Superfood Kale & Dill Pâté
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Most of us could do with eating more greens a lot of the time, but it’s not always easy to include them. This kale and dill pâté brings a healthy dose of green in luxurious style, along with abundant phytochemicals and more!
You will need
- 2 handfuls kale, stalks removed
- 1 cup soft cheese (you can use our Healthy Plant-Based Cream Cheese recipe if you like)
- 2 tbsp fresh dill, chopped
- 1 tsp capers
- 1 tsp black pepper, coarse ground
- ½ tsp MSG, or 1 tsp low-sodium salt
Method
(we suggest you read everything at least once before doing anything)
1) Steam the kale for about 5 minutes or until wilted and soft. Run under cold water to halt the cooking process.
2) Combine all the ingredients, including the kale you just blanched, in a food processor and blitz to make a smooth pâté.
3) Serve with oatcakes or vegetable sticks, or keep in the fridge to enjoy it later:

Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How To Beat Loneliness & Isolation
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Overcoming Loneliness & Isolation
One of the biggest mental health threats that faces many of us as we get older is growing isolation, and the loneliness that can come with it. Family and friends thin out over the years, and getting out and about isn’t always as easy as it used to be for everyone.
Nor is youth a guaranteed protection against this—in today’s world of urban sprawl and nothing-is-walkable cities, in which access to social spaces such as cafés and the like means paying the rising costs with money that young people often don’t have… And that’s without getting started on how much the pandemic impacted an entire generation’s social environments (or lack thereof).
Why is this a problem?
Humans are, by evolution, social creatures. As individuals we may have something of a spectrum from introvert to extrovert, but as a species, we thrive in community. And we suffer, when we don’t have that.
What can we do about it?
We can start by recognizing our needs, such as they are, and identifying to what extent they are being met (or not).
- Some of us may be very comfortable with a lot of alone time—but need someone to talk to sometimes.
- Some of us may need near-constant company to feel at our best—and that’s fine too! We just need to plan accordingly.
In the former case, it’s important to remember that needing someone to talk to is not being a burden to them. Not only will our company probably enrich them too, but also, we are evolved to care for one another, and that itself can bring fulfilment to them as much as to you. But what if you don’t a friend to talk to?
- You might be surprised at who would be glad of you reaching out. Have a think through whom you know, and give it a go. This can be scary, because what if they reject us, or worse, they don’t reject us but silently resent us instead? Again, they probably won’t. Human connection requires taking risks and being vulnerable sometimes.
- If that’s not an option, there are services that can fill your need. For some, therapy might serve a dual purpose in this regard. For others, you might want to check out the list of (mostly free) resources at the bottom of this article
In the second case (that we need near-constant company to feel at our best) we probably need to look more at our overall lifestyle, and find ways to be part of a community. That can include:
- Living in a close-knit community (places with a lot of retirees in one place often have this; or younger folk might look at communal living/working spaces, for example)
- Getting involved in local groups (you can check out NextDoor.com or MeetUp.com for this)
- Volunteering for a charity (not only are acts of service generally fulfilling in and of themselves, but also, you will probably be working with other people of a charitable nature, and such people tend to make for good company!)
Need a little help?
There are many, many organizations that will love to help you (or anyone else) overcome loneliness and isolation.
Rather than list them all here and make this email very long by describing how each of them works, here’s a great compilation of resources:
Share This Post
-
Fatigue? Unexplained weight gain and dry skin? Could it be Hashimoto’s disease?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Maybe you feel worn out. Perhaps you’re also having trouble losing weight. Generally, you just don’t feel 100%.
Could it be Hashimoto’s disease? This common autoimmune thyroid disorder is when your immune system (which fights off viruses and bacteria), mistakenly attacks a part of your body. In this case, it’s your thyroid – a gland located at the base of your neck – and can cause low thyroid hormones levels (hypothyroidism).
Hypothyroidism affects one in 33 Australians and Hashimoto’s is one of the most common thyroid conditions in first-world countries.
While symptoms can be subtle, untreated Hashimoto’s can cause long-term problems with your heart, memory and fertility. Here is what you need to know.
What happens when you have Hashimoto’s?
Your thyroid gland is a butterfly-shaped gland in the neck. It is essential in regulating things like muscle function, digestion, metabolism, the heart and lungs. In children, thyroid hormones are also needed for normal growth and development.
Hashimoto’s thyroid disease, named after the Japanese doctor who discovered it in 1912, is also known as Hashimoto’s thyroiditis or chronic lymphocytic thyroiditis. The disease can cause the immune system to mistakenly produce proteins called antibodies (thyroid peroxidase and thyroglobulin). These can cause inflammation and long-term damage to the thyroid gland. Over time, as thyroid tissue is inflamed and/or destroyed, there can be a decrease in the production of thyroid hormones (hypothyroidism).
Hashimoto’s can present subtly at first. If you only have antibodies with no change in thyroid levels, it is likely you won’t have any symptoms.
However, as the disease progresses, you may experience fatigue, weight gain (or difficulty losing weight), increased sensitivity to the cold, constipation, dry skin, muscle aches, irregular or heavy menstrual cycles, enlarged thyroid (goitre) and occasionally hair loss, including at the ends of your eyebrows.
What causes Hashimoto’s thyroid disease?
Several risk factors can contribute to the development of Hashimoto’s including:
-
genetic risk – your risk is higher if you have family members with Hashimoto’s
-
gender – women are up to ten times more likely than men to develop the disease
-
age – you are more likely to develop the disease from 30 to 50 years of age
-
autoimmune condition – having another autoimmune condition like systemic lupus, Type 1 diabetes and celiac disease increases your risk
-
excessive iodine intake and radiation exposure may also increase risk in people who are already genetically at greater risk.
What are the long-term risks?
Long-term, untreated Hashimoto’s thyroiditis can cause heart issues, higher cholesterol levels, nerve damage (peripheral neuropathy), reduced cognition and infertility.
In pregnancy, Hashimoto’s has a higher risk of pre-eclampsia (high blood pressure affecting several organs), premature birth, placental abruption (when the placenta separates from the inner wall of the uterus before birth) and, in severe cases, pregnancy loss.
The disease has also been linked with an increased risk (but low incidence) of the lymphocytes of the thyroid turning into cancer cells to cause thyroid lymphoma.
How is Hashimoto’s diagnosed?
Diagnosis can be confirmed with a blood test to check thyroid levels and antibodies.
Thyroid peroxidase antibodies are commonly present but about 5% of patients test antibody-negative. In those people, diagnosis depends on the thyroid levels, clinical presentation and ultrasound appearance of general inflammation. An ultrasound may not be required though, especially if the diagnosis is obvious.
Three hormone levels are tested to determine if you have Hashimoto’s.
Thyroid stimulating hormone (TSH) is produced by the brain to speak to the thyroid, telling it to produce two types of thyroid hormones – T3 and T4.
If you have either relative or absolute thyroid hormone deficiency, a test will show the stimulating hormones as high because the brain is trying to get the thyroid to work harder.
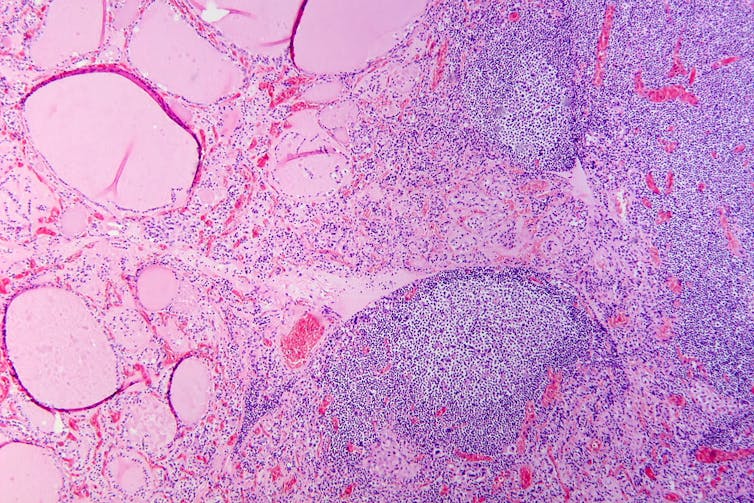
Hashimoto’s thyroiditis under the microscope. Antibodies against thyroid peroxidase and thyroglobulin were elevated.
Patho/Wikimedia Commons, CC BY-SACan it be treated?
The management of Hashimoto’s depends on the severity of the thyroid levels. Up to 20% of the population can have antibodies but normal thyroid levels. This is still Hashimoto’s thyroid disease, but it is very mild and does not require treatment. There is no current treatment to reduce antibody levels alone.
Because thyroid peroxidase antibodies increase the risk of abnormal thyroid levels in the future, regular thyroid testing is recommended.
When the thyroid stimulating hormone is high with normal thyroid hormone levels it is termed “subclinical hypothyroidism”. When it is paired with low hormone levels it is called “overt hypothyroidism”. The first is a mild form of the disease and treatment depends on the degree of stimulating hormone elevation.
Overt hypothyroidism warrants treatment. The main form of this is thyroid hormone replacement therapy (levothyroxine) with the dose of the drug adjusted until thyroid levels are within the normal range. This is usually a lifelong treatment but, once the dose is optimised, hormone levels usually remain relatively stable.
In some people with very enlarged thyroid glands causing compressive symptoms (such as difficulty swallowing or breathing), thyroidectomy (surgical removal of the thyroid) is considered.
Hashimoto’s thyroiditis is a common condition caused by your body’s immune system incorrectly damaging to your thyroid and can go undetected. Long-term, untreated, it can cause issues with your heart, cognition, and fertility. It can be diagnosed with a simple blood test. Speak to your doctor if you have any concerns as early diagnosis and treatment can help prevent complications.
Aakansha Zala, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
-
Less Common Oral Hygiene Options
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Less Common Alternatives For Oral Hygiene!
You almost certainly brush your teeth. You might use mouthwash. A lot of people floss for three weeks at a time, often in January.
There are a lot of options for oral hygiene; variations of the above, and many alternatives too. This is a big topic, so rather than try to squeeze it all in one, this will be a several-part series.
- The first part was: Toothpastes & Mouthwashes: Which Help And Which Harm?
- The second part was: Flossing, Better (And Easier!)
- The third (and for now at least, final) part will look at some less common alternatives.
Tooth soap
The idea here is simplicity, and brushing with as few ingredients as possible. Soap cleans your teeth the same way it cleans your (sometimes compositionally quite similar—enamel and all) dishes, without damaging them.
We’d love to link to some science here, but alas, it appears to have not yet been done—at least, we couldn’t find any!
You can make your own tooth soap if you are feeling confident, or you might prefer to buy one ready-made (here’s an example product on Amazon, with various flavor options)
Oil pulling
We are getting gradually more scientific now; there is science for this one… But the (scientific) reviews are mixed:
Wooley et al., 2020, conducted a review of extant studies, and concluded:
❝The limited evidence suggests that oil pulling with coconut oil may have a beneficial effect on improving oral health and dental hygiene❞
The “Science-Based Medicine” project was less positive in its assessment, and declared that all and any studies that found oil pulling to be effective were a matter of researcher/publication bias. We would note that SBM is a private project and is not without its own biases, but for balance, here is what they had to offer:
A more rounded view seems to be that it is a good method for cleaning your teeth if you don’t have better options available (whereby, “better options” is “almost any other method”).
One final consideration, which the above seemed not to consider, is:
If you have sensitive teeth/gums, oil-pulling is the gentlest way of cleaning them, and getting them back into sufficient order that you can comfortably use other methods.
Want to try it? You can use any food-grade oil (coconut oil or olive oil are common choices).
Chewing stick
Not just any stick—a twig of the Salvadora persica tree. This time, there’s lots of science for it, and it’s uncontroversially effective:
❝A number of scientific studies have demonstrated that the miswak (Salvadora persica) possesses antibacterial, anti-fungal, anti-viral, anti-cariogenic, and anti-plaque properties.
Several studies have also claimed that miswak has anti-oxidant, analgesic, and anti-inflammatory effects. The use of a miswak has an immediate effect on the composition of saliva.
Several clinical studies have confirmed that the mechanical and chemical cleansing efficacy of miswak chewing sticks are equal and at times greater than that of the toothbrush❞
Read in full: A review of the therapeutic effects of using miswak (Salvadora Persica) on oral health
And about the efficacy vs using a toothbrush, here’s an example:
Comparative effect of chewing sticks and toothbrushing on plaque removal and gingival health
Want to try the miswak stick? Here’s an example product on Amazon.
Enjoy!
Share This Post
Related Posts
-
How to Change – by Katy Milkman
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sometimes it seems that we know everything we should be doing… We have systems and goals and principles, we know about the importance of habits, and we do our best to live them. Yet, somehow, life has other plans for us and things don’t quite come together they way they did in our genius masterplan.
So, what happened? And more importantly, what are we supposed to do about this? Katy Milkman has answers, right from the start.
Sometimes, it can be as simple as when we try to implement a change. It’s not that there’s a “wrong time” for a good change, so much that there are times that are much more likely to succeed than others… and those times can be identified and used.
Sometimes we’re falling prey to vices—which she explains how to overcome—such as:
- Impulsivity
- Procrastination
- Forgetfulness
- Laziness
We also learn some counterintuitive truths about what can boost or sabotage our confidence along the way!
Milkman writes in a compelling, almost narrative style, that makes for very easy reading. The key ideas, built up to by little (ostensibly true) stories and then revealed, become both clear and memorable. Most importantly, applicable.
Bottom line: this is a great troubleshooting guide for when you know how everything should be working, but somehow, it just doesn’t—and you’d like to fix that.
Click here to check out “How To Change” on Amazon, and get those changes rolling!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
In This Oklahoma Town, Most Everyone Knows Someone Who’s Been Sued by the Hospital
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
McALESTER, Okla. — It took little more than an hour for Deborah Hackler to dispense with the tall stack of debt collection lawsuits that McAlester Regional Medical Center recently brought to small-claims court in this Oklahoma farm community.
Hackler, a lawyer who sues patients on behalf of the hospital, buzzed through 51 cases, all but a handful uncontested, as is often the case. She bantered with the judge as she secured nearly $40,000 in judgments, plus 10% in fees for herself, according to court records.
It’s a payday the hospital and Hackler have shared frequently over the past three decades, records show. The records indicate McAlester Regional Medical Center and an affiliated clinic have filed close to 5,000 debt collection cases since the early 1990s, most often represented by the father-daughter law firm of Hackler & Hackler.
Some of McAlester’s 18,000 residents have been taken to court multiple times. A deputy at the county jail and her adult son were each sued recently, court records show. New mothers said they compare stories of their legal run-ins with the medical center.
“There’s a lot that’s not right,” Sherry McKee, a dorm monitor at a tribal boarding school outside McAlester, said on the courthouse steps after the hearing. The hospital has sued her three times, most recently over a $3,375 bill for what she said turned out to be vertigo.
In recent years, major health systems in Virginia, North Carolina, and elsewhere have stopped suing patients following news reports about lawsuits. And several states, such as Maryland and New York, have restricted the legal actions hospitals can take against patients.
But with some 100 million people in the U.S. burdened by health care debt, medical collection cases still clog courtrooms across the country, researchers have found. In places like McAlester, a hospital’s debt collection machine can hum away quietly for years, helped along by powerful people in town. An effort to limit hospital lawsuits failed in the Oklahoma Legislature in 2021.
In McAlester, the lawsuits have provided business for some, such as the Adjustment Bureau, a local collection agency run out of a squat concrete building down the street from the courthouse, and for Hackler, a former president of the McAlester Area Chamber of Commerce. But for many patients and their families, the lawsuits can take a devastating toll, sapping wages, emptying retirement accounts, and upending lives.
McKee said she wasn’t sure how long it would take to pay off the recent judgment. Her $3,375 debt exceeds her monthly salary, she said.
“This affects a large number of people in a small community,” said Janet Roloff, an attorney who has spent years assisting low-income clients with legal issues such as evictions in and around McAlester. “The impact is great.”
Settled more than a century ago by fortune seekers who secured land from the Choctaw Nation to mine coal in the nearby hills, McAlester was once a boom town. Vestiges of that era remain, including a mammoth, 140-foot-tall Masonic temple that looms over the city.
Recent times have been tougher for McAlester, now home by one count to 12 marijuana dispensaries and the state’s death row. The downtown is pockmarked by empty storefronts, including the OKLA theater, which has been dark for decades. Nearly 1 in 5 residents in McAlester and the surrounding county live below the federal poverty line.
The hospital, operated by a public trust under the city’s authority, faces its own struggles. Paint is peeling off the front portico, and weeds poke up through the parking lots. The hospital has operated in the red for years, according to independent audit reports available on the state auditor’s website.
“I’m trying to find ways to get the entire community better care and more care,” said Shawn Howard, the hospital’s chief executive. Howard grew up in McAlester and proudly noted he started his career as a receptionist in the hospital’s physical therapy department. “This is my hometown,” he said. “I am not trying to keep people out of getting care.”
The hospital operates a clinic for low-income patients, whose webpage notes it has “limited appointments” at no cost for patients who are approved for aid. But data from the audits shows the hospital offers very little financial assistance, despite its purported mission to serve the community.
In the 2022 fiscal year, it provided just $114,000 in charity care, out of a total operating budget of more than $100 million, hospital records show. Charity care totaling $2 million or $3 million out of a $100 million budget would be more in line with other U.S. hospitals.
While audits show few McAlester patients get financial aid, many get taken to court.
Renee Montgomery, the city treasurer in an adjoining town and mother of a local police officer, said she dipped into savings she’d reserved for her children and grandchildren after the hospital sued her last year for more than $5,500. She’d gone to the emergency room for chest pain.
Dusty Powell, a truck driver, said he lost his pickup and motorcycle when his wages were garnished after the hospital sued him for almost $9,000. He’d gone to the emergency department for what turned out to be gastritis and didn’t have insurance, he said.
“Everyone in this town probably has a story about McAlester Regional,” said another former patient who spoke on the condition she not be named, fearful to publicly criticize the hospital in such a small city. “It’s not even a secret.”
The woman, who works at an Army munitions plant outside town, was sued twice over bills she incurred giving birth. Her sister-in-law has been sued as well.
“It’s a good-old-boy system,” said the woman, who lowered her voice when the mayor walked into the coffee shop where she was meeting with KFF Health News. Now, she said, she avoids the hospital if her children need care.
Nationwide, most people sued in debt collection cases never challenge them, a response experts say reflects widespread misunderstanding of the legal process and anxiety about coming to court.
At the center of the McAlester hospital’s collection efforts for decades has been Hackler & Hackler.
Donald Hackler was city attorney in McAlester for 13 years in the ’70s and ’80s and a longtime member of the local Lions Club and the Scottish Rite Freemasons.
Daughter Deborah Hackler, who joined the family firm 30 years ago, has been a deacon at the First Presbyterian Church of McAlester and served on the board of the local Girl Scouts chapter, according to the McAlester News-Capital newspaper, which named her “Woman of the Year” in 2007. Since 2001, she also has been a municipal judge in McAlester, hearing traffic cases, including some involving people she has sued on behalf of the hospital, municipal and county court records show.
For years, the Hacklers’ debt collection cases were often heard by Judge James Bland, who has retired from the bench and now sits on the hospital board. Bland didn’t respond to an inquiry for interview.
Hackler declined to speak with KFF Health News after her recent court appearance. “I’m not going to visit with you about a current client,” she said before leaving the courthouse.
Howard, the hospital CEO, said he couldn’t discuss the lawsuits either. He said he didn’t know the hospital took its patients to court. “I had to call and ask if we sue people,” he said.
Howard also said he didn’t know Deborah Hackler. “I never heard her name before,” he said.
Despite repeated public records requests from KFF Health News since September, the hospital did not provide detailed information about its financial arrangement with Hackler.
McAlester Mayor John Browne, who appoints the hospital’s board of trustees, said he, too, didn’t know about the lawsuits. “I hadn’t heard anything about them suing,” he said.
At the century-old courthouse in downtown McAlester, it’s not hard to find the lawsuits, though. Every month or two, another batch fills the docket in the small-claims court, now presided over by Judge Brian McLaughlin.
After court recently, McLaughlin, who is not from McAlester, shook his head at the stream of cases and patients who almost never show up to defend themselves, leaving him to issue judgment after judgment in the hospital’s favor.
“All I can do is follow the law,” said McLaughlin. “It doesn’t mean I like it.”
About This Project
“Diagnosis: Debt” is a reporting partnership between KFF Health News and NPR exploring the scale, impact, and causes of medical debt in America.
The series draws on original polling by KFF, court records, federal data on hospital finances, contracts obtained through public records requests, data on international health systems, and a yearlong investigation into the financial assistance and collection policies of more than 500 hospitals across the country.
Additional research was conducted by the Urban Institute, which analyzed credit bureau and other demographic data on poverty, race, and health status for KFF Health News to explore where medical debt is concentrated in the U.S. and what factors are associated with high debt levels.
The JPMorgan Chase Institute analyzed records from a sampling of Chase credit card holders to look at how customers’ balances may be affected by major medical expenses. And the CED Project, a Denver nonprofit, worked with KFF Health News on a survey of its clients to explore links between medical debt and housing instability.
KFF Health News journalists worked with KFF public opinion researchers to design and analyze the “KFF Health Care Debt Survey.” The survey was conducted Feb. 25 through March 20, 2022, online and via telephone, in English and Spanish, among a nationally representative sample of 2,375 U.S. adults, including 1,292 adults with current health care debt and 382 adults who had health care debt in the past five years. The margin of sampling error is plus or minus 3 percentage points for the full sample and 3 percentage points for those with current debt. For results based on subgroups, the margin of sampling error may be higher.
Reporters from KFF Health News and NPR also conducted hundreds of interviews with patients across the country; spoke with physicians, health industry leaders, consumer advocates, debt lawyers, and researchers; and reviewed scores of studies and surveys about medical debt.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
For women with antenatal depression, micronutrients might help them and their babies – new study
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Getty Images Julia J Rucklidge, University of Canterbury; Elena Moltchanova, University of Canterbury; Roger Mulder, University of Otago, and Siobhan A Campbell, University of Canterbury
Antenatal depression affects 15% to 21% of pregnant women worldwide. It can influence birth outcomes and children’s development, as well as increase the risk of post-natal depression.
Current treatments like therapy can be inaccessible and antidepressants can carry risks for developing infants.
Over the past two decades, research has highlighted that poor nutrition is a contributing risk factor to mental health challenges. Most pregnant women in New Zealand aren’t adhering to nutritional guidelines, according to a longitudinal study. Only 3% met the recommendations for all food groups.
Another cohort study carried out in Brazil shows that ultra-processed foods (UPF) accounted for at least 30% of daily dietary energy during pregnancy, displacing healthier options.
UPFs are chemically manufactured and contain additives to improve shelf life, as well as added sugar and salt. Importantly, they are low in essential micronutrients (vitamins and minerals).
The consumption of these foods is concerning because a nutrient-poor diet during pregnancy has been linked to poorer mental health outcomes in children. This includes depression, anxiety, hyperactivity, and inattention.
Increasing nutrients in maternal diets and reducing consumption of UPFs could improve the mental health of the mother and the next generation. Good nutrition can have lifelong benefits for the offspring.
However, there are multiple factors that mean diet change alone may not in itself be sufficient to address mental health challenges. Supplementing with additional nutrients may also be important to address nutritional needs during pregnancy.
Micronutrients as treatment for depression
Our earlier research suggests micronutrient supplements for depression have benefits outside pregnancy.
But until now there have been no published randomised controlled trials specifically designed to assess the efficacy and safety of broad-spectrum micronutrients on antenatal depression and overall functioning.
The NUTRIMUM trial, which ran between 2017 and 2022, recruited 88 women in their second trimester of pregnancy who reported moderate depressive symptoms. They were randomly allocated to receive either 12 capsules (four pills, three times a day) of a broad-spectrum micronutrient supplement or an active placebo containing iodine and riboflavin for a 12-week period.
Micronutrient doses were generally between the recommended dietary allowance and the tolerable upper level.
Based on clinician ratings, micronutrients significantly improved overall psychological functioning compared to the placebo. The findings took into account all noted changes based on self-assessment and clinician observations. This includes sleep, mood regulation, coping, anxiety and side effects.
Adding micronutrients to the diet of pregnant women with antenatal depression significantly improved their overall psychological functioning. Getty Images Both groups reported similar reductions in symptoms of depression. More than three quarters of participants were in remission at the end of the trial. But 69% of participants in the micronutrient group rated themselves as “much” or “very much” improved, compared to 39% in the placebo group.
Participants taking the micronutrients also experienced significantly greater improvements in sleep and overall day-to-day functioning, compared to participants taking the placebo. There were no group differences on measures of stress, anxiety and quality of life.
Importantly, there were no group differences in reported side effects, and reports of suicidal thoughts dropped over the course of the study for both groups. Blood tests confirmed increased vitamin levels (vitamin C, D, B12) and fewer deficiencies in the micronutrient group.
Micronutrients were particularly helpful for women with chronic mental health challenges and those who had taken psychiatric medications in the past. Those with milder symptoms improved with or without the micronutrients, suggesting general care and monitoring might suffice for some women.
The benefits of micronutrients were comparable to psychotherapy but with less contact. There are no randomised controlled trials of antidepressant medication to compare these results.
Retention in the study was good (81%) and compliance excellent (90%).
Beyond maternal mental health
We followed the infants of mothers enrolled in the NUTRIMUM trial (who were therefore exposed to micronutrients during pregnancy) for 12 months, alongside infants from the general population of Aotearoa New Zealand.
This second group of infants from the general population contained a smaller sub-group who were exposed to antidepressant medication for the treatment of antenatal depression.
We assessed the neuro-behavioural development of each infant within the first four weeks of life, and temperament up to one year after birth.
These observational follow-ups showed positive effects of micronutrients on the infants’ ability to regulate their behaviour. These results were on par with or better than typical pregnancies, and better than treatments with antidepressants.
Micronutrients during pregnancy improved the neurological and behavioural development of infants. Getty Images Infants exposed to micronutrients during pregnancy were significantly better at attending to external stimuli. They were also better able to block out external stimuli during sleep. They showed fewer signs of stress and had better muscle tone compared to infants not exposed to micronutrients.
They also displayed greater ability to interact with their environment. They were better at regulating their emotional state and had fewer abnormal muscle reflexes than infants exposed to antidepressant medication in pregnancy.
Reassuringly, micronutrients had no negative impact on infant temperament.
These findings highlight the potential of micronutrients as a safe and effective alternative to traditional medication treatments for antenatal depression.
The prenatal environment sets the foundation for a child’s future. Further investigation into the benefits of micronutrient supplementation would gives us more confidence in their use for other perinatal (from the start of pregnancy to a year after birth) mental health issues. This could provide future generations with a better start to life.
We would like to acknowledge the contribution of Dr Hayley Bradley to this research project.
Julia J Rucklidge, Professor of Psychology, University of Canterbury; Elena Moltchanova, Professor of Statistics, University of Canterbury; Roger Mulder, Professor of Psychiatry, University of Otago, and Siobhan A Campbell, Intern Psychologist, Researcher – Te Puna Toiora (Mental Health and Nutrition Research Lab), University of Canterbury
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: