Black Forest Chia Pudding
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This pudding tastes so decadent, it’s hard to believe it’s so healthy, but it is! Not only is it delicious, it’s also packed with nutrients including protein, carbohydrates, healthy fats (including omega-3s), fiber, vitamins, minerals, and assorted antioxidant polyphenols. Perfect dessert or breakfast!
You will need
- 1½ cups pitted fresh or thawed-from-frozen cherries
- ½ cup mashed banana
- 3 tbsp unsweetened cocoa powder
- 2 tbsp chia seeds, ground
- Optional: 2 pitted dates, soaked in hot water for 10 minutes and then drained (include these if you prefer a sweeter pudding)
- Garnish: a few almonds, and/or berries, and/or cherries and/or cacao nibs
Method
(we suggest you read everything at least once before doing anything)
1) Blend the ingredients except for the chia seeds and the garnish, with ½ cup of water, until completely smooth
2) Divide into two small bowls or glass jars
3) Add 1 tbsp ground chia seeds to each, and stir until evenly distributed
4) Add the garnish and refrigerate overnight or at least for some hours. There’s plenty of wiggle-room here, so make it at your convenience and serve at your leisure.

Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Cherries’ Very Healthy Wealth Of Benefits!
- If You’re Not Taking Chia, You’re Missing Out
- Cacao vs Carob – Which is Healthier?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Codependent No More – by Melody Beattie
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is a book review, not a book summary, but first let’s quickly cover a common misconception, because the word “codependent” gets misused a lot in popular parlance:
- What codependence isn’t: “we depend on each other and must do everything together”
- What codependence is:“person 1 has a dependency on a substance (or perhaps a behavior, such as gambling); person 2 is trying to look after person 1, and so has developed a secondary relationship with the substance/behavior. Person 2 is now said to be codependent, because it becomes all-consuming for them too, even if they’re not using the substance/behavior directly”
Funny how often it happens that the reality is more complex than the perception, isn’t it?
Melody Beattie unravels all this for us. We get a compassionate and insightful look at how we can look after ourselves, while looking after another. Perhaps most importantly: how and where to draw a line of what we can and cannot do/change for them.
Because when we love someone, of course we want to fight their battles with them, if not for them. But if we want to be their rock of strength, we can’t get lost in it too, and of course that hurts.
Beatty takes us through these ideas and more, for example:
- How to examine our own feelings even when it’s scary
- How to practice self-love and regain self-worth, while still caring for them
- How to stop being reactionary, step back, and act with purpose
If the book has any weak point, it’s that it repeatedly recommends 12-step programs, when in reality that’s just one option. But for those who wish to take another approach, this book does not require involvement in a 12-step program, so it’s not a barrier to usefulness.
Click here to check out Codependent No More and take care of yourself, too
Share This Post
-
Pasteurization: What It Does And Doesn’t Do
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Pasteurization’s Effect On Risks & Nutrients
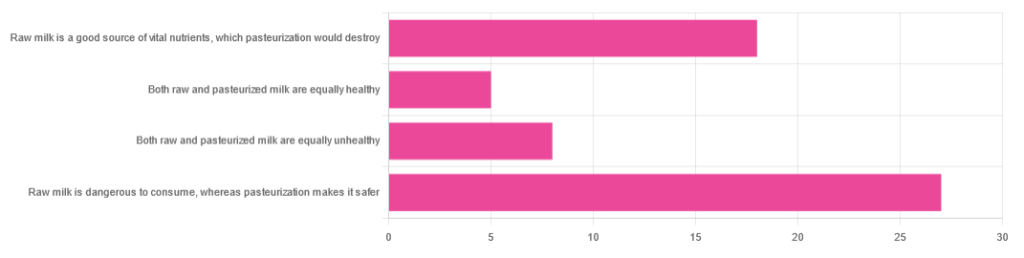
In Wednesday’s newsletter, we asked you for your health-related opinions of raw (cow’s) milk, and got the above-depicted, below-described, set of responses:
- About 47% said “raw milk is dangerous to consume, whereas pasteurization makes it safer”
- About 31% said “raw milk is a good source of vital nutrients which pasteurization would destroy”
- About 14% said “both raw milk and pasteurized milk are equally unhealthy”
- About 9% said “both raw milk and pasteurized milk are equally healthy”
Quite polarizing! So, what does the science say?
“Raw milk is dangerous to consume, whereas pasteurization makes it safer: True or False?”
True! Coincidentally, the 47% who voted for this are mirrored by the 47% of the general US population in a similar poll, deciding between the options of whether raw milk is less safe to drink (47%), just as safe to drink (15%), safer to drink (9%), or not sure (30%):
Public Fails to Appreciate Risk of Consuming Raw Milk, Survey Finds
As for what those risks are, by the way, unpasteurized dairy products are estimated to cause 840x more illness and 45x more hospitalizations than pasteurized products.
This is because unpasteurized milk can (and often does) contain E. coli, Listeria, Salmonella, Cryptosporidium, and other such unpleasantries, which pasteurization kills.
Source for both of the above claims:
(we know the title sounds vague, but all this information is easily visible in the abstract, specifically, the first two paragraphs)
Raw milk is a good source of vital nutrients which pasteurization would destroy: True or False?
False! Whether it’s a “good” source can be debated depending on other factors (e.g., if we considered milk’s inflammatory qualities against its positive nutritional content), but it’s undeniably a rich source. However, pasteurization doesn’t destroy or damage those nutrients.
Incidentally, in the same survey we linked up top, 16% of the general US public believed that pasteurization destroys nutrients, while 41% were not sure (and 43% knew that it doesn’t).
Note: for our confidence here, we are skipping over studies published by, for example, dairy farming lobbies and so forth. Those do agree, by the way, but nevertheless we like sources to be as unbiased as possible. The FDA, which is not completely unbiased, has produced a good list of references for this, about half of which we would consider biased, and half unbiased; the clue is generally in the journal names. For example, Food Chemistry and the Journal of Food Science and Journal of Nutrition are probably less biased than the International Dairy Association and the Journal of Dairy Science:
FDA | Raw Milk Misconceptions and the Danger of Raw Milk Consumption
this page covers a lot of other myths too, more than we have room to “bust” here, but it’s very interesting reading and we recommend to check it out!
Notably, we also weren’t able to find any refutation by counterexample on PubMed, with the very slight exception that some studies sometimes found that in the case of milks that were of low quality, pasteurization can reduce the vitamin E content while increasing the vitamin A content. For most milks however, no significant change was found, and in all cases we looked at, B-vitamins were comparable and vitamin D, popularly touted as a benefit of cow’s milk, is actually added later in any case. And, importantly, because this is a common argument, no change in lipid profiles appears to be findable either.
In science, when something has been well-studied and there aren’t clear refutations by counterexample, and the weight of evidence is clearly very much tipped into one camp, that usually means that camp has it right.
Milk generally is good/bad for the health: True or False?
True or False, depending on what we want to look at. It’s definitely not good for inflammation, but the whole it seems to be cancer-neutral and only increases heart disease risk very slightly:
- Keep Inflammation At Bay ← short version is milk is bad, fermented milk products are fine in moderation
- Is Dairy Scary? ← short version is that milk is neither good nor terrible; fermented dairy products however are health-positive in numerous ways when consumed in moderation
You may be wondering…
…how this goes for the safety of dairy products when it comes to the bird flu currently affecting dairy cows, so:
Take care!
Share This Post
-
Ear Candling: Is It Safe & Does It Work?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Does This Practice Really Hold A Candle To Evidence-Based Medicine?
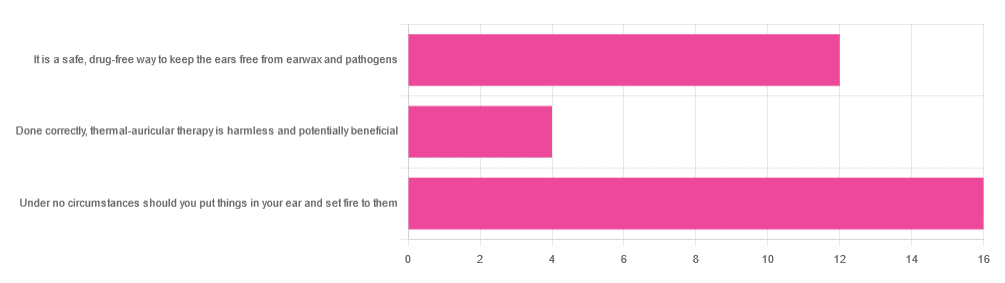
In Tuesday’s newsletter, we asked you your opinion of ear candling, and got the above-depicted, below-described set of responses:
- Exactly 50% said “Under no circumstances should you put things in your ear and set fire to them”
- About 38% said “It is a safe, drug-free way to keep the ears free from earwax and pathogens”
- About 13% said “Done correctly, thermal-auricular therapy is harmless and potentially beneficial”
This means that if we add the two positive-to-candling answers together, it’s a perfect 50:50 split between “do it” and “don’t do it”.
(Yes, 38%+13%=51%, but that’s because we round to the nearest integer in these reports, and more precisely it was 37.5% and 12.5%)
So, with the vote split, what does the science say?
First, a quick bit of background: nobody seems keen to admit to having invented this. One of the major manufacturers of ear candles refers to them as “Hopi” candles, which the actual Hopi tribe has spent a long time asking them not to do, as it is not and never has been used by the Hopi people. Other proposed origins offered by advocates of ear candling include Traditional Chinese Medicine (not used), Ancient Egypt (no evidence of such whatsoever), and Atlantis:
Quackwatch | Why Ear Candling Is Not A Good Idea
It is a safe, drug-free way to keep the ears free from earwax and pathogens: True or False?
False! In a lot of cases of alternative therapy claims, there’s an absence of evidence that doesn’t necessarily disprove the treatment. In this case, however, it’s not even an open matter; its claims have been actively disproven by experimentation:
- It doesn’t remove earwax; on the contrary, experimentation “showed no removal of cerumen from the external auditory canal. Candle wax was actually deposited in some“
- It doesn’t remove pathogens, and the proposed mechanism of action for removing pathogens, that of the “chimney effect”: the idea that the burning candle creates a vacuum that draws wax out of the ear along with debris and bacteria, simply does not work; on the contrary, “Tympanometric measurements in an ear canal model demonstrated that ear candles do not produce negative pressure”.
- It isn’t safe; on the contrary, “Ear candles have no benefit in the management of cerumen and may result in serious injury”
In a medium-sized survey (n=122), the following injuries were reported:
- 13 x burns
- 7 x occlusion of the ear canal
- 6 x temporary hearing loss
- 3 x otitis externa (this also called “swimmer’s ear”, and is an inflammation of the ear, accompanied by pain and swelling)
- 1 x tympanic membrane perforation
Indeed, authors of one paper concluded:
❝Ear candling appears to be popular and is heavily advertised with claims that could seem scientific to lay people. However, its claimed mechanism of action has not been verified, no positive clinical effect has been reliably recorded, and it is associated with considerable risk.
No evidence suggests that ear candling is an effective treatment for any condition. On this basis, we believe it can do more harm than good and we recommend that GPs discourage its use❞
Source: Canadian Family Physician | Ear Candling
Under no circumstances should you put things in your ear and set fire to them: True or False?
True! It’s generally considered good advice to not put objects in general in your ears.
Inserting flaming objects is a definite no-no. Please leave that for the Cirque du Soleil.
You may be thinking, “but I have done this and suffered no ill effects”, which seems reasonable, but is an example of survivorship bias in action—it doesn’t make the thing in question any safer, it just means you were one of the one of the ones who got away unscathed.
If you’re wondering what to do instead… Ear oils can help with the removal of earwax (if you don’t want to go get it sucked out at a clinic—the industry standard is to use a suction device, which actually does what ear candles claim to do). For information on safely getting rid of earwax, see our previous article:
Take care!
Share This Post
Related Posts
-
A Peek Behind The 10almonds Curtain
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
At 10almonds we give a lot of health information, so you may wonder: how much do we (the 10almonds team) put into practice? Is it even possible to do all these things? Do we have an 80:20 rule going on?
So, here’s what someone who thinks, reads, and writes about health all day, does for her health—and how it ties in with what you read here at 10almonds.
Hi, it’s me, a member of the 10almonds team and regular writer here, and I’m going to do the rest of this article in the first-person, since it’s using me as an example!
(PS: yes, the thumbnail is a digital impression of my appearance, though I would correct it that my hair is much longer, and my eyes are more gray; I must admit though it captured my smile, not to mention my collarbones-that-you-could-sit-on)
Dietary habits
Before we get to foods, let’s talk intermittent fasting. I practise 16:8 intermittent fasting… Approximately. That is to say, I’m mostly not religious about it, but I will generally breakfast around 12 noon, and have finished eating dinner before 8pm, with no food outside of those hours.
See also: Intermittent Fasting: What’s the truth?
Importantly, while I feel free to be a little flexible around start and finish times, I do very consciously decide “I am now fasting” and “I will now break the fast”.
Note my imperfection: it would be ideal to have the eating period earlier in the day, and have a bigger breakfast and small dinner. However, that doesn’t really work for me (leisurely evening meal is an important daily event in this household), so this is how I do it instead.
Foods!
It gets an exclamation mark because a thing about me is that I do love foods.
Breakfast: a typical breakfast for me these past months is a couple of ounces of mixed nuts with about 1oz of goji berries.
The mixed nuts are in equal proportions: almonds, walnuts, hazelnuts, cashews. Why those four? Simple, it’s because that’s what Aldi sells as “mixed nuts” and they are the cheapest nuts around, as well as containing absolute nutritional heavyweights almonds and walnuts in generous portions.
Often, but not always, I’ll have some dates with it, or dried apricots, or prunes.
I go through phases; sometimes I’ll enjoy overnight oats as my breakfast for a month or two at a time. I really just follow my gut in this regard.
See for example: Spiced Pear & Pecan Polyphenol Porridge
Lunch: I don’t really lunch per se, but between breakfast and dinner I’ll usually snack on a 3–5 organic carrots (I literally just cut the tops off and otherwise eat them like Bugs Bunny—peeling them would be extra work just to lose fiber). Note my imperfection: I don’t buy all of my vegetables organic, but I do for the ones where it makes the biggest difference.
If I’m feeling like it, I may lunch on a selection of herbs sabzi khordan style (see: Invigorating Sabzi Khordan), though I’m vegan so for simplicity I just skip the cheeses that are also traditional with that dish. On the other hand, for protein and fat I’ll usually add a cup of beans (usually black beans or kidney beans), seasoned with garlic and black pepper in an olive oil and balsamic vinegar dressing (that I make myself, so it’s just those ingredients). See also: Kidney Beans vs Black Beans – Which Is Healthier?
Dinner: this is my main sit-down meal of the day, and it’s enjoyed in a leisurely fashion (say, 40 minutes average with a normal distribution bell curve running between 20 and 60 minutes) with my son who lives with me. I mention all of this, because of the importance of relaxed mindful eating. In the instances of it being nearer the 20 minutes end, it’s not because of rushing, but rather because of a lighter meal some days.
See also: How To Get More Nutrition From The Same Food
Regular recurrences in the menu include:
I’ll often snack on something probiotic (e.g. kimchi) while I’m cooking.
See also: Make Friends With Your Gut! (You Can Thank Us Later)
In terms of what’s not in my diet: as mentioned, I’m vegan, so animal products are out. I don’t drink alcohol or use other recreational drugs, and I mostly drink decaffeinated coffee, but I’ll have a caffeinated one if I’m out somewhere. I’m not a puritan when it comes to sugar, but also, I simply don’t like it and I know well its health effects, so it doesn’t really form part of my diet except insofar as it’s in some ready-made condiments I may sometimes use (e.g. sriracha, teriyaki sauce). I’m also not a puritan when it comes to wheat, but it’s not something I consume daily. Usually on a weekly basis I’ll have a wholegrain pasta dish, and a dish with some kind of wholegrain flatbread.
See also:
Exercise!
First, some things that are lifestyle factors:
- I do not own a car, and I dislike riding in cars, buses, etc. So, I walk everywhere, unless it’s far enough that I must take the train, and even then I usually stand between carriages rather than sitting down.
- I have a standing desk setup, that hasn’t been lowered even once since I got it. I highly recommend it, as someone who spends a lot of time at my desk.
- You may imagine that I spend a lot of time reading; if it’s books (as opposed to scientific papers etc, which I read at my desk), then I’ll most of the time read them while perched like a gargoyle in a sitting squat (Slav squat, Asian squat, resting squat, deep squat, etc) on a balance ball. Yes, it is comfortable once you’re used to it!
About that latter, see also: The Most Anti Aging Exercise
In terms of “actual” exercise, I get 150–300 minutes “moderate exercise” per week, which is mostly composed of:
- Most days I walk into town to get groceries; it’s a 40-minute round trip on foot
- On days I don’t do that, even if I do walk to a more local shop, I spend at least 20 minutes on my treadmill.
See also: The Doctor Who Wants Us To Exercise Less, & Move More
Strength and mobility training, for me, comes mostly in what has been called “exercise snacking”, that is to say, I intersperse my working day with brief breaks to do Pilates exercises. I have theme days (lower body, core, upper body) and on average one rest day (from Pilates exercises) per week, though honestly, that’s usually more likely because of time constraints than anything else, because a deadline is looming.
See also: Four Habits That Drastically Improve Mobility
You may be wondering about HIIT: when I’m feeling extra-serious about it, I use my exercise bike for this, but I’ll be honest, I don’t love the bike, so on a daily basis, I’m much more likely to do HIIT by blasting out a hundred or so Hindu squats, resting, and repeating.
See also: How To Do HIIT (Without Wrecking Your Body)
Supplements
First I’ll mention, I do have HRT, of which the hormones I have are bioidentical estradiol gel in the morning, and a progesterone pessary in the evening. They may not be for everybody, but they’ve made a world of difference to me.
See also: HRT: A Tale Of Two Approaches
In terms of what one usually means when one says supplements, many I use intermittently (which is good in some cases, as otherwise the body may stop using them so well, or other problems can arise), but regular features include:
- Magnesium glycinate, malate, & citrate (See: Which Magnesium? (And: When?))
- Active vitamers of vitamins B9 and B12 (See: Which B Vitamins? It Makes A Difference!)
- Liposomal vitamin C (I actually get enough for general purposes in my diet, but as a vegan I don’t get dietary collagen, so this helps collagen synthesis)
- L-theanine (bedtime only) (See: L-Theanine: What’s The Tea?)
- Lion’s mane mushroom (See: What does lion’s mane mushroom actually do, anyway?)
- Quercetin (See: Fight Inflammation & Protect Your Brain, With Quercetin)
- Fisetin (weekends only) (See: Fisetin: The Anti-Aging Assassin)
Why weekends only for Fisetin? See: The Drug & Supplement Combo That Reverses Aging ← the supplement is fisetin, which outperforms quercetin in this role, and/but it only needs be taken for two days every two weeks, as a sort of “clearing out” of senescent cells. There is no need to take it every day, because if you just cleared out your senescent cells, then guess what, they’re not there now. Also, while sensescent cells are a major cause of aging, on a lower level they do have some anti-tumor effects, so it can be good to let some live a least for a while now and again. In short, cellular sensescence can help prevent tumors on a daily level, but it doesn’t hurt that capacity to have a clearing-out every couple of weeks; so says the science (linked above). Note my imperfection: I take it at weekends instead of for two days every two weeks (as is standard in studies, like those linked above), because it is simpler than remembering to count the weeks.
Cognitive exercise
Lest we forget, exercising our mind is also important! In my case:
- I’m blessed to have work that’s quite cognitively stimulating; our topics here at 10almonds are interesting. If it weren’t for that, I’d still be reading and writing a lot.
- I play chess, though these days I don’t play competitively anymore, and play rather for the social aspect, but this too is important in avoiding cognitive decline.
- I am one of those people who compulsively learns languages, and uses them a lot. This is very beneficial, as language ability is maintained in a few small areas of the brain, and it’s very much “use it or lose it”. Now, while I may not need my French or Russian or Arabic to keep the lights on in this part of the brain or that, the fact that I am pushing my limits every day is the important part. It’s not about how much I know—it’s about how much I engage those parts of my brain on a daily basis. Thus, even if you speak only one language right now, learning even just one more, and learning even only a little bit, you will gain the brain benefits—because you’re engaging it regularly in a new way, and that forces the brain to wire new synapses and also to maintain volume in those parts.
See also: How To Reduce Your Alzheimer’s Risk
And about language-learning specifically: An Underrated Tool Against Alzheimer’s ←this also shows how you don’t have to be extreme about language learning like I admittedly am.
How’s all this working out for me?
I can say: it works! My general health is better now than it was decades ago. I’ve personally focused a lot on reducing inflammation, and that really pays dividends when it comes to the rest of health. I didn’t talk about it above, but focusing on my sleep regularity and quality has helped a lot too.
In terms of measurable results, I recently had a general wellness checkup done by means of a comprehensive panel of 14 blood tests, and various physical metrics (BMI, body fat %, blood pressure, etc), and per those, I could not be in better health; it was as though I had cheated and written in all the best answers. I say this not to brag (you don’t know me, after all), but rather to say: it can be done!
Even without extreme resources, and without an abundance of free time, etc, it can be done!
Caveat: if you have some currently incurable chronic disease, there may be some limits. For example, if you have Type 1 Diabetes, probably your HbA1c* is going to be a little off even if you do everything right.
*HbA1c = glycated hemoglobin, a very accurate measure of what your blood glucose has been on average for the past 2–3 months—why 2–3 months? Because that’s the approximate lifespan of a red blood cell, and we’re measuring how much hemoglobin (in the red blood cells) has been glycated (because of blood glucose).
In summary
The stuff we write about at 10almonds can be implemented, on a modest budget and while juggling responsibilities (work, family, classes, etc).
I’m not saying that my lifestyle should be everyone’s template, but it’s at least an example of one that can work.
- Maybe you hate walking and love swimming.
- Maybe you have no wish to give up fish and eggs, say (both of which are fine/good in moderation healthwise).
- Maybe you have different priorities with supplements.
- Maybe you find language-learning uninteresting but take singing lessons.
- And so on.
In the absolute fewest words, the real template is:
- Decide your health priorities (what matters most for you)
- Look them up on 10almonds
- Put the things into action in a way that works for you!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
10almonds Subcribers Take The Wheel!
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
❓ Q&A With 10almonds Subscribers!
Q: What kind of salt is best for neti pots?
A: Non-iodised salt is usually recommended, but really, any human-safe salt is fine. By this we mean for example:
- Sodium chloride (like most kitchen salts),
- Potassium chloride (as found in “reduced sodium” kitchen salts), or
- Magnesium sulfate (also known as epsom salts).
Q: You talked about spearmint as reducing testosterone levels, what about ginseng for increasing them?
A: Hormones are complicated and often it’s not a simple matter of higher or lower levels! It can also be a matter of…
- how your body converts one thing into another
- how your body responds (or not) to something according to how the relevant hormone’s receptors are doing
- …and whether there’s anything else blocking those receptors.
All this to say: spearmint categorically is an anti-androgen, but the mechanism of action remains uncertain.
Panax ginseng, meanwhile, is one of the most well-established mysteries in herbal medicine.
Paradoxically, it seems to improve both male and female hormonal regulation, despite being more commonly associated with the former.
- It doesn’t necessarily increase or decrease testosterone or estrogen levels (but it can, even if indirectly)
- It does improve sexual function
- …and alleviates symptoms associated with conditions as varied as:
- Late-onset hypogonadism (common for men during the andropause)
- Benign prostate hyperplasia (again common for men during the andropause)
- …and also counteracts unwanted side-effects of finasteride. Finasteride is often taken by men as a hair loss remedy or, less often but critically, in the case of an enlarged prostate.
But it also…
- Alleviates symptoms of PCOS (polycystic ovary syndrome, which effects around 20% of women)
- May even be an effective treatment for PCOS (rat model only so far)
- It also may improve female reproductive fertility more generally (the studies are down to fruit flies now though)
Bottom line: Panax ginseng is popularly taken to improve natural hormone function, a task at which it appears to excel.
Scientists are still working out exactly how it does the many things it appears to do.
Progress has been made, and it clearly is science rather than witchcraft, but there are still far more unanswered questions than resolved ones!
Q: I like that the quizzes (I’ve done two so far) give immediate results , with no “give us your email to get your results”. Thanks!
A: You’re welcome! That’s one of the factors that influences what things we include here! Our mission statement is “to make health and productivity crazy simple”, and the unwritten part of that is making sure to save your time and energy wherever we reasonably can!
Q: Do you know if adrafanil is as good as modafinil? It seems to be a lot cheaper for the same result?
A: Adrafinil is the pro-drug of modafinil. What this means is that if you take it, your own liver will use it to make modafinil inside you. So the end result is chemically the same drug.
As to whether it’s as good, it depends what you need. It’s worth noting that anything that taxes liver function can be harmful if you take too much, and/or your liver is already strained for some reason.
If in doubt, consult a doctor! And if it’s something that’s accessible to you, a recent lipids test (a kind of blood test that checks your liver health) is always a good thing to have.
Q: Would love to see your take on polyphasic sleep!
A: Watch this space
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Parsley vs Spinach – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing parsley to spinach, we picked the parsley.
Why?
First of all, writer’s anecdote: today’s choice brought to you by a real decision here in my household! You see, a certain dish I sometimes prepare (it’s just a wrap-based dish, nothing fancy) requires a greenery component, and historically I’ve used kale or spinach. Of those two, I prefer kale while my son, who lives (and dines) with me, prefers spinach. However, we both like parsley equally, so I’m going to use that today. But I was curious about how it performed nutritionally, hence today’s comparison!
Ok, now for the stats…
In terms of macros, the only difference is that parsley has more fiber and carbs, for an approximately equal glycemic index, so we’ll go with the one with the highest total fiber, which is parsley.
In the category of vitamins, parsley has more of vitamins B3, B5, B7, B9, C, and K, while spinach has more of vitamins A, B2, B6, E, and choline. So, a marginal 6:5 win for parsley (and in the margins of difference are also in parsley’s favor, for example parsley has 13x the vitamin C, and 2x or 3x the other vitamins it won with, while spinach boasts 2x for some vitamins, and only 1.2x or 1.5x the others).
When it comes to minerals, parsley has more iron, phosphorus, potassium, and zinc, while spinach has more copper, magnesium, manganese, and selenium. So, a 4:4 tie on these.
In terms of phytochemicals, parsley has a much higher polyphenol content (that’s good) while spinach has a much higher oxalate content (that’s neutral for most people, but bad if you have certain kidney problems). So, another win for parsley.
Adding up the sections makes a clear overall win for parsley, but by all means enjoy either or both, unless you are avoiding oxalates, in which case, the oxalates in spinach can be reduced by cooking, but honestly, for most dishes you might as well just pick a different greens option (like parsley, or collard greens if you want something closer to the culinary experience of eating spinach).
Want to learn more?
You might like:
Invigorating Sabzi Khordan ← another great way to enjoy parsley as main ingredient rather than just a seasoning
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: