Parents are increasingly saying their child is ‘dysregulated’. What does that actually mean?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Welcome aboard the roller coaster of parenthood, where emotions run wild, tantrums reign supreme and love flows deep.
As children reach toddlerhood and beyond, parents adapt to manage their child’s big emotions and meltdowns. Parenting terminology has adapted too, with more parents describing their child as “dysregulated”.
But what does this actually mean?

More than an emotion
Emotional dysregulation refers to challenges a child faces in recognising and expressing emotions, and managing emotional reactions in social settings.
This may involve either suppressing emotions or displaying exaggerated and intense emotional responses that get in the way of the child doing what they want or need to do.
“Dysregulation” is more than just feeling an emotion. An emotion is a signal, or cue, that can give us important insights to ourselves and our preferences, desires and goals.
An emotionally dysregulated brain is overwhelmed and overloaded (often, with distressing emotions like frustration, disappointment and fear) and is ready to fight, flight or freeze.
Developing emotional regulation
Emotion regulation is a skill that develops across childhood and is influenced by factors such as the child’s temperament and the emotional environment in which they are raised.
In the stage of emotional development where emotion regulation is a primary goal (around 3–5 years old), children begin exploring their surroundings and asserting their desires more actively.

It’s typical for them to experience emotional dysregulation when their initiatives are thwarted or criticised, leading to occasional tantrums or outbursts.
A typically developing child will see these types of outbursts reduce as their cognitive abilities become more sophisticated, usually around the age they start school.
Express, don’t suppress
Expressing emotions in childhood is crucial for social and emotional development. It involves the ability to convey feelings verbally and through facial expressions and body language.
When children struggle with emotional expression, it can manifest in various ways, such as difficulty in being understood, flat facial expressions even in emotionally charged situations, challenges in forming close relationships, and indecisiveness.
Several factors, including anxiety, attention-deficit hyperactivity disorder (ADHD), autism, giftedness, rigidity and both mild and significant trauma experiences, can contribute to these issues.
Common mistakes parents can make is dismissing emotions, or distracting children away from how they feel.
These strategies don’t work and increase feelings of overwhelm. In the long term, they fail to equip children with the skills to identify, express and communicate their emotions, making them vulnerable to future emotional difficulties.
We need to help children move compassionately towards their difficulties, rather than away from them. Parents need to do this for themselves too.
Caregiving and skill modelling
Parents are responsible for creating an emotional climate that facilitates the development of emotion regulation skills.
Parents’ own modelling of emotion regulation when they feel distressed. The way they respond to the expression of emotions in their children, contributes to how children understand and regulate their own emotions.
Children are hardwired to be attuned to their caregivers’ emotions, moods, and coping as this is integral to their survival. In fact, their biggest threat to a child is their caregiver not being OK.
Unsafe, unpredictable, or chaotic home environments rarely give children exposure to healthy emotion expression and regulation. Children who go through maltreatment have a harder time controlling their emotions, needing more brainpower for tasks that involve managing feelings. This struggle could lead to more problems with emotions later on, like feeling anxious and hypervigilant to potential threats.
Recognising and addressing these challenges early on is essential for supporting children’s emotional wellbeing and development.
A dysregulated brain and body
When kids enter “fight or flight” mode, they often struggle to cope or listen to reason. When children experience acute stress, they may respond instinctively without pausing to consider strategies or logic.
If your child is in fight mode, you might observe behaviours such as crying , clenching fists or jaw, kicking, punching, biting, swearing, spitting or screaming.
In flight mode, they may appear restless, have darting eyes, exhibit excessive fidgeting, breathe rapidly, or try to run away.
A shut-down response may look like fainting or a panic attack.
When a child feels threatened, their brain’s frontal lobe, responsible for rational thinking and problem-solving, essentially goes offline.
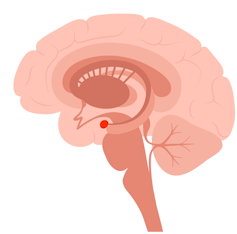
This happens when the amygdala, the brain’s alarm system, sends out a false alarm, triggering the survival instinct.
In this state, a child may not be able to access higher functions like reasoning or decision-making.
While our instinct might be to immediately fix the problem, staying present with our child during these moments is more effective. It’s about providing support and understanding until they feel safe enough to engage their higher brain functions again.
Reframe your thinking so you see your child as having a problem – not being the problem.
Tips for parents
Take turns discussing the highs and lows of the day at meal times. This is a chance for you to be curious, acknowledge and label feelings, and model that you, too, experience a range of emotions that require you to put into practice skills to cope and has shown evidence in numerous physical, social-emotional, academic and behavioural benefits.

Spending even small amounts (five minutes a day!) of quality one-on-one time with your child is an investment in your child’s emotional wellbeing. Let them pick the activity, do your best to follow their lead, and try to notice and comment on the things they do well, like creative ideas, persevering when things are difficult, and being gentle or kind.
Take a tip from parents of children with neurodiversity: learn about your unique child. Approaching your child’s emotions, temperament, and behaviours with curiosity can help you to help them develop emotion regulation skills.
When to get help
If emotion dysregulation is a persistent issue that is getting in the way of your child feeling happy, calm, or confident – or interfering with learning or important relationships with family members or peers – talk to their GP about engaging with a mental health professional.
Many families have found parenting programs helpful in creating a climate where emotions can be safely expressed and shared.
Remember, you can’t pour from an empty cup. Parenting requires you to be your best self and tend to your needs first to see your child flourish.
Cher McGillivray, Assistant Professor Psychology Department, Bond University and Shawna Mastro Campbell, Assistant Professor Psychology, Bond University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Internal Organs Can Be Affected By Spicy Foods (Doctor Explains)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Capsaicin has an array of health-giving properties in moderation, but consumed in immoderation and/or without building up tolerance first, can cause problems—serious health issues such as heart attacks, brain spasms, torn esophagus, and even death can occur.
Heating up
Capsaicin, the compound that gives peppers their “heat”, is a chemical irritant and neurotoxin that activates pain receptors (TRPV1) tricking the brain into sensing heat, leading to a burning sensation, sweating, and flushing. The pain signal can also trigger the fight-or-flight response, causing a surge of adrenaline. Endorphins are eventually released, creating a pain-relief effect similar to a runner’s high, and ultimately it reduces systemic inflammation, boosts the metabolism, and increases healthy longevity.
However, in cases of extreme consumption and/or lack of preparation, woe can befall, for example:
- A man ruptured his esophagus after vomiting from eating a ghost pepper.
- A participant experienced severe brain blood vessel constriction (reversible cerebral vasoconstriction syndrome) after eating a Carolina reaper.
- A 25-year-old suffered permanent heart damage from cayenne pepper pills due to restricted blood flow.
- A teenager died after the “one chip challenge,” although the cause of death was undetermined.
So, what does moderation and preparation look like?
Moderation can be different to different people, since genetics do play a part—some people have more TRPV1 receptors than other people. However, for all people (unless in case of having an allergy or similar), acclimatization is important, and a much bigger factor than genetics.
Writer’s anecdote: on the other hand, when my son was a toddler I once left the room and came back to find him cheerfully drinking hot sauce straight from the bottle, so it can be suspected that genetics are definitely relevant too, as while I did season his food and he did already enjoy curries and such, he didn’t exactly have a background of entering chili-eating competitions.
Still, regardless of genes (unless you actually have a medical condition that disallows this), a person who regularly eats spicy food will develop an increasing tolerance for spicy food, and will get to enjoy the benefits without the risks, provided they don’t suddenly jump way past their point of tolerance.
On which note, in this video you can also see what happens when Dr. Deshauer goes from biting a jalapeño (relatively low on the Scoville heat scale) to biting a Scotch bonnet pepper (about 10x higher on the Scoville heat scale):
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Capsaicin For Weight Loss And Against Inflammation
Take care!
Share This Post
-
Reduce Your Stroke Risk
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
❝Each year in the U.S., over half a million people have a first stroke; however, up to 80% of strokes may be preventable.❞
~ American Stroke Association
Source: New guideline: Preventing a first stroke may be possible with screening, lifestyle changes
So, what should we do?
Some of the risk factors are unavoidable or not usefully avoidable, like genetic predispositions and old age, respectively (i.e. it is possible to avoid old age—by dying young, which is not a good approach).
Some of the risk factors are avoidable. Let’s look at the most obvious first:
You cannot drink to your good health
While overall, the World Health Organization has declared that “the only safe amount of alcohol is zero”, when it comes to stroke risk specifically, it seems that low consumption is not associated with stroke, while moderate to high consumption is associated with a commensurately increased risk of stroke:
Alcohol Intake as a Risk Factor for Acute Stroke
Note: there are some studies out there that say that a low to moderate consumption may decrease the risk compared to zero consumption. However, any such study that this writer has seen has had the methodological flaw of not addressing why those who do not drink alcohol, do not drink it. In many cases, someone who drinks no alcohol at all does so because either a) it would cause problems with some medication(s) they are taking, or b) they used to drink heavily, and quit. In either case, their reasons for not drinking alcohol may themselves be reasons for an increased stroke risk—not the lack of alcohol itself.
Smoke now = stroke later
This one is straightforward; smoking is bad for pretty much everything, and that includes stroke risk, as it’s bad for your heart and brain both, increasing stroke risk by 200–400%:
Smoking and stroke: the more you smoke the more you stroke
So, the advice here of course is: don’t smoke
Diet matters
The American Stroke Association’s guidelines recommend, just for a change, the Mediterranean Diet. This does not mean just whatever is eaten in the Mediterranean region though, and there are specifically foods that are included and excluded, and the ratios matter, so here’s a run-down of what the Mediterranean Diet does and doesn’t include:
The Mediterranean Diet: What Is It Good For? ← what isn’t it good for?!
You can outrun stroke
Or out-walk it; that’s fine too. Most important here is frequency of exercise, more than intensity. So basically, getting those 150 minutes moderate exercise per week as a minimum.
See also: The Doctor Who Wants Us To Exercise Less & Move More
Which is good, because it means we can get a lot of exercise in that doesn’t feel like “having to do” exercise, for example:
Do You Love To Go To The Gym? No? Enjoy These “No-Exercise Exercises”!
Your brain needs downtime too
Your brain (and your heart) both need you to get good regular sleep:
Sleep Disorders in Stroke: An Update on Management
We sometimes say that “what’s good for your heart is good for your brain” (because the heart feeds the brain, and also ultimately clears away detritus), and that’s true here too, so we might also want to prioritize sleep regularity over other factors, even over duration:
How Regularity Of Sleep Can Be Even More Important Than Duration ← this is about adverse cardiovascular events, including ischemic stroke
Keep on top of your blood pressure
High blood pressure is a very modifiable risk factor for stroke. Taking care of the above things will generally take care of this, especially the DASH variation of the Mediterranean diet:
Hypertension: Factors Far More Relevant Than Salt
However, it’s still important to actually check your blood pressure regularly, because sometimes an unexpected extra factor can pop up for no obvious reason. As a bonus, you can do this improved version of the usual blood pressure test, still using just a blood pressure cuff:
Try This At Home: ABI Test For Clogged Arteries
Consider GLP-1 receptor agonists (or…)
GLP-1 receptor agonists (like Ozempic et al.) seem to have cardioprotective and neuroprotective (thus: anti-stroke) activity independent of their weight loss benefits:
Of course, GLP-1 RAs aren’t everyone’s cup of tea, and they do have their downsides (including availability, cost, and the fact benefits reverse themselves if you stop taking them), so if you want a similar effect from a natural approach, there are some foods that work on the body’s incretin responses in the same way as GLP-1 RAs do:
5 Foods That Naturally Mimic The “Ozempic Effect”
Better to know sooner rather than too late
Rather than waiting until one half of our face is drooping to know that there was a stroke risk, here are things to watch out for to know about it before it’s too late:
6 Signs Of Stroke (One Month In Advance)
Take care!
Share This Post
-
How old’s too old to be a doctor? Why GPs and surgeons over 70 may need a health check to practise
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A growing number of complaints against older doctors has prompted the Medical Board of Australia to announce today that it’s reviewing how doctors aged 70 or older are regulated. Two new options are on the table.
The first would require doctors over 70 to undergo a detailed health assessment to determine their current and future “fitness to practise” in their particular area of medicine.
The second would require only general health checks for doctors over 70.
A third option acknowledges existing rules requiring doctors to maintain their health and competence. As part of their professional code of conduct, doctors must seek independent medical and psychological care to prevent harming themselves and their patients. So, this third option would maintain the status quo.
PeopleImages.com – Yuri A/Shutterstock Haven’t we moved on from set retirement ages?
It might be surprising that stricter oversight of older doctors’ performance is proposed now. Critics of mandatory retirement ages in other fields – for judges, for instance – have long questioned whether these rules are “still valid in a modern society”.
However, unlike judges, doctors are already required to renew their registration annually to practise. This allows the Medical Board of Australia not only to access sound data about the prevalence and activity of older practitioners, but to assess their eligibility regularly and to conduct performance assessments if and when they are needed.
What has prompted these proposals?
This latest proposal identifies several emerging concerns about older doctors. These are grounded in external research about the effect of age on doctors’ competence as well as the regulator’s internal data showing surges of complaints about older doctors in recent years.
Studies of medical competence in ageing doctors show variable results. However, the Medical Board of Australia’s consultation document emphasises studies of neurocognitive loss. It explains how physical and cognitive impairment can lead to poor record-keeping, improper prescribing, as well as disruptive behaviour.
The other issue is the number of patient complaints against older doctors. These “notifications” have surged in recent years, as have the number of disciplinary actions against older doctors.
In 2022–2023, the Medical Board of Australia took disciplinary action against older doctors about 1.7 times more often than for doctors under 70.
In 2023, notifications against doctors over 70 were 81% higher than for the under 70s. In that year, patients sent 485 notifications to the Medical Board of Australia about older doctors – up from 189 in 2015.
While older doctors make up only about 5.3% of the doctor workforce in Australia (less than 1% over 80), this only makes the high numbers of complaints more starkly disproportionate.
It’s for these reasons that the Medical Board of Australia has determined it should take further regulatory action to safeguard the health of patients.
So what distinguishes the two new proposed options?
The “fitness to practise” assessment option would entail a rigorous assessment of doctors over 70 based on their specialisation. It would be required every three years after the age of 70 and every year after 80.
Surgeons, for example, would be assessed by an independent occupational physician for dexterity, sight and the ability to give clinical instructions.
Importantly, the results of these assessments would usually be confidential between the assessor and the doctor. Only doctors who were found to pose a substantial risk to the public, which was not being managed, would be obliged to report their health condition to the Medical Board of Australia.
The second option would be a more general health check not linked to the doctor’s specific role. It would occur at the same intervals as the “fitness to practise” assessment. However, its purpose would be merely to promote good health-care decision-making among health practitioners. There would be no general obligation on a doctor to report the results to the Medical Board of Australia.
In practice, both of these proposals appear to allow doctors to manage their own general health confidentially.
Older surgeons could be independently assessed for dexterity, sight and the ability to give clinical instructions. worradirek/Shutterstock The law tends to prioritise patient safety
All state versions of the legal regime regulating doctors, known as the National Accreditation and Registration Scheme, include a “paramountcy” provision. That provision basically says patient safety is paramount and trumps all other considerations.
As with legal regimes regulating childcare, health practitioner regulation prioritises the health and safety of the person receiving the care over the rights of the licensed professional.
Complicating this further, is the fact that a longstanding principle of health practitioner regulation has been that doctors should not be “punished” for errors in practice.
All of this means that reforms of this nature can be difficult to introduce and that the balance between patient safety and professional entitlements must be handled with care.
Could these proposals amount to age discrimination?
It is premature to analyse the legal implications of these proposals. So it’s difficult to say how these proposals interact with Commonwealth age- and other anti-discrimination laws.
For instance, one complication is that the federal age discrimination statute includes an exemption to allow “qualifying bodies” such as the Medical Board of Australia to discriminate against older professionals who are “unable to carry out the inherent requirements of the profession, trade or occupation because of his or her age”.
In broader terms, a licence to practise medicine is often compared to a licence to drive or pilot an aircraft. Despite claims of discrimination, New South Wales law requires older drivers to undergo a medical assessment every year; and similar requirements affect older pilots and air traffic controllers.
Where to from here?
When changes are proposed to health practitioner regulation, there is typically much media attention followed by a consultation and behind-the-scenes negotiation process. This issue is no different.
How will doctors respond to the proposed changes? It’s too soon to say. If the proposals are implemented, it’s possible some older doctors might retire rather than undergo these mandatory health assessments. Some may argue that encouraging more older doctors to retire is precisely the point of these proposals. However, others have suggested this would only exacerbate shortages in the health-care workforce.
The proposals are open for public comment until October 4.
Christopher Rudge, Law lecturer, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Could Just Two Hours Sleep Per Day Be Enough?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Polyphasic Sleep… Super-Schedule Or An Idea Best Put To Rest?
What is it?
Let’s start by defining some terms:
- Monophasic sleep—sleeping in one “chunk” per day. For example, a good night’s “normal” sleep.
- Biphasic sleep—sleeping in two “chunks” per day. Typically, a shorter night’s sleep, with a nap usually around the middle of the day / early afternoon.
- Polyphasic sleep—sleeping in two or more “chunks per day”. Some people do this in order to have more hours awake per day, to do things. The idea is that sleeping this way is more efficient, and one can get enough rest in less time. The most popular schedules used are:
- The Überman schedule—six evenly-spaced 20-minute naps, one every four hours, throughout the 24-hour day. The name is a semi-anglicized version of the German word Übermensch, “Superman”.
- The Everyman schedule—a less extreme schedule, that has a three-hours “long sleep” during the night, and three evenly-spaced 20-minute naps during the day, for a total of 4 hours sleep.
There are other schedules, but we’ll focus on the most popular ones here.
Want to learn about the others? Visit: Polyphasic.Net (a website by and for polyphasic sleep enthusiasts)
Some people have pointed to evidence that suggests humans are naturally polyphasic sleepers, and that it is only modern lifestyles that have forced us to be (mostly) monophasic.
There is at least some evidence to suggest that when environmental light/dark conditions are changed (because of extreme seasonal variation at the poles, or, as in this case, because of artificial changes as part of a sleep science experiment), we adjust our sleeping patterns accordingly.
The counterpoint, of course, is that perhaps when at the mercy of long days/nights at the poles, or no air-conditioning to deal with the heat of the day in the tropics, that perhaps we were forced to be polyphasic, and now, with modern technology and greater control, we are free to be monophasic.
Either way, there are plenty of people who take up the practice of polyphasic sleep.
Ok, But… Why?
The main motivation for trying polyphasic sleep is simply to have more hours in the day! It’s exciting, the prospect of having 22 hours per day to be so productive and still have time over for leisure.
A secondary motivation for trying polyphasic sleep is that when the brain is sleep-deprived, it will prioritize REM sleep. Here’s where the Überman schedule becomes perhaps most interesting:
The six evenly-spaced naps of the Überman schedule are each 20 minutes long. This corresponds to the approximate length of a normal REM cycle.
Consequently, when your head hits the pillow, you’ll immediately begin dreaming, and at the end of your dream, the alarm will go off.
Waking up at the end of a dream, when one hasn’t yet entered a non-REM phase of sleep, will make you more likely to remember it. Similarly, going straight into REM sleep will make you more likely to be aware of it, thus, lucid dreaming.
Read: Sleep fragmentation and lucid dreaming (actually a very interesting and informative lucid dreaming study even if you don’t want to take up polyphasic sleep)
Six 20-minute lucid-dreaming sessions per day?! While awake for the other 22 hours?! That’s… 24 hours per day of wakefulness to use as you please! What sorcery is this?
Hence, it has quite an understandable appeal.
Next Question: Does it work?
Can we get by without the other (non-REM) kinds of sleep?
According to Überman cycle enthusiasts: Yes! The body and brain will adapt.
According to sleep scientists: No! The non-REM slow-wave phases of sleep are essential
Read: Adverse impact of polyphasic sleep patterns in humans—Report of the National Sleep Foundation sleep timing and variability consensus panel
(if you want to know just how bad it is… the top-listed “similar article” is entitled “Suicidal Ideation”)
But what about, for example, the Everman schedule? Three hours at night is enough for some non-REM sleep, right?
It is, and so it’s not as quickly deleterious to the health as the Überman schedule. But, unless you are blessed with rare genes that allow you to operate comfortably on 4 hours per day (you’ll know already if that describes you, without having to run any experiment), it’s still bad.
Adults typically need 7–9 hours of sleep per night, and if you don’t get it, you’ll accumulate a sleep debt. And, importantly:
When you accumulate sleep debt, you are borrowing time at a very high rate of interest!
And, at risk of laboring the metaphor, but this is important too:
Not only will you have to pay it back soon (with interest), you will be hounded by the debt collection agents—decreased cognitive ability and decreased physical ability—until you pay up.
In summary:
- Polyphasic sleep is really very tempting
- It will give you more hours per day (for a while)
- It will give the promised lucid dreaming benefits (which is great until you start micronapping between naps, this is effectively a mini psychotic break from reality lasting split seconds each—can be deadly if behind the wheel of a car, for instance!)
- It is unequivocally bad for the health and we do not recommend it
Bottom line:
Some of the claimed benefits are real, but are incredibly short-term, unsustainable, and come at a cost that’s far too high. We get why it’s tempting, but ultimately, it’s self-sabotage.
(Sadly! We really wanted it to work, too…)
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Boost Your Digestive Enzymes
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ll Try To Make This Easy To Digest
Do you have a digestion-related problem?
If so, you’re far from alone; around 40% of Americans have digestive problems serious enough to disrupt everyday life:
New survey finds forty percent of Americans’ daily lives are disrupted by digestive troubles
…which puts Americans just a little over the global average of 35%:
Mostly likely on account of the Standard American Diet, or “SAD” as it often gets abbreviated in scientific literature.
There’s plenty we can do to improve gut health, for example:
- Making Friends With Your Gut (You Can Thank Us Later)
- Level-Up Your Fiber Intake! (Without Difficulty Or Discomfort)
- How Much Difference Do Probiotic Supplements Make?
Today we’re going to be examining digestive enzyme supplements!
What are digestive enzymes?
Digestive enzymes are enzymes that break down food into stuff we can use. Important amongst them are:
- Protease: breaks down proteins (into amino acids)
- Amylase: breaks down starches (into sugars)
- Lipase: breaks down fats (into fatty acids)
All three are available as popular supplements to aid digestion. How does the science stack up for them?
Protease
For this, we only found animal studies like this one, but the results have been promising:
Amylase
Again, the studies for this alone (not combined with other enzymes) have been solely from animal agriculture; here’s an example:
The Effect of Exogenous Amylase Supplementation on the Nutritional Value of Peas
Lipase
Unlike for protease and amylase, now we have human studies as well, and here’s what they had to say:
❝Lipase supplementation significantly reduced stomach fullness without change of EGG.
Furthermore, lipase supplementation may be helpful in control of FD symptom such as postprandial symptoms❞
~ Dr. Seon-Young Park & Dr. Jong-Sun Rew
Read more: Is Lipase Supplementation before a High Fat Meal Helpful to Patients with Functional Dyspepsia?
(short answer: yes, it is)
More studies found the same, such as:
Lipase Supplementation before a High-Fat Meal Reduces Perceptions of Fullness in Healthy Subjects
All together now!
When we look at studies for combination supplementation of digestive enzymes, more has been done, and/but it’s (as you might expect) less specific.
The following paper gives a good rundown:
Pancrelipase Therapy: A Combination Of Protease, Amylase, & Lipase
Is it safe?
For most people it is quite safe, but if taking high doses for a long time it can cause problems, and also there may be complications if you have diabetes, are otherwise immunocompromised, or have some other conditions (listed towards the end of the above-linked paper, along with further information that we can’t fit in here).
As ever, check with your doctor/pharmacist if you’re not completely sure!
Want some?
We don’t sell them, but for your convenience, here’s an example product on Amazon that contains all three
Enjoy!
We’ll Try To Make This Easy To Digest
Do you have a digestion-related problem?
If so, you’re far from alone; around 40% of Americans have digestive problems serious enough to disrupt everyday life:
New survey finds forty percent of Americans’ daily lives are disrupted by digestive troubles
…which puts Americans just a little over the global average of 35%:
Mostly likely on account of the Standard American Diet, or “SAD” as it often gets abbreviated in scientific literature.
There’s plenty we can do to improve gut health, for example:
- Making Friends With Your Gut (You Can Thank Us Later)
- Level-Up Your Fiber Intake! (Without Difficulty Or Discomfort)
- How Much Difference Do Probiotic Supplements Make?
Today we’re going to be examining digestive enzyme supplements!
What are digestive enzymes?
Digestive enzymes are enzymes that break down food into stuff we can use. Important amongst them are:
- Protease: breaks down proteins (into amino acids)
- Amylase: breaks down starches (into sugars)
- Lipase: breaks down fats (into fatty acids)
All three are available as popular supplements to aid digestion. How does the science stack up for them?
Protease
For this, we only found animal studies like this one, but the results have been promising:
Amylase
Again, the studies for this alone (not combined with other enzymes) have been solely from animal agriculture; here’s an example:
The Effect of Exogenous Amylase Supplementation on the Nutritional Value of Peas
Lipase
Unlike for protease and amylase, now we have human studies as well, and here’s what they had to say:
❝Lipase supplementation significantly reduced stomach fullness without change of EGG.
Furthermore, lipase supplementation may be helpful in control of FD symptom such as postprandial symptoms❞
~ Dr. Seon-Young Park & Dr. Jong-Sun Rew
Read more: Is Lipase Supplementation before a High Fat Meal Helpful to Patients with Functional Dyspepsia?
(short answer: yes, it is)
More studies found the same, such as:
Lipase Supplementation before a High-Fat Meal Reduces Perceptions of Fullness in Healthy Subjects
All together now!
When we look at studies for combination supplementation of digestive enzymes, more has been done, and/but it’s (as you might expect) less specific.
The following paper gives a good rundown:
Pancrelipase Therapy: A Combination Of Protease, Amylase, & Lipase
Is it safe?
For most people it is quite safe, but if taking high doses for a long time it can cause problems, and also there may be complications if you have diabetes, are otherwise immunocompromised, or have some other conditions (listed towards the end of the above-linked paper, along with further information that we can’t fit in here).
As ever, check with your doctor/pharmacist if you’re not completely sure!
Want some?
We don’t sell them, but for your convenience, here’s an example product on Amazon that contains all three
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Sleeping on Your Back after 50; Yay or Nay?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sleeping Differently After 50
Sleeping is one of those things that, at any age, can be hard to master. Some of our most popular articles have been on getting better sleep, and effective sleep aids, and we’ve had a range of specific sleep-related questions, like whether air purifiers actually improve your sleep.
But perhaps there’s an underlying truth hidden in our opening sentence…is sleeping consistently difficult because the way we sleep should change according to our age?
Inspired by Brad and Mike’s video below (which was published to their 5 million+ subscribers!), there are 4 main elements to consider when sleeping on your back after you’ve hit the 50-year mark:
- Degenerative Disk Disease: As you age, your spine may start to show signs of wear and tear, which directly affects comfort while lying on your back.
- Sleep Apnea and Snoring: Sleep Apnea and snoring become more of an issue with age, and sleeping on your back can exacerbate these problems; when you sleep on your back, the soft tissues in your throat, as well as your tongue, “fall back” and partly obstruct your the airway.
- Spinal Stenosis: Spinal Stenosis–the often-age-related narrowing of your spinal canal–can put pressure on the nerves that travel through the spine, which equally makes back-sleeping harder.
- GERD: The all-too-familiar gastroesophageal reflux disease can be more problematic when lying flat on your back, as doing so can allow easy access for stomach acid to move upwards.
Alternatives to Back Sleeping
Referencing the Mayo Clinic’s Sleep Facility’s director, Dr. Virend Somers, today’s video suggests a simple solution: sleeping on your side. The video goes into a bit more detail but, as you know, here at 10almonds we like to cut to the chase.
Modifications for Back Sleeping
If you’re a lifelong back-sleeping and cannot bear the idea of changing to your side, or your stomach, then there are a few modifications that you can make to ease any pain and discomfort.
Most solutions revolve around either leg wedges or pillow adjustments. For instance, if you’re suffering from back pain, try propping your knees up. Or if GERD is your worst enemy, a wedge pillow could help keep that acid down.
As can be expected, the video dives into more detail:
How was the video? If you’ve discovered any great videos yourself that you’d like to share with fellow 10almonds readers, then please do email them to us!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: