Jamaican Coconut Rice
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is a great dish that can be enjoyed hot or cold, as a main or as a side. It has carbs, proteins, healthy fats, fiber, as well as an array of healthy phytochemicals. Not to mention, a great taste!
You will need
- 1 cup wholegrain basmati rice (it may also be called “brown basmati rice“; this is the same) (traditional recipe calls for pudding rice, but we’re going with the healthier option here)
- 2 cans (each 12 z / 400g) coconut milk
- 2 cups (or 2 cans, of which the drained weight is comparable to a cup each) cooked black beans. If you cook them yourself, this is better, as you will be able to cook them more al dente than you can get from a can, and this firmness is desirable. But canned is fine if that’s what’s available.
- 1 large red onion, finely chopped
- ½ cup low-sodium vegetable stock (ideally you made this yourself from vegetable offcuts you saved in the freezer for this purpose, but failing that, low-sodium stock cubes can be bought at any large supermarket)
- 2 serrano chilis, finely chopped
- 1 Scotch bonnet chili, without doing anything to it
- 1 tbsp black pepper, coarse ground
- 1 tbsp chia seeds
- 1 tbsp coconut oil
- Garnish: parsley, chopped
Note: we have erred on the side of low-heat when it comes to the chilis. If you know that you and (if applicable) everyone else eating would enjoy more heat, add more heat. If not, let extra heat be added at the table via your hot sauce of choice. Sounds heretical, but it ensures everyone gets the right amount! It’s easy to add heat than to take it out, after all.
However: if you do end up with too much heat in this or any other dish, adding acid will usually help to neutralize that. In the case of this dish, we’d recommend lime juice as a complementary flavor.
Method
(we suggest you read everything at least once before doing anything)
1) In a big sauté pan, add the coconut oil, melt it if not already melted, and add the chopped onion and the chopped chilis, at a temperature sufficient to sizzle. Keep them all moving. Once the coconut oil is absorbed into the onion (this will happen before the onion is fully cooked), add the vegetable stock, followed by the coconut milk; mix it all gently to create a smooth consistency.
2) Add the rice, chia seeds, and black pepper; mix it all gently but thoroughly; turn the temperature to a simmer, and add the Scotch bonnet chili, without cutting it at all.
3) Cover and keep on low for about 20–30 minutes until the rice is looking done. Check on it periodically to make sure it’s not running out of liquid, but resist the urge to stir it; it shouldn’t be burning but paradoxically, once you start stirring you can’t stop or it will definitely burn.
4) Take out the Scotch bonnet chili, and discard*. Add the black beans.
*its job was to add flavor without adding the high-level heat of that particular chili. If you’re a regular heat-fiend, feel free to experiment with using sliced Scotch bonnet chilis instead of serrano chilis; just be aware that there’s a big difference in heat. Only do this if you really like heat. Using it the way we described in the main recipe is what’s traditional in the Caribbean, by the way.
5) Now you can (and in fact must) stir, to mix in the black beans and bring them back to temperature within the dish. Be aware that once you start stirring, you need to keep stirring until you’re ready to take it off the heat.
6) Serve, adding the parsley garnish.

(this example went light on the beans; our recipe includes more for a heartier dish)
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Should You Go Light Or Heavy On Carbs?
- Our Top 5 Spices: How Much Is Enough For Benefits?
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
- Burn! How To Boost Your Metabolism
- Capsaicin For Weight Loss And Against Inflammation
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Metformin Slows Aging
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Metformin And How It Slows Down Aging
That’s a bold claim for a title, but the scientific consensus is clear, and this Research Review Monday we’re going to take a look at exactly that!
Metformin is a common diabetes-management drug, used to lower blood sugar levels in people who either don’t have enough insulin or the insulin isn’t being recognized well enough by the body.
However, it also slows aging, which is a quality it’s also been studied for for more than a decade. We’ll look at some of the more recent research, though. Let’s kick off with an initial broad statement, from the paper “The Use of Metformin to Increase the Human Healthspan”, as part of the “Advances in Experimental Medicine and Biology” series:
In recent years, more attention has been paid to the possibility of using metformin as an anti-aging drug. It was shown to significantly increase the lifespan in some model organisms and delay the onset of age-associated declines. Growing amounts of evidence from clinical trials suggest that metformin can effectively reduce the risk of many age-related diseases and conditions, including cardiometabolic disorders, neurodegeneration, chronic inflammation and frailty.
How does it work?
That’s still being studied, but the scientific consensus is that it works by inducing hormesis—the process by which minor stress signals cells to start repairing themselves. How does it induce that hormesis? Again, still being studied, but it appears to do it by activating a specific enzyme; namely, the AMP-activated protein kinase:
Read: Metformin-enhances resilience via hormesis
It also has been found to slow aging by means of an anti-inflammatory effect, as a bonus!
Any bad news?
Well, firstly, in most places it’s only prescribed for diabetes management, not for healthy life extension. A lot of anti-aging enthusiasts have turned to the grey market online to get it, and we can’t recommend that.
Secondly, it does have some limitations:
- Its bioavailability isn’t great in tablet form (the form in which it is most commonly given)
- It has quite a short elimination half-life (around 6 hours), which makes it great to fix transient hyperglycemia in diabetics—job done and it’s out—but presents a logistical challenge when it comes to something so pernicious as aging.
- Some people are non-responders (a non-responder, in medicine, is someone for whom a drug simply doesn’t work, for no obvious reason)
Want to know more? Check out:
Metformin in aging and aging-related diseases: clinical applications and relevant mechanism
Share This Post
-
Spelt vs Bulgur – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing spelt to bulgur, we picked the spelt.
Why?
An argument could be made for bulgur, but we say spelt comes out on top. Speaking of “sorting the wheat from the chaff”, be aware: spelt is a hulled wheat product and bulgur is a cracked wheat product.
Looking at macros first, it’s not surprising therefore that spelt has proportionally more carbs and bulgur has proportionally more fiber, resulting in a slightly lower glycemic index. That said, for the exact same reason, spelt is proportionally higher in protein. Still, fiber is usually the most health-relevant aspect in the macros category, so we’re going to call this a moderate win for bulgur.
When it comes to micronutrients, however, spelt is doing a lot better:
In the category of vitamins, spelt is higher in vitamins A, B1, B2, B3, and E (with the difference in E being 26x more!), while bulgur is higher only in vitamin B9 (and that, only slightly). A clear win for spelt here.
Nor are the mineral contents less polarized; spelt has more copper, iron, magnesium, manganese, phosphorus, potassium, selenium, and zinc, while bulgur is not higher in any minerals. Another easy win for spelt.
Adding these up makes a win for spelt, but again we’d urge to not underestimate the importance of fiber. Enjoy both in moderation, unless you are avoiding wheat/gluten in which case don’t, and for almost everyone, mixed whole grains are always going to be best.
Want to learn more?
You might like to read:
- Grains: Bread Of Life, Or Cereal Killer?
- Gluten: What’s The Truth?
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
Take care!
Share This Post
-
Acid Reflux After Meals? Here’s How To Stop It Naturally
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Harvard-trained gastroenterologist Dr. Saurabh Sethi advises:
Calming it down
First of all, what it actually is and how it happens: acid reflux occurs when the lower esophageal sphincter (LES) doesn’t close properly, allowing stomach acid to flow back into the esophagus. Chronic acid reflux is known as gastroesophageal reflux disease (GERD). Symptoms can include heartburn, an acid taste in the mouth, belching, bloating, sore throat, and a persistent cough—but most people do not get all of the symptoms, usually just some.
Things that help it acutely (as in, you can do them today and they will help today): consider skipping certain foods/substances like peppermint, tomatoes, chocolate, alcohol, and caffeine, which can worsen acid reflux. Eating smaller, more frequent meals instead of large ones and leaving a gap of 3–4 hours before lying down after meals can also help manage symptoms.
Things that can help it chronically (as in, you do them in an ongoing fashion and they will help in an ongoing fashion): lifestyle changes like quitting smoking, reducing alcohol intake, and wearing loose clothing can strengthen the LES. Maintaining a healthy weight and avoiding large meals, especially close to bedtime, can also reduce symptoms. Elevating the upper body while sleeping (using a wedge pillow or raising the bed by 10–20°) can make a big difference.
Medications to avoid, if possible, include: aspirin, ibuprofen, and calcium channel blockers.
Some drinks you can enjoy that will help: drinking water can quickly dilute stomach acid and provide relief. Herbal teas like basil tea, fennel tea, and ginger tea are also effective. But notably: not peppermint tea! Since, as mentioned earlier, peppermint is a known trigger for acid reflux (despite peppermint’s usual digestion-improving properties).
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Coughing/Wheezing After Dinner? Here’s How To Fix It ← this is about acid reflux and more
Take care!
Share This Post
Related Posts
-
How weight bias in health care can harm patients with obesity: Research
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Patients who weigh more than what medical authorities generally consider healthy often avoid seeing doctors for fear of being judged, insulted or misdiagnosed, decades of research find. Meanwhile, academic studies consistently show many health care professionals discriminate against heavier patients and that weight bias can drive people with obesity to gain weight.
Weight bias refers to negative attitudes, stereotypes and discrimination aimed at individuals with excess body fat. When scholars reviewed 41 studies about weight bias in health care, published from 1989 to 2021, they found it comes in many forms: contemptuous language, inappropriate gestures, expressing a preference for thinner patients, avoiding physical touch and eye contact, and attributing all of a person’s health issues to their weight.
“Weight bias has been reported in physicians, nurses, dietitians, physiotherapists, and psychologists, as well as nutritionists and exercise professionals, and it is as pervasive among medical professionals as it is within the general population,” write the authors of the research review, published in 2021 in the journal Obesity.
That’s a problem considering an estimated 4 out of 10 U.S. adults aged 20 years and older have obesity, a complex and often misunderstood illness that the American Medical Association voted in 2013 to recognize as a disease. By 2030, half of U.S. adults will have obesity, researchers project in a 2020 paper in the International Journal of Epidemiology.
Worldwide, the obesity rate among adults aged 18 and older was 13% in 2016, according to the World Health Organization. If current trends continue, the World Obesity Federation projects that, by 2035, 51% of the global population will be living with overweight or obesity.
The harms of weight bias
Weight stigma — the societal devaluation of people perceived to be carrying excess weight — drives weight bias. It’s so physically and emotionally damaging that a panel of 36 international experts issued a consensus statement in 2020 to raise awareness about and condemn it. Dozens of medical and academic organizations, including 15 scholarly journals, endorsed the document, published in Nature Medicine.
The release of a consensus statement is a significant event in research, considering it represents the collective position that experts in a particular field have taken on an issue, based on an analysis of all the available evidence.
Research to date indicates heavier individuals who experience weight bias and stigma often:
- Avoid doctors and other health care professionals, skipping routine screenings as well as needed treatments.
- Change doctors frequently.
- Are at a higher risk for depression, anxiety, mood disorders and other mental health problems.
- Avoid or put off exercise.
- Consume more food and calories.
- Gain weight.
- Have disrupted sleep.
The consensus statement notes that educating health care providers, journalists, policymakers and others about obesity is key to changing the narrative around the disease.
“Weight stigma is reinforced by misconceived ideas about body-weight regulation and lack of awareness of current scientific evidence,” write the experts, led by Francesco Rubino, the chair of metabolic and bariatric surgery at Kings College London.
“Despite scientific evidence to the contrary, the prevailing view in society is that obesity is a choice that can be reversed by voluntary decisions to eat less and exercise more. These assumptions mislead public health policies, confuse messages in popular media, undermine access to evidence-based treatments, and compromise advances in research.”
Weight bias and stigma appear to stimulate the secretion of the stress hormone cortisol and promote weight gain, researchers write in a 2016 paper published in Obesity.
A. Janet Tomiyama, a psychology professor at UCLA who directs the university’s Dieting, Stress, and Health research lab, describes weight stigma as “a ‘vicious cycle’ — a positive feedback loop wherein weight stigma begets weight gain.”
“This happens through increased eating behavior and increased cortisol secretion governed by behavioral, emotional, and physiological mechanisms, which are theorized to ultimately result in weight gain and difficulty of weight loss,” Tomiyama writes in her 2014 paper, “Weight Stigma is Stressful. A Review of Evidence for the Cyclic Obesity/Weight-Based Stigma Model.”
The consensus statement spotlights 13 recommendations for eliminating weight bias and stigma, some of which are specifically aimed at health care providers, the media, researchers or policymakers. One of the recommendations for the health care community: “[Health care providers] specialized in treating obesity should provide evidence of stigma-free practice skills. Professional bodies should encourage, facilitate, and develop methods to certify knowledge of stigma and its effects, along with stigma-free skills and practices.”
The one recommendation for the media: “We call on the media to produce fair, accurate, and non-stigmatizing portrayals of obesity. A commitment from the media is needed to shift the narrative around obesity.”
Why obesity is a complicated disease
It’s important to point out that having excess body fat does not, by itself, mean an individual is unhealthy, researchers explain in a 2017 article in The Conversation, which publishes research-based news articles and essays. But it is a major risk factor for cardiovascular disease, including stroke, as well as diabetes, some types of cancer, and musculoskeletal disorders such as osteoarthritis.
Doctors often look at patients’ body mass index — a number that represents their weight in relation to their height — to gauge the amount of fat on their bodies. A BMI of 18.5 to 24.9 is ideal, according to the U.S. Centers for Disease Control and Prevention. A BMI of 25.0 to 29.9, indicates excess body fat, or “overweight,” while a BMI of 30 and above indicates obesity.
In June, the American Medical Association announced a new policy clarifying how BMI can be used to diagnose obesity. Because it’s an imperfect measure for body fat, the organization suggests BMI be used in conjunction with other measures such as a patient’s waist circumference and skin fold thickness.
Two specialists who have been working for years to dispel myths and misconceptions about obesity are Fatima Cody Stanford, an obesity physician and associate professor at Harvard Medical School, and Rebecca Puhl, the deputy director of the Rudd Center for Food Policy and Obesity at the University of Connecticut.
Cody Stanford has called obesity “a brain disease” because the brain tells the body how much to eat and what to do with the food consumed. One pathway in the brain directs the body to eat less and store less fat, she explains in a February 2023 podcast produced by the American Medical Association.
“For people that signal really great down this pathway, they tend to be very lean, not struggle with their weight in the same way that people that have excess weight do,” she says during the podcast, adding that people with obesity receive signals from an alternate pathway that “tells us to eat more and store more.”
Academic studies demonstrate that a wide variety of factors can affect weight regulation, including sleep quality and duration, gut health, genetics, medication, access to healthy foods and even early life experiences.
For example, a 2020 paper in the journal JAMA Network Open suggests female infants born by cesarean delivery have a higher risk of obesity during adulthood than female infants born by vaginal delivery. The study of 33,226 U.S. women born between 1946 and 1964 found that a cesarean delivery is associated with an 11% higher risk of developing obesity and a 46% higher risk of developing type 2 diabetes.
Scholars have also found that traumatic childhood experiences such as abuse and neglect are linked to adult obesity, according to a research review published in 2020.
Income inequality seems to play a role as well. When researchers from the Johns Hopkins Bloomberg School of Public Health studied the link between income inequality and obesity for a sample of 36,665 U.S. adults, they discovered women with lower incomes are more likely to have obesity than women with higher incomes.
Their analysis indicates the opposite is true for men, whose odds of obesity rise with their income, the researchers write in a 2021 paper in the International Journal of Environmental Research and Public Health.
Weight bias among doctor trainees
While scholars have learned a lot about obesity and weight bias in recent decades, the information might not be reaching people training to become doctors. A study published in October finds that some resident physicians believe obesity to be the result of poor choices and weak willpower.
Researchers asked 3,267 resident physicians who graduated from a total of 49 U.S. medical schools a series of questions to gauge their knowledge of obesity and attitudes toward heavier patients. What they learned: Nearly 40% of resident physicians agreed with the statement, “Fat people tend to be fat pretty much through their own fault.” Almost half agreed with the statement, “Some people are fat because they have no willpower.”
The study also reveals that about one-third of participants said they “feel more irritated when treating an obese patient than a non-obese patient.”
“Notably, more than a quarter of residents expressed slight-to-strong agreement with the item ‘I dislike treating obese patients,’” the researchers write.
Another takeaway from the paper: Resident physicians specializing in orthopedic surgery, anesthesiology and urology expressed the highest levels of dislike of heavier patients. Of the 16 medical specialties represented, residents in family medicine, psychiatry and pediatrics reported the lowest levels of dislike.
Kimberly Gudzune, medical director of the American Board of Obesity Medicine, asserts that doctors and medical students need to be educated about obesity. The topic “is grossly neglected” in medical schools and medical training programs worldwide, research has found.
Many physicians don’t understand obesity, Gudzune explains in a July 2023 interview on the internal medicine podcast “The Curbsiders.”
“I think back to when I was a medical student, when I was a resident, I really didn’t learn much about obesity and how to treat it, yet it’s a problem that affects the majority of our patients,” she tells podcast listeners. “I think there’s a lot of evidence out there showing that primary care physicians don’t really know where to start.”
In 2011, the American Board of Obesity Medicine established a program through which doctors could become certified in obesity medicine. Since then, a total of 6,729 U.S. doctors have earned certification, the vast majority of whom specialize in family and internal medicine.
What health care providers think
The experts who created the consensus statement on weight bias and stigma noted health care providers’ shortcomings in the document. They write that the common themes they discovered in the research include “contemptuous, patronizing, and disrespectful treatment” of patients, a lack of training, poor communication and assumptions about weight gain.
Puhl, the deputy director of the Rudd Center at the University of Connecticut, is a pioneer in weight bias research and one of the experts who wrote the consensus statement. During an episode of “The Leading Voices in Food,” a podcast created by Duke University’s World Food Policy Center, she shares details about what she has learned over the years.
“[Health care providers’] views that patients with obesity are lazy or lacking control, are to blame for their weight or noncompliant with treatment,” she says during the interview. “We know, for example, that some physicians spend less time in their appointments with patients [who] have a larger body size. They give them less education about health. They’re more reluctant to perform certain screenings. They talk about treating patients with obesity as being a greater waste of their time than providing care to thinner patients. And we know that patients seem to be aware of these biases from providers and that can really contribute to patients avoiding health care because they just don’t want to repeat those negative experiences of bias.”
To set the record straight, the experts who wrote the the consensus statement listed the following five common assumptions as being “at odds with a definitive body of biological and clinical evidence.”
1. Body weight = calories in – calories out.
This equation oversimplifies the relationship between body weight and energy consumed and used, the experts write. “Both variables of the equation depend on factors additional to just eating and exercising. For instance, energy intake depends on the amount of food consumed, but also on the amount of food-derived energy absorbed through the gastrointestinal tract, which in turn is influenced by multiple factors, such as digestive enzymes, bile acids, microbiota, gut hormones, and neural signals, none of which are under voluntary control.”
2. Obesity is primarily caused by voluntary overeating and a sedentary lifestyle.
According to the experts, overeating and forgoing exercise might be symptoms of obesity rather than the root causes. There are many possible causes and contributors “including geneticand epigenetic factors, foodborne factors, sleep deprivation and circadian dysrhythmia, psychological stress, endocrine disruptors, medications, and intrauterine and intergenerational effects. These factors do not require overeating or physical inactivity to explain excess weight.” they write.
3. Obesity is a lifestyle choice.
“People with obesity typically recognize obesity as a serious health problem, rather than a conscious choice,” the experts write. “Given the negative effects of obesity on quality of life, the well-known risks of serious complications and reduced life expectancy associated with it, it is a misconception to define obesity as a choice.”
4. Obesity is a condition, not a disease.
The criteria generally used to determine disease status “are clearly fulfilled in many individuals with obesity as commonly defined, albeit not all,” the experts explain. “These criteria include specific signs or symptoms (such as increased adiposity), reduced quality of life, and/or increased risk of further illness, complications, and deviation from normal physiology — or well-characterized pathophysiology (for example, inflammation, insulin resistance, and alterations of hormonal signals regulating satiety and appetite).”
5. Severe obesity is usually reversible by voluntarily eating less and exercising more.
“A large body of clinical evidence has shown that voluntary attempts to eat less and exercise more render only modest effects on body weight in most individuals with severe obesity,” the experts write. “When fat mass decreases, the body responds with reduced resting energy expenditure and changes in signals that increase hunger and reduce satiety (for example, leptin, ghrelin). These compensatory metabolic and biologic adaptations promote weight regain and persist for as long as persons are in the reduced-energy state, even if they gain some weight back.”
Health care facility improvements
The expert panel also determined that many health care facilities aren’t equipped to treat people with obesity. Examination gowns, blood pressure cuffs, chairs and examination tables often are too small, patients have reported.
When researchers from the University of Minnesota, Minneapolis Veterans Affairs Medical Center and Mayo Clinic studied the quality of care that patients with obesity receive, they learned that a clinic’s physical environment can have a big effect on a patient’s experience.
They write in a 2015 study published in Obesity Reviews: “Waiting room chairs with armrests can be uncomfortable or too small. Equipment such as scales, blood pressure cuffs, examination gowns and pelvic examination instruments are often designed for use with smaller patients. When larger alternatives are not available, or are stored in a place that suggests infrequent use, it can signal to patients that their size is unusual and that they do not belong. These experiences, which are not delivered with malicious intent, can be humiliating.”
When medical equipment is the wrong size, it may not work correctly. For instance, chances are high that a blood pressure reading will be inaccurate if a health care professional uses a blood pressure cuff that’s too small on a patient with obesity, a 2022 paper finds.
To create a comfortable environment for patients with high body weights, the Rudd Center for Food Policy and Obesity recommends that health care facilities provide, among other things, extra-large exam gowns, chairs that can support more than 300 pounds and do not have arms, and wide exam tables that are bolted to the floor so they don’t move.
The consensus statement also recommends improvements to health care facilities.
“Given the prevalence of obesity and obesity-related diseases,” the 36 international experts write, “appropriate infrastructure for the care and management of people with obesity, including severe obesity, must be standard requirement for accreditation of medical facilities and hospitals.”
Source list:
Weight Bias Among Health Care Professionals: A Systematic Review and Meta-Analysis
Blake J. Lawrence; et al. Obesity, November 2021.Joint International Consensus Statement for Ending Stigma of Obesity
Francesco Rubino, et al. Nature Medicine, March 2020.Perceived Weight Discrimination and Chronic Biochemical Stress: A Population-Based Study Using Cortisol in Scalp Hair
Sarah E. Jackson, Clemens Kirschbaum and Andrew Steptoe. Obesity, December 2016.Weight Stigma is Stressful. A Review of Evidence for the Cyclic Obesity/Weight-Based Stigma Model
A. Janet Tomiyama. Appetite, November 2014.Association of Birth by Cesarean Delivery with Obesity and Type 2 Diabetes Among Adult Women
Jorge E. Chavarro. JAMA Network Open, April 2020.Adverse Childhood Experiences and Adult Obesity: A Systematic Review of Plausible Mechanisms and Meta-Analysis of Cross-Sectional Studies
David A. Wiss and Timothy D. Brewerton. Physiology & Behavior, September 2020.Income Inequality and Obesity among U.S. Adults 1999–2016: Does Sex Matter?
Hossein Zare, Danielle D. Gaskin and Roland J. Thorpe Jr. International Journal of Environmental Research and Public Health, July 2021.Comparisons of Explicit Weight Bias Across Common Clinical Specialties of U.S. Resident Physicians
Samantha R. Philip, Sherecce A. Fields, Michelle Van Ryn and Sean M. Phelan. Journal of General Internal Medicine, October 2023.Impact of Weight Bias and Stigma on Quality of Care and Outcomes for Patients with Obesity
S.M. Phelan; et al. Obesity Reviews, April 2015.One Size Does Not Fit All: Impact of Using A Regular Cuff For All Blood Pressure Measurements
Tammy. M. Brady; et al. Circulation, April 2022.This article first appeared on The Journalist’s Resource and is republished here under a Creative Commons license.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Should Men Over 50 Get PSA?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? You can always hit “reply” to any of our emails, or use the feedback widget at the bottom!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝Loved the information on prostate cancer. Do recommend your readers get a PSA or equivalent test annually for over 50 yr old men.❞
(This is about: Prostate Health: What You Should Know)
Yep, or best yet, the much more accurate PSE test! But if PSA test is what’s available, it’s a lot better than nothing. And, much as it’s rarely the highlight of anyone’s day, a prostate exam by a suitably qualified professional is also a good idea.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Hearing voices is common and can be distressing. Virtual reality might help us meet and ‘treat’ them
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Have you ever heard something that others cannot – such as your name being called? Hearing voices or other noises that aren’t there is very common. About 10% of people report experiencing auditory hallucinations at some point in their life.
The experience of hearing voices can be very different from person to person, and can change over time. They might be the voice of someone familiar or unknown. There might be many voices, or just one or two. They can be loud or quiet like a whisper.
For some people these experiences are positive. They might represent a spiritual or supernatural experience they welcome or a comforting presence. But for others these experiences are distressing. Voices can be intrusive, negative, critical or threatening. Difficult voices can make a person feel worried, frightened, embarrassed or frustrated. They can also make it hard to concentrate, be around other people and get in the way of day-to-day activities.
Although not everyone who hears voices has a mental health problem, these experiences are much more common in people who do. They have been considered a hallmark symptom of schizophrenia, which affects about 24 million people worldwide.
However, such experiences are also common in other mental health problems, particularly in mood- and trauma-related disorders (such as bipolar disorder or depression and post-traumatic stress disorder) where as many as half of people may experience them.
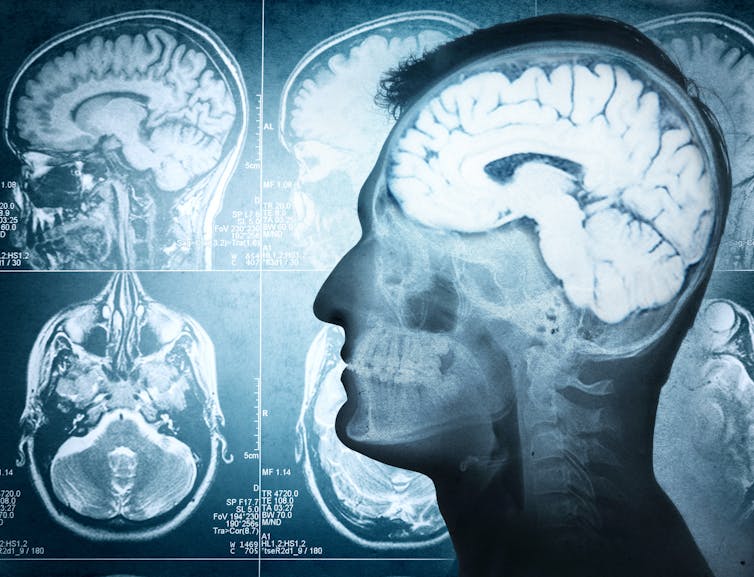
Rawpixel/Shutterstock Why do people hear voices?
It is unclear exactly why people hear voices but exposure to prolonged stress, trauma or depression can increase the chances.
Some research suggests people who hear voices might have brains that are “wired” differently, particularly between the hearing and speaking parts of the brain. This may mean parts of our inner speech can be experienced as external voices. So, having the thought “you are useless” when something goes wrong might be experienced as an external person speaking the words.
Other research suggests it may relate to how our brains use past experiences as a template to make sense of and make predictions about the world. Sometimes those templates can be so strong they lead to errors in how we experience what is going on around us, including hearing things our brain is “expecting” rather than what is really happening.
What is clear is that when people tell us they are hearing voices, they really are! Their brain perceives voice experiences as if someone were talking in the room. We could think of this “mistake” as working a bit like being susceptible to common optical tricks or visual illusions.
There may be differences in the brains of people who hear voices. Triff/Shutterstock Coping with hearing voices
When hearing voices is getting in the way of life, treatment guidelines recommend the use of medications. But roughly a third of people will experience ongoing distress. As such, treatment guidelines also recommend the use of psychological therapies such as cognitive behavioural therapy.
The next generation of psychological therapies are beginning to use digital technologies and virtual reality offers a promising new medium.
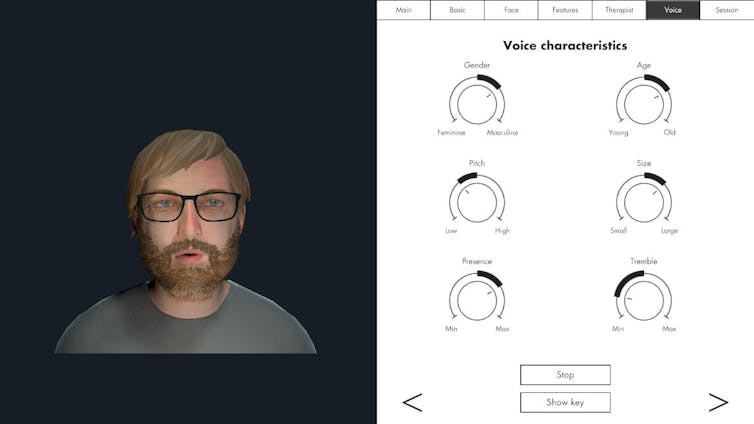
Avatar therapy allows a person to create a virtual representation of the voice or voices, which looks and sounds like what they are experiencing. This can help people regain power in the “relationship” as they interact with the voice character, supported by a therapist.
Jason’s experience
Aged 53, Jason (not his real name) had struggled with persistent voices since his early 20s. Antipsychotic medication had helped him to some extent over the years, but he was still living with distressing voices. Jason tried out avatar therapy as part of a research trial.
He was initially unable to stand up to the voices, but he slowly gained confidence and tested out different ways of responding to the avatar and voices with his therapist’s support.
Jason became more able to set boundaries, such as not listening to them for periods throughout the day. He also felt more able to challenge what they said and make his own choices.
Over a couple of months, Jason started to experience some breaks from the voices each day and his relationship with them started to change. They were no longer like bullies, but more like critical friends pointing out things he could consider or be aware of.
A screenshot from HekaVR, the software used in the Australian AMETHYST trial. HekaVR, CC BY-ND Gaining recognition
Following promising results overseas and its recommendation by the United Kingdom’s National Institute for Health and Care Excellence, our team has begun adapting the therapy for an Australian context.
We are trialling delivering avatar therapy from our specialist voices clinic via telehealth. We are also testing whether avatar therapy is more effective than the current standard therapy for hearing voices, based on cognitive behavioural therapy.
As only a minority of people with psychosis receive specialist psychological therapy for hearing voices, we hope our trial will support scaling up these new treatments to be available more routinely across the country.
We would like to acknowledge the advice and input of Dr Nadine Keen (consultant clinical psychologist at South London and Maudsley NHS Foundation Trust, UK) on this article.
Leila Jameel, Trial Co-ordinator and Research Therapist, Swinburne University of Technology; Imogen Bell, Senior Research Fellow and Psychologist, The University of Melbourne; Neil Thomas, Professor of Clinical Psychology, Swinburne University of Technology, and Rachel Brand, Senior Lecturer in Clinical Psychology, University of the Sunshine Coast
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: