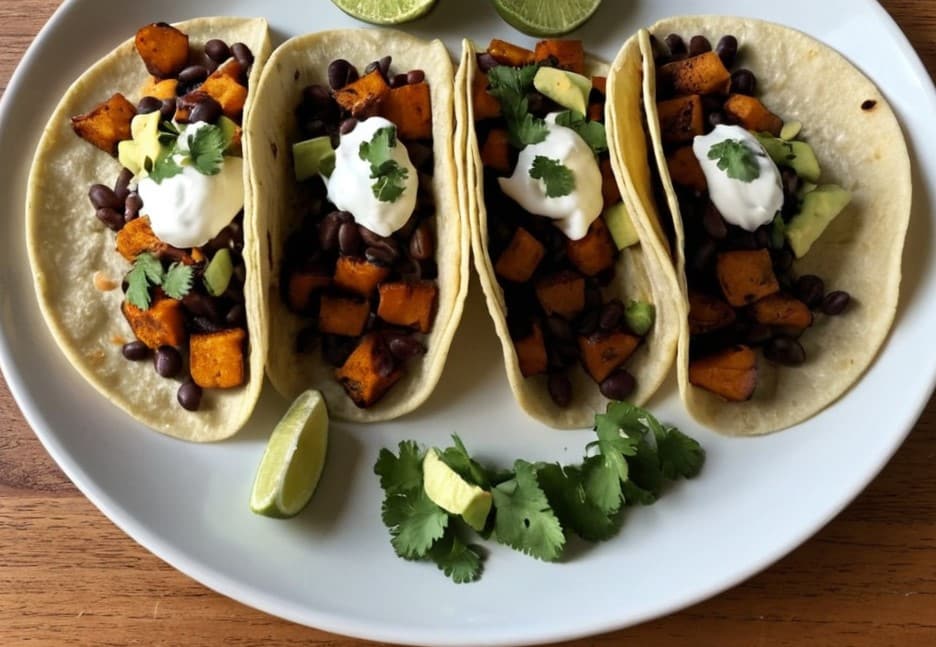The Longevity Diet – by Dr. Valter Longo
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Another book with “The New Science” in its subtitle, so, is this one a new science?
Yes and no; some findings are new, many are not, what really sets this book apart from many of its genre though is that rather than focusing on fighting aging, it focuses on retaining youth. While this may seem like one and the same thing, there is a substantive difference beyond the ideological, which is: while anti-aging research focuses on what causes people to suffer age-related decline and fights each of those things, Dr. Longo’s research focuses on what is predominant in youthful bodies, cells, DNA, and looks to have more of that. Looking in a slightly different place means finding slightly different things, and knowledge is power indeed.
Dr. Longo bases his research and focus on his “5 pillars of longevity”. We’ll not keep them a mystery; they are:
- Juventology research
- Epidemiology
- Clinical studies
- Centenarian studies
- Study of complex systems
The first there (juventology research) may sound like needless jargon, but it is the counterpoint of the field of gerontology, and is otherwise something that didn’t have an established name.
You may wonder why “clinical studies” gets a separate item when the others already include studies; this is because many studies when it comes to aging and related topics are population-based studies, cohort studies, observational studies, or (as is often the case) multiple of the above at once.
Of course, all this discussion of academia is not itself practical information for the reader (unless we happen to work in the field), but it is interesting and does give confidence in the conclusions upon which the practical parts of the book are based.
And what are they? As the title suggests, it’s about diet, and specifically, it’s about Dr. Longo’s “fast-mimicking diet”, which boasts the benefits of intermittent fasting without intermittent fasting. This hinges, of course, on avoiding metabolic overload, which can be achieved with a fairly simple diet governed by the principles outlined in this book, based on the research referenced.
In the category of subjective criticism, there is quite a bit of fluff, much of it self-indulgently autobiographical and very complimentary, but its presence does not take anything away from the excellent content contained in the book.
Bottom line: if you’d like a fresh perspective on regaining/retaining youthfulness, then this is a great book to read.
Click here to check out The Longevity Diet, and stay younger!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:

Bone on Bone – by Dr. Meredith Warner
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What this is not: a book about one specific condition, injury, or surgery.
What this is: a guide to dealing with the common factors of many musculoskeletal conditions, inflammatory diseases, and their consequences.
Dr. Warner takes the opportunity to address the whole patient—presumably: the reader, though it could equally be a reader’s loved one, or even a reader’s patient, insofar as this book will probably be read by doctors also.
She takes an “inside-out and outside-in” approach; that is to say, addressing the problem from as many vectors as reasonably possible—including supplements, diet, dietary habits (things like intermittent fasting etc), exercise, and even sleep. And yes, she knows how difficult those latter items can be, and addresses them not merely with a “but it’s important” but also with practical advice.
As an orthopedic surgeon, she’s not a fan of surgery, and counsels the reader to avoid that if reasonably possible. She also talks about how many people in the US are encouraged to have MRI scans for financial reasons (as in, they can be profitable for the doctor/institution), and then any abnormality is used as justification for surgery, to backwards-justify the use of the MRI, even if the abnormality is not actually the cause of the pain.
Noteworthily, humans in general are a typically a pile of abnormalities in a trenchcoat. Our propensity to mutation has made us one of the most adaptable species on the planet, yet many would have us pretend that the insides of people look like they do in textbooks, or else are wrong. The reality is not so, and Dr. Warner rightly shows this for what it is.
Bottom line: if you or a loved one are suffering from, or at risk of, musculoskeletal and/or inflammatory conditions, this is a top-tier book for having a much easier time of it.
Share This Post

Nasal Hair; How Far To Go?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
t’s Q&A Day at 10almonds!
Have a question or a request? You can always hit “reply” to any of our emails, or use the feedback widget at the bottom!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝As a man in his sixties I find I need to trim my nasal hair quite frequently, otherwise it sticks out in an unsightly manner. But I’m never sure how severely I should cut the hairs back, or even how best to do it. Please advise.❞
As you might know, those hairs are really important for our health, so let’s start by mentioning that yes, trimming is the way, not plucking!
In an ideal world, we’d not trim them further back than the entrance to our nostrils, but given the constant nature of hair-growing, that could become a Sisyphean task.
A good compromise, if you’re not up for trimming when you get up and having visible hairs by evening, is to put the scissors away (if you haven’t already) and use a nasal hair trimmer; these are good at a) trimming nasal hairs b) abstaining from trimming them too far back.
By all means shop around, but here’s an example product on Amazon, for your convenience!
- Note 1: despite the product description, please do not stick this in your ear (or any other orifice that’s not your nose, for the love of all that is holey)
- Note 2: we chose that one for a reason; the shape of the head prevents overtrimming.
- In contrast, we do not recommend this cheaper one that has a different shape head for a closer trim, which in this case, is not what we want.
Enjoy!
Share This Post

Sweet Potato & Black Bean Tacos
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fiber, protein, and polyphenols! What more could one ask for? Well, great taste and warm healthy goodness, which these deliver:
You will need
For the sweet potatoes:
- 2 medium sweet potatoes, cubed (we recommend leaving the skin on, but you can peel them if you really want to)
- 1 tbsp extra virgin olive oil
- 2 tsp garlic powder
- 2 tsp smoked paprika
- 1 tsp chili powder
- 1 tsp black pepper
- 1 tsp ground cumin
- 1 tsp ground turmeric
- ½ tsp MSG or 1 tsp low-sodium salt
For the black beans:
- 2 cans black beans, drained and rinsed (or 2 cups black beans that you cooked yourself)
- ¼ bulb garlic, minced
- 1 fresh jalapeño finely chopped (or ¼ cup jalapeños from a jar, finely chopped) ← adjust quantities per your preference and per the quality of the pepper(s) you’re using; we can’t judge that from here without tasting them, so we give a good basic starting suggestion.
- 2 tsp black pepper
- 1 tsp red chili flakes
- ½ tsp MSG or 1 tsp low-sodium salt
For serving:
- 8 small corn tortillas, or your preference if substituting
- 1 avocado, pitted, peeled, cubed, and tossed in lime juice ← we’re mentioning this here because you want to do this as soon as you cut it, to avoid oxidation
- Any other salad you’d like to include; fresh parsley is also a good option when it comes to greenery, or cilantro if you don’t have the soap gene
- Tomato salsa (quantity and spice level per your preference)
Method
(we suggest you read everything at least once before doing anything)
1) Preheat the oven to 400°F / 200°C.
2) Toss the sweet potato cubes in a large bowl with the rest of the ingredients from the sweet potato section above, ensuring they are evenly coated.
3) Bake them in the oven, on a baking tray lined with baking paper, for about 30 minutes or until tender inside and crispy at the edges. Turn them over halfway through.
4) While that’s happening, mix the black beans in a bowl with the other ingredients from the black bean section above, and heat them gently. You could do this in a saucepan, but honestly, while it’s not glamorous, the microwave is actually better for this. Note: many people find the microwave cooks food unevenly, but there are two reasons for this and they’re both easily fixable:
- instead of using high power for x minutes, use medium power for 2x minutes; this will produce better results
- instead of putting the food just in a bowl, jug, or similar, use a wide bowl or similar container, and then inside that, place a small empty microwave-safe glass jar or similar upturned in the middle, and then add the food around it, so that the food is arranged in a donut shape rather than a wide cylinder shape. This means there is no “middle bit” to go underheated while the edges are heated excessively; instead, it will heat through evenly.
If you really don’t want to do that though, use a saucepan on a very low heat, add a small amount of liquid (or tomato salsa), and stir constantly.
5) Heat the tortillas in a dry skillet for about 30 seconds each on each side, when ready to serve.
6) Assemble the tacos; you can do this how you like but a good order of operations is: tortilla, leafy salad (if using), potato, beans, non-leafy salad including avocado, salsa or other topping per your preference.

Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- White Potato vs Sweet Potato – Which is Healthier?
- Kidney Beans or Black Beans – Which is Healthier?
- Coconut vs Avocado – Which is Healthier?
- Glutathione: More Than An Antioxidant
- Our Top 5 Spices: How Much Is Enough For Benefits? ← we hit 4/5 today!
Take care!
Share This Post
Related Posts

Immunity – by Dr. William Paul
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This book gives a very person-centric (i.e., focuses on the contributions of named individuals) overview of advances in the field of immunology—up to its publication date in 2015. So, it’s not cutting edge, but it is very good at laying the groundwork for understanding more recent advances that occur as time goes by. After all, immunology is a field that never stands still.
We get a good grounding in how our immune system works (and how it doesn’t), the constant arms race between pathogens and immune responses, and the complexities of autoimmune disorders and—which is functionally in an overlapping category of disease—cancer. And, what advances we can expect soon to address those things.
Given the book was published 8 years ago, how did it measure up? Did we get those advances? Well, for the mostpart yes, we have! Some are still works in progress. But, we’ve also had obvious extra immunological threats in years since, which have also resulted in other advances along the way!
If the book has a downside, it’s that sometimes the author can be a little too person-centric. It’s engaging to focus on human characters, and helps us bring information to life; name-dropping to excess, along with awards won, can sometimes feel a little like the book was co-authored by Tahani Al-Jamil.
Nevertheless, it certainly does keep the book from getting too dry!
Bottom line: this book is a great overview of immunology and immunological research, for anyone who wants to understand these things better.
Click here to check out Immunity, and boost your knowledge of yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:

The Powerful Constraints on Medical Care in Catholic Hospitals Across America
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Nurse midwife Beverly Maldonado recalls a pregnant woman arriving at Ascension Saint Agnes Hospital in Maryland after her water broke. It was weeks before the baby would have any chance of survival, and the patient’s wishes were clear, she recalled: “Why am I staying pregnant then? What’s the point?” the patient pleaded.
But the doctors couldn’t intervene, she said. The fetus still had a heartbeat and it was a Catholic hospital, subject to the “Ethical and Religious Directives for Catholic Health Care Services” that prohibit or limit procedures like abortion that the church deems “immoral” or “intrinsically evil,” according to its interpretation of the Bible.
“I remember asking the doctors. And they were like, ‘Well, the baby still has a heartbeat. We can’t do anything,’” said Maldonado, now working as a nurse midwife in California, who asked them: “What do you mean we can’t do anything? This baby’s not going to survive.”
The woman was hospitalized for days before going into labor, Maldonado said, and the baby died.
Ascension declined to comment for this article.
The Catholic Church’s directives are often at odds with accepted medical standards, especially in areas of reproductive health, according to physicians and other medical practitioners.
The American College of Obstetricians and Gynecologists’ clinical guidelines for managing pre-labor rupture of membranes, in which a patient’s water breaks before labor begins, state that women should be offered options, including ending the pregnancy.
Maldonado felt her patient made her wishes clear.
“Under the ideal medical practice, that patient should be helped to obtain an appropriate method of terminating the pregnancy,” said Christian Pettker, a professor of obstetrics, gynecology, and reproductive sciences at the Yale School of Medicine, who helped author the guidelines.
He said, “It would be perfectly medically appropriate to do a termination of pregnancy before the cessation of cardiac activity, to avoid the health risks to the pregnant person.”
“Patients are being turned away from necessary care,” said Jennifer Chin, an OB-GYN at UW Medicine in Seattle, because of the “emphasis on these ethical and religious directives.”
They can be a powerful constraint on the care that patients receive at Catholic hospitals, whether emergency treatment when a woman’s health is at risk, or access to birth control and abortions.
More and more women are running into barriers to obtaining care as Catholic health systems have aggressively acquired secular hospitals in much of the country. Four of the 10 largest U.S. hospital chains by number of beds are Catholic, according to federal data from the Agency for Healthcare Research and Quality. There are just over 600 Catholic general hospitals nationally and roughly 100 more managed by Catholic chains that place some religious limits on care, a KFF Health News investigation reveals.
Maldonado’s experience in Maryland came just months before the Supreme Court’s ruling in 2022 to overturn Roe v. Wade, a decision that compounded the impact of Catholic health care restrictions. In its wake, roughly a third of states have banned or severely limited access to abortion, creating a one-two punch for women seeking to prevent pregnancy or to end one. Ironically, some states where Catholic hospitals dominate — such as Washington, Oregon, and Colorado — are now considered medical havens for women in nearby states that have banned abortion.
KFF Health News analyzed state-level birth data to discover that more than half a million babies are born each year in the U.S. in Catholic-run hospitals, including those owned by CommonSpirit Health, Ascension, Trinity Health, and Providence St. Joseph Health. That’s 16% of all hospital births each year, with rates in 10 states exceeding 30%. In Washington, half of all babies are born at such hospitals, the highest share in the country.
“We had many instances where people would have to get in their car to drive to us while they were bleeding, or patients who had had their water bags broken for up to five days or even up to a week,” said Chin, who has treated patients turned away by Catholic hospitals.
Physicians who turned away patients like that “were going against evidence-based care and going against what they had been taught in medical school and residency,” she said, “but felt that they had to provide a certain type of care — or lack of care — just because of the strength of the ethical and religious directives.”
Following religious mandates can be dangerous, Chin and other clinicians said.
When a patient has chosen to end a pregnancy after the amniotic sac — or water — has broken, Pettker said, “any delay that might be added to a procedure that is inevitably going to happen places that person at risk of serious, life-threatening complications,” including sepsis and organ infection.
Reporters analyzed American Hospital Association data as of August and used Catholic Health Association directories, news reports, government documents, and hospital websites and other materials to determine which hospitals are Catholic or part of Catholic systems, and gathered birth data from state health departments and hospital associations. They interviewed patients, medical providers, academic experts, advocacy organizations, and attorneys, and reviewed hundreds of pages of court and government records and guidance from Catholic health institutions and authorities to understand how the directives affect patient care.
Nationally, nearly 800,000 people have only Catholic or Catholic-affiliated birth hospitals within an hour’s drive, according to KFF Health News’ analysis. For example, that’s true of 1 in 10 North Dakotans. In South Dakota, it’s 1 in 20. When care is more than an hour away, academic researchers often define the area as a hospital desert. Pregnant women who must drive farther to a delivery facility are at higher risk of harm to themselves or their fetus, research shows.
Many Americans don’t have a choice — non-Catholic hospitals are too far to reach in an emergency or aren’t in their insurance networks. Ambulances may take patients to a Catholic facility without giving them a say. Women often don’t know that hospitals are affiliated with the Catholic Church or that they restrict reproductive care, academic research suggests.
And, in most of the country, state laws shield at least some hospitals from lawsuits for not performing procedures they object to on religious grounds, leaving little recourse for patients who were harmed because care was withheld. Thirty-five states prevent patients from suing hospitals for not providing abortions, including 25 states where abortion remains broadly legal. About half of those laws don’t include exceptions for emergencies, ectopic pregnancies, or miscarriages. Sixteen states prohibit lawsuits against hospitals for refusing to perform sterilization procedures.
“It’s hard for the ordinary citizen to understand, ‘Well, what difference does it make if my hospital is bought by this other big health system, as long as it stays open? That’s all I care about,’” said Erin Fuse Brown, who is the director of the Center for Law, Health & Society at Georgia State University and an expert in health care consolidation. Catholic directives also ban medical aid in dying for terminally ill patients.
People “may not realize that they’re losing access to important services, like reproductive health [and] end-of-life care,” she said.
‘Our Faith-Based Health Care Ministry’
After the Supreme Court ended the constitutional right to abortion in June 2022, Michigan resident Kalaina Sullivan wanted surgery to permanently prevent pregnancy.
Michigan voters in November that year enshrined the right to abortion under the state constitution, but the state’s concentration of Catholic hospitals means people like Sullivan sometimes still struggle to obtain reproductive health care.
Because her doctor worked for the Catholic chain Trinity Health, the nation’s fourth-largest hospital system, she had the surgery with a different doctor at North Ottawa Community Health System, an independent hospital near the shores of Lake Michigan.
Less than two months later, that, too, became a Catholic hospital, newly acquired by Trinity.
To mark the transition, Cory Mitchell, who at the time was the mission leader of Trinity Health Muskegon, stood before his new colleagues and offered a blessing.
“The work of your hands is what makes our faith-based health care ministry possible,” he said, according to a video of the ceremony Trinity Health provided to KFF Health News. “May these hands continue to bring compassion, compassion and healing, to all those they touch.”
Trinity Health declined to answer detailed questions about its merger with North Ottawa Community Health System and the ethical and religious directives. “Our commitment to high-quality, compassionate care means informing our patients of all appropriate care options, and trusting and supporting our physicians to make difficult and medically necessary decisions in the best interest of their patients’ health and safety,” spokesperson Jennifer Amundson said in an emailed statement. “High-quality, safe care is critical for the women in our communities and in cases where a non-critical service is not available at our facility, the physician will transfer care as appropriate.”
Leaders in Catholic-based health systems have hammered home the importance of the church’s directives, which are issued by the U.S. Conference of Catholic Bishops, all men, and were first drafted in 1948. The essential view on abortion is as it was in 1948. The last revision, in 2018, added several directives addressing Catholic health institution acquisitions or mergers with non-Catholic ones, including that “whatever comes under control of the Catholic institution — whether by acquisition, governance, or management — must be operated in full accord with the moral teaching of the Catholic Church.”
“While many of the faithful in the local church may not be aware of these requirements for Catholic health care, the local bishop certainly is,” wrote Sister Doris Gottemoeller, a former board member of the Bon Secours Mercy Health system, in a 2023 Catholic Health Association journal article. “In fact, the bishop should be briefed on a regular basis about the hospital’s activities and strategies.”
Now, for care at a non-Catholic hospital, Sullivan would need to travel nearly 30 miles.
“I don’t see why there’s any reason for me to have to follow the rules of their religion and have that be a part of what’s going on with my body,” she said.
Risks Come With Religion
Nathaniel Hibner, senior director of ethics at the Catholic Health Association, said the ethical and religious directives allow clinicians to provide medically necessary treatments in emergencies. In a pregnancy crisis when a person’s life is at risk, “I do not believe that the ERDs should restrict the physician in acting in the way that they see medically indicated.”
“Catholic health care is committed to the health of all women and mothers who enter into our facilities,” Hibner said.
The directives permit care to cure “a proportionately serious pathological condition of a pregnant woman” even if it would “result in the death of the unborn child.” Hibner demurred when asked who defines what that means and when such care is provided, saying, “for the most part, the physician and the patients are the ones that are having a conversation and dialogue with what is supposed to be medically appropriate.”
It is common for practitioners at any hospital to consult an ethics board about difficult cases — such as whether a teenager with cancer can decline treatment. At Catholic hospitals, providers must ask a board for permission to perform procedures restricted by the religious directives, clinicians and researchers say. For example, could an abortion be performed if a pregnancy threatened the mother’s life?
How and when an ethics consultation occurs depends on the hospital, Hibner said. “That ethics consultation can be initiated by anyone involved in the direct care of that situation — the patient, the surrogate of that patient, the physician, the nurse, the social worker all have the ability to request a consultation,” he said. When asked whether a consultation with an ethics board can occur without a request, he said “sometimes it could.”
How strictly directives are followed can depend on the hospital and the views of the local bishop.
“If the hospital has made a difficult decision about a critical pregnancy or an end-of-life care situation, the bishop should be the first to know about it,” Gottemoeller wrote.
In an interview, Gottemoeller said that even when pregnancy termination decisions are made on sound ethical grounds, not informing the bishop puts him in a bad position and hurts the church. “If there’s a possibility of it being misunderstood, or misinterpreted, or criticized,” Gottemoeller said, the bishop should understand what happened and why “before the newspapers call him and ask him for an opinion.”
“And if he has to say, ‘Well, I think you made a mistake,’ well, all right,” she said. “But don’t let him be blindsided. I mean, we’re one church and the bishop has pastoral concern over everything in his diocese.”
Katherine Parker Bryden, a nurse midwife in Iowa who works for MercyOne, said she regularly tells pregnant patients that the hospital cannot perform tubal sterilization surgery, to prevent future pregnancies, or refer patients to other hospitals that do. MercyOne is one of the largest health systems in Iowa. Nearly half of general hospitals in the state are Catholic or Catholic-affiliated — the highest share among all states.
The National Catholic Bioethics Center, an ethics authority for Catholic health institutions, has said that referrals for care that go against church teaching would be “immoral.”
“As providers, you’re put in this kind of moral dilemma,” Parker Bryden said. “Am I serving my patients or am I serving the archbishop and the pope?”
In response to questions, MercyOne spokesperson Eve Lederhouse said in an email that its providers “offer care and services that are consistent with the guidelines of a Catholic health system.”
Maria Rodriguez, an OB-GYN professor at Oregon Health & Science University, said that as a resident in the early 2000s at a Catholic hospital she was able to secure permission — what she calls a “pope note” — to sterilize some patients with conditions such as gestational diabetes.
Annie Iriye, a retired OB-GYN in Washington state, said that more than a decade ago she sought permission to administer medication to hasten labor for a patient experiencing a second-trimester miscarriage at a Catholic hospital. She said she was told no because the fetus had a heartbeat. The patient took 10 hours to deliver — time that would have been cut by half, Iriye said, had she been able to follow her own medical training and expertise. During that time, she said, the patient developed an infection.
Iriye and Chin were part of an effort by reproductive rights groups and medical organizations that pushed for a state law to protect physicians if they act against Catholic hospital restrictions. The bill, which Washington enacted in 2021, was opposed by the Washington State Hospital Association, whose membership includes multiple large Catholic health systems.
State lawmakers in Oregon in 2021 enacted legislation that beefed up powers to reject health care mergers if they would reduce access to the types of care constrained by Catholic directives. The hospital lobby has sued to block the statute. Washington state lawmakers introduced similar legislation last year, which the hospital association opposes.
Hibner said Catholic hospitals are committed to instituting systemic changes that improve maternal and child health, including access to primary, prenatal, and postpartum care. “Those are the things that I think rural communities really need support and advocacy for,” he said.
Maldonado, the nurse midwife, still thinks of her patient who was forced to stay pregnant with a baby who could not survive. “To feel like she was going to have to fight to have an abortion of a baby that she wanted?” Maldonado said. “It was just horrible.”
KFF Health News data editor Holly K. Hacker contributed to this report.
Click to open the methodology Methodology
By Hannah Recht
KFF Health News identified areas of the country where patients have only Catholic hospital options nearby. The “Ethical and Religious Directives for Catholic Health Care Services” — which are issued by the U.S. Conference of Catholic Bishops, all men — dictate how patients receive reproductive care at Catholic health facilities. In our analysis, we focused on hospitals where babies are born.
We constructed a national database of hospital locations, identified which ones are Catholic or Catholic-affiliated, found how many babies are born at each, and calculated how many people live near those hospitals.
Hospital Universe
We identified hospitals in the 50 states and the District of Columbia using the American Hospital Association database from August 2023. We removed hospitals that had closed or were listed more than once, added hospitals that were not included, and corrected inaccurate or out-of-date information about ownership, primary service type, and location. We excluded federal hospitals, such as military and Indian Health Service facilities, because they are not open to everyone.
Catholic Affiliation
To identify Catholic hospitals, we used the Catholic Health Association’s member directory. We also counted as Catholic a handful of hospitals that are not part of this voluntary membership group but explicitly follow the Ethical and Religious Directives, according to their mission statements, websites, or promotional materials.
We also tracked Catholic-affiliated hospitals: those that are owned or managed by a Catholic health system, such as CommonSpirit Health or Trinity Health, and are influenced by the religious directives but do not necessarily adhere to them in full. To identify Catholic-affiliated hospitals, we consulted health system and hospital websites, government documents, and news reports.
We combined both Catholic and Catholic-affiliated hospitals for analysis, in line with previous research about the influence of Catholic directives on health care.
Births
To determine the share of births that occur at Catholic or Catholic-affiliated hospitals, we gathered the latest annual number of births by hospital from state health departments. Where recent data was not publicly available, we submitted records requests for the most recent complete year available.
The resulting data covered births in 2022 for nine states and D.C., births in 2021 for 23 states, births in 2020 for nine states, and births in 2019 for one state. We used data from the 2021 American Hospital Association survey, the latest available at the time of analysis, for the eight remaining states that did not provide birth data in response to our requests. A small number of hospitals have recently opened or closed labor and delivery units. The vast majority of the rest record about the same number of births each year. This means that the results would not be substantially different if data from 2023 were available.
We used this data to calculate the number of babies born in Catholic and Catholic-affiliated hospitals, as well as non-Catholic hospitals by state and nationally.
We used hospitals’ Catholic status as of August 2023 in this analysis. In 10 cases where the hospital had already closed, we used Catholic status at the time of the closure.
Because our analysis focuses on hospital care, we excluded births that occurred in non-hospital settings, such as homes and stand-alone birth centers, as well as federal hospitals.
Several states suppressed data from hospitals with fewer than 10 births due to privacy restrictions. Because those numbers were so low, this suppression had a negligible effect on state-level totals.
Drive-Time Analysis
We obtained hospitals’ geographic coordinates based on addresses in the AHA dataset using HERE’s geocoder. For addresses that could not be automatically geocoded with a high degree of certainty, we verified coordinates manually using hospital websites and Google Maps.
We calculated the areas within 30, 60, and 90 minutes of travel time from each birth hospital that was open in August 2023 using tools from HERE. We included only hospitals that had 10 or more births as a proxy for hospitals that have labor and delivery units, or where births regularly occur.
The analysis focused on the areas with hospitals within an hour’s drive. Researchers often define hospital deserts as places where one would have to drive an hour or more for hospital care. (For example: [1] “Disparities in Access to Trauma Care in the United States: A Population-Based Analysis,” [2] “Injury-Based Geographic Access to Trauma Centers,” [3] “Trends in the Geospatial Distribution of Inpatient Adult Surgical Services Across the United States,” [4] “Access to Trauma Centers in the United States.”)
We combined the drive-time areas to see which areas of the United States have only Catholic or Catholic-affiliated birth hospitals nearby, both Catholic and non-Catholic, non-Catholic only, or none. We then joined these areas to the 2021 census block group shapefile from IPUMS NHGIS and removed water bodies using the U.S. Geological Survey’s National Hydrography Dataset to calculate the percentage of each census block group that falls within each hospital access category. We calculated the number of people in each area using the 2021 “American Community Survey” block group population totals. For example, if half of a block group’s land area had access to only Catholic or Catholic-affiliated hospitals, then half of the population was counted in that category.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:

The Checklist Manifesto – by Dr. Atul Gawande
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Gawande, himself a general surgeon, uses checklists a lot. He is, unequivocally, an expert in his field. He “shouldn’t” need a checklist to tell him to do such things as “Check you have the correct patient”. But checklists are there as a safety net. And, famously, “safety regulations are written in blood”, after all.
And, who amongst us has never made such a “silly” error? From forgetting to turn the oven on, to forgetting to take the handbrake off, it takes only a momentary distraction to think we’ve done something we haven’t.
You may be wondering: why a whole book on this? Is it just many examples of the usefulness of checklists? Because I’m already sold on that, so, what else am I going to get out of it?
Dr. Gawande also explains in clear terms:
- How to optimize “all necessary steps” with “as few steps as possible”
- The important difference between read-do checklists and do-confirm checklists
- To what extent we should try to account for the unexpected
- How to improve compliance (i.e., making sure you actually use it, no matter how tempting it will be to go “yeah this is automatic for me now” and gloss over it)
- The role of checklists in teams, and in passing on knowledge
…and more.
Bottom line: if you’ve ever tried to make tea without putting the tea-leaves in the pot, this is the book that will help you avoid making more costly mistakes—whatever your area of activity or interest.
Click here to check out the Checklist Manifesto, and make fewer mistakes!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: