Cleaning Up Your Mental Mess – by Dr. Caroline Leaf
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
First of all, what mental mess is this? Well, that depends on you, but common items include:
- Anxiety
- Depression
- Stress
- Trauma
Dr. Caroline Leaf also includes the more nebulous item “toxic thoughts”, but this is mostly a catch-all term.
Given that it says “5 simple scientifically proven steps”, it would be fair if you are wondering:
“Is this going to be just basic CBT stuff?”
And… First, let’s not knock basic CBT stuff. It’s not a panacea, but it’s a great tool for a lot of things. However… Also, no, this book is not about just basic CBT stuff.
In fact, this book’s methods are presented in such a novel way that this reviewer was taken aback by how unlike it was to anything she’d read before.
And, it’s not that the components themselves are new—it’s just that they’re put together differently, in a much more organized comprehensive and systematic way, so that a lot less stuff falls through the cracks (a common problem with standalone psychological tools and techniques).
Bottom line: if you buy one mental health self-help book this year, we recommend that it be this one
Click here to check out Cleaning Up Your Mental Mess, and take a load off your mind!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Not To Die – by Dr. Michael Greger
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We previously reviewed this book some years ago, but we’re revisiting it now because:
- It really is a book that should be in every healthspan-enjoyer’s collection
- Our book reviews back then were not as comprehensive as now (though we still generally try to fit into the “it takes about one minute to read this review” idea, sometimes we’ll spend a little extra time).
Dr. Greger (of “Dr. Greger’s Daily Dozen” fame) outlines for us in cold hard facts and stats what’s most likely to be our cause of death. While this is not a cheery premise for a book, he then sets out to work back from there—what could have prevented those specific things?
Thus, while the book doesn’t confer immortality (the title is not “how to not die”, after all), it does teach us how not to die—i.e, from heart disease, lung diseases, brain diseases, digestive cancers, infections, diabetes, high blood pressure, liver disease, blood cancers, kidney disease, breast cancer, suicidal depression, prostate cancer, Parkinson’s disease, and even iatrogenic causes.
This it does with a lot of solid science, explained for the layperson, and/but without holding back when it comes to big words, and a lot of them, at that. If you want to add in daily exercises, just lifting the book could be a start; weighing in at 678 pages, it’s an information-dense tome that’s more likely to be sifted through than read cover-to-cover.
The style is thus dense science somewhat editorialized for lay readability, and well-evidenced with around 3,000 citations. That’s not a typo; there are 178 pages of bibliography at the back with about 15–20 scientific references per page.
In terms of practical use, he does also devote chapters to that, it’s not just all textbook. Indeed, he discusses the reasonings behind the items, portion sizes, and quantities of his “daily dozen” foods, so that the reader will understand how much bang-for-buck they deliver, and then it’ll seem a lot less like an arbitrary list, and more likely to be adopted and maintained.
Bottom line: if you care about not getting life-threatening illnesses (which at the end of the day, come to most people at some point), then this book is a must-read.
Share This Post
-
Menopause, & When Not To Let Your Guard Down
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This is Dr. Jessica Shepherd, a physician Fellow of the American College of Obstetricians & Gynecologists, CEO at Sanctum Medical & Wellness, and CMO at Hers.
She’s most well-known for her expertise in the field of the menopause. So, what does she want us to know?
Untreated menopause is more serious than most people think
Beyond the famous hot flashes, there’s also the increased osteoporosis risk, which is more well-known at least amongst the health-conscious, but oft-neglected is the increased cardiovascular disease risk:
What Menopause Does To The Heart
…and, which a lot of Dr. Shepherd’s work focuses on, it also increases dementia risk; she cites that 60–80% of dementia cases are women, and it’s also established that it progresses more quickly in women than men too, and this is associated with lower estrogen levels (not a problem for men, because testosterone does it for them) which had previously been a protective factor, but in untreated menopause, was no longer there to help:
Alzheimer’s Sex Differences May Not Be What They Appear
Treated menopause is safer than many people think
The Women’s Health Initiative (WHI) study, conducted in the 90s and published in 2002, linked HRT to breast cancer, causing fear, but it turned out that this was quite bad science in several ways and the reporting was even worse (even the flawed data did not really support the conclusion, much less the headlines); it was since broadly refuted (and in fact, it can be a protective factor, depending on the HRT regimen), but fearmongering headlines made it to mainstream news, whereas “oopsies, never mind, we take that back” didn’t.
The short version of the current state of the science is: breast cancer risk varies depending on age, HRT type, and dosage; some kinds of HRT can increase the risk marginally in those older than 60, but absolute risk is low compared to placebo, and taking estrogen alone can reduce risk at any age in the event of not having a uterus (almost always because of having had a hysterectomy; as a quirk, it is possible to be born without, though).
It’s worth noting that even in the cases where HRT marginally increased the risk of breast cancer, it significantly decreased the risk of cancers in total, as well fractures and all-cause-mortality compared to the placebo group.
In other words, it might be worth having a 0.12% risk of breast cancer, to avoid the >30% risk of osteoporosis, which can ultimately be just as fatal (without even looking at the other things the HRT is protective against).
However! In the case of those who already have (or have had) breast cancer, increasing estrogen levels can indeed make that worse/return, and it becomes more complicated in cases where you haven’t had it, but there is a family history of it, or you otherwise know you have the gene for it.
You can read more about HRT and breast cancer risk (increases and decreases) here:
…and about the same with regard to HMT, here:
The Hormone Therapy That Reduces Breast Cancer Risk & More
Lifestyle matters, and continues to matter
Menopause often receives the following attention from people:
- Perimenopause: “Is this menopause?”
- Menopause: “Ok, choices to make about HRT or not, plus I should watch out for osteoporosis”
- Postmenopause: “Yay, that’s behind me now, back to the new normal”
The reality, Dr. Shepherd advises, is that “postmenopause” is a misnomer because if it’s not being treated, then the changes are continuing to occur in your body.
This is a simple factor of physiology; your body is always rebuilding itself, will never stop until you die, and in untreated menopause+postmenopause, it’s now doing it without much estrogen.
So, you can’t let your guard down!
Thus, she recommends: focus on maintaining muscle mass, bone health, and cardiovascular health. If you focus on those things, the rest (including your brain, which is highly dependent on cardiovascular health) will mostly take care of itself.
Because falls and fractures, particularly hip fractures, drastically reduce quality and length of life in older adults, it is vital to avoid those, and try to be sufficiently robust so that if you do go A over T, you won’t injure yourself too badly, because your bones are strong. As a bonus, the same things (especially that muscle mass we talked about) will help you avoid falling in the first place, by improving stability.
See also: Resistance Is Useful! (Especially As We Get Older)
And about falls specifically: Fall Special: Be Robust, Mobile, & Balanced!
Want to know more from Dr. Shepherd?
You might like this book of hers that we reviewed not long back:
Generation M – by Dr. Jessica Shepherd
Take care!
Share This Post
-
What’s the difference between a food allergy and an intolerance?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
At one time or another, you’ve probably come across someone who is lactose intolerant and might experience some unpleasant gut symptoms if they have dairy. Maybe it’s you – food intolerances are estimated to affect up to 25% of Australians.
Meanwhile, cow’s milk allergy is one of the most common food allergies in infants and young children, affecting around one in 100 infants.
But what’s the difference between food allergies and food intolerances? While they might seem alike, there are some fundamental differences between the two.
Feel good studio/Shutterstock What is an allergy?
Australia has one of the highest rates of food allergies in the world. Food allergies can develop at any age but are more common in children, affecting more than 10% of one-year-olds and 6% of children at age ten.
A food allergy happens when the body’s immune system mistakenly reacts to certain foods as if they were dangerous. The most common foods that trigger allergies include eggs, peanuts and other nuts, milk, shellfish, fish, soy and wheat.
Mild to moderate signs of food allergy include a swollen face, lips or eyes; hives or welts on your skin; or vomiting. A severe allergic reaction (called anaphylaxis) can cause trouble breathing, persistent dizziness or collapse.
What is an intolerance?
Food intolerances (sometimes called non-allergic reactions) are also reactions to food, but they don’t involve your immune system.
For example, lactose intolerance is a metabolic condition that happens when the body doesn’t produce enough lactase. This enzyme is needed to break down the lactose (a type of sugar) in dairy products.
Food intolerances can also include reactions to natural chemicals in foods (such as salicylates, found in some fruits, vegetables, herbs and spices) and problems with artificial preservatives or flavour enhancers.
Lactose intolerance is caused by a problem with breaking down lactose in milk. Pormezz/Shutterstock Symptoms of food intolerances can include an upset stomach, headaches and fatigue, among others.
Food intolerances don’t cause life-threatening reactions (anaphylaxis) so are less dangerous than allergies in the short term, although they can cause problems in the longer term such as malnutrition.
We don’t know a lot about how common food intolerances are, but they appear to be more commonly reported than allergies. They can develop at any age.
It can be confusing
Some foods, such as peanuts and tree nuts, are more often associated with allergy. Other foods or ingredients, such as caffeine, are more often associated with intolerance.
Meanwhile, certain foods, such as cow’s milk and wheat or gluten (a protein found in wheat, rye and barley), can cause both allergic and non-allergic reactions in different people. But these reactions, even when they’re caused by the same foods, are quite different.
For example, children with a cow’s milk allergy can react to very small amounts of milk, and serious reactions (such as throat swelling or difficulty breathing) can happen within minutes. Conversely, many people with lactose intolerance can tolerate small amounts of lactose without symptoms.
There are other differences too. Cow’s milk allergy is more common in children, though many infants will grow out of this allergy during childhood.
Lactose intolerance is more common in adults, but can also sometimes be temporary. One type of lactose intolerance, secondary lactase deficiency, can be caused by damage to the gut after infection or with medication use (such as antibiotics or cancer treatment). This can go away by itself when the underlying condition resolves or the person stops using the relevant medication.
Whether an allergy or intolerance is likely to be lifelong depends on the food and the reason that the child or adult is reacting to it.
Allergies to some foods, such as milk, egg, wheat and soy, often resolve during childhood, whereas allergies to nuts, fish or shellfish, often (but not always) persist into adulthood. We don’t know much about how likely children are to grow out of different types of food intolerances.
How do you find out what’s wrong?
If you think you may have a food allergy or intolerance, see a doctor.
Allergy tests help doctors find out which foods might be causing your allergic reactions (but can’t diagnose food intolerances). There are two common types: skin prick tests and blood tests.
In a skin prick test, doctors put tiny amounts of allergens (the things that can cause allergies) on your skin and make small pricks to see if your body reacts.
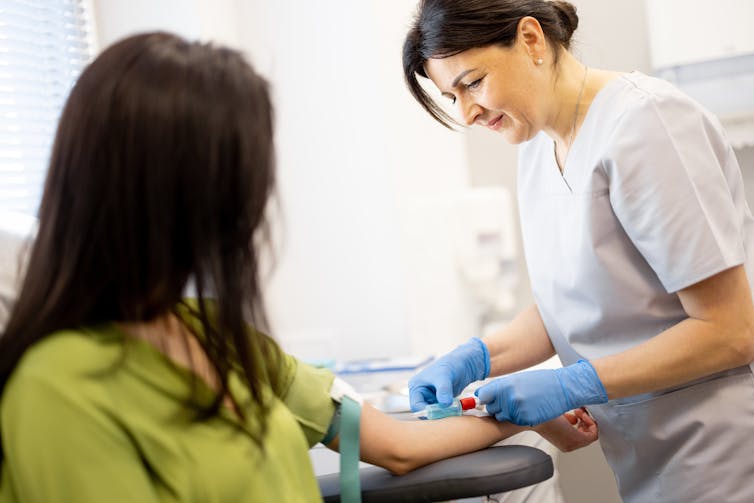
A blood test checks for allergen-specific immunoglobulin E (IgE) antibodies in your blood that show if you might be allergic to a particular food.
Blood tests can help diagnose allergies. RossHelen/Shutterstock Food intolerances can be tricky to figure out because the symptoms depend on what foods you eat and how much. To diagnose them, doctors look at your health history, and may do some tests (such as a breath test). They may ask you to keep a record of foods you eat and timing of symptoms.
A temporary elimination diet, where you stop eating certain foods, can also help to work out which foods you might be intolerant to. But this should only be done with the help of a doctor or dietitian, because eliminating particular foods can lead to nutritional deficiencies, especially in children.
Is there a cure?
There’s currently no cure for food allergies or intolerances. For allergies in particular, it’s important to strictly avoid allergens. This means reading food labels carefully and being vigilant when eating out.
However, researchers are studying a treatment called oral immunotherapy, which may help some people with food allergies become less sensitive to certain foods.
Whether you have a food allergy or intolerance, your doctor or dietitian can help you to make sure you’re eating the right foods.
Victoria Gibson, a Higher Degree by Research student and Research Officer at the School of Nursing, Midwifery and Social Work at the University of Queensland, and Rani Scott-Farmer, a Senior Research Assistant at the University of Queensland, contributed to this article.
Jennifer Koplin, Group Leader, Childhood Allergy & Epidemiology, The University of Queensland and Desalegn Markos Shifti, Postdoctoral Research Fellow, Child Health Research Centre, Faculty of Medicine, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
These Signs Often Mean These Nutrient Deficiencies (Do You Have Any?)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
These are not a necessary “if this then this” equation, but rather a “if this, then probably this”, and it’s a cue to try upping that thing in your diet, and if that doesn’t quickly fix it, get some tests done:
- White bumps on the skin: vitamin A, omega 3
- Craving sour foods: vitamin C
- Restless leg syndrome: iron, magnesium
- Cracked lips: vitamin B2
- Tingling hands and feet: vitamin B12
- Easy bruising: vitamin K and vitamin C
- Canker sores: vitamin B9 (folate), vitamin B12, iron
- Brittle or misshapen nails: vitamin B7 (biotin)
- Craving salty foods: sodium, potassium
- Prematurely gray hair: copper, vitamin B9 (folate), vitamin B12
- Dandruff: omega 3, zinc, vitamin B6
- Craving ice: iron
Dr. LeGrand Peterson has more to say about these though, as well as a visual guide to symptoms, so do check out the video:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to know more?
You might like this previous main feature about supplements vs nutrients from food
Do We Need Supplements, And Do They Work?
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Red Cabbage vs Brussels Sprouts – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing red cabbage to Brussels sprouts, we picked the sprouts.
Why?
First let’s note that we have an interesting comparison today, because these two plants are the exact same species (and indeed, also the exact same species as broccoli, cauliflower. and kale)—just a different cultivar. All of these plants and more are simply cultivars of Brassica oleracea.
Them being the same species notwithstanding, there are nutritional differences:
In terms of macros, the sprouts have more than 2x the protein, slightly more carbs, and nearly 2x the fiber. An easy win for sprouts here.
Looking at vitamins next, red cabbage has more vitamin A (whence the color), while Brussels sprouts have more of vitamins B1, B2, B3, B5, B6, B7, B9, C, E, K, and choline. Another easy win for sprouts.
In the category of minerals, red cabbage has a tiny bit more calcium, while Brussels sprouts have more copper, iron, magnesium, manganese, phosphorus, potassium, selenium, and zinc—while being literally just a few mg/100g behind red cabbage on calcium anyway. So, once again, sprouts are sweeping the victory.
Both vegetables are a rich source of assorted polyphenols; for most polyphenols, Brussels sprouts scores higher—an exception being that red cabbage is very slightly higher in quercetin. So, we’ll call this category a win for Brussels sprouts, too.
In short: enjoy both; diversity is great and so is pretty much any iteration of Brassica oleracea. Standing next to Brussels sprouts made red cabbage look bad, but we assure you that cabbage in general is a nutritional powerhouse, and in this case it was hot the heels of sprouts in most of those micronutrients. If you’re going to pick one though, the Brussels sprouts are indeed the more nutritionally dense.
Want to learn more?
You might like to read:
Sprout Your Seeds, Grains, Beans, Etc ← sprout your Brassica oleracea, too!
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Best Salt for Neti Pots?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
❓ Q&A With 10almonds Subscribers!
Q: What kind of salt is best for neti pots?
A: Non-iodised salt is usually recommended, but really, any human-safe salt is fine. By this we mean for example:
- Sodium chloride (like most kitchen salts),
- Potassium chloride (as found in “reduced sodium” kitchen salts), or
- Magnesium sulfate (also known as epsom salts).
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: