Once-A-Week Strategy to Stop Procrastination – by Brad Meir
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Procrastination is perhaps the most frustrating bad habit to kick!
We know we should do the things. We know why we should do the things. We want to do the things. We’re afraid of what will happen if we don’t do the things. And then we… don’t do the things? What is going on?!
Brad Meir has answers, and—what a relief—solutions. But enough about him, because first he wants to focus a little on you:
Why do you procrastinate? No, you’re probably not “just lazy”, and he’ll guide you through figuring out what it is that makes you procrastinate. There’s an exploration of various emotions here, as well as working out: what type of procrastinator are you?
Then, per what you figured out with his guidance, exercises, and tests, it’s time for an action plan.
But, importantly: one you can actually do, because it won’t fall foul of the problems you’ve been encountering so far. The exact mechanism you’ll use may vary a bit based on you, but some tools here are good for everyone—as well as an outline of the mistakes you could easily make, and how to avoid falling into those traps. And, last but very definitely not least, his “once a week plan”, per the title.
All in all, a highly recommendable and potentially life-changing book.
Grab Your Copy of “Once-A-Week Strategy to Stop Procrastination” NOW (don’t put it off!)
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Healthy Recipes When There Are A Lot Of Restrictions
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small 😎
❝I need to cook for a family event and the combined dietary restrictions are: vegetarian, no lactose, no gluten, no nuts, including peanuts and coconuts, no discernible carbs, including lentils and chickpeas, no garlic or onions, no cabbage, no soup, and it can’t be remotely spicy. The nut allergy is of course absolute and we are vegetarian, the other things may be slightly negotiable but I’d like a stress-free dinner. Ideas?❞
That is indeed quite restrictive! But a challenge is (almost) always fun.
To answer generally first: one approach is to do buffet-style dining, with many small dishes. While nuts will still need to be absent, because of the nature of nut allergies, the rest can just be skipped on a per-person basis.
But, let’s see what we can do with a one-dish-fits-all approach!
The biggest challenge seems to be getting protein and flavor. Protein options are more limited without meat, lactose, or legumes, and flavor requires some attention without being able to rely on spices.
To give a sample à la carte menu… With these things in mind, we’ve selected three of our recipes from the recipes section of our site, that will require only minor modifications:
1) Invigorating Sabzi Khordan: skip the walnuts and either partition or omit the scallions, and ensure the cheese is lactose-free (most supermarkets stock lactose-free cheeses, nowadays).
With regard to the flatbreads, you can either skip, or use our gluten-free Healthy Homemade Flatbreads recipe, though it does use chickpea flour and quinoa flour, so the “no discernible carbs” person(s) might still want to skip them. If it’s not an issue on the carbs front, then you might also consider, in lieu of one of the more traditional cheeses, using our High-Protein Paneer recipe which, being vegan, is naturally lactose-free. Also, which is not traditional but would work fine, you might want to add cold hard-boiled halved eggs, since the next course will be light on protein:
2) Speedy Easy Ratatouille: skip the red chili and garlic; that’s all for this one!
3) Black Forest Chia Pudding: the glycemic index of this should hopefully be sufficient to placate the “no discernible carbs” person(s), but if it’s not, we probably don’t have a keto-friendlier dessert than this. And obviously, when it comes to the garnish of “a few almonds, and/or berries, and/or cherries and/or cacao nibs”, don’t choose the almonds.
Want to know more?
For any who might be curious:
Gluten: What’s The Truth? ← this also discusses the differences between an allergy/intolerance/sensitivity—it’s more than just a matter of severity!
Take care!
Share This Post
-
How To Plan For The Unplannable
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
How To Always Follow Through
❝Two roads diverged in a wood, and I—
I took the one less traveled by,
And that has made all the difference:
Now my socks are wet.❞~ with apologies to Robert Frost
The thing is, much like a different Robert wrote, “The best-laid schemes o’ mice an’ men gang aft agley”, and when we have a plan and the unexpected occurs, we often find ourselves in a position of “well then, now what?”
This goes for New Year’s Resolutions that lasted until around January the 4th, and it goes for “xyz in a month” plans of diet, exercise, or so forth.
We’ve written before on bolstering flagging motivation when all is as expected but we just need an extra boost:
How To Keep On Keeping On… Long Term!
…but what about when the unexpected happens?
First rule: wear a belt and suspenders
Not literally, unless that’s your thing. But you might have heard this phrase from the business world, and it applies to healthful practices too:
If your primary plan fails, you need a second one already in place.
In business, we see this as “business continuity management”. For example, your writer here, I have backups for every important piece of tech I own, Internet connections from two different companies in case one goes down, and if there’s a power cut, I have everything accessible and sync’d on a fully-charged tablet so I can complete my work there if necessary. And yes, I have low-tech coffee-brewing equipment too.
In health, we should be as serious. We all learned back in 2020 that grocery stores and supply chains can fail; how do we eat healthily when all that is on sale is an assortment of random odds and ends? The answer, as we now know because hindsight really is 2020 in this case, is to keep a well-stocked pantry of healthy things with a long shelf life. Also a good stock of whatever supplements we take, and medicines, and water. And maintain them and rotate the stock!
And what of exercise? We must not rely on gyms, we can use and enjoy them sure, but we should have at least one good go-to routine for which we need nothing more than a bit of floorspace at home.
If you’re unsure where to start with that one, we strongly recommend this book that we reviewed recently:
Science of Pilates: Understand the Anatomy and Physiology to Perfect Your Practice – by Tracy Ward
Second rule: troubleshoot up front
With any given intended diet or exercise regime or other endeavor, we must ask ourselves: what could prevent me from doing this? Set a timer for at least 10 minutes, and write down as many things as possible. Then plan for those.
You can read a bit more about some of this here, the below article was written about facing depression and anxiety, but if you can enact your plans when unmotivated and fearful, then you will surely be able to enact them when not, so this information is good anyway:
When You Know What You “Should” Do (But Knowing Isn’t The Problem)
Third rule: don’t err the same way twice
We all screw up sometimes. To err is, indeed, human. So to errantly eat the wrong food, or do so at the wrong time, or miss a day’s exercise session etc, these things happen.
Just, don’t let it happen twice.
Once is an outlier; twice is starting to look like a pattern.
How To Break Out Of Cycles Of Self-Sabotage, And Stop Making The Same Mistakes
Enjoy!
Share This Post
-
Hummus vs Guacamole – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing hummus to guacamole, we picked the guacamole.
Why?
First up, let’s assume that the standards are comparable, for example that both have been made with simple whole foods. The hummus is mostly chickpeas with tahini and a little olive oil and some seasoning; the guacamole is mostly avocado with a little lime juice and some seasoning.
In terms of macronutrients, hummus has slightly more protein and fiber, 2x the carbohydrates (but they are healthy carbs), and usually slightly less fat (but the fats are healthy in both cases).
In terms of micronutrients, the hummus is rich in iron and B vitamins, and the guacamole is rich in potassium, magnesium, vitamins C, E, and K.
So far, it’s pretty much tied. What else is there to consider?
We picked the guacamole because some of its nutrients (especially the potassium, magnesium, and vitamin K) are more common deficiencies in most people’s diets than iron and B vitamins. So, on average, it’s probably the one with the nutrients that you need more of at any given time.
So, it was very very close, and it came down to the above as the deciding factor.
However!
- If you like one and not the other? Eat that one; it’s good.
- If you like both but feel like eating one of them in particular? Eat that one; your body is probably needing those nutrients more right now.
- If you are catering for a group of people? Serve both!
- If you are catering for just yourself and would enjoy both? Serve both! There’s nobody to stop you!
Want to read more?
You might like: Avocado Oil vs Olive Oil – Which is Healthier?
Enjoy!
Share This Post
Related Posts
-
How To Nap Like A Pro (No More “Sleep Hangovers”!)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
How To Be An Expert Nap-Artist
There’s a lot of science to say that napping can bring us health benefits—but mistiming it can just make us more tired. So, how to get some refreshing shut-eye, without ending up with a case of the midday melatonin blues?
First, why do we want to nap?
Well, maybe we’re just tired, but there are specific benefits even if we’re not. For example:
- Increased alertness
- Helps with learning
- Improved memory
- Boost to immunity
- Enhance athletic performance
What can go wrong?
There are two main things that can go wrong, physiologically speaking:
- We can overdo it, and not sleep well at night
- We can awake groggy and confused and tired
The first is self-explanatory—it messes with the circadian rhythm. For this reason, we should not sleep more than 90 minutes during the day. If that seems like a lot, and maybe you’ve heard that we shouldn’t sleep more than half an hour, there is science here, so read on…
The second is a matter of sleep cycles. Our brain naturally organizes our sleep into multiples of 20-minute segments, with a slight break of a few minutes between each. Consequently, naps should be:
- 25ish minutes
- 40–45 minutes
- 90ish minutes
If you wake up mid-cycle—for example, because your alarm went off, or someone disturbed you, or even because you needed to pee, you will be groggy, disoriented, and exhausted.
For this reason, a nap of one hour (a common choice, since people like “round” numbers) is a recipe for disaster, and will only work if you take 15 minutes to fall asleep. In which case, it’d really be a nap of 45 minutes, made up of two 20-minute sleep cycles.
Some interruptions are better/worse than others
If you’re in light or REM sleep, a disruption will leave you not very refreshed, but not wiped out either. And as a bonus, if you’re interrupted during a REM cycle, you’re more likely to remember your dreams.
If you’re in deep sleep, a disruption will leave you with what feels like an incredible hangover, minus the headache, and you’ll be far more tired than you were before you started the nap.
The best way to nap
Taking these factors into account, one of the “safest” ways to nap is to set your alarm for the top end of the time-bracket above the one you actually want to nap for (e.g., if you want to nap for 25ish minutes, set your alarm for 45).
Unless you’re very sleep-deprived, you’ll probably wake up briefly after 20–25 minutes of sleep. This may seem like nearer 30 minutes, if it took you some minutes to fall asleep!
If you don’t wake up then, or otherwise fail to get up, your alarm will catch you later at what will hopefully be between your next sleep cycles, or at the very least not right in the middle of one.
When you wake up from a nap before your alarm, get up. This is not the time for “5 more minutes” because “5 more minutes” will never, ever, be refreshing.
Rest well!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Why are tall people more likely to get cancer? What we know, don’t know and suspect
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
People who are taller are at greater risk of developing cancer. The World Cancer Research Fund reports there is strong evidence taller people have a higher chance of of developing cancer of the:
- pancreas
- large bowel
- uterus (endometrium)
- ovary
- prostate
- kidney
- skin (melanoma) and
- breast (pre- and post-menopausal).
But why? Here’s what we know, don’t know and suspect.
Pexels/Andrea Piacquadio Height does increase your cancer risk – but only by a very small amount. Christian Vinces/Shutterstock A well established pattern
The UK Million Women Study found that for 15 of the 17 cancers they investigated, the taller you are the more likely you are to have them.
It found that overall, each ten-centimetre increase in height increased the risk of developing a cancer by about 16%. A similar increase has been found in men.
Let’s put that in perspective. If about 45 in every 10,000 women of average height (about 165 centimetres) develop cancer each year, then about 52 in each 10,000 women who are 175 centimetres tall would get cancer. That’s only an extra seven cancers.
So, it’s actually a pretty small increase in risk.
Another study found 22 of 23 cancers occurred more commonly in taller than in shorter people.
Why?
The relationship between height and cancer risk occurs across ethnicities and income levels, as well as in studies that have looked at genes that predict height.
These results suggest there is a biological reason for the link between cancer and height.
While it is not completely clear why, there are a couple of strong theories.
The first is linked to the fact a taller person will have more cells. For example, a tall person probably has a longer large bowel with more cells and thus more entries in the large bowel cancer lottery than a shorter person.
Scientists think cancer develops through an accumulation of damage to genes that can occur in a cell when it divides to create new cells.
The more times a cell divides, the more likely it is that genetic damage will occur and be passed onto the new cells.
The more damage that accumulates, the more likely it is that a cancer will develop.
A person with more cells in their body will have more cell divisions and thus potentially more chance that a cancer will develop in one of them.
Some research supports the idea having more cells is the reason tall people develop cancer more and may explain to some extent why men are more likely to get cancer than women (because they are, on average, taller than women).
However, it’s not clear height is related to the size of all organs (for example, do taller women have bigger breasts or bigger ovaries?).
One study tried to assess this. It found that while organ mass explained the height-cancer relationship in eight of 15 cancers assessed, there were seven others where organ mass did not explain the relationship with height.
It is worth noting this study was quite limited by the amount of data they had on organ mass.
Is it because tall people have more cells? Halfpoint/Shutterstock Another theory is that there is a common factor that makes people taller as well as increasing their cancer risk.
One possibility is a hormone called insulin-like growth factor 1 (IGF-1). This hormone helps children grow and then continues to have an important role in driving cell growth and cell division in adults.
This is an important function. Our bodies need to produce new cells when old ones are damaged or get old. Think of all the skin cells that come off when you use a good body scrub. Those cells need to be replaced so our skin doesn’t wear out.
However, we can get too much of a good thing. Some studies have found people who have higher IGF-1 levels than average have a higher risk of developing breast or prostate cancer.
But again, this has not been a consistent finding for all cancer types.
It is likely that both explanations (more cells and more IGF-1) play a role.
But more research is needed to really understand why taller people get cancer and whether this information could be used to prevent or even treat cancers.
I’m tall. What should I do?
If you are more LeBron James than Lionel Messi when it comes to height, what can you do?
Firstly, remember height only increases cancer risk by a very small amount.
Secondly, there are many things all of us can do to reduce our cancer risk, and those things have a much, much greater effect on cancer risk than height.
We can take a look at our lifestyle. Try to:
- eat a healthy diet
- exercise regularly
- maintain a healthy weight
- be careful in the sun
- limit alcohol consumption.
And, most importantly, don’t smoke!
If we all did these things we could vastly reduce the amount of cancer.
You can also take part in cancer screening programs that help pick up cancers of the breast, cervix and bowel early so they can be treated successfully.
Finally, take heart! Research also tells us that being taller might just reduce your chance of having a heart attack or stroke.
Susan Jordan, Associate Professor of Epidemiology, The University of Queensland and Karen Tuesley, Postdoctoral Research Fellow, School of Public Health, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
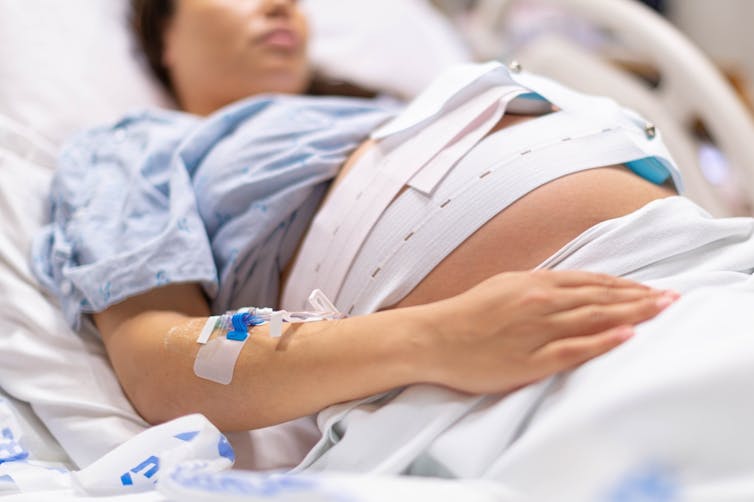
What is a ‘vaginal birth after caesarean’ or VBAC?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A vaginal birth after caesarean (known as a VBAC) is when a woman who has had a caesarean has a vaginal birth down the track.
In Australia, about 12% of women have a vaginal birth for a subsequent baby after a caesarean. A VBAC is much more common in some other countries, including in several Scandinavian ones, where 45-55% of women have one.
So what’s involved? What are the risks? And who’s most likely to give birth vaginally the next time round?
MVelishchuk/Shutterstock What happens? What are the risks?
When a woman chooses a VBAC she is cared for much like she would during a planned vaginal birth.
However, an induction of labour is avoided as much as possible, due to the slightly increased risk of the caesarean scar opening up (known as uterine rupture). This is because the medication used in inductions can stimulate strong contractions that put a greater strain on the scar.
In fact, one of the main reasons women may be recommended to have a repeat caesarean over a vaginal birth is due to an increased chance of her caesarean scar rupturing.
This is when layers of the uterus (womb) separate and an emergency caesarean is needed to deliver the baby and repair the uterus.
Uterine rupture is rare. It occurs in about 0.2-0.7% of women with a history of a previous caesarean. A uterine rupture can also happen without a previous caesarean, but this is even rarer.
However, uterine rupture is a medical emergency. A large European study found 13% of babies died after a uterine rupture and 10% of women needed to have their uterus removed.
The risk of uterine rupture increases if women have what’s known as complicated or classical caesarean scars, and for women who have had more than two previous caesareans.
Most care providers recommend you avoid getting pregnant again for around 12 months after a caesarean, to allow full healing of the scar and to reduce the risk of the scar rupturing.
National guidelines recommend women attempt a VBAC in hospital in case emergency care is needed after uterine rupture.
During a VBAC, recommendations are for closer monitoring of the baby’s heart rate and vigilance for abnormal pain that could indicate a rupture is happening.
If labour is not progressing, a caesarean would then usually be advised.
Giving birth in hospital is recommended for a vaginal birth after a caesarean. christinarosepix/Shutterstock Why avoid multiple caesareans?
There are also risks with repeat caesareans. These include slower recovery, increased risks of the placenta growing abnormally in subsequent pregnancies (placenta accreta), or low in front of the cervix (placenta praevia), and being readmitted to hospital for infection.
Women reported birth trauma and post-traumatic stress more commonly after a caesarean than a vaginal birth, especially if the caesarean was not planned.
Women who had a traumatic caesarean or disrespectful care in their previous birth may choose a VBAC to prevent re-traumatisation and to try to regain control over their birth.
We looked at what happened to women
The most common reason for a caesarean section in Australia is a repeat caesarean. Our new research looked at what this means for VBAC.
We analysed data about 172,000 low-risk women who gave birth for the first time in New South Wales between 2001 and 2016.
We found women who had an initial spontaneous vaginal birth had a 91.3% chance of having subsequent vaginal births. However, if they had a caesarean, their probability of having a VBAC was 4.6% after an elective caesarean and 9% after an emergency one.
We also confirmed what national data and previous studies have shown – there are lower VBAC rates (meaning higher rates of repeat caesareans) in private hospitals compared to public hospitals.
We found the probability of subsequent elective caesarean births was higher in private hospitals (84.9%) compared to public hospitals (76.9%).
Our study did not specifically address why this might be the case. However, we know that in private hospitals women access private obstetric care and experience higher caesarean rates overall.
What increases the chance of success?
When women plan a VBAC there is a 60-80% chance of having a vaginal birth in the next birth.
The success rates are higher for women who are younger, have a lower body mass index, have had a previous vaginal birth, give birth in a home-like environment or with midwife-led care.
For instance, an Australian study found women who accessed continuity of care with a midwife were more likely to have a successful VBAC compared to having no continuity of care and seeing different care providers each time.
An Australian national survey we conducted found having continuity of care with a midwife when planning a VBAC can increase women’s sense of control and confidence, increase their chance to be upright and active in labour and result in a better relationship with their health-care provider.
Seeing the same midwife throughout your maternity care can help. Tyler Olson/Shutterstock Why is this important?
With the rise of caesareans globally, including in Australia, it is more important than ever to value vaginal birth and support women to have a VBAC if this is what they choose.
Our research is also a reminder that how a woman gives birth the first time greatly influences how she gives birth after that. For too many women, this can lead to multiple caesareans, not all of them needed.
Hannah Dahlen, Professor of Midwifery, Associate Dean Research and HDR, Midwifery Discipline Leader, Western Sydney University; Hazel Keedle, Senior Lecturer of Midwifery, Western Sydney University, and Lilian Peters, Adjunct Research Fellow, Western Sydney University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: