Chaat Masala Spiced Potato Salad With Beans
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is an especially gut-healthy dish; the cooked-and-cooled potatoes are not rich with resistant starches (that’s good), the beans bring protein (as well as more fiber and micronutrients), and many of the spices bring their own benefits. A flavorful addition to your table!
You will need
- 1 lb new potatoes, boiled or steamed, with skin on, quartered, cooled ← this is a bit of a “mini recipe”, but we expect you can handle it
- 5 oz blanched broad beans
- 2 oz sun-dried tomatoes, chopped
- ¼ bulb garlic, crushed
- 1 tbsp extra virgin olive oil
- 2 tsp amchoor
- 2 tsp ground cumin
- 2 tsp ground coriander
- 1 tsp ground ginger
- 1 tsp ground asafoetida
- 1 tsp black pepper, coarse ground
- 1 tsp red chili powder
- 1 tsp ground turmeric
- ½ tsp MSG or 1 tsp low-sodium salt
- Juice of ½ lemon
And then…
- To garnish: finely chopped cilantro, or if you have the “cilantro tastes like soap” gene, then substitute with parsley
- To serve: a nice chutney; you can use our Spiced Fruit & Nut Chutney recipe
Method
(we suggest you read everything at least once before doing anything)
1) Mix all the ingredients from the main section, ensuring an even distribution on the spices.
2) Add the garnish, and serve with the chutney. That’s it. There was more work in the prep (and potentially, finding all the ingredients) today.

Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Our Top 5 Spices: How Much Is Enough For Benefits? ← we scored all five today!
- Lycopene’s Benefits For The Gut, Heart, Brain, & More ← don’t underestimate those sun-dried tomatoes, either!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Taking A Trip Through The Evidence On Psychedelics
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
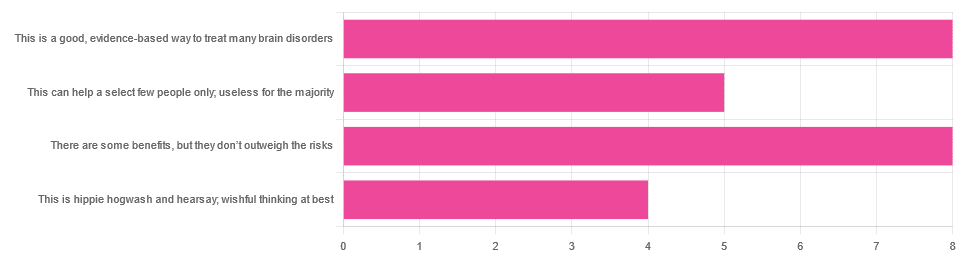
In Tuesday’s newsletter, we asked you for your opinions on the medicinal use of psychedelics, and got the above-depicted, below-described, set of responses:
- 32% said “This is a good, evidence-based way to treat many brain disorders”
- 32% said “There are some benefits, but they don’t outweigh the risks”
- 20% said “This can help a select few people only; useless for the majority”
- 16% said “This is hippie hogwash and hearsay; wishful thinking at best”
Quite a spread of answers, so what does the science say?
This is hippie hogwash and hearsay; wishful thinking at best! True or False?
False! We’re tackling this one first, because it’s easiest to answer:
There are some moderately-well established [usually moderate] clinical benefits from some psychedelics for some people.
If that sounds like a very guarded statement, it is. Part of this is because “psychedelics” is an umbrella term; perhaps we should have conducted separate polls for psilocybin, MDMA, ayahuasca, LSD, ibogaine, etc, etc.
In fact: maybe we will do separate main features for some of these, as there is a lot to say about each of them separately.
Nevertheless, looking at the spread of research as it stands for psychedelics as a category, the answers are often similar across the board, even when the benefits/risks may differ from drug to drug.
To speak in broad terms, if we were to make a research summary for each drug it would look approximately like this in each case:
- there has been research into this, but not nearly enough, as “the war on drugs” may well have manifestly been lost (the winner of the war being: drugs; still around and more plentiful than ever), but it did really cramp science for a few decades.
- the studies are often small, heterogenous (often using moderately wealthy white student-age population samples), and with a low standard of evidence (i.e. the methodology often has some holes that leave room for reasonable doubt).
- the benefits recorded are often small and transient.
- in their favor, though, the risks are also generally recorded as being quite low, assuming proper safe administration*.
*Illustrative example:
Person A takes MDMA in a club, dances their cares away, has had only alcohol to drink, sweats buckets but they don’t care because they love everyone and they see how we’re all one really and it all makes sense to them and then they pass out from heat exhaustion and dehydration and suffer kidney damage (not to mention a head injury when falling) and are hospitalized and could die;
Person B takes MDMA in a lab, is overwhelmed with a sense of joy and the clarity of how their participation in the study is helping humanity; they want to hug the researcher and express their gratitude; the researcher reminds them to drink some water.
Which is not to say that a lab is the only safe manner of administration; there are many possible setups for supervised usage sites. But it does mean that the risks are often as much environmental as they are risks inherent to the drug itself.
Others are more inherent to the drug itself, such as adverse cardiac events for some drugs (ibogaine is one that definitely needs medical supervision, for example).
For those who’d like to see numbers and clinical examples of the bullet points we gave above, here you go; this is a great (and very readable) overview:
NIH | Evidence Brief: Psychedelic Medications for Mental Health and Substance Use Disorders
Notwithstanding the word “brief” (intended in the sense of: briefing), this is not especially brief and is rather an entire book (available for free, right there!), but we do recommend reading it if you have time.
This can help a select few people only; useless for the majority: True or False?
True, technically, insofar as the evidence points to these drugs being useful for such things as depression, anxiety, PTSD, addiction, etc, and estimates of people who struggle with mental health issues in general is often cited as being 1 in 4, or 1 in 5. Of course, many people may just have moderate anxiety, or a transient period of depression, etc; many, meanwhile, have it worth.
In short: there is a very large minority of people who suffer from mental health issues that, for each issue, there may be one or more psychedelic that could help.
This is a good, evidence-based way to treat many brain disorders: True or False?
True if and only if we’re willing to accept the so far weak evidence that we discussed above. False otherwise, while the jury remains out.
One thing in its favor though is that while the evidence is weak, it’s not contradictory, insofar as the large preponderance of evidence says such therapies probably do work (there aren’t many studies that returned negative results); the evidence is just weak.
When a thousand scientists say “we’re not completely sure, but this looks like it helps; we need to do more research”, then it’s good to believe them on all counts—the positivity and the uncertainty.
This is a very different picture than we saw when looking at, say, ear candling or homeopathy (things that the evidence says simply do not work).
We haven’t been linking individual studies so far, because that book we linked above has many, and the number of studies we’d have to list would be:
n = number of kinds of psychedelic drugs x number of conditions to be treated
e.g. how does psilocybin fare for depression, eating disorders, anxiety, addiction, PTSD, this, that, the other; now how does ayahuasca fare for each of those, and so on for each drug and condition; at least 25 or 30 as a baseline number, and we don’t have that room.
But here are a few samples to finish up:
- Psilocybin as a New Approach to Treat Depression and Anxiety in the Context of Life-Threatening Diseases—A Systematic Review and Meta-Analysis of Clinical Trials
- Therapeutic Use of LSD in Psychiatry: A Systematic Review of Randomized-Controlled Clinical Trials
- Efficacy of Psychoactive Drugs for the Treatment of Posttraumatic Stress Disorder: A Systematic Review of MDMA, Ketamine, LSD and Psilocybin
- Changes in self-rumination and self-compassion mediate the effect of psychedelic experiences on decreases in depression, anxiety, and stress.
- Psychedelic Treatments for Psychiatric Disorders: A Systematic Review and Thematic Synthesis of Patient Experiences in Qualitative Studies
- Repeated lysergic acid diethylamide (LSD) reverses stress-induced anxiety-like behavior, cortical synaptogenesis deficits and serotonergic neurotransmission decline
In closing…
The general scientific consensus is presently “many of those drugs may ameliorate many of those conditions, but we need a lot more research before we can say for sure”.
On a practical level, an important take-away from this is twofold:
- drugs, even those popularly considered recreational, aren’t ontologically evil, generally do have putative merits, and have been subject to a lot of dramatization/sensationalization, especially by the US government in its famous war on drugs.
- drugs, even those popularly considered beneficial and potentially lifechangingly good, are still capable of doing great harm if mismanaged, so if putting aside “don’t do drugs” as a propaganda of the past, then please do still hold onto “don’t do drugs alone”; trained professional supervision is a must for safety.
Take care!
Share This Post
-
Your friend has been diagnosed with cancer. Here are 6 things you can do to support them
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Across the world, one in five people are diagnosed with cancer during their lifetime. By age 85, almost one in two Australians will be diagnosed with cancer.
When it happens to someone you care about, it can be hard to know what to say or how to help them. But providing the right support to a friend can make all the difference as they face the emotional and physical challenges of a new diagnosis and treatment.
Here are six ways to offer meaningful support to a friend who has been diagnosed with cancer.
1. Recognise and respond to emotions
When facing a cancer diagnosis and treatment, it’s normal to experience a range of emotions including fear, anger, grief and sadness. Your friend’s moods may fluctuate. It is also common for feelings to change over time, for example your friend’s anxiety may decrease, but they may feel more depressed.
Spending time together can mean a lot to someone who is feeling isolated during cancer treatment. Chokniti-Studio/Shutterstock Some friends may want to share details while others will prefer privacy. Always ask permission to raise sensitive topics (such as changes in physical appearance or their thoughts regarding fears and anxiety) and don’t make assumptions. It’s OK to tell them you feel awkward, as this acknowledges the challenging situation they are facing.
When they feel comfortable to talk, follow their lead. Your support and willingness to listen without judgement can provide great comfort. You don’t have to have the answers. Simply acknowledging what has been said, providing your full attention and being present for them will be a great help.
2. Understand their diagnosis and treatment
Understanding your friend’s diagnosis and what they’ll go through when being treated may be helpful.
Being informed can reduce your own worry. It may also help you to listen better and reduce the amount of explaining your friend has to do, especially when they’re tired or overwhelmed.
Explore reputable sources such as the Cancer Council website for accurate information, so you can have meaningful conversations. But keep in mind your friend has a trusted medical team to offer personalised and accurate advice.
3. Check in regularly
Cancer treatment can be isolating, so regular check-ins, texts, calls or visits can help your friend feel less alone.
Having a normal conversation and sharing a joke can be very welcome. But everyone copes with cancer differently. Be patient and flexible in your support – some days will be harder for them than others.
Remembering key dates – such as the next round of chemotherapy – can help your friend feel supported. Celebrating milestones, including the end of treatment or anniversary dates, may boost morale and remind your friend of positive moments in their cancer journey.
Always ask if it’s a good time to visit, as your friend’s immune system may be compromised by their cancer or treatments such as chemotherapy or radiotherapy. If you’re feeling unwell, it’s best to postpone visits – but they may still appreciate a call or text.
4. Offer practical support
Sometimes the best way to show your care is through practical support. There may be different ways to offer help, and what your friend needs might change at the beginning, during and after treatment.
For example, you could offer to pick up prescriptions, drive them to appointments so they have transport and company to debrief, or wait with them at appointments.
Meals will always be welcome. However it’s important to remember cancer and its treatments may affect taste, smell and appetite, as well as your friend’s ability to eat enough or absorb nutrients. You may want to check first if there are particular foods they like. Good nutrition can help boost their strength while dealing with the side effects of treatment.
There may also be family responsibilities you can help with, for example, babysitting kids, grocery shopping or taking care of pets.
There may be practical ways you can help, such as dropping off meals. David Trinks/Unsplash 5. Explore supports together
Studies have shown mindfulness practices can be an effective way for people to manage anxiety associated with a cancer diagnosis and its treatment.
If this is something your friend is interested in, it may be enjoyable to explore classes (either online or in-person) together.
You may also be able to help your friend connect with organisations that provide emotional and practical help, such as the Cancer Council’s support line, which offers free, confidential information and support for anyone affected by cancer, including family, friends and carers.
Peer support groups can also reduce your friend’s feelings of isolation and foster shared understanding and empathy with people who’ve gone through a similar experience. GPs can help with referrals to support programs.
6. Stick with them
Be committed. Many people feel isolated after their treatment. This may be because regular appointments have reduced or stopped – which can feel like losing a safety net – or because their relationships with others have changed.
Your friend may also experience emotions such as worry, lack of confidence and uncertainty as they adjust to a new way of living after their treatment has ended. This will be an important time to support your friend.
But don’t forget: looking after yourself is important too. Making sure you eat well, sleep, exercise and have emotional support will help steady you through what may be a challenging time for you, as well as the friend you love.
Our research team is developing new programs and resources to support carers of people who live with cancer. While it can be a challenging experience, it can also be immensely rewarding, and your small acts of kindness can make a big difference.
Stephanie Cowdery, Research Fellow, Carer Hub: A Centre of Excellence in Cancer Carer Research, Translation and Impact, Deakin University; Anna Ugalde, Associate Professor & Victorian Cancer Agency Fellow, Deakin University; Trish Livingston, Distinguished Professor & Director of Special Projects, Faculty of Health, Deakin University, and Victoria White, Professor of Pyscho-Oncology, School of Psychology, Deakin University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
The Fast-Mimicking Diet
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Live, Fast, Live Long
This is Dr. Valter Longo. He’s a biogerontologist and cell biologist, whose work has focused on fasting and nutrient response genes, and how we can leverage them against diseases and aging in general.
We reviewed his book recently:
What does he want us to know?
What to eat
Dr. Longo recommends a mostly plant-based diet (especially vegetables, whole grains, and legumes), but also having some fish. The bulk of our dietary fats, however, he says are best coming from olive oil and nuts.
He also advises aiming for nutritional density of vitamins and minerals in our diet, and/but supplementing with a multivitamin once every few days to cover any gaps.
If in doubt choosing between plant-based whole foods, he recommends that we choose those our ancestors will have eaten.
Read more: Longevity Diet For Adults
When to eat
Dr. Longo recommends time-restricted eating within a 12-hour window per day.
See also: Intermittent Fasting: We Sort The Science From The Hype
However, he also recommends (additionally or separately; it’s up to us; additionally is better but the point is it still has excellent benefits separately too) his “fast-mimicking diet” (FMD), which involves eating according to what we said in “What to eat”, but restricting it to 750 kcal per day, 5 days in a row, but not necessarily 5 days per week.
For example, the following was a 3-month study that involved doing this for only one 5-day cycle per month:
❝Three FMD cycles reduced body weight, trunk, and total body fat; lowered blood pressure; and decreased insulin-like growth factor 1 (IGF-1). No serious adverse effects were reported.
A post hoc analysis of subjects from both FMD arms showed that body mass index, blood pressure, fasting glucose, IGF-1, triglycerides, total and low-density lipoprotein cholesterol, and C-reactive protein were more beneficially affected in participants at risk for disease than in subjects who were not at risk.
Thus, cycles of a 5-day FMD are safe, feasible, and effective in reducing markers/risk factors for aging and age-related diseases.❞
~ Dr. Min Wei et al. ← Dr. Longo was
Note: the introduction mentions FMD in mice, but this is just referencing previous studies. This study is about FMD in humans!
Read in full: Fasting-mimicking diet and markers/risk factors for aging, diabetes, cancer, and cardiovascular disease
Want to know more?
You might like this (text-based) interview with Dr. Longo, with the Health Sciences Academy:
Eat, fast and live longer? Interview with Professor Valter Longo
Take care!
Share This Post
Related Posts
-
Nature Valley Protein Granola vs Kellog’s All-Bran – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing Nature Valley Protein Granola to Kellog’s All-Bran, we picked the All-Bran.
Why?
While the Protein Granola indeed contains more protein (13g/cup, compared to 5g/cup), it also contains three times as much sugar (18g/cup, compared to 9g/cup) and only ⅓ as much fiber (4g/cup, compared to 12g/cup)
Given that fiber is what helps our bodies to absorb sugar more gently (resulting in fewer spikes), this is extremely important, especially since 18g of sugar in one cup of Protein Granola is already most of the recommended daily allowance, all at once!
For reference: the AHA recommends no more than 25g added sugar for women, or 32g for men
Hence, we went for the option with 3x as much fiber and ⅓ of the sugar, the All-Bran.
For more about keeping blood sugars stable, see:
10 Ways To Balance Blood Sugars
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Lost for words? Research shows art therapy brings benefits for mental health
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Creating art for healing purposes dates back tens of thousands of years, to the practices of First Nations people around the world. Art therapy uses creative processes, primarily visual art such as painting, drawing or sculpture, with a view to improving physical health and emotional wellbeing.
When people face significant physical or mental ill-health, it can be challenging to put their experiences into words. Art therapists support people to explore and process overwhelming thoughts, feelings and experiences through a reflective art-making process. This is distinct from art classes, which often focus on technical aspects of the artwork, or the aesthetics of the final product.
Art therapy can be used to support treatment for a wide range of physical and mental health conditions. It has been linked to benefits including improved self-awareness, social connection and emotional regulation, while lowering levels of distress, anxiety and even pain scores.
In a study published this week in the Journal of Mental Health, we found art therapy was associated with positive outcomes for children and adolescents in a hospital-based mental health unit.
An option for those who can’t find the words
While a person’s engagement in talk therapies may sometimes be affected by the nature of their illness, verbal reflection is optional in art therapy.
Where possible, after finishing an artwork, a person can explore the meaning of their work with the art therapist, translating unspoken symbolic material into verbal reflection.
However, as the talking component is less central to the therapeutic process, art therapy is an accessible option for people who may not be able to find the words to describe their experiences.
Art therapy has supported improved mental health outcomes for people who have experienced trauma, people with eating disorders, schizophrenia and dementia, as well as children with autism.
Art therapy has also been linked to improved outcomes for people with a range of physical health conditions. These include lower levels of anxiety, depression and fatigue among people with cancer, enhanced psychological stability for patients with heart disease, and improved social connection among people who have experienced a traumatic brain injury.
Art therapy has been associated with improved mood and anxiety levels for patients in hospital, and lower pain, tiredness and depression among palliative care patients.
Studies suggest art therapy could support people with a range of health conditions. mojo cp/Shutterstock Our research
Mental ill-health, including among children and young people, presents a major challenge for our society. While most care takes place in the community, a small proportion of young people require care in hospital to ensure their safety.
In this environment, practices that place even greater restriction, such as seclusion or physical restraint, may be used briefly as a last resort to ensure immediate physical safety. However, these “restrictive practices” are associated with negative effects such as post-traumatic stress for patients and health professionals.
Worryingly, staff report a lack of alternatives to keep patients safe. However, the elimination of restrictive practices is a major aim of mental health services in Australia and internationally.
Our research looked at more than six years of data from a child and adolescent mental health hospital ward in Australia. We sought to determine whether there was a reduction in restrictive practices during the periods when art therapy was offered on the unit, compared to times when it was absent.
We found a clear association between the provision of art therapy and reduced frequency of seclusion, physical restraint and injection of sedatives on the unit.
We don’t know the precise reason for this. However, art therapy may have lessened levels of severe distress among patients, thereby reducing the risk they would harm themselves or others, and the likelihood of staff using restrictive practices to prevent this.
This artwork was described by the young person who made it as a dead tree with new growth, representing a sense of hope emerging as they started to move towards their recovery. Author provided That said, hospital admission involves multiple therapeutic interventions including talk-based therapies and medications. Confirming the effect of a therapeutic intervention requires controlled clinical trials where people are randomly assigned one treatment or another.
Although ours was an observational study, randomised controlled trials support the benefits of art therapy in youth mental health services. For instance, a 2011 hospital-based study showed reduced symptoms of post-traumatic stress disorder among adolescents randomised to trauma-focussed art therapy compared to a “control” arts and crafts group.
Artwork made by a young person during an art therapy session in an in-patient mental health unit. Author provided What do young people think?
In previous research we found art therapy was considered by adolescents in hospital-based mental health care to be the most helpful group therapy intervention compared to other talk-based therapy groups and creative activities.
In research not yet published, we’re speaking with young people to better understand their experiences of art therapy, and why it might reduce distress. One young person accessing art therapy in an acute mental health service shared:
[Art therapy] is a way of sort of letting out your emotions in a way that doesn’t involve being judged […] It let me release a lot of stuff that was bottling up and stuff that I couldn’t explain through words.
A promising area
The burgeoning research showing the benefits of art therapy for both physical and especially mental health highlights the value of creative and innovative approaches to treatment in health care.
There are opportunities to expand art therapy services in a range of health-care settings. Doing so would enable greater access to art therapy for people with a variety of physical and mental health conditions.
Sarah Versitano, Academic, Master of Art Therapy Program, Western Sydney University and Iain Perkes, Senior Lecturer, Child and Adolescent Psychiatry, UNSW Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What Seasonal Allergies Mean For Your Heart
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Most people associate seasonal allergies with itchy eyes and stuffy noses, but the effects can go a lot deeper.
This is because allergic reactions don’t just affect the respiratory system; they trigger chronic inflammation throughout the body, and in fact:
❝Allergic disease is a systemic and inflammatory condition❞
~ Dr. Rauno Joks, whose work we will cite in a moment
The important thing to understand in terms of heart health, is that chronic* systemic inflammation can contribute to coronary artery disease, where plaque buildup in arteries (bearing in mind, arterial plaque is in large part made of dead immune cells) raises the risk of heart attacks and strokes.
*Yes, a season once or twice per year counts as “chronic”.
A large (n=603,140) study found that allergic rhinitis (hay fever) increased the odds of coronary heart disease by 25% and heart attacks by 20%. Asthma, especially during flare-ups, posed an even greater risk:
Beyond biology
The effects aren’t just biological; allergies can limit physical activity, leading to a sedentary lifestyle that harms heart health.
In other words: if you’re not going outdoors because there’s pollen, and you’re not exercising because you’re exhausted, then the rest of your health is going to take a nose-dive (so to speak) too.
So, one more reason to take it seriously and not just dismiss it as “it’s just allergies, I’ll survive”.
Practical takeaways
Some things we can all do:
- Monitor your risk factors; i.e. keep on top of your heart health metrics, especially blood pressure and cholesterol, as well as any known genetic predisposition to cardiovascular disease.
- Watch out for alternative causes: symptoms like fatigue or shortness of breath may not always be allergies; they could signal asthma, reflux (for example if wheezing), or even heart disease. An allergist is a good first port-of-call, though.
- Be cautious with medications: some decongestants / allergy meds / asthma meds can raise blood pressure and/or interfere with other medications. Your pharmacist is the best person to speak to about this; they know this kind of thing much better than doctors, as a rule. And whenever you get a new medication, it is good practice to make a habit of always reading the information leaflet that comes with it, and/or look it up on a reputable website such as Drugs.com or the the BNF, to learn about what it is, how it works, what the risks are, what its contraindications are, etc.
- Don’t ignore warning signs: lightheadedness or chest pain could indicate a heart issue and should be addressed immediately. It’s better to be wrong and temporarily embarrassed, than wrong and permanently dead. Besides, even if it’s not a heart issue, it may be something else that would benefit from attention, so taking it seriously is always a good idea.
Want to know more?
Check out:
- What Your Mucus Says About Your Health
- Antihistamines’ Generation Gap
- Oh, Honey: The Bee’s Knees? ← what science has to say about “honey will inoculate you against allergies”
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: