first five months of Kooth’s Pennsylvania pilot, 6% of students who had access to the app signed up.
Brightline and Kooth represent a growing number of health tech firms seeking to profit in this space. They beat out dozens of other bidders including international consulting companies and other youth telehealth platforms that had already snapped up contracts in California.
Although the service is intended to be free with no insurance requirement, Brightline’s app, BrightLife Kids, is folded into and only accessible through the company’s main app, which asks for insurance information and directs users to paid licensed counseling options alongside the free coaching. After KFF Health News questioned why the free coaching was advertised below paid options, Brightline reordered the page so that, even if a child has high-acuity needs, free coaching shows up first.
The apps take an expansive view of behavioral health, making the tools available to all California youth under age 26 as well as caregivers of babies, toddlers, and children 12 and under. When KFF Health News asked to speak with an app user, Brightline connected a reporter with a mother whose 3-year-old daughter was learning to sleep on her own.
‘It’s Like Crickets’
Despite being months into the launch and having millions in marketing funds, the companies don’t have a definitive rollout timeline. Brightline said it hopes to have deployed teams across the state to present the tools in person by midyear. Kooth said developing a strategy to hit every school would be “the main focus for this calendar year.”
“It’s a big state — 58 counties,” Bob McCullough of Kooth said. “It’ll take us a while to get to all of them.”
So far BrightLife Kids is available only on Apple phones. Brightline said it’s aiming to launch the Android version over the summer.
“Nobody’s really done anything like this at this magnitude, I think, in the U.S. before,” said Naomi Allen, a co-founder and the CEO of Brightline. “We’re very much in the early innings. We’re already learning a lot.”
The contracts, obtained by KFF Health News through a records request, show the companies operating the two apps could earn as much as $498 million through the contract term, which ends in June 2027, months after Newsom is set to leave office. And the state is spending hundreds of millions more on Newsom’s virtual behavioral health strategy. The state said it aims to make the apps available long-term, depending on usage.
The state said 15,000 people signed up in the first three months. When KFF Health News asked how many of those users actively engaged with the app, it declined to say, noting that data would be released this summer.
KFF Health News reached out to nearly a dozen California mental health professionals and youths. None of them were aware of the apps.
“I’m not hearing anything,” said Loretta Whitson, executive director of the California Association of School Counselors. “It’s like crickets.”
Whitson said she doesn’t think the apps are on “anyone’s” radar in schools, and she doesn’t know of any schools that are actively advertising them. Brightline will be presenting its tool to the counselor association in May, but Whitson said the company didn’t reach out to plan the meeting; she did.
Concern Over Referrals
Whitson isn’t comfortable promoting the apps just yet. Although both companies said they have a clinical team on staff to assist, Whitson said she’s concerned that the coaches, who aren’t all licensed therapists, won’t have the training to detect when users need more help and refer them to clinical care.
This sentiment was echoed by other school-based social workers, who also noted the apps’ duplicative nature — in some counties, like Los Angeles, youths can access free virtual counseling sessions through Hazel Health, a for-profit company. Nonprofits, too, have entered this space. For example, Teen Line, a peer-to-peer hotline operated by Southern California-based Didi Hirsch Mental Health Services, is free nationwide.
While the state is also funneling money to the schools as part of Newsom’s master plan, students and school-based mental health professionals voiced confusion at the large app investment when, in many school districts, few in-person counseling roles exist, and in some cases are dwindling.
Kelly Merchant, a student at College of the Desert in Palm Desert, noted that it can be hard to access in-person therapy at her school. She believes the community college, which has about 15,000 students, has only one full-time counselor and one part-time bilingual counselor. She and several students interviewed by KFF Health News said they appreciated having engaging content on their phone and the ability to speak to a coach, but all said they’d prefer in-person therapy.
“There are a lot of people who are seeking therapy, and people close to me that I know. But their insurances are taking forever, and they’re on the waitlist,” Merchant said. “And, like, you’re seeing all these people struggle.”
Fiscal conservatives question whether the money could be spent more effectively, like to bolster county efforts and existing youth behavioral health programs.
Republican state Sen. Roger Niello, vice chair of the Senate Budget and Fiscal Review Committee, noted that California is forecasted to face deficits for the next three years, and taxpayer watchdogs worry the apps might cost even more in the long run.
“What starts as a small financial commitment can become uncontrollable expenses down the road,” said Susan Shelley of the Howard Jarvis Taxpayers Association.
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: