Studies of Parkinson’s disease have long overlooked Pacific populations – our work shows why that must change
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A form of Parkinson’s disease caused by mutations in a gene known as PINK1 has long been labelled rare. But our research shows it’s anything but – at least for some populations.
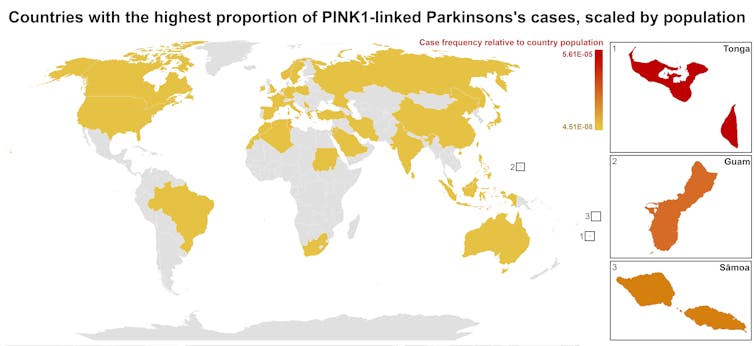
Our meta-analysis revealed that people in specific Polynesian communities have a much higher rate of PINK1-linked Parkinson’s than expected. This finding reshapes not only our understanding of who is most at risk, but also how soon symptoms may appear and what that might mean for treatment and testing.
Parkinson’s disease is often thought of as a single condition. In reality, it is better understood as a group of syndromes caused by different factors – genetic, environmental or a combination of both.
These varying causes lead to differences in disease patterns, progression and subsequent diagnosis. Recognising this distinction is crucial as it paves the way for targeted interventions and may even help prevent the disease altogether.

Why we focus on PINK1-linked Parkinson’s
We became interested in this gene after a 2021 study highlighted five people of Samoan and Tongan descent living in New Zealand who shared the same PINK1 mutation.
Previously, this mutation had been spotted only in a few more distant places –Malaysia, Guam and the Philippines. The fact it appeared in people from Samoan and Tongan backgrounds suggested a historical connection dating back to early Polynesian migrations.
One person in 1,300 West Polynesians carries this mutation. This is a frequency well above what scientists usually classify as rare (below one in 2,200). This discovery means we may be overlooking entire communities in Parkinson’s research if we continue to assume PINK1-linked cases are uncommon.
Traditional understanding says PINK1-linked Parkinson’s is both rare and typically strikes younger people, mostly in their 30s or 40s, if they inherit two faulty copies of the gene. In other words, it’s considered a recessive condition, needing two matching puzzle pieces before the disease can unfold.
Our work challenges this view. We show that even one defective PINK1 gene can cause Parkinson’s at an average age of 43, much earlier than the typical onset after 65. That’s a significant departure from the standard belief that only people with two defective gene copies are at risk.
Why this matters for people with the disease
It’s not just genetics that challenge long-held views. Historically, PINK1-linked Parkinson’s was thought to lack some of the classic features of the disease, such as toxic clumps of alpha-synuclein protein.
In typical Parkinson’s, alpha-synuclein builds up in the brain, forming sticky clumps known as Lewy bodies. Our results, contrary to prior beliefs, show that alpha-synuclein pathology is present in 87.5% of PINK1 cases. This finding opens up a promising new avenue for future treatment development.
The biggest concern is early onset. PINK1-linked Parkinson’s can begin as early as 11 years old, although a more common starting point is around the mid-30s. This early onset means living longer with the disease, which can profoundly affect education, work opportunities and family life.
Current treatments (such as levodopa, a precursor of dopamine) help manage symptoms, but they’re not designed to address the root cause. If we know someone has a PINK1 mutation, scientists and clinicians can explore therapies for specific genetic pathways, potentially delivering relief beyond symptom management.
Sex differences add a layer of complexity
In Parkinson’s, generally, men are at higher risk and tend to develop symptoms earlier. However, our findings suggest the opposite pattern for PINK1-linked cases. Particularly, women with two defective copies of the gene experience onset earlier than men.
This highlights the need to consider sex-related factors in Parkinson’s research. Overlooking them risks missing key elements of the disease.
Genetic testing could be a game-changer for PINK1-linked Parkinson’s. Because it often appears earlier, doctors may not recognise it immediately, especially if they are more familiar with the common, later-onset form of Parkinson’s.
Early genetic testing could lead to a faster, more accurate diagnosis, allowing treatment to begin when interventions are most effective. It would help families understand how the disease is inherited, enabling relatives to get tested.
In some cases, where appropriate and culturally acceptable, embryo screening may be considered to prevent the passing of the faulty gene.
Knowing you have a PINK1 mutation could also make finding the right treatment more efficient. Instead of a lengthy trial-and-error process with different medications, doctors could use emerging therapies designed to target the underlying PINK1 mutation rather than relying on general Parkinson’s treatments meant for the broader population.
Addressing research gaps
These findings underscore how crucial it is to include diverse populations in health research.
Many communities, such as those in Samoa, Tonga and other Pacific nations, have had little to no involvement in global Parkinson’s genetics studies. This has created gaps in knowledge and real-world consequences for people who may not receive timely or accurate diagnoses.
Researchers, funding bodies and policymakers must prioritise projects beyond the usual focus on European or industrialised countries to ensure research findings and treatments are relevant to all affected populations.
To better diagnose and treat Parkinson’s, we need a more inclusive approach. Recognising that PINK1-linked Parkinson’s is not as rare as previously thought – and that genetics, sex differences and cultural factors all play a role – allows us to improve care for everyone.
By expanding genetic testing, refining treatments and ensuring research reflects the full spectrum of Parkinson’s, we can move closer to more precise diagnoses, targeted therapies and better support systems for all.
Victor Dieriks, Research Fellow in Health Sciences, University of Auckland, Waipapa Taumata Rau and Eden Paige Yin, PhD candidate in Health Sciences, University of Auckland, Waipapa Taumata Rau
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Avocado vs Jackfruit – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing avocado to jackfruit, we picked the avocado.
Why?
In terms of macros, avocado is higher in fats (famously healthy ones, including a good dose of omega-3), fiber (nearly 5x more), and protein (despite jackfruit being more often used as a meaty element in recipes, avocado has slightly more). Meanwhile, jackfruit is about 3x higher in carbs. All in all, a clear win for avocado.
Looking at vitamins, avocado has more of vitamins A, B2, B3, B5, B7, B9, E, K, and choline, while jackfruit has more of vitamins B1, B6, and C. Another win for avocado in this category.
In the category of minerals, avocado has more copper, iron, manganese, phosphorus, potassium, selenium, and zinc, while jackfruit has more calcium. One more win for avocado.
Adding up the sections makes for an easy overall win for avocado, but by all means enjoy either or both; diversity is good!
Want to learn more?
You might like:
Jackfruit vs Durian – Which is Healthier? ← including some fun durian facts (such as how to pick a good one, and what happens if you eat durian and drink alcohol)
Enjoy!
Share This Post
-
CBD Against Diabetes!
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝CBD for diabetes! I’ve taken CBD for body pain. Did no good. Didn’t pay attention as to diabetes. I’m type 1 for 62 years. Any ideas?❞
Thanks for asking! First up, for reference, here’s our previous main feature on the topic of CBD:
CBD Oil: What Does The Science Say?
There, we touched on CBD’s effects re diabetes:
in mice / in vitro / in humans
In summary, according to the above studies, it…
- lowered incidence of diabetes in non-obese diabetic mice. By this they mean that pancreatic function improved (reduced insulitis and reduced inflammatory Th1-associated cytokine production). Obviously this has strong implications for Type 1 Diabetes in humans—but so far, just that, implications (because you are not a mouse).
- attenuated high glucose-induced endothelial cell inflammatory response and barrier disruption. Again, this is promising, but it was an in vitro study in very controlled lab conditions, and sometimes “what happens in the Petri dish, stays in the Petri dish”—in order words, these results may or may not translate to actual living humans.
- Improved insulin response ← is the main take-away that we got from reading through their numerical results, since there was no convenient conclusion given. Superficially, this may be of more interest to those with type 2 diabetes, but then again, if you have T1D and then acquire insulin resistance on top of that, you stand a good chance of dying on account of your exogenous insulin no longer working. In the case of T2D, “the pancreas will provide” (more or less), T1D, not so much.
So, what else is there out there?
The American Diabetes Association does not give a glowing review:
❝There’s a lot of hype surrounding CBD oil and diabetes. There is no noticeable effect on blood glucose (blood sugar) or insulin levels in people with type 2 diabetes. Researchers continue to study the effects of CBD on diabetes in animal studies. ❞
~ American Diabetes Association
Source: ADA | CBD & Diabetes
Of course, that’s type 2, but most research out there is for type 2, or else have been in vitro or rodent studies (and not many of those, at that).
Here’s a relatively more recent study that echoes the results of the previous mouse study we mentioned; it found:
❝CBD-treated non-obese diabetic mice developed T1D later and showed significantly reduced leukocyte activation and increased FCD in the pancreatic microcirculation.
Conclusions: Experimental CBD treatment reduced markers of inflammation in the microcirculation of the pancreas studied by intravital microscopy. ❞
~ Dr. Christian Lehmann et al.
Read more: Experimental cannabidiol treatment reduces early pancreatic inflammation in type 1 diabetes
…and here’s a 2020 study (so, more recent again) that was this time rats, and/but still more promising, insofar as it was with rats that had full-blown T1D already:
Read in full: Two-weeks treatment with cannabidiol improves biophysical and behavioral deficits associated with experimental type-1 diabetes
Finally, a paper in July 2023 (so, since our previous article about CBD), looked at the benefits of CBD against diabetes-related complications (so, applicable to most people with any kind of diabetes), and concluded:
❝CBDis of great value in the treatment of diabetes and its complications. CBD can improve pancreatic islet function, reduce pancreatic inflammation and improve insulin resistance. For diabetic complications, CBD not only has a preventive effect but also has a therapeutic value for existing diabetic complications and improves the function of target organs❞
…before continuing:
❝However, the safety and effectiveness of CBD are still needed to prove. It should be acknowledged that the clinical application of CBD in the treatment of diabetes and its complications has a long way to go.
The dissecting of the pharmacology and therapeutic role of CBD in diabetes would guide the future development of CBD-based therapeutics for treating diabetes and diabetic complications❞
~ Ibid.
Now, the first part of that is standard ass-covering, and the second part of that is standard “please fund more studies please”. Nevertheless, we must also not fail to take heed—little is guaranteed, especially when it comes to an area of research where the science is still very young.
In summary…
It seems well worth a try, and with ostensibly nothing to lose except the financial cost of the CBD.
If you do, you might want to keep careful track of a) your usual diabetes metrics (blood sugar levels before and after meals, insulin taken), and b) when you took CBD, what dose, etc, so you can do some citizen science here.
Lastly: please remember our standard disclaimer; we are not doctors, let alone your doctors, so please do check with your endocrinologist before undertaking any such changes!
Want to read more?
You might like our previous main feature:
How To Prevent And Reverse Type 2 Diabetes ← obviously this will not prevent or reverse Type 1 Diabetes, but avoiding insulin resistance is good in any case!
If you’re not diabetic and you’ve perhaps been confused throughout this article, then firstly thank you for your patience, and secondly you might like this quick primer:
The Sweet Truth About Diabetes: Debunking Diabetes Myths! ← this gives a simplified but fair overview of types 1 & 2
(for space, we didn’t cover the much less common types 3 & 4; perhaps another time we will)
Meanwhile, take care!
Share This Post
-
What is AuDHD? 5 important things to know when someone has both autism and ADHD
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You may have seen some new ways to describe when someone is autistic and also has attention-deficit hyperactivity disorder (ADHD). The terms “AuDHD” or sometimes “AutiADHD” are being used on social media, with people describing what they experience or have seen as clinicians.
It might seem surprising these two conditions can co-occur, as some traits appear to be almost opposite. For example, autistic folks usually have fixed routines and prefer things to stay the same, whereas people with ADHD usually get bored with routines and like spontaneity and novelty.
But these two conditions frequently overlap and the combination of diagnoses can result in some unique needs. Here are five important things to know about AuDHD.
Kosro/Shutterstock 1. Having both wasn’t possible a decade ago
Only in the past decade have autism and ADHD been able to be diagnosed together. Until 2013, the Diagnostic and Statistical Manual of Mental Disorders (DSM) – the reference used by health workers around the world for definitions of psychological diagnoses – did not allow for ADHD to be diagnosed in an autistic person.
The manual’s fifth edition was the first to allow for both diagnoses in the same person. So, folks diagnosed and treated prior to 2013, as well as much of the research, usually did not consider AuDHD. Instead, children and adults may have been “assigned” to whichever condition seemed most prominent or to be having the greater impact on everyday life.
2. AuDHD is more common than you might think
Around 1% to 4% of the population are autistic.
They can find it difficult to navigate social situations and relationships, prefer consistent routines, find changes overwhelming and repetition soothing. They may have particular sensory sensitivities.
ADHD occurs in around 5–8% of children and adolescents and 2–6% of adults. Characteristics can include difficulties with focusing attention in a flexible way, resulting in procrastination, distraction and disorganisation. People with ADHD can have high levels of activity and impulsivity.
Studies suggest around 40% of those with ADHD also meet diagnostic criteria for autism and vice versa. The co-occurrence of having features or traits of one condition (but not meeting the full diagnostic criteria) when you have the other, is even more common and may be closer to around 80%. So a substantial proportion of those with autism or ADHD who don’t meet full criteria for the other condition, will likely have some traits.
3. Opposing traits can be distressing
Autistic people generally prefer order, while ADHDers often struggle to keep things organised. Autistic people usually prefer to do one thing at a time; people with ADHD are often multitasking and have many things on the go. When someone has both conditions, the conflicting traits can result in an internal struggle.
For example, it can be upsetting when you need your things organised in a particular way but ADHD traits result in difficulty consistently doing this. There can be periods of being organised (when autistic traits lead) followed by periods of disorganisation (when ADHD traits dominate) and feelings of distress at not being able to maintain organisation.
There can be eventual boredom with the same routines or activities, but upset and anxiety when attempting to transition to something new.
Autistic special interests (which are often all-consuming, longstanding and prioritised over social contact), may not last as long in AuDHD, or be more like those seen in ADHD (an intense deep dive into a new interest that can quickly burn out).
Autism can result in quickly being overstimulated by sensory input from the environment such as noises, lighting and smells. ADHD is linked with an understimulated brain, where intense pressure, novelty and excitement can be needed to function optimally.
For some people the conflicting traits may result in a balance where people can find a middle ground (for example, their house appears tidy but the cupboards are a little bit messy).
There isn’t much research yet into the lived experience of this “trait conflict” in AuDHD, but there are clinical observations.
4. Mental health and other difficulties are more frequent
Our research on mental health in children with autism, ADHD or AuDHD shows children with AuDHD have higher levels of mental health difficulites than autism or ADHD alone.
This is a consistent finding with studies showing higher mental health difficulties such as depression and anxiety in AuDHD. There are also more difficulties with day-to-day functioning in AuDHD than either condition alone.
So there is an additive effect in AuDHD of having the executive foundation difficulties found in both autism and ADHD. These difficulties relate to how we plan and organise, pay attention and control impulses. When we struggle with these it can greatly impact daily life.
5. Getting the right treatment is important
ADHD medication treatments are evidence-based and effective. Studies suggest medication treatment for ADHD in autistic people similarly helps improve ADHD symptoms. But ADHD medications won’t reduce autistic traits and other support may be needed.
Non-pharmacological treatments such as psychological or occupational therapy are less researched in AuDHD but likely to be helpful. Evidence-based treatments include psychoeducation and psychological therapy. This might include understanding one’s strengths, how traits can impact the person, and learning what support and adjustments are needed to help them function at their best. Parents and carers also need support.
The combination and order of support will likely depend on the person’s current functioning and particular needs. https://www.youtube.com/embed/pMx1DnSn-eg?wmode=transparent&start=0 ‘Up until recently … if you had one, you couldn’t have the other.’
Do you relate?
Studies suggest people may still not be identified with both conditions when they co-occur. A person in that situation might feel misunderstood or that they can’t fully relate to others with a singular autism and ADHD diagnosis and something else is going on for them.
It is important if you have autism or ADHD that the other is considered, so the right support can be provided.
If only one piece of the puzzle is known, the person will likely have unexplained difficulties despite treatment. If you have autism or ADHD and are unsure if you might have AuDHD consider discussing this with your health professional.
Tamara May, Psychologist and Research Associate in the Department of Paediatrics, Monash University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
What Grief Does To Your Body (And How To Manage It)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What Grief Does To The Body (And How To Manage It)
In life, we will almost all lose loved ones and suffer bereavement. For most people, this starts with grandparents, eventually moves to parents, and then people our own generation; partners, siblings, close friends. And of course, sometimes and perhaps most devastatingly, we can lose people younger than ourselves.
For something that almost everyone suffers, there is often very little in the way of preparation given beforehand, and afterwards, a condolences card is nice but can’t do a lot for our mental health.
And with mental health, our physical health can go too, if we very understandably neglect it at such a time.
So, how to survive devastating loss, and come out the other side, hopefully thriving? It seems like a tall order indeed.
First, the foundations:
You’re probably familiar with the stages of grief. In their most commonly-presented form, they are:
- Denial
- Anger
- Bargaining
- Depression
- Acceptance
You’ve probably also heard/read that we won’t always go through them in order, and also that grief is deeply personal and proceeds on its own timescale.
It is generally considered healthy to go through them.
What do they look like?
Naturally this can vary a lot from person to person, but examples in the case of bereavement could be:
- Denial: “This surely has not really happened; I’ll carry on as though it hasn’t”
- Anger: “Why didn’t I do xyz differently while I had the chance?!”
- Bargaining: “I will do such-and-such in their honor, and this will be a way of expressing the love I wish I could give them in a way they could receive”
- Depression: “What is the point of me without them? The sooner I join them, the better.”
- Acceptance: “I was so lucky that we had the time together that we did, and enriched each other’s lives while we could”
We can speedrun these or we can get stuck on one for years. We can bounce back and forth. We can think we’re at acceptance, and then a previous stage will hit us like a tonne of bricks.
What if we don’t?
Assuming that our lost loved one was indeed a loved one (as opposed to someone we are merely societally expected to mourn), then failing to process that grief will tend to have a big impact on our life—and health. These health problems can include:
As you can see, three out of five of those can result in death. The other two aren’t great either. So why isn’t this taken more seriously as a matter of health?
Death is, ironically, considered something we “just have to live with”.
But how?
Coping strategies
You’ll note that most of the stages of grief are not enjoyable per se. For this reason, it’s common to try to avoid them—hence denial usually being first.
But, that is like not getting a lump checked out because you don’t want a cancer diagnosis. The emotional reasoning is understandable, but it’s ultimately self-destructive.
First, have a plan. If a death is foreseen, you can even work out this plan together.
But even if that time has now passed, it’s “better late than never” to make a plan for looking after yourself, e.g:
- How you will try to get enough sleep (tricky, but sincerely try)
- How you will remember to eat (and ideally, healthily)
- How you will still get exercise (a walk in the park is fine; see some greenery and get some sunlight)
- How you will avoid self-destructive urges (from indirect, e.g. drinking, to direct, e.g. suicidality)
- How you will keep up with the other things important in your life (work, friends, family)
- How you will actively work to process your grief (e.g. journaling, or perhaps grief counselling)
Some previous articles of ours that may help:
- How To Keep On Keeping On ← this is about looking after general health when motivation is low
- The Mental Health First-Aid You’ll Hopefully Never Need ← this is about managing depression
- How To Stay Alive (When You Really Don’t Want To) ← this is about managing suicidality
- Life After Death? (Your Life; A Loved One’s Death) ← this is about bereavement and romance
If it works, it works
If we are all unique, then any relationship between any two people is uniqueness squared. Little wonder, then, that our grief may be unique too. And it can be complicated further:
- Sometimes we had a complicated relationship with someone
- Sometimes the circumstances of their death were complicated
There is, for that matter, such a thing as “complicated grief”:
Read more: Complicated grief and prolonged grief disorder (Medical News Today)
We also previously reviewed a book on “ambiguous loss”, exploring grieving when we cannot grieve in the normal way because someone is gone and/but/maybe not gone.
For example, if someone is in a long-term coma from which they may never recover, or if they are missing-presumed-dead. Those kinds of situations are complicated too.
Unusual circumstances may call for unusual coping strategies, so how can we discern what is healthy and what isn’t?
The litmus test is: is it enabling you to continue going about your life in a way that allows you to fulfil your internal personal aspirations and external social responsibilities? If so, it’s probably healthy.
Look after yourself. And if you can, tell your loved ones you love them today.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Strength training has a range of benefits for women. Here are 4 ways to get into weights
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Picture a gym ten years ago: the weights room was largely a male-dominated space, with women mostly doing cardio exercise. Fast-forward to today and you’re likely to see women of all ages and backgrounds confidently navigating weights equipment.
This is more than just anecdotal. According to data from the Australian Sports Commission, the number of women participating in weightlifting (either competitively or not) grew nearly five-fold between 2016 and 2022.
Women are discovering what research has long shown: strength training offers benefits beyond sculpted muscles.
John Arano/Unsplash Health benefits
Osteoporosis, a disease in which the bones become weak and brittle, affects more women than men. Strength training increases bone density, a crucial factor for preventing osteoporosis, especially for women negotiating menopause.
Strength training also improves insulin sensitivity, which means your body gets better at using insulin to manage blood sugar levels, reducing the risk of type 2 diabetes. Regular strength training contributes to better heart health too.
There’s a mental health boost as well. Strength training has been linked to reduced symptoms of depression and anxiety.
Strength training can have a variety of health benefits. Ground Picture/Shutterstock Improved confidence and body image
Unlike some forms of exercise where progress can feel elusive, strength training offers clear and tangible measures of success. Each time you add more weight to a bar, you are reminded of your ability to meet your goals and conquer challenges.
This sense of achievement doesn’t just stay in the gym – it can change how women see themselves. A recent study found women who regularly lift weights often feel more empowered to make positive changes in their lives and feel ready to face life’s challenges outside the gym.
Strength training also has the potential to positively impact body image. In a world where women are often judged on appearance, lifting weights can shift the focus to function.
Instead of worrying about the number on the scale or fitting into a certain dress size, women often come to appreciate their bodies for what they can do. “Am I lifting more than I could last month?” and “can I carry all my groceries in a single trip?” may become new measures of physical success.
Strength training can have positive effects on women’s body image. Drazen Zigic/Shutterstock Lifting weights can also be about challenging outdated ideas of how women “should” be. Qualitative research I conducted with colleagues found that, for many women, strength training becomes a powerful form of rebellion against unrealistic beauty standards. As one participant told us:
I wanted something that would allow me to train that just didn’t have anything to do with how I looked.
Society has long told women to be small, quiet and not take up space. But when a woman steps up to a barbell, she’s pushing back against these outdated rules. One woman in our study said:
We don’t have to […] look a certain way, or […] be scared that we can lift heavier weights than some men. Why should we?
This shift in mindset helps women see themselves differently. Instead of worrying about being objects for others to look at, they begin to see their bodies as capable and strong. Another participant explained:
Powerlifting changed my life. It made me see myself, or my body. My body wasn’t my value, it was the vehicle that I was in to execute whatever it was that I was executing in life.
This newfound confidence often spills over into other areas of life. As one woman said:
I love being a strong woman. It’s like going against the grain, and it empowers me. When I’m physically strong, everything in the world seems lighter.
Feeling inspired? Here’s how to get started
1. Take things slow
Begin with bodyweight exercises like squats, lunges and push-ups to build a foundation of strength. Once you’re comfortable, add external weights, but keep them light at first. Focus on mastering compound movements, such as deadlifts, squats and overhead presses. These exercises engage multiple joints and muscle groups simultaneously, making your workouts more efficient.
2. Prioritise proper form
Always prioritise proper form over lifting heavier weights. Poor technique can lead to injuries, so learning the correct way to perform each exercise is crucial. To help with this, consider working with an exercise professional who can provide personalised guidance and ensure you’re performing exercises correctly, at least initially.
Bodyweight exercises, such as lunges, are a good way to get started before lifting weights. antoniodiaz/Shutterstock 3. Consistency is key
Like any fitness regimen, consistency is key. Two to three sessions a week are plenty for most women to see benefits. And don’t be afraid to occupy space in the weights room – remember you belong there just as much as anyone else.
4. Find a community
Finally, join a community. There’s nothing like being surrounded by a group of strong women to inspire and motivate you. Engaging with a supportive community can make your strength-training journey more enjoyable and rewarding, whether it’s an in-person class or an online forum.
Are there any downsides?
Gym memberships can be expensive, especially for specialist weightlifting gyms. Home equipment is an option, but quality barbells and weightlifting equipment can come with a hefty price tag.
Also, for women juggling work and family responsibilities, finding time to get to the gym two to three times per week can be challenging.
If you’re concerned about getting too “bulky”, it’s very difficult for women to bulk up like male bodybuilders without pharmaceutical assistance.
The main risks come from poor technique or trying to lift too much too soon – issues that can be easily avoided with some guidance.
Erin Kelly, Lecturer and PhD Candidate, Discipline of Sport and Exercise Science, University of Canberra
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Why We Get Fat: And What to Do About It – by Gary Taubes
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve previously reviewed Taubes’ “The Case Against Sugar“. What does this one bring differently?
Mostly, it’s a different focus. Unsurprisingly, Taubes’ underlying argument is the same: sugar is the biggest dietary health hazard we face. However, this book looks at it specifically through the lens of weight loss, or avoiding weight gain.
Taubes argues for low-carb in general; he doesn’t frame it specifically as the ketogenic diet here, but that is what he is advocating. However, he also acknowledges that not all carbs are created equal, and looks at several categories that are relatively better or worse for our insulin response, and thus, fat management.
If the book has a fault it’s that it does argue a bit too much for eating large quantities of meat, based on Weston Price’s outdated and poorly-conducted research. However, if one chooses to disregard that, the arguments for a low-carb diet for weight management remain strong.
Bottom line: if you’d like to cut some fat without eating less (or exercising more), this book offers a good, well-explained guide for doing so.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: