Death by Food Pyramid – by Denise Minger
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This one is less about “here’s the perfect way of eating” or even “these specific foods are ontologically evil”, but more about teaching science literacy.
The author explores various health trends from the 70s until time of writing (the book was published in 2014), what rationales originally prompted them, and what social phenomena either helped them to persist, or caused them to get dropped quite quickly.
Of course, even in the case of fads that are societally dropped quite quickly, on an individual level there will always be someone just learning about it for the first time, reading some older material, and thinking “that sounds like just the miracle life-changer I need!”
What she teaches the reader to do is largely what we do a lot of here at 10almonds—examine the claims, go to the actual source material (studies! Not just books about studies!), and see whether the study conclusions actually support the claim, to start with, and then further examine to see if there’s some way (or sometimes, a plurality of ways) in which the study itself is methodologically flawed.
Which does happen sometimes, do actually watch out for that!
The style is quite personal and entertaining for the most part, and yet even moving sometimes (the title is not hyperbole; deaths will be discussed). As one might expect of a book teaching science literacy, it’s very easy to read, with copious footnotes (well, actually they are at the back of the book doubling up as a bibliography, but they are linked-to throughout) for those who wish to delve deeper—something the author, of course, encourages.
Bottom line: if you’d like to be able to sort the real science from the hype yourself, then this book can set you on the right track!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Best morning routine?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You’ve Got Questions? We’ve Got Answers!
Q: Best morning routine?
A: The best morning routine is whatever makes you feel most ready to take on your day!
This one’s going to vary a lot—one person’s morning run could be another person’s morning coffee and newspaper, for example.
In a nutshell, though, ask yourself these questions:
- How long does it take me to fully wake up in the morning, and what helps or hinders that?
- When I get out of bed, what do I really need before I can take on my day?
- If I could have the perfect morning, what would it look like?
- What can evening me do, to look after morning me’s best interests? (Semi-prepare breakfast ready? Lay out clothes ready? Running shoes? To-Do list?)
Share This Post
-
Eat Dirt – by Dr. Josh Axe
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Axe describes leaky gut as “a serious disease with a silly name”, and hopes for people to take increased intestinal permeability (as it is otherwise known) seriously, because it can be found at the root of very many diseases, especially inflammatory / autoimmune diseases, which obviously also has significant implications for dementia (of which neuroinflammation is a fair part of the pathogenesis) and cancer (which has been described as largely a matter of immune dysfunction).
He starts strong, albeit anecdotally, with the story of his own mother’s battle with cancer and other diseases, and how her health did a U-turn (for the better) upon taking care of her gut as per the methods described in this book. Dr. Axe doesn’t go so far as to claim the gut-healthy protocol cured her cancer, but makes the (very reasonable) argument that it was a major contributory factor, especially as it was the main input variable that changed.
The book describes the various things that can go wrong with our gut and why, and for each of them presents a solution.
Some of it is as you might guess from the title—live a little dirtier, because the ubiquity of antimicrobials is leaving our immune system slack and maladjusted, causing it to varyingly a) turn on us b) not rise to the occasion when an actual pathogen arrives c) often both. Other matters of consideration include normal gut health nutrition (prebiotics and probiotics, skipping inflammatory foods), matters of medication (especially those that harm the gut), nutraceuticals such as Boswellia serrata, and even stress management.
He provides a program so that the reader can follow along step-by-step, and even a chapter of recipes, but the greatest value in the book is the explanation of gut pathology—because understanding that is foundational to recognizing a lot of things (and he does provide diagnostic questionnaires also, which are helpful).
Bottom line: if you’d like to improve almost any aspect of your health, then your gut is almost always an excellent place to start, and this book will set you on the right path.
Share This Post
-
10 Lessons For A Healthy Mind & Body
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sadia Badiei, food scientist of “Pick Up Limes” culinary fame, has advice in and out of the kitchen:
Pick up a zest for life
Here’s what she picked up, and we all can too:
- “I can’t do it… yet”: it’s never too late to adopt a growth mindset by adding “yet” to your self-doubt, focusing on progress and the possibility of improvement.
- The spotlight effect: people are generally too absorbed in their own lives to focus on you, so don’t worry too much about others’ perceptions.
- Nutrition by addition: focus on adding healthier foods to your diet rather than eliminating the less healthy ones to avoid restrictive mindsets. You can still eliminate the less healthy ones if you want to! It just shouldn’t be the primary focus. Focusing on a conceptually negative thing is rarely helpful.
- It’s ok to change: embrace change as a sign of growth and evolution, rather than seeing it as a failure or waste of time.
- The way you do one thing is the way you do everything: be mindful of how you approach small tasks, regular tasks, boring tasks, unwanted tasks—you can either create a habit of enthusiasm or a habit of suffering (it’s entirely your choice which)
- Setting goals for success: set goals based on actions you can control (inputs) rather than outcomes that are uncertain. Less “lose 10 lbs”, and more “eat fiber before starch”, for example.
- You probably can’t have it all at once: you can achieve all your dreams, but often not simultaneously; goals and desires unfold in stages over time.
- The five-year rule: before adopting a new lifestyle or habit, ask yourself if you can realistically sustain it for five years to ensure it’s not just a short-term fix. If you struggle with this prognostic, look backwards first instead. Which healthy habits have you maintained for decades, and which were you never able to make stick?
- Are you afraid or excited?: reframe fear as excitement, as both emotions share similar physical sensations and signify that you care about the outcome.
- The voice you hear most: speak kindly to yourself in self-talk to create a softer, more compassionate tone. Your subconscious is always listening, so reinforce healthy rather than unhealthy thought patterns.
For more on each of these, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
80-Year-Olds Share Their Biggest Regrets
Take care!
Share This Post
Related Posts
-
Is thirst a good predictor of dehydration?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Water is essential for daily functioning and health, and we can only survive a few days without it. Yet we constantly lose water through sweat, urination and even evaporation when we breathe.
This is why we have evolved a way to regulate and maintain water in our bodies. Like other animals, our survival relies on a strong biological drive that tells us to find and drink water to balance fluid loss.
This is thirst – a sensation of dryness in the mouth signalling we need to have a drink. This basic physiological mechanism is controlled mainly by part of the brain’s “control centre”, called the hypothalamus. The hypothalamus receives signals from various regions of the body and in return, releases hormones that act as a messenger to signal the thirst sensation.
KieferPix/Shutterstock What is dehydration?
Staying hydrated (having enough water in our bodies) is important for several reasons, including:
- regulating body temperature through sweat and respiration
- lubricating joints and eyes
- preventing infections
- digesting and absorbing nutrients
- flushing out waste (via the kidneys)
- preventing constipation
- brain function (including memory and concentration)
- mood and energy levels
- physical performance and recovery from exercise
- skin health.
Dehydration occurs when our body doesn’t have enough water. Even slight drops in fluid levels have noticeable consequences, such as headaches, feeling dizzy, lethargy and struggling to concentrate.
Chronic dehydration can pose more serious health risks, including urinary tract infections, constipation and kidney stones.
What does the evidence say?
Despite thirst being one of the most basic biological drivers for good hydration, science suggests our feelings of thirst and subsequent fluid intake don’t always correlate with hydration levels.
For example, a recent study explored the impact of thirst on fluid intake and hydration status. Participants attended a lab in the morning and then later in the afternoon to provide markers of hydration status (such as urine, blood samples and body weight). The relationship between levels of thirst in the morning and afternoon hydration status was negligible.
Further, thirst may be driven by environmental factors, such as access to water. For example, one study looked at whether ample access to water in a lab influenced how much people drank and how hydrated they were. The link between how thirsty they felt and how hydrated they were was weak, suggesting the availability of water influenced their fluid intake more than thirst.
Exercise can also change our thirst mechanism, though studies are limited at this stage.
Being thirsty doesn’t necessarily mean we’re dehydrated. puhhha/Shutterstock Interestingly, research shows women experience thirst more strongly than men, regardless of hydration status. To understand gender differences in thirst, researchers infused men and women with fluids and then measured their thirst and how hydrated they were. They found women generally reported thirst at a lower level of fluid loss. Women have also been found to respond more to feeling thirsty by drinking more water.
Other ways to tell if you need to drink some water
While acknowledging some people will need to drink more or less, for many people, eight cups (or two litres) a day is a good amount of water to aim for.
But beyond thirst, there are many other ways to tell whether you might need to drink more water.
1. urine colour: pale yellow urine typically indicates good hydration, while darker, concentrated urine suggests dehydration
2. frequency of going to the toilet: urinating regularly (around four to six times a day) indicates good hydration. Infrequent urination can signal dehydration
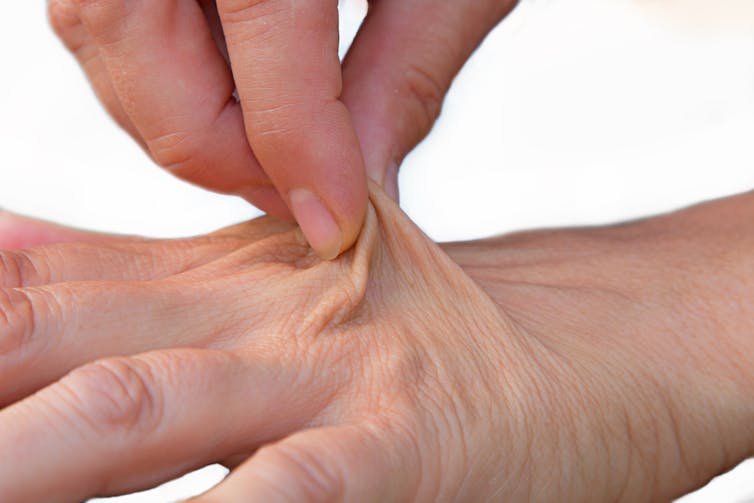
3. skin turgor test: gently pinching the skin (for example, on the back of the hand) and observing how quickly the skin returns to its normal position can help assess hydration. Slow return may indicate dehydration
If skin stays elevated after pinching it may be a sign of dehydration. SusaZoom/Shutterstock 4. mouth and lips: a dry mouth or cracked lips can be early signs of dehydration
5. headaches and fatigue: frequent headaches, dizziness, or unexplained fatigue can be signs of inadequate hydration
6. sweating: in physically active people, monitoring how much they sweat during activity can help estimate fluid loss and hydration needs. Higher levels of sweat may predispose a person to dehydration if they are unable to replace the fluid lost through water intake
These indicators, used together, provide a more comprehensive picture of hydration without solely depending on the sensation of thirst.
Of course, if you do feel thirsty, it’s still a good idea to drink some water.
Lauren Ball, Professor of Community Health and Wellbeing, The University of Queensland and Kiara Too, PhD candidate, School of Human Movement and Nutrition Sciences, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Pinch Of Nom, Everyday Light – by Kay Featherstone and Kate Allinson
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
One of the biggest problems with “light”, “lean” or “under this many calories” cookbooks tends to be the portion sizes perhaps had sparrows in mind. Not so, here!
Nor do they go for the other usual trick, which is giving us something that’s clearly not a complete meal. All of these recipes are for complete meals, or else come with a suggestion of a simple accompaniment that will still keep the dish under 400kcal.
The recipes are packed with vegetables and protein, perfect for keeping lean while also making sure you’re full until the next meal.
Best of all, they are indeed rich and tasty meals—there’s only so many times one wants salmon with salad, after all. There are healthy-edition junk food options, too! Sausage and egg muffins, fish and chips, pizza-loaded fries, sloppy dogs, firecracker prawns, and more!
Most of the meals are quite quick and easy to make, and use common ingredients.
Nearly half are vegetarian, and gluten-free options involve only direct simple GF substitutions. Similarly, turning a vegetarian meal into a vegan meal is usually not rocket science! Again, quick and easy substitutions, à la “or the plant-based milk of your choice”.
Recipes are presented in the format: ingredients, method, photo. Super simple (and no “chef’s nostalgic anecdote storytime” introductions that take more than, say, a sentence to tell).
All in all, a fabulous addition to anyone’s home kitchen!
Get your copy of “Pinch of Nom—Everyday Light” from Amazon today!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Jamaican Coconut Rice
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is a great dish that can be enjoyed hot or cold, as a main or as a side. It has carbs, proteins, healthy fats, fiber, as well as an array of healthy phytochemicals. Not to mention, a great taste!
You will need
- 1 cup wholegrain basmati rice (it may also be called “brown basmati rice“; this is the same) (traditional recipe calls for pudding rice, but we’re going with the healthier option here)
- 2 cans (each 12 z / 400g) coconut milk
- 2 cups (or 2 cans, of which the drained weight is comparable to a cup each) cooked black beans. If you cook them yourself, this is better, as you will be able to cook them more al dente than you can get from a can, and this firmness is desirable. But canned is fine if that’s what’s available.
- 1 large red onion, finely chopped
- ½ cup low-sodium vegetable stock (ideally you made this yourself from vegetable offcuts you saved in the freezer for this purpose, but failing that, low-sodium stock cubes can be bought at any large supermarket)
- 2 serrano chilis, finely chopped
- 1 Scotch bonnet chili, without doing anything to it
- 1 tbsp black pepper, coarse ground
- 1 tbsp chia seeds
- 1 tbsp coconut oil
- Garnish: parsley, chopped
Note: we have erred on the side of low-heat when it comes to the chilis. If you know that you and (if applicable) everyone else eating would enjoy more heat, add more heat. If not, let extra heat be added at the table via your hot sauce of choice. Sounds heretical, but it ensures everyone gets the right amount! It’s easy to add heat than to take it out, after all.
However: if you do end up with too much heat in this or any other dish, adding acid will usually help to neutralize that. In the case of this dish, we’d recommend lime juice as a complementary flavor.
Method
(we suggest you read everything at least once before doing anything)
1) In a big sauté pan, add the coconut oil, melt it if not already melted, and add the chopped onion and the chopped chilis, at a temperature sufficient to sizzle. Keep them all moving. Once the coconut oil is absorbed into the onion (this will happen before the onion is fully cooked), add the vegetable stock, followed by the coconut milk; mix it all gently to create a smooth consistency.
2) Add the rice, chia seeds, and black pepper; mix it all gently but thoroughly; turn the temperature to a simmer, and add the Scotch bonnet chili, without cutting it at all.
3) Cover and keep on low for about 20–30 minutes until the rice is looking done. Check on it periodically to make sure it’s not running out of liquid, but resist the urge to stir it; it shouldn’t be burning but paradoxically, once you start stirring you can’t stop or it will definitely burn.
4) Take out the Scotch bonnet chili, and discard*. Add the black beans.
*its job was to add flavor without adding the high-level heat of that particular chili. If you’re a regular heat-fiend, feel free to experiment with using sliced Scotch bonnet chilis instead of serrano chilis; just be aware that there’s a big difference in heat. Only do this if you really like heat. Using it the way we described in the main recipe is what’s traditional in the Caribbean, by the way.
5) Now you can (and in fact must) stir, to mix in the black beans and bring them back to temperature within the dish. Be aware that once you start stirring, you need to keep stirring until you’re ready to take it off the heat.
6) Serve, adding the parsley garnish.
(this example went light on the beans; our recipe includes more for a heartier dish)
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Should You Go Light Or Heavy On Carbs?
- Our Top 5 Spices: How Much Is Enough For Benefits?
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
- Burn! How To Boost Your Metabolism
- Capsaicin For Weight Loss And Against Inflammation
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: