From eye exams to blood tests and surgery: how doctors use light to diagnose disease
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is the next article in our ‘Light and health’ series, where we look at how light affects our physical and mental health in sometimes surprising ways. Read other articles in the series.
You’re not feeling well. You’ve had a pounding headache all week, dizzy spells and have vomited up your past few meals.
You visit your GP to get some answers and sit while they shine a light in your eyes, order a blood test and request some medical imaging.
Everything your GP just did relies on light. These are just some of the optical technologies that have had an enormous impact in how we diagnose disease.

1. On-the-spot tests
Point-of-care diagnostics allow doctors to test patients on the spot and get answers in minutes, rather than sending samples to a lab for analysis.
The “flashlight” your GP uses to view the inside of your eye (known as an ophthalmoscope) is a great example. This allows doctors to detect abnormal blood flow in the eye, deformations of the cornea (the outermost clear layer of the eye), or swollen optical discs (a round section at the back of the eye where the nerve link to the brain begins). Swollen discs are a sign of elevated pressure inside your head (or in the worst case, a brain tumour) that could be causing your headaches.
The invention of lasers and LEDs has enabled many other miniaturised technologies to be provided at the bedside or clinic rather than in the lab.
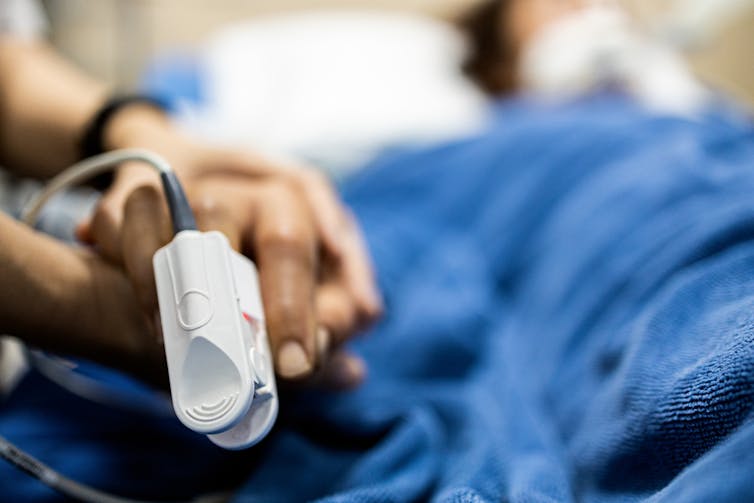
Pulse oximetry is a famous example, where a clip attached to your finger reports how well your blood is oxygenated. It does this by measuring the different responses of oxygenated and de-oxygenated blood to different colours of light.
Pulse oximetry is used at hospitals (and sometimes at home) to monitor your respiratory and heart health. In hospitals, it is also a valuable tool for detecting heart defects in babies.
2. Looking at molecules
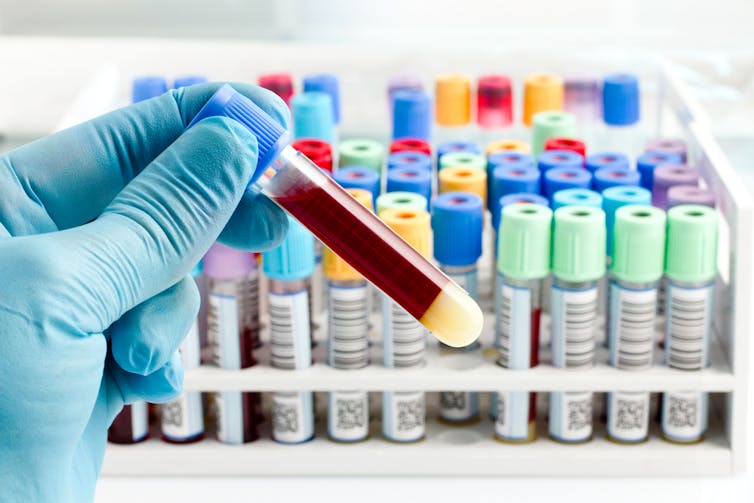
Now, back to that blood test. Analysing a small amount of your blood can diagnose many different diseases.
A machine called an automated “full blood count analyser” tests for general markers of your health. This machine directs focused beams of light through blood samples held in small glass tubes. It counts the number of blood cells, determines their specific type, and reports the level of haemoglobin (the protein in red blood cells that distributes oxygen around your body). In minutes, this machine can provide a snapshot of your overall health.
For more specific disease markers, blood serum is separated from the heavier cells by spinning in a rotating instrument called a centrifuge. The serum is then exposed to special chemical stains and enzyme assays that change colour depending on whether specific molecules, which may be the sign of a disease, are present.
These colour changes can’t be detected with the naked eye. However, a light beam from an instrument called a spectrometer can detect tiny amounts of these substances in the blood and determine if the biomarkers for diseases are present, and at what levels.
3. Medical imaging
Let’s re-visit those medical images your GP ordered. The development of fibre-optic technology, made famous for transforming high-speed digital communications (such as the NBN), allows light to get inside the body. The result? High-resolution optical imaging.
A common example is an endoscope, where fibres with a tiny camera on the end are inserted into the body’s natural openings (such as your mouth or anus) to examine your gut or respiratory tracts.
Surgeons can insert the same technology through tiny cuts to view the inside of the body on a video screen during laparoscopic surgery (also known as keyhole surgery) to diagnose and treat disease.

How about the future?
Progress in nanotechnology and a better understanding of the interactions of light with our tissues are leading to new light-based tools to help diagnose disease. These include:
- nanomaterials (materials on an extremely small scale, many thousands of times smaller than the width of a human hair). These are being used in next-generation sensors and new diagnostic tests
- wearable optical biosensors the size of your fingernail can be included in devices such as watches, contact lenses or finger wraps. These devices allow non-invasive measurements of sweat, tears and saliva, in real time
- AI tools to analyse how blood serum scatters infrared light. This has allowed researchers to build a comprehensive database of scatter patterns to detect any cancer
- a type of non-invasive imaging called optical coherence tomography for more detailed imaging of the eye, heart and skin
- fibre optic technology to deliver a tiny microscope into the body on the tip of a needle.
So the next time you’re at the GP and they perform (or order) some tests, chances are that at least one of those tests depend on light to help diagnose disease.
Matthew Griffith, Associate Professor and ARC Future Fellow and Director, UniSA Microscopy and Microanalysis Facilities, University of South Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Can I Eat That? – by Jenefer Roberts
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The answer to the question in the title is: you can eat pretty much anything, if you’re prepared for the consequences!
This book looks to give you the information to make your own decisions in that regard. There’s a large section on the science of glucose metabolism in the context of food (other aspects of glucose metabolism aren’t covered), so you will not simply be told “raw carrots are good; mashed potatoes are bad”, you’ll understand many factors that affect it, e.g:
- Macronutrient profiles of food and resultant base glycemic indices
- How the glycemic index changes if you cut something, crush it, mash it, juice it, etc
- How the glycemic index changes if you chill something, heat it, fry it, boil it, etc
- The many “this food works differently in the presence of this other food” factors
- How your relative level of insulin resistance affects things itself
…and much more.
The style is simple and explanatory, without deep science, but with good science and comprehensive advice.
There are also the promised recipes; they’re in an appendix at the back and aren’t the main meat of the book, though.
Bottom line: if you’ve ever found it confusing working out what works how in the mysterious world of diabetes nutrition, this book is a top tier demystifier.
Click here to check out Can I Eat That?, and gain confidence in your food choices!
Share This Post
-
Does Ginseng Increase Testosterone Levels?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
❓ Q&A With 10almonds Subscribers!
Q: You talked about spearmint as reducing testosterone levels, what about ginseng for increasing them?
A: Hormones are complicated and often it’s not a simple matter of higher or lower levels! It can also be a matter of…
- how your body converts one thing into another
- how your body responds (or not) to something according to how the relevant hormone’s receptors are doing
- …and whether there’s anything else blocking those receptors.
All this to say: spearmint categorically is an anti-androgen, but the mechanism of action remains uncertain.
Panax ginseng, meanwhile, is one of the most well-established mysteries in herbal medicine.
Paradoxically, it seems to improve both male and female hormonal regulation, despite being more commonly associated with the former.
- It doesn’t necessarily increase or decrease testosterone or estrogen levels (but it can, even if indirectly)
- It does improve sexual function
- …and alleviates symptoms associated with conditions as varied as:
- Late-onset hypogonadism (common for men during the andropause)
- Benign prostate hyperplasia (again common for men during the andropause)
- …and also counteracts unwanted side-effects of finasteride. Finasteride is often taken by men as a hair loss remedy or, less often but critically, in the case of an enlarged prostate.
But it also…
- Alleviates symptoms of PCOS (polycystic ovary syndrome, which effects around 20% of women)
- May even be an effective treatment for PCOS (rat model only so far)
- It also may improve female reproductive fertility more generally (the studies are down to fruit flies now though)
Bottom line: Panax ginseng is popularly taken to improve natural hormone function, a task at which it appears to excel.
Scientists are still working out exactly how it does the many things it appears to do.
Progress has been made, and it clearly is science rather than witchcraft, but there are still far more unanswered questions than resolved ones!
Share This Post
-
Falling vaccination rates put children at risk of preventable diseases. Governments need a new strategy to boost uptake
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Child vaccination is one of the most cost-effective health interventions. It accounts for 40% of the global reduction in infant deaths since 1974 and has led to big health gains in Australia over the past two decades.
Australia has been a vaccination success story. Ten years after we begun mass vaccination against polio in 1956, it was virtually eliminated. Our child vaccination rates have been among the best in the world.
But after peaking in 2020, child vaccination in Australia is falling. Governments need to implement a comprehensive strategy to boost vaccine uptake, or risk exposing more children to potentially preventable infectious diseases.
Yuri A/Shutterstock Child vaccination has been a triumph
Thirty years ago, Australia’s childhood vaccination rates were dismal. Then, in 1997, governments introduced the National Immunisation Program to vaccinate children against diseases such as diphtheria, tetanus, and measles.
Measures to increase coverage included financial incentives for parents and doctors, a public awareness campaign, and collecting and sharing local data to encourage the least-vaccinated regions to catch up with the rest of the country.
What followed was a public health triumph. In 1995, only 52% of one-year-olds were fully immunised. By 2020, Australia had reached 95% coverage for one-year-olds and five-year-olds. At this level, it’s difficult even for highly infectious diseases, such as measles, to spread in the community, protecting both the vaccinated and unvaccinated.
By 2020, 95% of children were vaccinated. Drazen Zigic/Shutterstock Gaps between regions and communities closed too. In 1999, the Northern Territory’s vaccination rate for one-year-olds was the lowest in the country, lagging the national average by six percentage points. By 2020, that gap had virtually disappeared.
The difference between vaccination rates for First Nations children and other children also narrowed considerably.
It made children healthier. The years of healthy life lost due to vaccine-preventable diseases for children aged four and younger fell by nearly 40% in the decade to 2015.
Some diseases have even been eliminated in Australia.
Our success is slipping away
But that success is at risk. Since 2020, the share of children who are fully vaccinated has fallen every year. For every child vaccine on the National Immunisation Schedule, protection was lower in 2024 than in 2020.
Gaps between parts of Australia are opening back up. Vaccination rates in the highest-coverage parts of Australia are largely stable, but they are falling quickly in areas with lower vaccination.
In 2018, there were only ten communities where more than 10% of one-year-old children were not fully vaccinated. Last year, that number ballooned to 50 communities. That leaves more areas vulnerable to disease and outbreaks.
While Noosa, the Gold Coast Hinterland and Richmond Valley (near Byron Bay) have persistently had some of the country’s lowest vaccination rates, areas such as Manjimup in Western Australia and Tasmania’s South East Coast have recorded big declines since 2018.
Missing out on vaccination isn’t just a problem for children.
One preprint study (which is yet to be peer-reviewed) suggests vaccination during pregnancy may also be declining.
Far too many older Australians are missing out on recommended vaccinations for flu, COVID, pneumococcal and shingles. Vaccination rates in aged care homes for flu and COVID are worryingly low.
What’s going wrong?
Australia isn’t alone. Since the pandemic, child vaccination rates have fallen in many high-income countries, including New Zealand, the United Kingdom and the United States.
Globally, in 2023, measles cases rose by 20%, and just this year, a measles outbreak in rural Texas has put at least 13 children in hospital.
Alarmingly, some regions in Australia have lower measles vaccination than that Texas county.
The timing of trends here and overseas suggests things shifted, or at least accelerated, during the pandemic. Vaccine hesitancy, fuelled by misinformation about COVID vaccines, is a growing threat.
This year, vaccine sceptic Robert F. Kennedy Jr was appointed to run the US health system, and Louisiana’s top health official has reportedly cancelled the promotion of mass vaccination.
In Australia, a recent survey found 6% of parents didn’t think vaccines were safe, and 5% believed they don’t work.
Those concerns are far more common among parents with children who are partially vaccinated or unvaccinated. Among the 2% of parents whose children are unvaccinated, almost half believe vaccines are not safe for their child, and four in ten believe vaccines didn’t work.
Other consequences of the pandemic were a spike in the cost of living, and a health system struggling to meet demand. More than one in ten parents said cost and difficulty getting an appointment were barriers to vaccinating their children.
There’s no single cause of sliding vaccination rates, so there’s no one solution. The best way to reverse these worrying trends is to work on all the key barriers at once – from a lack of awareness, to inconvenience, to lack of trust.
What governments should do
Governments should step up public health campaigns that counter misinformation, boost awareness of immunisation and its benefits, and communicate effectively to low-vaccination groups. The new Australian Centre for Disease Control should lead the charge.
Primary health networks, the regional bodies responsible for improving primary care, should share data on vaccination rates with GPs and pharmacies. These networks should also help make services more accessible to communities who are missing out, such as migrant groups and disadvantaged families.
State and local governments should do the same, sharing data and providing support to make maternal child health services and school-based vaccination programs accessible for all families.
Governments can communicate better about the benefits of vaccination. Yuri A/Shutterstock Governments should also be more ambitious about tackling the growing vaccine divides between different parts of the country. The relevant performance measure in the national vaccination agreement is weak. States must only increase five-year-old vaccination rates in four of the ten areas where it is lowest. That only covers a small fraction of low-vaccination areas, and only the final stage of child vaccination.
Australia needs to set tougher goals, and back them with funding.
Governments should fund tailored interventions in areas with the lowest rates of vaccination. Proven initiatives include training trusted community members as “community champions” to promote vaccinations, and pop-up clinics or home visits for free vaccinations.
At this time of year, childcare centres and schools are back in full swing. But every year, each new intake has less protection than the previous cohort. Governments are developing a new national vaccination strategy and must seize the opportunity to turn that trend around. If it commits to a bold national plan, Australia can get back to setting records for child vaccination.
Peter Breadon, Program Director, Health and Aged Care, Grattan Institute and Wendy Hu, Associate, Health Program, Grattan Institute
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Toothpastes & Mouthwashes: Which Help And Which Harm?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Toothpastes and mouthwashes: which kinds help, and which kinds harm?
You almost certainly brush your teeth. You might use mouthwash. A lot of people floss for three weeks at a time, often in January.
There are a lot of options for oral hygiene; variations of the above, and many alternatives too. This is a big topic, so rather than try to squeeze it all in one, this will be a several-part series.
For today, let’s look at toothpastes and mouthwashes, to start!
Toothpaste options
Toothpastes may contain one, some, or all of the following, so here are some notes on those:
Fluoride
Most toothpastes contain fluoride; this is generally recognized as safe though is not without its controversies. The fluoride content is the reason it’s recommended not to swallow toothpaste, though.
The fluoride in toothpaste can cause some small problems if overused; if you see unusually white patches on your teeth (your teeth are supposed to be ivory-colored, not truly white), that is probably a case of localized overcalcification because of the fluoride, and yes, you can have too much of a good thing.
Overall, the benefits are considered to far outweigh the risks, though.
Baking soda
Whether by itself or as part of a toothpaste, baking soda is a safe and effective choice, not just for cosmetic purposes, but for boosting genuine oral hygiene too:
- Enhanced plaque removal to improve gingival health: 3-month randomized clinical study of the effects of baking soda toothpaste on plaque and gingivitis
- The effects of two baking-soda toothpastes in enhancing mechanical plaque removal and improving gingival health: A 6-month randomized clinical study
- The efficacy of baking soda dentifrice in controlling plaque and gingivitis: A systematic review
Activated charcoal
Activated charcoal is great at removing many chemicals from things it touches. That includes the kind you might see on your teeth in the form of stains.
A topical aside on safety: activated charcoal is a common ingredient in a lot of black-colored Halloween-themed foods and drinks around this time of year. Beware, if you ingest these, there’s a good chance of it also cleaning out any meds you are taking. Ask your pharmacist about your own personal meds, but meds that (ingested) activated charcoal will usually remove include:
- Oral HRT / contraceptives
- Antidepressants (many kinds)
- Heart medications (at least several major kinds)
Toothpaste, assuming you are spitting-not-swallowing, won’t remove your medications though. Nor, in case you were worrying, will it strip tooth enamel, even if you have extant tooth enamel erosion:
Source: Activated charcoal toothpastes do not increase erosive tooth wear
However, it’s of no special extra help when it comes to oral hygiene itself, just removing stains.
So, if you’d like to use it for cosmetic reasons, go right ahead. If not, no need.
Hydrogen peroxide
This is generally not a good idea, speaking for the health. For whitening, yes, it works. But for health, not so much:
To be clear, when they say “alter”, they mean “in a bad way”. It increases inflammation and tissue damage.
If buying commercially-available whitening toothpaste made with hydrogen peroxide, the academic answer is that it’s a lottery, because brands’ proprietorial compounding processes vary widely and constantly with little oversight and even less transparency:
Is whitening toothpaste safe for dental health?: RDA-PE method
Mouthwash options
In the case of fluoride and hydrogen peroxide, the same advice (for and against) goes as per toothpaste.
Alcohol
There has been some concern about the potential carcinogenic effect of alcohol-based mouthwashes. According to the best current science, this one’s not an easy yes-or-no, but rather:
- If there are no other cancer risk factors, it does not seem to increase cancer risk
- If there are other cancer risk factors, it does make the risk worse
Read more:
- Does the use of alcohol mouthwash increase the risk of developing oral cancer?
- Alcohol-based mouthwash as a risk factor of oral cancer: A systematic review
Non-Alcohol
Non-alcoholic mouthwashes are not without their concerns either. In this case, the potential problem is changing the oral microbiome (we are supposed to have one!), and specifically, that the spread of what it kills and what it doesn’t may result in an imbalance that causes a lowering of the pH of the mouth.
Put differently: it makes your saliva more acidic.
Needless to say, that can cause its own problems for teeth. The research on this is still emerging, with regard to whether the benefits outweigh the problems, but the fact that it has this effect seems to be a consensus. Here’s an example paper; there are others:
Effects of Chlorhexidine mouthwash on the oral microbiome
Flossing, scraping, and alternatives
These are important (and varied, and interesting) enough to merit their own main feature, rather than squeezing them in at the end.
So, watch this space for a main feature on these soon!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Delicious Daily Daal
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You’re not obliged to eat this every day, but you might want to. The reason we called this one this, is because it’s a super simple recipe (don’t be put off by the long ingredients list; it’s mostly spices making it look long) which, after you’ve done it a couple of times, you could practically do it in your sleep quickly and easily.
The name “lentil daal” is a bit like “naan bread”—a redundant tautology repeated more than once unnecessarily, but it helps for international clarity. The dish is usually served with naan, by the way, and rice. We don’t have room for those today, maybe we’ll do them another day; for now, you can just cook rice how you normally do, and buy naan if necessary.
Writer’s note: I love strong flavors; many people don’t. For this reason I’m going to give a “basic” version. Please feel free to multiply the spices if you feel so inclined. Where I give “one teaspoon” of a spice below, I’d use a tablespoon at home. Chili peppers can vary in heat a lot even within the same type, so what I do for any given batch is taste one (raw), judge the heat, and use an appropriate number of peppers accordingly. If you don’t want to do that, I suggest just guessing low (as per the instructions below) and if you find at the end you want more heat, you can always stir in a little hot sauce. I know that sounds heretical, but at the end of the day, the primary goal of cooking is to have the meal you want at the end of it.
You will need
- 1 1/2 cups red lentils
- 1 large onion, chopped
- 1 large bulb garlic, minced
- 1 oz ginger, grated
- 2 hot peppers (e.g. serrano), chopped
- 1 tsp ground cumin
- 1 tsp ground coriander
- 1 tsp ground turmeric
- 1 tsp garam masala (this is also ground, but it doesn’t come any other way)
- 1 tsp chili flakes (omit if you’re not a fan of heat)
- 2 tsp cracked black pepper
- 1 tsp salt ← I wouldn’t recommend multiplying this one unless later, to taste. In fact, instead of 1 tsp salt I use 2 tsp MSG, which has less sodium than 1 tsp salt. But “1 tsp salt” is the “easy to find in the store” version.
- 2 large or 3 small tomatoes, chopped (or 1 can chopped tomatoes)
- 2 shallots, thinly sliced
- 1 tsp cumin seeds
- 1 tsp mustard seeds
- 1 tsp coriander seeds
- 1 tsp black peppercorns
- 1 lime
- 1/2 cup fresh cilantro, or if you have the “that tastes like soap” gene, parsley, chopped
- Coconut oil for cooking (if you don’t like coconut, consider springing for avocado oil—if you use olive oil, it’ll add an olivey taste which changes the dish a lot; not inherently bad, but it feels a lot less like traditional daal; seed oils are less healthy and we don’t recommend them; ghee is a traditional option and not bad in moderation, but not as healthy as the oils we mentioned first)
- Water for cooking the lentils
Method
(we suggest you read everything at least once before doing anything)
1) In a saucepan, boil water and add the lentils; let them simmer while doing the next things.
2) Sauté the onions until translucent. This should only take a few minutes.
3) Add the garlic, ginger, and hot peppers, and keep stirring for another couple of minutes.
4) Add the ground spices (cumin, coriander, turmeric, garam masala) chili flakes, and cracked black pepper, as well as the salt or MSG if using (not both), and stir them in quickly but thoroughly.
For the next step, you may need to transfer to larger pan if your sauté pan isn’t big enough to take the volume; if so, that’s fine, the sauté has done its job and can have a rest now. If your sauté pan is big enough, just carry on in the same pan; this is perfect.
5) Add the lentils with the water you cooked them in (there might not be much water left now, as the lentils will have absorbed a lot of it; this is fine) as well as the chopped tomatoes.
6) Simmer until it has the consistency of a very thick sauce (you can add a splash more water here and there if it seems to need more). In the West it’s common to serve lentils “al dente”, but in the East it’s usual to (for dishes like this) cook them until they start to
7) Add the juice of at least 1/2 of your lime, or the whole lime if you feel so inclined.
8) In a pre-heated skillet, flash-fry the sliced shallots and the seeds (cumin, coriander, mustard, black peppercorns) at the hottest temperature you can muster. Don’t worry if the oil smokes; we’re only going to be at this tadka-making stage for a moment and nothing will stick provided you keep it moving. When the seeds start popping, it’s ready. Add it all to the big pan and stir in.
9) Add the cilantro-or-parsley garnish once you’re ready to serve.
Enjoy!
Learn more
For those interested in some of the science of what we have going on today:
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
- How Much Spice Is Right?
- Tasty Polyphenols
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What the Health – by Kip Andersen, Keegan Kuhn, & Eunice Wong
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is a book from the makers of the famous documentary of the same name. Which means that yes, they are journalists not scientists, but they got input from very many scientists, doctors, nutritionists, and so forth, for a very reliable result.
It’s worth noting however that while a lot of the book is about the health hazards of a lot of the “Standard American Diet”, or “SAD” as it is appropriately abbreviated, a lot is also about how various industries
bribelobby the government to either push, or give them leeway to push, their products over healthier ones. So, there’s a lot about what would amount to corruption if it weren’t tied up in legalese that makes it just “lobbying” rather than bribery.The style is mostly narrative, albeit with very many citations adding up to 50 pages of references. There’s also a recipe section, which is… fairly basic, and despite getting a shoutout in the subtitle, the recipes are certainly not the real meat of the book.
The recipes themselves are entirely plant-based, and de facto vegan.
Bottom line: this one’s more of a polemic against industry malfeasance than it is a textbook of nutrition science, but there is enough information in here that it could have been the textbook if it wanted to, changing only the style and not the content.
Click here to check out What The Health, and make informed choices about yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: