Almond Butter vs Cashew Butter – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing almond butter to cashew butter, we picked the almond.
Why?
It’s not just our pro-almonds bias! And of course exact nutritional values may vary depending on the recipe, but we’re using the USDA’s standardized figures which should represent a reasonable average. Specifically, we’re looking at the USDA entries for “[Nut] butter, plain, without salt added”.
In terms of macros, almond butter takes the lead immediately with nearly 2x the protein and over 3x the fiber. In contrast, cashew butter has 1.5x the carbs, and the two nut butters are approximately equal on fat. An easy win for almond butter so far.
When it comes to vitamins, almond butter has more of vitamins A, B2, B3, B5, E, and choline, while cashew butter has more of vitamins B1, B6, and K. Thus, a 6:3 win for almond butter.
In the category of minerals, things are closer, but almond butter has more calcium, magnesium, manganese, phosphorus, and potassium, while cashew butter has more copper, iron, zinc, and selenium. So, a 5:4 win for almond butter.
In short, these three wins for almond butter add up to one total win for almond butter, unless you have a pressing reason to have different priorities in what you’re looking for in terms of nutrition.
Enjoy both, of course! Unless you are allergic, in which case, please don’t.
Want to learn more?
You might like to read:
Why You Should Diversify Your Nuts
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Does This New Machine Cure Depression?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Let us first talk briefly about the slightly older tech that this may replace, transcranial magnetic stimulation (TMS).
TMS involves electromagnetic fields to stimulate the left half of the brain and inhibit the right half of the brain. It sounds like something from the late 19th century—“cure your melancholy with the mystical power of magnetism”—but the thing is, it works:
The main barriers to its use are that the machine itself is expensive, and it has to be done in a clinic by a trained clinician. Which, if it were treating one’s heart, say, would not be so much of an issue, but when treating depression, there is a problem that depressed people are not the most likely to commit to (and follow through with) going somewhere probably out-of-town regularly to get a treatment, when merely getting out of the door was already a challenge and motivation is thin on the ground to start with.
Thus, antidepressant medications are more often the go-to for cost-effectiveness and adherence. Of course, some will work better than others for different people, and some may not work at all in the case of what is generally called “treatment-resistant depression”:
Antidepressants: Personalization Is Key!
Transcranial stimulation… At home?
Move over transcranial magnetic stimulation; it’s time for transcranial direct-current stimulation (tDCS).
First, what it’s not: electroconvulsive therapy (ECT). Rather, it uses a very low current.
What it is: a small and portable headset (as opposed to the big machine to go sit in for TMS) that one can use at home. Here’s an example product on Amazon, though there are more stylish versions around, this is the same basic technology.
In a recent study, 45% of those who received treatment with this device experienced remission in 10 weeks, significantly beating placebo (bearing in mind that placebo effect is strongest when it comes to invisible ailments such as depression).
See also: How To Leverage Placebo Effect For Yourself ← this explains more about how the placebo effect works, to the extent that it can even be an adjuvant tool to augment “real” therapies
And as for the study, here it is:
…which rather cuts through the “depressed people don’t make it to the clinic consistently, if at all” problem. Of course, it still requires adherence to its use at home, for example three 30-minute sessions per week, but honestly, “lie/sit still” is likely within the abilities of the majority of depressed people. However…
Important note: you remember we said “in 10 weeks”? That may be critical, because shorter studies (e.g. 6 weeks) have previously returned without such glowing results:
Home-Use Transcranial Direct Current Stimulation for the Treatment of a Major Depressive Episode
This means that if you get this tech for yourself or a loved one, it’ll be necessary to persist for likely 10 weeks, certainly more than 6 weeks, and not abandon it after a few sessions when it hasn’t been life-changing yet. And that may be more of a challenge for a depressed person, so likely an “accountability buddy” of some kind is in order (partner, close friend, etc) to help ensure adherence and generally bug you/them into doing it consistently.
And then, of course, you/they might still be in the 55% of people for whom it didn’t work. And that does suck, but random antidepressant medications (i.e., not personalized) don’t fare much better, statistically.
Want something else against depression meanwhile?
Here are some strategies that not only can significantly help, but also are tailored to be actually doable while depressed:
The Mental Health First-Aid You’ll Hopefully Never Need ← written by your writer who has previously suffered extensively from depression and knows what it is like
Take care!
Share This Post
-
Healing Your Gut: Anastasia’s Journey and Tips
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Anastasia Gurova shares her inspiring journey from chronic gut issues to vibrant health.
A Personal Journey to Gut Health
In the below video, Anastasia shares her long struggle with gut problems, including SIBO, IBS, and gastritis. She talks about ending up in the hospital with severe bloating, only to find that a range of medical approaches didn’t provide her with any lasting relief. This led her to explore the importance of the microbiome and its crucial role in gut health, which is what we’ll be focusing on in this overview.
Key Insights and Tips
The most valuable parts of Anastasia’s story for 10almonds readers are, in our opinion, the solutions she discovered to her gut issues. You’ll have to watch her video to discover all of them, but here are some of our favorites:
- Reintroduce Whole Grains and Legumes: Despite the popularity of grain-free diets, Anastasia found significant improvements in her gut health by adding whole grains like quinoa, oats, and buckwheat back into her diet. These foods provide essential fibers that feed beneficial gut bacteria.
- Soaking and Fermenting Foods: To make grains and legumes more digestible, Anastasia recommends soaking them overnight. This is similar to the common technique people use on oats. She also includes fermented foods like sauerkraut, kimchi, and yogurt in her diet, which introduce beneficial bacteria to the gut.
- Resistant Starches: Foods like cooked and cooled rice, potatoes, and green bananas contain resistant starches that promote healthy gut bacteria. Anastasia emphasizes incorporating these into meals to support gut health.
- Mindful Eating: Anastasia found that taking time to chew food thoroughly and savor each bite helped improve her digestion. She avoids distractions like TV while eating and pays attention to the textures and flavors of her meals.
- Avoid Overly Restrictive Diets: Anastasia warns against overly restrictive diets like keto and strict SIBO diets that cut out all carbs and fiber. These can worsen gut health by starving beneficial bacteria.
That’s Only The Beginning
Anastasia’s video goes far beyond what we’ve covered in this short introduction; she provides a detailed look at the steps she took, from dietary changes to lifestyle adjustments, and offers tips that anyone can apply. Plus, she explains the science behind these changes, which, of course, we love.
Enjoy the video! (It would be remiss for us to not bring up our general intro to gut health, or our more specific article on the gut-brain connection)
Good luck on your gut-health journey!
Share This Post
-
We looked at over 166,000 psychiatric records. Over half showed people were admitted against their will
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Picture two people, both suffering from a serious mental illness requiring hospital admission. One was born in Australia, the other in Asia.
Hopefully, both could be treated on a voluntary basis, taking into account their individual needs, preferences and capacity to consent. If not, you might imagine they should be equally likely to receive treatment against their will (known colloquially as being “sectioned” or “scheduled”).
However, our research published in British Journal of Psychiatry Open suggests this is not the case.
In the largest study globally of its kind, we found Australians are more likely to be treated in hospital for their acute mental illness against their will if they are born overseas, speak a language other than English or are unemployed.
What we did and what we found
We examined more than 166,000 episodes of voluntary and involuntary psychiatric care in New South Wales public hospitals between 2016 and 2021. Most admissions (54%) included at least one day of involuntary care.
Being brought to hospital via legal means, such as by police or via a court order, was strongly linked to involuntary treatment.
While our study does not show why this is the case, it may be due to mental health laws. In NSW, which has similar laws to most jurisdictions in Australia, doctors may treat a person on an involuntary basis if they present with certain symptoms indicating serious mental illness (such as hallucinations and delusions) which cause them to require protection from serious harm, and there is no other less-restrictive care available. Someone who has been brought to hospital by police or the courts may be more likely to meet the legal requirement of requiring protection from serious harm.
The likelihood of involuntary care was also linked to someone’s diagnosis. A person with psychosis or organic brain diseases, such as dementia and delirium, were about four times as likely to be admitted involuntarily compared to someone with anxiety or adjustment disorders (conditions involving a severe reaction to stressors).
However, our data suggest non-clinical factors contribute to the decision to impose involuntary care.
Compared with people born in Australia, we found people born in Asia were 42% more likely to be treated involuntarily.
People born in Africa or the Middle East were 32% more likely to be treated this way.
Overall, people who spoke a language other than English were 11% more likely to receive involuntary treatment compared to those who spoke English as their first language.
Some international researchers have suggested higher rates of involuntary treatment seen in people born overseas might be due to higher rates of psychotic illness. But our research found a link between higher rates of involuntary care in people born overseas or who don’t speak English regardless of their diagnosis.
We don’t know why this is happening. It is likely to reflect a complex interplay of factors about both the people receiving treatment and the way services are provided to them.
People less likely to be treated involuntarily included those who hold private health insurance, and those referred through a community health centre or outpatients unit.
Our findings are in line with international studies. These show higher rates of involuntary treatment among people from Black and ethnic minority groups, and people living in areas of higher socioeconomic disadvantage.
A last resort? Or should we ban it?
Both the NSW and Australian mental health commissions have called involuntary psychiatric care an avoidable harm that should only be used as a last resort.
Despite this, one study found Australia’s rate of involuntary admissions has increased by 3.4% per year and it has one of the highest rates of involuntary admissions in the world.
Involuntary psychiatric treatment is also under increasing scrutiny globally.
When Australia signed up to the UN Convention on the Rights of Persons with Disabilities, it added a declaration noting it would allow for involuntary treatment of people with mental illness where such treatments are “necessary, as a last resort and subject to safeguards”.
However, the UN has rejected this, saying it is a fundamental human right “to be free from involuntary detention in a mental health facility and not to be forced to undergo mental health treatment”.
Others question if involuntary treatment could ever be removed entirely.
Where to from here?
Our research not only highlights concerns regarding how involuntary psychiatric treatment is implemented, it’s a first step towards decreasing its use. Without understanding how and when it is used it will be difficult to create effective interventions to reduce it.
But Australia is still a long way from significantly reducing involuntary treatment.
We need to provide more care options outside hospital, ones accessible to all Australians, including those born overseas, who don’t speak English, or who come from disadvantaged communities. This includes intervening early enough that people are supported to not become so unwell they end up being referred for treatment via police or the criminal justice system.
More broadly, we need to do more to reduce stigma surrounding mental illness and to ensure poverty and discrimination are tackled to help prevent more people becoming unwell in the first place.
Our study also shows we need to do more to respect the autonomy of someone with serious mental illness to choose if they are treated. That’s whether they are in NSW or other jurisdictions.
And legal reform is required to ensure more states and territories more fully reflect the principal that people who have the capacity to make such decisions should have the right to decline mental health treatment in the same way they would any other health care.
If this article has raised issues for you, or if you’re concerned about someone you know, call Lifeline on 13 11 14.
Amy Corderoy, Medical doctor and PhD candidate studying involuntary psychiatric treatment, School of Psychiatry, UNSW Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
What’s the difference between wholemeal and wholegrain bread? Not a whole lot
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
If you head to the shops to buy bread, you’ll face a variety of different options.
But it can be hard to work out the difference between all the types on sale.
For instance, you might have a vague idea that wholemeal or wholegrain bread is healthy. But what’s the difference?
Here’s what we know and what this means for shoppers in Australia and New Zealand.
Phish Photography/Shutterstock Let’s start with wholemeal bread
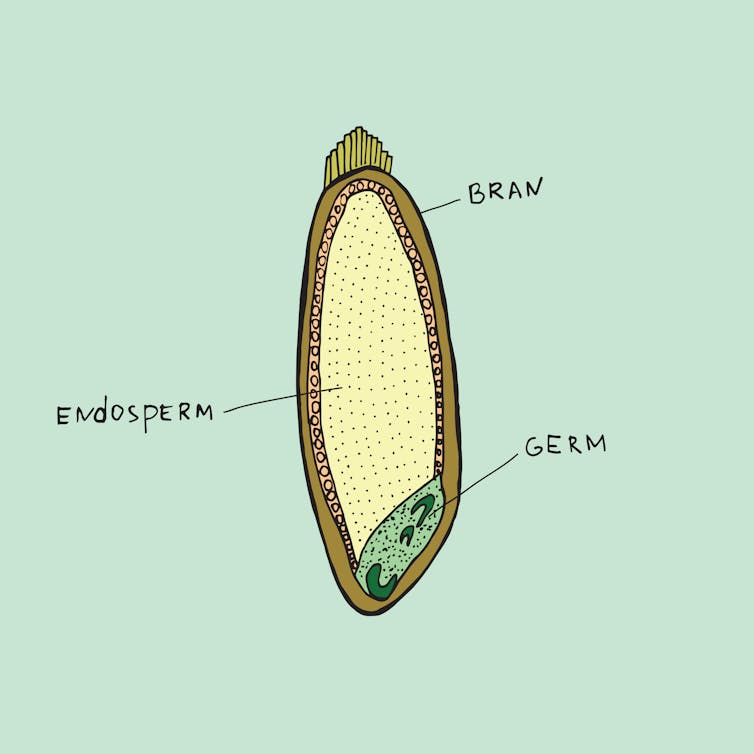
According to Australian and New Zealand food standards, wholemeal bread is made from flour containing all parts of the original grain (endosperm, germ and bran) in their original proportions.
Because it contains all parts of the grain, wholemeal bread is typically darker in colour and slightly more brown than white bread, which is made using only the endosperm.
Wholemeal flour is made from all parts of the grain. Rerikh/Shutterstock How about wholegrain bread?
Australian and New Zealand food standards define wholegrain bread as something that contains either the intact grain (for instance, visible grains) or is made from processed grains (flour) where all the parts of the grain are present in their original proportions.
That last part may sound familiar. That’s because wholegrain is an umbrella term that encompasses both bread made with intact grains and bread made with wholemeal flour. In other words, wholemeal bread is a type of wholegrain bread, just like an apple is a type of fruit.
Don’t be confused by labels such as “with added grains”, “grainy” or “multigrain”. Australian and New Zealand food standards don’t define these so manufacturers can legally add a small amount of intact grains to white bread to make the product appear healthier. This doesn’t necessarily make these products wholegrain breads.
So unless a product is specifically called wholegrain bread, wholemeal bread or indicates it “contains whole grain”, it is likely to be made from more refined ingredients.
Which one’s healthier?
So when thinking about which bread to choose, both wholemeal and wholegrain breads are rich in beneficial compounds including nutrients and fibre, more so than breads made from further-refined flour, such as white bread.
The presence of these compounds is what makes eating wholegrains (including wholemeal bread) beneficial for our overall health. Research has also shown eating wholegrains helps reduce the risk of common chronic diseases, such as heart disease.
The table below gives us a closer look at the nutritional composition of these breads, and shows some slight differences.
Wholegrain bread is slightly higher in fibre, protein, niacin (vitamin B3), iron, zinc, phosphorus and magnesium than wholemeal bread. But wholegrain bread is lower in carbohydrates, thiamin (vitamin B1) and folate (vitamin B9).
However the differences are relatively small when considering how these contribute to your overall dietary intake.
Which one should I buy?
Next time you’re shopping, look for a wholegrain bread (one made from wholemeal flour that has intact grains and seeds throughout) as your number one choice for fibre and protein, and to support overall health.
If you can’t find wholegrain bread, wholemeal bread comes in a very close second.
Wholegrain and wholemeal bread tend to cost the same, but both tend to be more expensive than white bread.
Margaret Murray, Senior Lecturer, Nutrition, Swinburne University of Technology
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Stop Cancer 20 Years Ago
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Get Abreast And Keep Abreast
This is Dr. Jenn Simmons. Her specialization is integrative oncology, as she—then a breast cancer surgeon—got breast cancer, decided the system wasn’t nearly as good from the patients’ side of things as from the doctors’ side, and took to educate herself, and now others, on how things can be better.
What does she want us to know?
Start now
If you have breast cancer, the best time to start adjusting your lifestyle might be 20 years ago, but the second-best time is now. We realize our readers with breast cancer (or a history thereof) probably have indeed started already—all strength to you.
What this means for those of us without breast cancer (or a history therof) is: start now
Even if you don’t have a genetic risk factor, even if there’s no history of it in your family, there’s just no reason not to start now.
Start what, you ask? Taking away its roots. And how?
Inflammation as the root of cancer
To oversimplify: cancer occurs because an accidentally immortal cell replicates and replicates and replicates and takes any nearby resources to keep on going. While science doesn’t know all the details of how this happens, it is a factor of genetic mutation (itself a normal process, without which evolution would be impossible), something which in turn is accelerated by damage to the DNA. The damage to the DNA? That occurs (often as not) as a result of cellular oxidation. Cellular oxidation is far from the only genotoxic thing out there, and a lot of non-food “this thing causes cancer” warnings are usually about other kinds of genotoxicity. But cellular oxidation is a big one, and it’s one that we can fight vigorously with our lifestyle.
Because cellular oxidation and inflammation go hand-in-hand, reducing one tends to reduce the other. That’s why so often you’ll see in our Research Review Monday features, a line that goes something like:
“and now for those things that usually come together: antioxidant, anti-inflammatory, anticancer, and anti-aging”
So, fight inflammation now, and have a reduced risk of a lot of other woes later.
See: How to Prevent (or Reduce) Inflammation
Don’t settle for “normal”
People are told, correctly but not always helpfully, such things as:
- It’s normal to have less energy at your age
- It’s normal to have a weaker immune system at your age
- It’s normal to be at a higher risk of diabetes, heart disease, etc
…and many more. And these things are true! But that doesn’t mean we have to settle for them.
We can be all the way over on the healthy end of the distribution curve. We can do that!
(so can everyone else, given sufficient opportunity and resources, because health is not a zero-sum game)
If we’re going to get a cancer diagnosis, then our 60s are the decade where we’re most likely to get it. Earlier than that and the risk is extant but lower; later than that and technically the risk increases, but we probably got it already in our 60s.
So, if we be younger than 60, then now’s a good time to prepare to hit the ground running when we get there. And if we missed that chance, then again, the second-best time is now:
See: Focusing On Health In Our Sixties
Fast to live
Of course, anything can happen to anyone at any age (alas), but this is about the benefits of living a fasting lifestyle—that is to say, not just fasting for a 4-week health kick or something, but making it one’s “new normal” and just continuing it for life.
This doesn’t mean “never eat”, of course, but it does mean “practice intermittent fasting, if you can”—something that Dr. Simmons strongly advocates.
See: Intermittent Fasting: We Sort The Science From The Hype
While this calls back to the previous “fight inflammation”, it deserves its own mention here as a very specific way of fighting it.
It’s never too late
All of the advices that go before a cancer diagnosis, continue to stand afterwards too. There is no point of “well, I already have cancer, so what’s the harm in…?”
The harm in it after a diagnosis will be the same as the harm before. When it comes to lifestyle, preventing a cancer and preventing it from spreading are very much the same thing, which is also the same as shrinking it. Basically, if it’s anticancer, it’s anticancer, no matter whether it’s before, during, or after.
Dr. Simmons has seen too many patients get a diagnosis, and place their lives squarely in the hands of doctors, when doctors can only do so much.
Instead, Dr. Simmons recommends taking charge of your health as best you are able, today and onwards, no matter what. And that means two things:
- Knowing stuff
- Doing stuff
So it becomes our responsibility (and our lifeline) to educate ourselves, and take action accordingly.
Want to know more?
We recently reviewed her book, and heartily recommend it:
The Smart Woman’s Guide to Breast Cancer – by Dr. Jenn Simmons
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Sweet Dreams Are Made Of Cheese (Or Are They?)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? You can always hit “reply” to any of our emails, or use the feedback widget at the bottom!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝In order to lose a little weight I have cut out cheese from my diet – and am finding that I am sleeping better. Would be interested in your views on cheese and sleep, and whether some types of cheese are worse for sleep than others. I don’t want to give up cheese entirely!❞
In principle, there’s nothing in cheese that, biochemically, should impair sleep. If anything, its tryptophan content could aid good sleep.
Tryptophan is found in many foods, including cheese, which (of common foods, anyway), for example cheddar cheese ranks second only to pumpkin seeds in tryptophan content.
Tryptophan can be converted by the body into 5-HTP, which you’ve maybe seen sold as a supplement. Its full name is 5-hydroxytryptophan.
5-HTP can, in turn, be used to make melatonin and/or serotonin. Which of those you will get more of, depends on what your body is being cued to do by ambient light/darkness, and other environmental cues.
If you are having cheese and then checking your phone, for instance, or otherwise hanging out where there are white/blue lights, then your body may dutifully convert the tryptophan into serotonin (calm wakefulness) instead of melatonin (drowsiness and sleep).
In short: the cheese will (in terms of this biochemical pathway, anyway) augment some sleep-inducing or wakefulness-inducing cues, depending on which are available.
You may be wondering: what about casein?
Casein is oft-touted as producing deep sleep, or disturbed sleep, or vivid dreams, or bad dreams. There’s no science to back any of this up, though the following research review is fascinating:
Dreams of the Rarebit Fiend: food and diet as instigators of bizarre and disturbing dreams
(it largely supports the null hypothesis of “not a causal factor” but does look at the many more likely alternative explanations, ranging from associated actually casual factors (such as alcohol and caffeine) and placebo/nocebo effect)
Finally, simple digestive issues may be the real thing at hand:
Worth noting that around two thirds of all people, including those who regularly enjoy dairy products, have some degree of lactose intolerance:
Lactose Intolerance in Adults: Biological Mechanism and Dietary Management
So, in terms of what cheese may be better/worse for you in this context, you might try experimenting with lactose-free cheese, which will help you identify whether that was the issue!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: