
What is ‘double pneumonia’, the condition that’s put Pope Francis in hospital?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Pope Francis has been in hospital for more than a week with what some media reports are now calling “double pneumonia”.
The Vatican released a statement on Tuesday evening saying
laboratory tests, chest X-rays, and the clinical condition of the Holy Father continue to present a complex picture.
The 88-year-old Catholic leader has a long history of respiratory illness.
So, what makes this bout of pneumonia – a severe lung infection – so “complex”? And how will it be treated?

What is double pneumonia?
Pneumonia is a serious infection that fills the lungs with liquid or pus and can make it difficult to breathe. People may also have chest pain, cough up green mucus and have a fever.
“Double pneumonia” is not an official medical term. It may be being used to describe two different aspects of Pope Francis’s condition.
1. A bilateral infection
Pope Francis has pneumonia in both lungs. This is known as “bilateral pneumonia”.
An infection in both lungs doesn’t necessarily mean it’s more severe, but location is important. It can make a difference which parts of the lung are affected.
When just one part of the lung or one lung is affected, the person can continue to breathe using the other lung while their body fights the infection.
However when both lungs are compromised, the person will be receiving very little oxygen.
2. A polymicrobial infection
The Vatican has also said the infection affecting Pope Francis’s lungs is “polymicrobial”.
This means the infection is being caused by more than one kind of microorganism (or “pathogen”).
So, the cause could be two (or more) different kinds of bacteria, or any combination of bacteria, virus and fungus. It’s vital to know what’s causing the infection to effectively treat it.
How is it diagnosed?
Usually, when someone presents with suspected pneumonia the hospital will sample their lungs with a sputum test or swab.
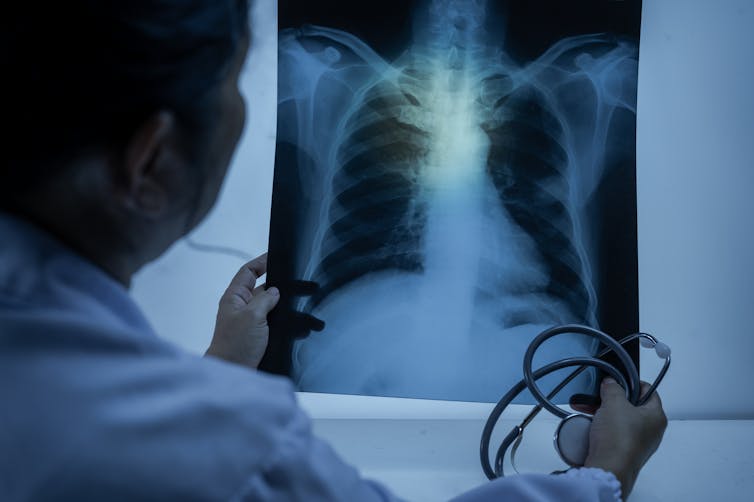
They will often also undergo an X-ray, usually to confirm which parts of the lung are involved.
Healthy lungs look “empty” on an X-ray, because they are filled with air. But pneumonia fills the lungs with fluid.
This means it’s usually very easy to see where pneumonia is affecting them, because the infection shows up as solid white mass on the scan.
How is it treated?
The sputum or swab helps detect what is causing the infection and determine treatment. For example, a specific antibiotic will be used to target a certain bacterium.
Usually this works well. But if the infection is polymicrobial, the normal treatment might not be effective.
For example, the antibiotics may work on the bacteria. But if there’s also a virus – which can’t be treated with antibiotics – it may become the dominant pathogen driving the infection.
As a result, the patient may initially respond well to medication and then begin deteriorating again.
If the infection is caused by multiple bacteria, the patient might be given a broad-spectrum antibiotic rather than a single targeted drug.
A viral infection is harder to treat, as the anti-viral drugs that are available aren’t very effective or targeted.
In severe cases, a patient will also need to be in intensive care on a breathing machine because they can’t breathe alone. This helps make sure they receive enough oxygen while their body fights the infection.
Who is most susceptible?
It’s possible to recover, even from severe infections. However having pneumonia can damage the lungs, and this can make a repeat infection more likely.
Most people will never have a severe infection from these same pathogens. They may only experience a minor cold or flu, because their immune system can adequately fight the infection.
However, certain groups are much more vulnerable to developing a serious case of pneumonia.
Risk factors include:
- age: babies under two, whose immune systems are still developing, and adults over 65, who tend to have weakened immune systems
- lung damage: previous infections can cause scarring
- lung disease: for example, if you have emphysema or chronic obstructive pulmonary disease
- being a smoker
- immunosuppression: if your immune system is weakened, for example by medication you take after a transplant or during cancer treatment.
Pope Francis has a number of these risk factors. The pontiff is 88 years old and has a history of respiratory illness.
He also had pleurisy (a condition that inflames the lungs) as a young adult. As a result, he had part of one lung removed, making him susceptible to lung infections.
On Tuesday, the Vatican said Pope Francis remains “in good spirits” while he receives medical care and is grateful for the support he has received.
Brian Oliver, Professor, School of Life Sciences, University of Technology Sydney and Min Feng, PhD Candidate in Respiratory Disease, University of Technology Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Just One Thing – by Dr. Michael Mosley
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is a collection of easy-to-implement changes that have good science behind them to show how they can benefit us. Some things are obvious (e.g: drink water); others, less so (e.g: sing, to reduce inflammation).
The book is divided thematically into times of the day, though in many cases it’s not a hard rule that a thing needs to be done at a certain time. Others are, like a cold shower in the morning and hot bath before bed—you might not want to switch those around!
The style is very pop-science, and does not have in-line citations for claims, but it does have a bibliography in the bag organized by each “one thing”, e.g. it might say “get some houseplants” and then list a number of references supporting that, with links to the studies showing how that helps. For those with the paper version, don’t worry, you can copy the URL from the book into your browser and see it that way. In any case, there are 2–6 scientific references for each claim, which is very respectable for a pop-sci book.
Bottom line: if you’re looking for evidence-based “one little thing” changes that can make a big difference, this book has lots!
Click here to check out Just One Thing, and improve your life!
Share This Post
-
Yes, adults can develop food allergies. Here are 4 types you need to know about
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
If you didn’t have food allergies as a child, is it possible to develop them as an adult? The short answer is yes. But the reasons why are much more complicated.
Preschoolers are about four times more likely to have a food allergy than adults and are more likely to grow out of it as they get older.
It’s hard to get accurate figures on adult food allergy prevalence. The Australian National Allergy Council reports one in 50 adults have food allergies. But a US survey suggested as many as one in ten adults were allergic to at least one food, with some developing allergies in adulthood.
What is a food allergy
Food allergies are immune reactions involving immunoglobulin E (IgE) – an antibody that’s central to triggering allergic responses. These are known as “IgE-mediated food allergies”.
Food allergy symptoms that are not mediated by IgE are usually delayed reactions and called food intolerances or hypersensitivity.
Food allergy symptoms can include hives, swelling, difficulty swallowing, vomiting, throat or chest tightening, trouble breathing, chest pain, rapid heart rate, dizziness, low blood pressure or anaphylaxis.
Symptoms include hives. wisely/Shutterstock IgE-mediated food allergies can be life threatening, so all adults need an action management plan developed in consultation with their medical team.
Here are four IgE-mediated food allergies that can occur in adults – from relatively common ones to rare allergies you’ve probably never heard of.
1. Single food allergies
The most common IgE-mediated food allergies in adults in a US survey were to:
- shellfish (2.9%)
- cow’s milk (1.9%)
- peanut (1.8%)
- tree nuts (1.2%)
- fin fish (0.9%) like barramundi, snapper, salmon, cod and perch.
In these adults, about 45% reported reacting to multiple foods.
This compares to most common childhood food allergies: cow’s milk, egg, peanut and soy.
Overall, adult food allergy prevalence appears to be increasing. Compared to older surveys published in 2003 and 2004, peanut allergy prevalence has increased about three-fold (from 0.6%), while tree nuts and fin fish roughly doubled (from 0.5% each), with shellfish similar (2.5%).
While new adult-onset food allergies are increasing, childhood-onset food allergies are also more likely to be retained into adulthood. Possible reasons for both include low vitamin D status, lack of immune system challenges due to being overly “clean”, heightened sensitisation due to allergen avoidance, and more frequent antibiotic use.
Some adults develop allergies to cow’s milk, while others retain their allergy from childhood. Sarah Swinton/Unsplash 2. Tick-meat allergy
Tick-meat allergy, also called α-Gal syndrome or mammalian meat allergy, is an allergic reaction to galactose-alpha-1,3-galactose, or α-Gal for short.
Australian immunologists first reported links between α-Gal syndrome and tick bites in 2009, with cases also reported in the United States, Japan, Europe and South Africa. The US Centers for Disease Control estimates about 450,000 Americans could be affected.
The α-Gal contains a carbohydrate molecule that is bound to a protein molecule in mammals.
The IgE-mediated allergy is triggered after repeated bites from ticks or chigger mites that have bitten those mammals. When tick saliva crosses into your body through the bite, antibodies to α-Gal are produced.
When you subsequently eat foods that contain α-Gal, the allergy is triggered. These triggering foods include meat (lamb, beef, pork, rabbit, kangaroo), dairy products (yoghurt, cheese, ice-cream, cream), animal-origin gelatin added to gummy foods (jelly, lollies, marshmallow), prescription medications and over-the counter supplements containing gelatin (some antibiotics, vitamins and other supplements).
Tick-meat allergy reactions can be hard to recognise because they’re usually delayed, and they can be severe and include anaphylaxis. Allergy organisations produce management guidelines, so always discuss management with your doctor.
3. Fruit-pollen allergy
Fruit-pollen allergy, called pollen food allergy syndrome, is an IgE-mediated allergic reaction.
In susceptible adults, pollen in the air provokes the production of IgE antibodies to antigens in the pollen, but these antigens are similar to ones found in some fruits, vegetables and herbs. The problem is that eating those plants triggers an allergic reaction.
The most allergenic tree pollens are from birch, cypress, Japanese cedar, latex, grass, and ragweed. Their pollen can cross-react with fruit and vegetables, including kiwi, banana, mango, avocado, grapes, celery, carrot and potato, and some herbs such as caraway, coriander, fennel, pepper and paprika.
Fruit-pollen allergy is not common. Prevalence estimates are between 0.03% and 8% depending on the country, but it can be life-threatening. Reactions range from itching or tingling of lips, mouth, tongue and throat, called oral allergy syndrome, to mild hives, to anaphylaxis.
4. Food-dependent, exercise-induced food allergy
During heavy exercise, the stomach produces less acid than usual and gut permeability increases, meaning that small molecules in your gut are more likely to escape across the membrane into your blood. These include food molecules that trigger an IgE reaction.
If the person already has IgE antibodies to the foods eaten before exercise, then the risk of triggering food allergy reactions is increased. This allergy is called food-dependent exercise-induced allergy, with symptoms ranging from hives and swelling, to difficulty breathing and anaphylaxis.
This type of allergy is extremely rare. Ben O’Sullivan/Unsplash Common trigger foods include wheat, seafood, meat, poultry, egg, milk, nuts, grapes, celery and other foods, which could have been eaten many hours before exercising.
To complicate things even further, allergic reactions can occur at lower levels of trigger-food exposure, and be more severe if the person is simultaneously taking non-steroidal inflammatory medications like aspirin, drinking alcohol or is sleep-deprived.
Food-dependent exercise-induced allergy is extremely rare. Surveys have estimated prevalence as between one to 17 cases per 1,000 people worldwide with the highest prevalence between the teenage years to age 35. Those affected often have other allergic conditions such as hay fever, asthma, allergic conjunctivitis and dermatitis.
Allergies are a growing burden
The burden on physical health, psychological health and health costs due to food allergy is increasing. In the US, this financial burden was estimated as $24 billion per year.
Adult food allergy needs to be taken seriously and those with severe symptoms should wear a medical information bracelet or chain and carry an adrenaline auto-injector pen. Concerningly, surveys suggest only about one in four adults with food allergy have an adrenaline pen.
If you have an IgE-mediated food allergy, discuss your management plan with your doctor. You can also find more information at Allergy and Anaphylaxis Australia.
Clare Collins, Laureate Professor in Nutrition and Dietetics, University of Newcastle
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Longevity… Simplified – by Dr. Howard Luks
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In the spirit of the book itself, we’ll keep this one simple:
The information in this book will not be new to regular readers of 10almonds, or at least, not if you’ve been with us for a while (because we can only cover so much per day, so long-time readers will have accumulated more knowledge).
On the other hand, the information is clear, correct, and very much stripped down to the most important basics. Not the very simplest basics, which would be an oversimplification to the point of inutility, but the most important basics.
To take an example, when it comes to exercise, he doesn’t say “exercise more” but rather that “a complete exercise program has four pillars: aerobic training, resistance training, balance training, and high-intensity interval training (HIIT)”, and then he goes about explaining, in clear and simple terms, how to do those.
The style is similar when it comes to diet, sleep, and body-part-specific chapters such as about heart health, brain health, and so forth.
Bottom line: if you’re a long-time 10almonds reader, you probably don’t need this one, but it’d be a great book for someone else who has expressed an interest in getting healthier, as it really is a top-tier “primer” in increasing health and healthspan.
Click here to check out Longevity… Simplified, and enjoy simplified longevity!
Share This Post
Related Posts
-
How To Beat Loneliness & Isolation
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Overcoming Loneliness & Isolation
One of the biggest mental health threats that faces many of us as we get older is growing isolation, and the loneliness that can come with it. Family and friends thin out over the years, and getting out and about isn’t always as easy as it used to be for everyone.
Nor is youth a guaranteed protection against this—in today’s world of urban sprawl and nothing-is-walkable cities, in which access to social spaces such as cafés and the like means paying the rising costs with money that young people often don’t have… And that’s without getting started on how much the pandemic impacted an entire generation’s social environments (or lack thereof).
Why is this a problem?
Humans are, by evolution, social creatures. As individuals we may have something of a spectrum from introvert to extrovert, but as a species, we thrive in community. And we suffer, when we don’t have that.
What can we do about it?
We can start by recognizing our needs, such as they are, and identifying to what extent they are being met (or not).
- Some of us may be very comfortable with a lot of alone time—but need someone to talk to sometimes.
- Some of us may need near-constant company to feel at our best—and that’s fine too! We just need to plan accordingly.
In the former case, it’s important to remember that needing someone to talk to is not being a burden to them. Not only will our company probably enrich them too, but also, we are evolved to care for one another, and that itself can bring fulfilment to them as much as to you. But what if you don’t a friend to talk to?
- You might be surprised at who would be glad of you reaching out. Have a think through whom you know, and give it a go. This can be scary, because what if they reject us, or worse, they don’t reject us but silently resent us instead? Again, they probably won’t. Human connection requires taking risks and being vulnerable sometimes.
- If that’s not an option, there are services that can fill your need. For some, therapy might serve a dual purpose in this regard. For others, you might want to check out the list of (mostly free) resources at the bottom of this article
In the second case (that we need near-constant company to feel at our best) we probably need to look more at our overall lifestyle, and find ways to be part of a community. That can include:
- Living in a close-knit community (places with a lot of retirees in one place often have this; or younger folk might look at communal living/working spaces, for example)
- Getting involved in local groups (you can check out NextDoor.com or MeetUp.com for this)
- Volunteering for a charity (not only are acts of service generally fulfilling in and of themselves, but also, you will probably be working with other people of a charitable nature, and such people tend to make for good company!)
Need a little help?
There are many, many organizations that will love to help you (or anyone else) overcome loneliness and isolation.
Rather than list them all here and make this email very long by describing how each of them works, here’s a great compilation of resources:
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The S.T.E.P.S. To A Healthier Heart
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Stepping Into Better Heart Health
This is Dr. Jennifer H. Mieres, FACC, FAHA, MASNC. she’s an award-winning (we counted 9 major awards) professor of cardiology, and a leading advocate for women’s heart health. This latter she’s done via >70 scientific publications, >100 research presentations at national and international conferences, 3 books so far, and 4 documentaries, including the Emmy-nominated “A Woman’s Heart”.
What does she want us to know?
A lot of her work is a top-down approach, working to revolutionize the field of cardiology in its application, to result in far fewer deaths annually. Which is fascinating, but unless you’re well-placed in that industry, not something too actionable as an individual (if you are well-placed in that industry, do look her up, of course).
For the rest of us…
Dr. Mieres’ S.T.E.P.S. to good heart health
She wants us to do the following things:
1) Stock your kitchen with heart health in mind
This is tied to the third item in the list of course, but it’s a critical step not to be overlooked. It’s all very well to know “eat more fiber; eat less red meat” and so forth, but if you go to your kitchen and what’s there is not conducive to heart health, you’re just going to do the best with what’s available.
Instead, actually buy foods that are high in fiber, and preferably, foods that you like. Not a fan of beans? Don’t buy them. Love pasta? Go wholegrain. Like leafy greens in principle, but they don’t go with what you cook? Look up some recipes, and then buy them.
Love a beef steak? Well we won’t lie to you, that is not good for your heart, but make it a rare option—so to speak—and enjoy it mindfully (see also: mindful eating) once in a blue moon for a special occasion, rather than “I don’t know what to cook tonight, so sizzle sizzle I guess”.
Meal planning goes a long way for this one! And if meal-planning sounds like an overwhelming project to take on, then consider trying one of the many healthy-eating meal kit services that will deliver ingredients (and their recipes) to your door—opting for a plants-forward plan, and the rest should fall into place.
2) Take control of your activity
Choose to move! Rather than focusing on what you can’t do (let’s say, those 5am runs, or your regularly-scheduled, irregularly attended, gym sessions), focus on what you can do, and do it.
See also: No-Exercise Exercise!
3) Eat for a healthier heart
This means following through on what you did on the first step, and keeping it that way. Buying fresh fruit and veg is great, but you also have to actually eat it. Do not let the perishables perish!
For you too, dear reader, are perishable (and would presumably like to avoid perishing).
This item in the list may seem flippant, but actually this is about habit-forming, and without it, the whole plan will grind to a halt a few days after your first heart-health-focused shopping trip.
See also: Where Nutrition Meets Habits!
4) Partner with your doctor, family, and friends
Good relationships, both professional and personal, count for a lot. Draw up a plan with your doctor; don’t just guess at when to get this or that checked—or what to do about it if the numbers aren’t to your liking.
Partnership with your doctor goes both ways, incidentally. Read up, have opinions, discuss them! Doing so will ultimately result in better care than just going in blind and coming out with a recommendation you don’t understand and just trust (but soon forget, because you didn’t understand).
And as for family and friends, this is partly about social factors—we tend to influence, and be influenced by, those around us. It can be tricky to be on a health kick if your partner wants take-out every night, so some manner of getting everyone on the same page is important, be it by compromise or, in an ideal world, gradually trending towards better health. But any such changes must come from a place of genuine understanding and volition, otherwise at best they won’t stick, and at worst they’ll actively create a pushback.
Same goes for exercise as for diet—exercising together is a good way to boost commitment, especially if it’s something fun (dance classes are a fine example that many couples enjoy, for example).
5) Sleep more, stress less, savor life
These things matter a lot! Many people focus on cutting down salt or saturated fat, and that can be good if otherwise consumed to excess, but for most people they’re not the most decisive factors:
Hypertension: Factors Far More Relevant Than Salt ← sleep features here!
Stress is also a huge one, and let’s put it this way: people more often have heart attacks during a moment of excessive emotional stress—not during a moment when they had a bit too much butter on their toast.
It’s not even just that acute stress is the trigger, it’s that chronic stress is a contributory factor that erodes the body’s ability to handle the acute stress.
Changing this may seem “easier said than done” because often the stressors are external (e.g. work pressure, financial worries, caring for a sick relative, relationship troubles, major life change, etc), but it is possible to find peace even in the chaos of life:
Want to know more from Dr. Mieres?
You might like this book of hers, which goes into each of the above items in much more depth than we have room to here:
Heart Smarter for Women: Six Weeks to a Healthier Heart – by Dr. Jennifer Mieres
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Ex-Cyclone Alfred has left flooding in its wake. Here’s how floods affect our health
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Ex-Cyclone Alfred is bringing significant rainfall to southeast Queensland and the Northern Rivers of New South Wales. Flooding has hit Lismore, Ballina, Grafton, Brisbane and Hervey Bay, which received 150 mm of rainfall in two hours this morning.
Tragically, a 61-year-old man died after being swept away in floodwaters near Dorrigo in northern New South Wales.
More heavy rain and flash flooding is expected in the coming days as the weather system moves inland and weakens.
Climate change is making these weather events more intense and frequent. Earlier this year, far north Queensland experienced major flooding. As residents of the Northern Rivers, this latest disaster is especially tough because only three years ago we faced the catastrophic 2022 floods.
We’ve studied the impact of floods on human health and wellbeing, and found floods are linked to a range of physical and mental health effects in both the short- and long-term.
So what might you experience if you live in an area affected by these floods?
We reviewed the evidence
We recently reviewed research on the physical and mental health impacts of floods across mainland Australia. We included 69 studies in our review, published over 70 years. The majority were from the past ten years, examining the effects of floods in Queensland and NSW.
These studies suggest people can expect a range of health impacts. Immediate physical health effects of floods include drowning, falls and injuries.
Chronic diseases such as diabetes or renal disease can also worsen due to factors such as reduced access to transport, health-care services, medications and hospitals.
Exposure to contaminated floodwaters can lead to skin infections, while respiratory problems can occur due to mould and damp housing in the aftermath of floods.
Floods also create ideal conditions for mosquito borne infections such as Ross River virus and Murray Valley encephalitis, while also spreading infectious diseases including leptospirosis, a bacterial infection from contaminated soil.
There are mental health consequences too
Our review showed floods also affect mental health. The more you’re exposed to floodwaters in your home or business, the worse the mental health impacts are likely to be.
The After the Flood study examined mental health and wellbeing outcomes six months after the 2017 flood in the Northern Rivers. It found people who had floodwater in their home, yard or business, or who were displaced from their home for a more than six months, were much more likely to have probable post-traumatic stress disorder, anxiety or depression, compared to those who didn’t experience flooding or weren’t displaced.
Repeated natural disasters could compound these mental health consequences. Southeast Queensland and the Northern Rivers in NSW have experienced multiple disasters over recent years. The Northern Rivers faced major flooding in 2017, bushfires in 2020, further major floods in 2022, and now Cyclone Alfred in 2025. These repeated disasters have taken a toll on our community, creating a seemingly never-ending cycle of recovery, rebuilding and preparation for the next disaster.
Our understanding of the unique challenges faced by communities which experience multiple disasters is still growing. However, a recent Australian study showed exposure to repeated disasters has a compounding effect on people’s mental health, leading to worse mental health outcomes compared to people who experience a single disaster.
Mums and babies
The health effects of floods extend far beyond the initial emergency and beyond the infections and mental health consequences you might expect.
The Queensland Flood Study tracked pregnant women exposed to the 2011 Brisbane floods. Researchers assessed mothers’ stress related to the flood and tracked them and their children at six weeks old, six months, 16 months, 2.5 years, four and six years. It found some links between prenatal stress and developmental outcomes in children.
Some evidence suggests maternal stress from floods can affect children’s development. Nastyaofly/Shutterstock While the health effects after flooding are diverse, the research to date is not comprehensive. We need to learn more about how floods contribute to or exacerbate existing chronic illnesses, disability and long-term mental health issues.
The impacts are inequitable
Flooding exposes and worsens existing inequalities. Socially vulnerable groups are more likely to be exposed to flooding in their homes and have less access to resources to respond and recover from these events, putting some groups at higher risk of negative health impacts afterwards.
Some research has looked at the disproportionate impacts on people with disabilities and their carers, First Nations communities and people from disadvantaged backgrounds.
After the 2017 Northern Rivers floods, for example, people with disability and their carers were more likely than others to:
- experience disrupted access to food, support networks and essentials such as health care and social services
- continue to be distressed about the flood six months after it happened
- be at relatively high risk of post-traumatic stress disorder six months after the flood.
However, targeted flood research exploring the experiences of these vulnerable groups in Australia is limited.
Moving forward, it’s vital we examine the varied impacts of flood events for more vulnerable groups, so we can better support them in the wake of devastating events such as Cyclone Alfred.
If this article has raised issues for you, or if you’re concerned about someone you know, call Lifeline on 13 11 14.
Jodie Bailie, Senior Research Fellow, The University Centre for Rural Health and The Centre for Disability Research and Policy, University of Sydney; Jo Longman, Senior Research Fellow, The University Centre for Rural Health, University of Sydney; Rebecca McNaught, Research Fellow, Rural and Remote Health, University of Sydney, and Ross Bailie, School of Public Health, Honorary Professor, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:












