Peas vs Broad Beans – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing peas to broad beans, we picked the peas.
Why?
Both are great of course, but…
Looking at the macros to start with, peas have more protein and more fiber. The differences aren’t huge, but they are clear.
In terms of vitamins, peas have more of vitamins A, B1, B2, B3, B5, B6, B9, E, K, and choline (some with very large margins, some with small), while broad beans contain a little more vitamin C (the margin is quite narrow though).
When it comes to minerals, peas have more calcium, copper, iron, magnesium, manganese, phosphorus, potassium, selenium, and zinc, while broad beans have more sodium. So this category wasn’t close.
Adding up the win from each of the categories makes for a clear triple-win for peas.
Easy-peasy!
Want to learn more?
You might like to read:
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Beetroot vs Tomato – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing beetroot to tomato, we picked the beetroot.
Why?
Both are great! But we say beetroot comes out on top:
In terms of macros, beetroot has more protein, carbs, and fiber, making it the more nutritionally dense option. It has a slightly higher glycemic index, but also has specific phytochemicals that lower blood sugars and increase insulin sensitivity, more than cancelling that out. So, a clear win for beetroot in this regard.
In the category of vitamins, beetroot has more of vitamins B2, B5, B7, and B9, while tomato has more of vitamins A, C, E, and K. We’d call that a 4:4 tie, but tomato’s margins of difference are greater, so we say tomato wins this round.
When it comes to minerals, beetroot has more calcium, copper, iron, magnesium, manganese, phosphorus, potassium, selenium, and zinc, while tomatoes are not higher in any mineral. An easy win for beetroot here.
Looking at polyphenols and other remaining phytochemicals, beetroot has most, and especially its betalain content goes a long way. Tomatoes, meanwhile, have a famously high lycopene content (a highly beneficial carotenoid). All in all, it could swing either way based on subjective factors, so we’re saying it’s a tie this time.
Adding up the sections makes for an overall win for beetroot, but by all means enjoy either or both; diversity is good!
Want to learn more?
You might like:
- Beetroot For More Than Just Your Blood Pressure
- Lycopene’s Benefits For The Gut, Heart, Brain, & More
Enjoy!
Share This Post
-
How To Prevent And Reverse Type 2 Diabetes
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Turn back the clock on insulin resistance
This is Dr. Jason Fung. He’s a world-leading expert on intermittent fasting and low carbohydrate approaches to diet. He also co-founded the Intensive Dietary Management Program, later rebranded to the snappier title: The Fasting Method, a program to help people lose weight and reverse type 2 diabetes. Dr. Fung is certified with the Institute for Functional Medicine, for providing functional medicine certification along with educational programs directly accredited by the Accreditation Council for Continuing Medical Education (ACCME).
Why Intermittent Fasting?
Intermittent fasting is a well-established, well-evidenced, healthful practice for most people. In the case of diabetes, it becomes complicated, because if one’s blood sugars are too low during a fasting period, it will need correcting, thus breaking the fast.
Note: this is about preventing and reversing type 2 diabetes. Type 1 is very different, and sadly cannot be prevented or reversed in this fashion.
However, these ideas may still be useful if you have T1D, as you have an even greater need to avoid developing insulin resistance; you obviously don’t want your exogenous insulin to stop working.
Nevertheless, please do confer with your endocrinologist before changing your dietary habits, as they will know your personal physiology and circumstances in ways that we (and Dr. Fung) don’t.
In the case of having type 2 diabetes, again, please still check with your doctor, but the stakes are a lot lower for you, and you will probably be able to fast without incident, depending on your diet itself (more on this later).
Intermittent Fasting can be extra helpful for the body in the case of type 2 diabetes, as it helps give the body a rest from high insulin levels, thus allowing the body to become gradually re-sensitised to insulin.
Why low carbohydrate?
Carbohydrates, especially sugars, especially fructose*, cause excess sugar to be quickly processed by the liver and stored there. When the body’s ability to store glycogen is exceeded, the liver stores energy as fat instead. The resultant fatty liver is a major contributor to insulin resistance, when the liver can’t keep up with the demand; the blood becomes spiked full of unprocessed sugars, and the pancreas must work overtime to produce more and more insulin to deal with that—until the body starts becoming desensitized to insulin. In other words, type 2 diabetes.
There are other factors that affect whether we get type 2 diabetes, for example a genetic predisposition. But, our carb intake is something we can control, so it’s something that Dr. Fung focuses on.
*A word on fructose: actual fruits are usually diabetes-neutral or a net positive due to their fiber and polyphenols.
Fructose as an added ingredient, however, not so much. That stuff zips straight into your veins with nothing to slow it down and nothing to mitigate it.
The advice from Dr. Fung is simple here: cut the carbs. If you are already diabetic and do this with no preparation, you will probably simply suffer hypoglycemia, so instead:
- Enjoy a fibrous starter (a salad, some fruit, or perhaps some nuts)
- Load up with protein first, during your main meal—this will start to trigger your feelings of satedness
- Eat carbs last (preferably whole, unprocessed carbohydrates), and stop eating when 80% full.
Adapting Intermittent Fasting to diabetes
Dr. Fung advocates for starting small, and gradually increasing your fasting period, until, ideally, fasting 16 hours per day. You probably won’t be able to do this immediately, and that’s fine.
You also probably won’t be able to do this, if you don’t also make the dietary adjustments that help to give your liver a break, and thus by knock-on-effect, give your pancreas a break too.
With the dietary adjustments too, however, your insulin production-and-response will start to return to its pre-diabetic state, and finally its healthy state, after which, it’s just a matter of maintenance.
Want to hear more from Dr. Fung?
You may enjoy his blog, and for those who like videos, here is his YouTube channel:
Share This Post
-
What’s the difference between a psychopath and a sociopath? Less than you might think
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Articles about badly behaved people and how to spot them are common. You don’t have to Google or scroll too much to find headlines such as 7 signs your boss is a psychopath or How to avoid the sociopath next door.
You’ll often see the terms psychopath and sociopath used somewhat interchangeably. That applies to perhaps the most famous badly behaved fictional character of all – Hannibal Lecter, the cannibal serial killer from The Silence of the Lambs.
In the book on which the movie is based, Lecter is described as a “pure sociopath”. But in the movie, he’s described as a “pure psychopath”. Psychiatrists have diagnosed him with something else entirely.
So what’s the difference between a psychopath and a sociopath? As we’ll see, these terms have been used at different times in history, and relate to some overlapping concepts.
Benoit Daoust/Shutterstock What’s a psychopath?
Psychopathy has been mentioned in the psychiatric literature since the 1800s. But the latest edition of the Diagnostic Statistical Manual of Mental Disorders (known colloquially as the DSM) doesn’t list it as a recognised clinical disorder.
Since the 1950s, labels have changed and terms such as “sociopathic personality disturbance” have been replaced with antisocial personality disorder, which is what we have today.
Was Hannibal Lecter from The Silence of the Lambs a psychopath, a sociopath or something else entirely? Ralf Liebhold/Shutterstock Someone with antisocial personality disorder has a persistent disregard for the rights of others. This includes breaking the law, repeated lying, impulsive behaviour, getting into fights, disregarding safety, irresponsible behaviours, and indifference to the consequences of their actions.
To add to the confusion, the section in the DSM on antisocial personality disorder mentions psychopathy (and sociopathy) traits. In other words, according to the DSM the traits are part of antisocial personality disorder but are not mental disorders themselves.
US psychiatrist Hervey Cleckley provided the first formal description of psychopathy traits in his 1941 book The Mask of Sanity. He based his description on his clinical observations of nine male patients in a psychiatric hospital. He identified several key characteristics, including superficial charm, unreliability and a lack of remorse or shame.
Canadian psychologist Professor Robert Hare refined these characteristics by emphasising interpersonal, emotional and lifestyle characteristics, in addition to the antisocial behaviours listed in the DSM.
When we draw together all these strands of evidence, we can say a psychopath manipulates others, shows superficial charm, is grandiose and is persistently deceptive. Emotional traits include a lack of emotion and empathy, indifference to the suffering of others, and not accepting responsibility for how their behaviour impacts others.
Finally, a psychopath is easily bored, sponges off others, lacks goals, and is persistently irresponsible in their actions.
So how about a sociopath?
The term sociopath first appeared in the 1930s, and was attributed to US psychologist George Partridge. He emphasised the societal consequences of behaviour that habitually violates the rights of others.
Academics and clinicians often used the terms sociopath and psychopath interchangeably. But some preferred the term sociopath because they said the public sometimes confused the word psychopath with psychosis.
“Sociopathic personality disturbance” was the term used in the first edition of the DSM in 1952. This aligned with the prevailing views at the time that antisocial behaviours were largely the product of the social environment, and that behaviours were only judged as deviant if they broke social, legal, and/or cultural rules.
Some of these early descriptions of sociopathy are more aligned with what we now call antisocial personality disorder. Others relate to emotional characteristics similar to Cleckley’s 1941 definition of a psychopath.
In short, different people had different ideas about sociopathy and, even today, sociopathy is less-well defined than psychopathy. So there is no single definition of sociopathy we can give you, even today. But in general, its antisocial behaviours can be similar to ones we see with psychopathy.
Over the decades, the term sociopathy fell out of favour. From the late 60s, psychiatrists used the term antisocial personality disorder instead.
Born or made?
Both “sociopathy” (what we now call antisocial personality disorder) and psychopathy have been associated with a wide range of developmental, biological and psychological causes.
For example, people with psychopathic traits have certain brain differences especially in regions associated with emotions, inhibition of behaviour and problem solving. They also appear to have differences associated with their nervous system, including a reduced heart rate.
However, sociopathy and its antisocial behaviours are a product of someone’s social environment, and tends to run in families. These behaviours has been associated with physical abuse and parental conflict.
What are the consequences?
Despite their fictional portrayals – such as Hannibal Lecter in Silence of the Lambs or Villanelle in the TV series Killing Eve – not all people with psychopathy or sociopathy traits are serial killers or are physically violent.
But psychopathy predicts a wide range of harmful behaviours. In the criminal justice system, psychopathy is strongly linked with re-offending, particularly of a violent nature.
In the general population, psychopathy is associated with drug dependence, homelessness, and other personality disorders. Some research even showed psychopathy predicted failure to follow COVID restrictions.
But sociopathy is less established as a key risk factor in identifying people at heightened risk of harm to others. And sociopathy is not a reliable indicator of future antisocial behaviour.
In a nutshell
Neither psychopathy nor sociopathy are classed as mental disorders in formal psychiatric diagnostic manuals. They are both personality traits that relate to antisocial behaviours and are associated with certain interpersonal, emotional and lifestyle characteristics.
Psychopathy is thought to have genetic, biological and psychological bases that places someone at greater risk of violating other people’s rights. But sociopathy is less clearly defined and its antisocial behaviours are the product of someone’s social environment.
Of the two, psychopathy has the greatest use in identifying someone who is most likely to cause damage to others.
Bruce Watt, Associate Professor in Psychology, Bond University and Katarina Fritzon, Associate Professor of Psychology, Bond University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Mental illness, psychiatric disorder or psychological problem. What should we call mental distress?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We talk about mental health more than ever, but the language we should use remains a vexed issue.
Should we call people who seek help patients, clients or consumers? Should we use “person-first” expressions such as person with autism or “identity-first” expressions like autistic person? Should we apply or avoid diagnostic labels?
These questions often stir up strong feelings. Some people feel that patient implies being passive and subordinate. Others think consumer is too transactional, as if seeking help is like buying a new refrigerator.
Advocates of person-first language argue people shouldn’t be defined by their conditions. Proponents of identity-first language counter that these conditions can be sources of meaning and belonging.
Avid users of diagnostic terms see them as useful descriptors. Critics worry that diagnostic labels can box people in and misrepresent their problems as pathologies.
Underlying many of these disagreements are concerns about stigma and the medicalisation of suffering. Ideally the language we use should not cast people who experience distress as defective or shameful, or frame everyday problems of living in psychiatric terms.
Our new research, published in the journal PLOS Mental Health, examines how the language of distress has evolved over nearly 80 years. Here’s what we found.
Engin Akyurt/Pexels Generic terms for the class of conditions
Generic terms – such as mental illness, psychiatric disorder or psychological problem – have largely escaped attention in debates about the language of mental ill health. These terms refer to mental health conditions as a class.
Many terms are currently in circulation, each an adjective followed by a noun. Popular adjectives include mental, mental health, psychiatric and psychological, and common nouns include condition, disease, disorder, disturbance, illness, and problem. Readers can encounter every combination.
These terms and their components differ in their connotations. Disease and illness sound the most medical, whereas condition, disturbance and problem need not relate to health. Mental implies a direct contrast with physical, whereas psychiatric implicates a medical specialty.
Mental health problem, a recently emerging term, is arguably the least pathologising. It implies that something is to be solved rather than treated, makes no direct reference to medicine, and carries the positive connotations of health rather than the negative connotation of illness or disease.
Is ‘mental health problem’ actually less pathologising? Monkey Business Images/Shutterstock Arguably, this development points to what cognitive scientist Steven Pinker calls the “euphemism treadmill”, the tendency for language to evolve new terms to escape (at least temporarily) the offensive connotations of those they replace.
English linguist Hazel Price argues that mental health has increasingly come to replace mental illness to avoid the stigma associated with that term.
How has usage changed over time?
In the PLOS Mental Health paper, we examine historical changes in the popularity of 24 generic terms: every combination of the nouns and adjectives listed above.
We explore the frequency with which each term appears from 1940 to 2019 in two massive text data sets representing books in English and diverse American English sources, respectively. The findings are very similar in both data sets.
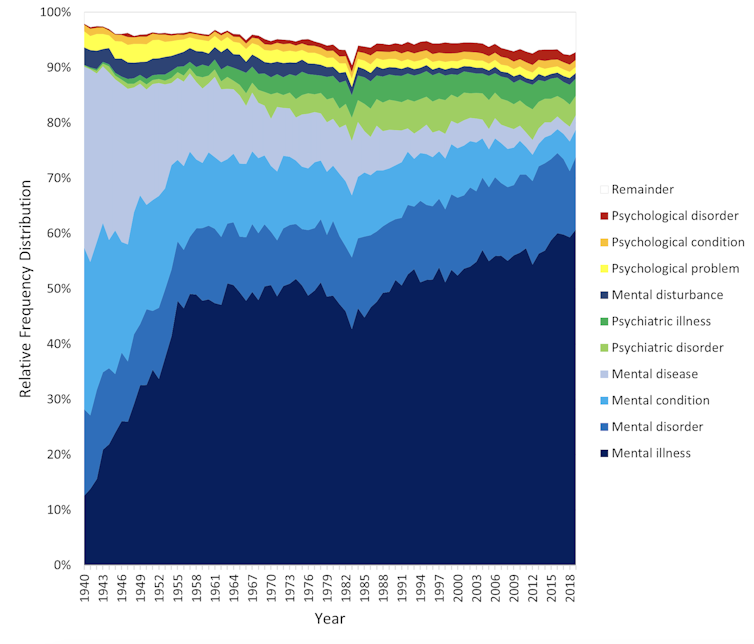
The figure presents the relative popularity of the top ten terms in the larger data set (Google Books). The 14 least popular terms are combined into the remainder.
Relative popularity of alternative generic terms in the Google Books corpus. Haslam et al., 2024, PLOS Mental Health. Several trends appear. Mental has consistently been the most popular adjective component of the generic terms. Mental health has become more popular in recent years but is still rarely used.
Among nouns, disease has become less widely used while illness has become dominant. Although disorder is the official term in psychiatric classifications, it has not been broadly adopted in public discourse.
Since 1940, mental illness has clearly become the preferred generic term. Although an assortment of alternatives have emerged, it has steadily risen in popularity.
Does it matter?
Our study documents striking shifts in the popularity of generic terms, but do these changes matter? The answer may be: not much.
One study found people think mental disorder, mental illness and mental health problem refer to essentially identical phenomena.
Other studies indicate that labelling a person as having a mental disease, mental disorder, mental health problem, mental illness or psychological disorder makes no difference to people’s attitudes toward them.
We don’t yet know if there are other implications of using different generic terms, but the evidence to date suggests they are minimal.
The labels we use may not have a big impact on levels of stigma. Pixabay/Pexels Is ‘distress’ any better?
Recently, some writers have promoted distress as an alternative to traditional generic terms. It lacks medical connotations and emphasises the person’s subjective experience rather than whether they fit an official diagnosis.
Distress appears 65 times in the 2022 Victorian Mental Health and Wellbeing Act, usually in the expression “mental illness or psychological distress”. By implication, distress is a broad concept akin to but not synonymous with mental ill health.
But is distress destigmatising, as it was intended to be? Apparently not. According to one study, it was more stigmatising than its alternatives. The term may turn us away from other people’s suffering by amplifying it.
So what should we call it?
Mental illness is easily the most popular generic term and its popularity has been rising. Research indicates different terms have little or no effect on stigma and some terms intended to destigmatise may backfire.
We suggest that mental illness should be embraced and the proliferation of alternative terms such as mental health problem, which breed confusion, should end.
Critics might argue mental illness imposes a medical frame. Philosopher Zsuzsanna Chappell disagrees. Illness, she argues, refers to subjective first-person experience, not to an objective, third-person pathology, like disease.
Properly understood, the concept of illness centres the individual and their connections. “When I identify my suffering as illness-like,” Chappell writes, “I wish to lay claim to a caring interpersonal relationship.”
As generic terms go, mental illness is a healthy option.
Nick Haslam, Professor of Psychology, The University of Melbourne and Naomi Baes, Researcher – Social Psychology/ Natural Language Processing, The University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
It’s Not You, It’s Your Hormones – by Nicki Williams, DipION, mBANT, CNHC
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
So, first a quick note: this book is very similar to the popular bestseller “The Galveston Diet”, not just in content, but all the way down to its formatting. Some Amazon reviewers have even gone so far as to suggest that “It’s Not You, It’s Your Hormones” (2017) brazenly plagiarized “The Galveston Diet” (2023). However, after carefully examining the publication dates, we feel quite confident that this book is not a copy of the one that came out six years after it. As such, we’ve opted for reviewing the original book.
Nicki Williams’ basic principle is that we can manage our hormonal fluctuations, by managing our diet. Specifically, in three main ways:
- Intermittent fasting
- Anti-inflammatory diet
- Eating more protein and healthy fats
Why should these things matter to our hormones? The answer is to remember that our hormones aren’t just the sex hormones. We have hormones for hunger and satedness, hormones for stress and relaxation, hormones for blood sugar regulation, hormones for sleep and wakefulness, and more. These many hormones make up our endocrine system, and affecting one part of it will affect the others.
Will these things magically undo the effects of the menopause? Well, some things yes, other things no. No diet can do the job of HRT. But by tweaking endocrine system inputs, we can tweak endocrine system outputs, and that’s what this book is for.
The style is very accessible and clear, and Williams walks us through the changes we may want to make, to avoid the changes we don’t want.
In the category of criticism, there is some extra support that’s paywalled, in the sense that she wants the reader to buy her personally-branded online plan, and it can feel a bit like she’s holding back in order to upsell to that.
Bottom line: this book is aimed at peri-menopausal and post-menopausal women. It could also definitely help a lot of people with PCOS too, and, when it comes down to it, pretty much anyone with an endocrine system. It’s a well-evidenced, well-established, healthy way of eating regardless of age, sex, or (most) physical conditions.
Click here to check out It’s Not You, It’s Your Hormones, and take control of yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How To Make Your Doctor’s Appointment Do More For You
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Doctor: “So, how are you today?”
Patient: “Can’t complain; how about you?”Hopefully your medical appointments don’t start quite like that, but there can be an element of being “along for the ride” when it comes to consultations. They ask questions, we answer, they prescribe something, we thank them.
In principle, the doctor should be able to handle that; ask the right questions, determine the problem, and not need too much from you. After all, they have been trained to deal with an unconscious patient, so the fact you can communicate at all is a bonus.
However, leaving it all to them isn’t really playing the field.
Before the appointment
Research your issue, as best you understand it. Some doctors will be very averse to you telling them about having done this (taking it as an affront to their expertise), but here’s the thing:
You don’t have to tell them.
You just have to understand as much as possible, so that you will be as “up to speed” as possible in the conversation, and not be quickly out of your depth.
Have an agenda, based on the above. Literally, have a little set of bullet-points to remind you what you came in to discuss, so that nothing escapes you in the moment. This should also include:
- If you have additional reasons for a particular concern (e.g. family history of a certain problem), make them known
- If you plan to request any specific tests or treatments, be able to clearly state your reasons for the specific tests or treatments
- If you plan to write off any specific tests or treatments as something to which you will not consent, have your reasons ready—in a way that makes it clear it’s something more than “don’t want it”, for example, “I’ve already decided that this treatment would make a sufficient hit to my quality of life, as to make it not worthwhile for me personally” (or whatever the reason may be for you). It needs to be something they can write on their notes instead of simply “patient refused treatment”.
Compile a record of your symptoms (as appropriate), and any previous tests/treatments (as appropriate), in chronological order. If you take all this with you, perhaps in a nice folder, you will enjoy the following advantages:
- not forgetting anything
- ability to answer questions accurately
- give the (correct) impression you take your health seriously, which means they are more likely to do so also—especially because they will now know that if they fob you off and/or mess something up, you’ll be taking a record of that to your next appointment.
Plan your outfit. No, you don’t have to dress for the red carpet, but you want to satisfy two main conditions:
- Accessibility for examination (for example, if you are going in with a knee pain, maybe don’t wear the tight jeans today; if they’re going to take blood, be either sleeveless or have sleeves that are easily moved out of the way, etc)
- General presentability (it’s a sad fact that doctors are not immune to biases, and will treat people better if they respect them more)
During the appointment
Be friendly; doctors (like most people) will respond much better to that than to grumpiness—even if you have good reason for grumpiness and even if the doctor has been trained to help grumpy patients.
Be confident: when we say “be friendly”, that doesn’t mean to necessarily be so agreeable as to not advocate for yourself. In particular:
- If they explain something and it isn’t clear to you, ask them to clarify
- If you disagree with them about a value judgement, say so. By “a value judgement” here we mean things in the realm of subjectivity. If the doctor says you are prediabetic, then you won’t get much mileage out of arguing otherwise; the numbers have the final say on that one. But if the doctor says “the side effects of the treatment you’re requesting will make it not worthwhile for you” and you have understood the side effects and you still disagree, then your opinion counts for more than theirs—it is your decision to make.
- If they dismiss a concern, ask them to put in writing that they dismissed your concern of X, despite you providing evidence that Y, and it being well-known that Z. Often, rather than doing that, they’ll just fold and actually address your concern instead.
Writer’s example in that last category: I recently made a request for a bone density scan. I expect my bone density is great, because I do all the right things, however, as both of my parents suffered from osteoporosis and assorted resultant crushed bones and the terrible consequences thereof, I a) have reasonable grounds for extra concern, and b) I believe that even if my bone density is fine now, it’s good to establish a baseline so I can know, in 5, 10, 20 years etc, whether there has been any deterioration. Now, happily the doctor I saw agreed with my assessment at first presentation and so I got the referral, but had she not been, I would have said “Could you please put in writing that I asked for a bone density scan, and you refused, on the grounds that [details about what happened with my parents], and that osteoporosis is known to have a strong genetic component is not, in your opinion, any reason to worry?”
Be honest, and/but err on the side of overstating your symptoms rather than understating. For example, if it is about a chronic condition and the doctor asks “are you able to do xyz”, take the question as meaning “are you able to do xyz on your worst days?”. You can clarify that if you like in your answer, but you need to include the information that xyz is something that your condition can and sometimes does impede you from doing.
Leave your embarrassment at the door. To the doctor (unless they are a very unprofessional one), you really are just one more patient with symptoms they have (unless your condition is very rare) seen a thousand times before. If your symptom is embarrassing, it will not faze them and you definitely should not hold back from mentioning it, for example. This goes extra in the case of discussions around sexual health, by the way, in which field the details you’d perhaps rather not share with anybody, are the details they need to adequately treat you.
After the appointment
Follow up on anything that doesn’t happen as promised (e.g. referrals, things ordered, etc), to make sure nothing got lost in a bureacratic error.
Get a second opinion if you’re not satisfied with the first one. Doctors are fallible, and as a matter of professional pride, it’s likely the second doctor will be glad to find something the first doctor missed.
See also: Make Your Negativity Work For You
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: