Easing Lower Back Pain
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Lower back pain often originates from an unexpected culprit: your pelvis. Similar to how your psoas can contribute to lower back pain, when your pelvis tilts forward due to tight hip flexors, it can misalign your spine, leading to discomfort and pain. As WeShape shows us in the below video, one simple stretch can help realign your pelvis and significantly ease lower back pain.
Why Your Pelvis Matters
Sitting for long periods causes your hip flexors to shorten, leading to an anterior pelvic tilt. This forward tilt puts pressure on your spine and SI joint, causing pain and discomfort in the lower back. To help resolve this, you can work on correcting your pelvic alignment, helping to significantly reduce this pressure and alleviate related pain. And no, this doesn’t require any spinal cord stimulation.
Easy Variations for All
A lot of you recognise the stretch in this video; it’s quite a well-known kneeling stretch. But, unlike other guides, WeShape also provides a fantastic variation for those who aren’t mobile enough for the kneeling variation
So, if you can’t comfortably get down on the ground, WeShape outlines a brilliant standing variation. So, regardless of your mobility, there’s an option for you!
See both variations here:
Excited to reduce your lower back pain? We hope so! Let us know if you have any tips that you’d like to share with us.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
I’ve recovered from a cold but I still have a hoarse voice. What should I do?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Cold, flu, COVID and RSV have been circulating across Australia this winter. Many of us have caught and recovered from one of these common upper respiratory tract infections.
But for some people their impact is ongoing. Even if your throat isn’t sore anymore, your voice may still be hoarse or croaky.
So what happens to the voice when we get a virus? And what happens after?
Here’s what you should know if your voice is still hoarse for days – or even weeks – after your other symptoms have resolved.
Why does my voice get croaky during a cold?
A healthy voice is normally clear and strong. It’s powered by the lungs, which push air past the vocal cords to make them vibrate. These vibrations are amplified in the throat and mouth, creating the voice we hear.
The vocal cords are two elastic muscles situated in your throat, around the level of your laryngeal prominence, or Adam’s apple. (Although everyone has one, it tends to be more pronounced in males.) The vocal cords are small and delicate – around the size of your fingernail. Any small change in their structure will affect how the voice sounds.
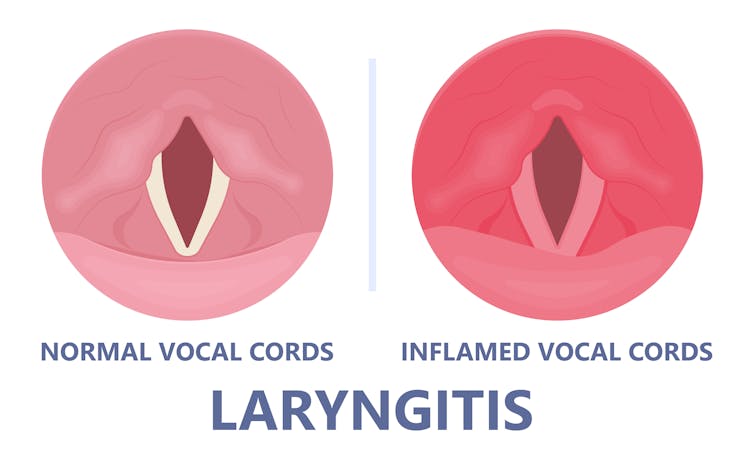
When the vocal cords become inflamed – known as laryngitis – your voice will sound different. Laryngitis is a common part of upper respiratory tract infections, but can also be caused through misuse.
Viruses such as the common cold can inflame the vocal cords. Pepermpron/Shutterstock Catching a virus triggers the body’s defence mechanisms. White blood cells are recruited to kill the virus and heal the tissues in the vocal cords. They become inflamed, but also stiffer. It’s harder for them to vibrate, so the voice comes out hoarse and croaky.
In some instances, you may find it hard to speak in a loud voice or have a reduced pitch range, meaning you can’t go as high or loud as normal. You may even “lose” your voice altogether.
Coughing can also make things worse. It is the body’s way of trying to clear the airways of irritation, including your own mucus dripping onto your throat (post-nasal drip). But coughing slams the vocal cords together with force.
Chronic coughing can lead to persistent inflammation and even thicken the vocal cords. This thickening is the body trying to protect itself, similar to developing a callus when a pair of new shoes rubs.
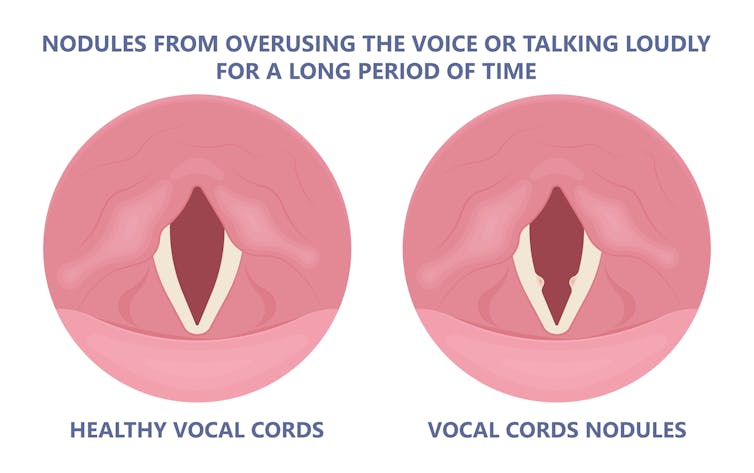
Thickening on your vocal cords can lead to physical changes in the vocal cords – such as developing a growth or “nodule” – and further deterioration of your voice quality.
Coughing and exertion can cause inflamed vocal cords to thicken and develop nodules. Pepermpron/Shutterstock How can you care for your voice during infection?
People who use their voices a lot professionally – such as teachers, call centre workers and singers – are often desperate to resume their vocal activities. They are more at risk of forcing their voice before it’s ready.
The good news is most viral infections resolve themselves. Your voice is usually restored within five to ten days of recovering from a cold.
Occasionally, your pharmacist or doctor may prescribe cough suppressants to limit additional damage to the vocal cords (among other reasons) or mucolytics, which break down mucus. But the most effective treatments for viral upper respiratory tract infections are hydration and rest.
Drink plenty of water, avoid alcohol and exposure to cigarette smoke. Inhaling steam by making yourself a cup of hot water will also help clear blocked noses and hydrate your vocal cords.
Rest your voice by talking as little as possible. If you do need to talk, don’t whisper – this strains the muscles.
Instead, consider using “confidential voice”. This is a soft voice – not a whisper – that gently vibrates your vocal cords but puts less strain on your voice than normal speech. Think of the voice you use when communicating with someone close by.
During the first five to ten days of your infection, it is important not to push through. Exerting the voice by talking a lot or loudly will only exacerbate the situation. Once you’ve recovered from your cold, you can speak as you would normally.
What should you do if your voice is still hoarse after recovery?
If your voice hasn’t returned to normal after two to three weeks, you should seek medical attention from your doctor, who may refer you to an ear nose and throat specialist.
If you’ve developed a nodule, the specialist would likely refer you to a speech pathologist who will show you how to take care of your voice. Many nodules can be treated with voice therapy and don’t require surgery.
You may have also developed a habit of straining your vocal cords, if you forced yourself to speak or sing while they were inflamed. This can be a reason why some people continue to have a hoarse voice even when they’ve recovered from the cold.
In those cases, a speech pathologist may play a valuable role. They may teach you to exercises that make voicing more efficient. For example, lip trills (blowing raspberries) are a fun and easy way you can learn to relax the voice. This can help break the habit of straining your voice you may have developed during infection.
Yeptain Leung, Postdoctoral Research and Lecturer of Speech Pathology, School of Health Sciences, The University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Chiropractors have been banned again from manipulating babies’ spines. Here’s what the evidence actually says
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Chiropractors in Australia will not be able to perform spinal manipulation on children under the age of two once more, following health concerns from doctors and politicians.
But what is the spinal treatment at the centre of the controversy? Does it work? Is there evidence of harm?
We’re a team of researchers who specialise in evidence-based musculoskeletal health. I (Matt) am a registered chiropractor, Joshua is a registered physiotherapist and Giovanni trained as a physiotherapist.
Here’s what the evidence says.
Dmitry Naumov/Shutterstock Remind me, how did this all come about?
A Melbourne-based chiropractor posted a video on social media in 2018 using a spring-loaded device (known as the Activator) to manipulate the spine of a two-week-old baby suspended upside down by the ankles.
The video sparked widespread concerns among the public, medical associations and politicians. It prompted a ban on the procedure in young children. The Victorian health minister commissioned Safer Care Victoria to conduct an independent review of spinal manipulation techniques on children.
Recently, the Chiropractic Board of Australia reinstated chiropractors’ authorisation to perform spinal manipulation on babies under two years old. But this week, it backflipped, following heavy criticism from medical associations and politicians.
What is spinal manipulation?
Spinal manipulation is a treatment used by chiropractors and other health professionals such as doctors, osteopaths and physiotherapists.
It is an umbrella term that includes popular “back cracking” techniques.
It also includes more gentle forms of treatment, such as massage or joint mobilisations. These involve applying pressure to joints without generating a “cracking” sound.
Does spinal manipulation in babies work?
Several international guidelines for health-care professionals recommend spinal manipulation to treat adults with conditions such as back pain and headache as there is an abundance of evidence on the topic. For example, spinal manipulation for back pain is supported by data from nearly 10,000 adults.
For children, it’s a different story. Safer Care Victoria’s 2019 review of spinal manipulation found very few studies testing whether this treatment was safe and effective in children.
Studies were generally small and were of poor quality. Some of those small, poor-quality studies, suggest spinal manipulation provides a very small benefit for back pain, colic and potentially bedwetting – some common reasons for parents to take their child to see a chiropractor. But overall, the review found the overall body of evidence was very poor.
Spinal manipulation doesn’t seem to help young children with an ear infection. MIA Studio/Shutterstock However, for most other children’s conditions chiropractors treat – such as headache, asthma, otitis media (a type of ear infection), cerebral palsy, hyperactivity and torticollis (“twisted neck”) – there did not appear to be a benefit.
The number of studies investigating the effectiveness of spinal manipulation on babies under two years of age was even smaller.
There was one high-quality study and two small, poor quality studies. These did not show an appreciable benefit of spinal manipulation on colic, otitis media with effusion (known as glue ear) or twisted neck in babies.
Is spinal manipulation on babies safe?
In terms of safety, most studies in the review found serious complications were extremely rare. The review noted one baby or child dying (a report from Germany in 2001 after spinal manipulation by a physiotherapist). The most common complications were mild in nature such as increased crying and soreness.
However, because studies were very small, they cannot tell us anything about the safety of spinal manipulation in a reliable way. Studies that are designed to properly investigate if a treatment is safe typically include thousands of patients. And these studies have not yet been done.
Why do people see chiropractors?
Safer Care Victoria also conducted surveys with more than 20,000 people living in Australia who had taken their children under 12 years old to a chiropractor in the past ten years.
Nearly three-quarters said that was for treatment of a child aged two years or younger.
Nearly all people surveyed reported a positive experience when they took their child to a chiropractor and reported that their child’s condition improved with chiropractic care. Only a small number of people (0.3%) reported a negative experience, and this was mostly related to cost of treatment, lack of improvement in their child’s condition, excessive use of x-rays, and perceived pressure to avoid medications.
Many of the respondents had also consulted their GP or maternity/child health nurse.
What now for spinal manipulation in children?
At the request of state and federal ministers, the Chiropractic Board of Australia confirmed that spinal manipulation on babies under two years old will continue to be banned until it discusses the issue further with health ministers.
Many chiropractors believe this is unfair, especially considering the strong consumer support for chiropractic care outlined in the Safer Care Victoria report, and the rarity of serious reported harms in children.
Others believe that in the absence of evidence of benefit and uncertainty around whether spinal manipulation is safe in children and babies, the precautionary principle should apply and children and babies should not receive spinal manipulation.
Ultimately, high quality research is urgently needed to better understand whether spinal manipulation is beneficial for the range of conditions chiropractors provide it for, and whether the benefit outweighs the extremely small chance of a serious complication.
This will help parents make an informed choice about health care for their child.
Matt Fernandez, Senior lecturer and researcher in chiropractic, CQUniversity Australia; Giovanni E. Ferreira, NHMRC Emerging Leader Research Fellow, Institute of Musculoskeletal Health, University of Sydney, and Joshua Zadro, NHMRC Emerging Leader Research Fellow, Sydney Musculoskeletal Health, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Ruminating vs Processing
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
When it comes to traumatic experiences, there are two common pieces of advice for being able to move forwards functionally:
- Process whatever thoughts and feelings you need to process
- Do not ruminate
The latter can seem, at first glance, a lot like the former. So, how to tell them apart, and how to do one without the other?
Getting tense
One major difference between the two is the tense in which our mental activity takes place:
- processing starts with the traumatic event (or perhaps even the events leading up to the traumatic event), analyses what happened and if possible why, and then asks the question “ok, what now?” and begins work on laying out a path for the future.
- rumination starts with the traumatic event (or perhaps even the events leading up to the traumatic event), analyses what happened and if why, oh why oh why, “I was such an idiot, if only I had…” and gets trapped in a fairly tight (and destructive*) cycle of blame and shame/anger, never straying far from the events in question.
*this may be directly self-destructive, but it can also sometimes be only indirectly self-destructive, for example if the blame and anger is consciously placed with someone else.
This idea fits in, by the way, with Dr. Elisabeth Kübler-Ross’s “five stages of grief” model; rumination here represents the stages “bargaining”, “despair”, and “anger”, while emotional processing here represents the stage “acceptance”. Thus, it may be that rumination does have a place in the overall process—just don’t get stuck there!
For more on healthily processing grief specifically:
What Grief Does To The Body (And How To Manage It)
Grief, by the way, can be about more than the loss of a loved one; a very similar process can play out with many other kinds of unwanted life changes too.
What are the results?
Another way to tell them apart is to look at the results of each. If you come out of a long rumination session feeling worse than when you started, it’s highly unlikely that you just stopped too soon and were on the verge of some great breakthrough. It’s possible! But not likely.
- Processing may be uncomfortable at first, and if it’s something you’ve ignored for a long time, that could be very uncomfortable at first, but there should quite soon be some “light at the end of the tunnel”. Perhaps not even because a solution seems near, but because your mind and body recognize “aha, we are doing something about it now, and thus may find a better way forward”.
- Rumination tends to intensify and prolong uncomfortable emotions, increases stress and anxiety, and likely disrupts sleep. At best, it may serve as a tipping point to seek therapy or even just recognize “I should figure out a way to deal with this, because this isn’t doing me any good”. At worst, it may serve as a tipping point to depression, and/or substance abuse, and/or suicidality.
See also: How To Stay Alive (When You Really Don’t Want To) ← which also has a link back to our article on managing depression, by the way!
Did you choose it, really?
A third way to tell them apart is the level of conscious decision that went into doing it.
- Processing is almost always something that one decides “ok, let’s figure this out”, and sits down to figure it out.
- Rumination tends to be about as voluntary as social media doomscrolling. Technically we may have decided to begin it (we also might not have made any conscious decision, and just acted on impulse), but let’s face it, our hands weren’t at the wheel for long, at all.
A good way to make sure that it is a conscious process, is to schedule time for it in advance, and then do it only during that time. If thoughts about it come up at other times, tell yourself “no, leave that for later”, and then deal with it when (and only when) the planned timeslot arrives.
It’s up to you and your schedule what time you pick, but if you’re unsure, consider an hour in the early evening. That means that the business of the day is behind you, but it’s also not right before bed, so you should have some decompression time as a buffer. So for example, perhaps after dinner you might set a timer* for an hour, and sit down to journal, brainstorm, or just plain think, about the matter that needs processing.
*electronic timers can be quite jarring, and may distract you while waiting for the beeps. So, consider investing in a relaxing sand timer like this one instead.
Is there any way to make rumination less bad?
As we mentioned up top, there’s a case to be made for “rumination is an early part of the process that gets us where we need to go, and may not be skippable, or may not be advisable to skip”.
So, if you are going to ruminate, then firstly, we recommend again bordering it timewise (with a timer as above) and having a plan to pull yourself out when you’re done rather than getting stuck there (such as: The Off-Button For Your Brain: How To Stop Negative Thought Spirals).
And secondly, you might want to consider the following technique, which allows one to let one’s brain know that the thing we’re thinking about / imagining is now to be filed away safely; not lost or erased, but sent to the same place that nightmares go after we wake up:
A Surprisingly Powerful Tool: Eye Movement Desensitization & Reprocessing (EMDR)
What if I actually do want to forget?
That’s not usually recommendable; consider talking it through with a therapist first. However, for your interest, there is a way:
The Dark Side Of Memory (And How To Forget)
Take care!
Share This Post
Related Posts
-
Do You Know These 10 Common Ovarian Cancer Symptoms?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s better to know in advance:
Things you may need to know
The symptoms listed in the video are:
- Abdominal bloating: persistent bloating due to fluid buildup, often mistaken for overeating or weight gain.
- Pelvic or abdominal pain: continuous pain in the lower abdomen or pelvis, unrelated to menstruation.
- Difficulty eating or feeling full quickly: loss of appetite or feeling full after eating only a small amount.
- Urgent or frequent urination: increased need to urinate due to tumor pressure on the bladder.
- Unexplained weight loss: sudden weight loss without changes in diet or exercise (this goes for cancer in general, of course).
- Fatigue: extreme tiredness that doesn’t improve with rest, possibly linked to anemia.
- Back pain: persistent lower back pain due to tumor pressure or fluid buildup.
- Changes in bowel habits: unexplained constipation, diarrhea, or a feeling of incomplete bowel movements.
- Menstrual changes: irregular, heavier, lighter, or missed periods in premenopausal women.
- Pain during intercourse: discomfort or deep pelvic pain during or after vaginal sex—often overlooked!
Of course, some of those things can be caused by many things, but it’s worth getting it checked out, especially if you have a cluster of them together. Even if it’s not ovarian cancer (and hopefully it won’t be), having multiple things from this list certainly means that “something wrong is not right” in any case.
For those who remember better from videos than what you read, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Take care
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Ouch. That ‘Free’ Annual Checkup Might Cost You. Here’s Why.
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
When Kristy Uddin, 49, went in for her annual mammogram in Washington state last year, she assumed she would not incur a bill because the test is one of the many preventive measures guaranteed to be free to patients under the 2010 Affordable Care Act. The ACA’s provision made medical and economic sense, encouraging Americans to use screening tools that could nip medical problems in the bud and keep patients healthy.
So when a bill for $236 arrived, Uddin — an occupational therapist familiar with the health care industry’s workings — complained to her insurer and the hospital. She even requested an independent review.
“I’m like, ‘Tell me why am I getting this bill?’” Uddin recalled in an interview. The unsatisfying explanation: The mammogram itself was covered, per the ACA’s rules, but the fee for the equipment and the facility was not.
That answer was particularly galling, she said, because, a year earlier, her “free” mammogram at the same health system had generated a bill of about $1,000 for the radiologist’s reading. Though she fought that charge (and won), this time she threw in the towel and wrote the $236 check. But then she dashed off a submission to the KFF Health News-NPR “Bill of the Month” project:
“I was really mad — it’s ridiculous,” she later recalled. “This is not how the law is supposed to work.”
The ACA’s designers might have assumed that they had spelled out with sufficient clarity that millions of Americans would no longer have to pay for certain types of preventive care, including mammograms, colonoscopies, and recommended vaccines, in addition to doctor visits to screen for disease. But the law’s authors didn’t reckon with America’s ever-creative medical billing juggernaut.
Over the past several years, the medical industry has eroded the ACA’s guarantees, finding ways to bill patients in gray zones of the law. Patients going in for preventive care, expecting that it will be fully covered by insurance, are being blindsided by bills, big and small.
The problem comes down to deciding exactly what components of a medical encounter are covered by the ACA guarantee. For example, when do conversations between doctor and patient during an annual visit for preventive services veer into the treatment sphere? What screenings are needed for a patient’s annual visit?
A healthy 30-year-old visiting a primary care provider might get a few basic blood tests, while a 50-year-old who is overweight would merit additional screening for Type 2 diabetes.
Making matters more confusing, the annual checkup itself is guaranteed to be “no cost” for women and people age 65 and older, but the guarantee doesn’t apply for men in the 18-64 age range — though many preventive services that require a medical visit (such as checks of blood pressure or cholesterol and screens for substance abuse) are covered.
No wonder what’s covered under the umbrella of prevention can look very different to medical providers (trying to be thorough) and billers (intent on squeezing more dollars out of every medical encounter) than it does to insurers (who profit from narrower definitions).
For patients, the gray zone has become a billing minefield. Here are a few more examples, gleaned from the Bill of the Month project in just the past six months:
Peter Opaskar, 46, of Texas, went to his primary care doctor last year for his preventive care visit — as he’d done before, at no cost. This time, his insurer paid $130.81 for the visit, but he also received a perplexing bill for $111.81. Opaskar learned that he had incurred the additional charge because when his doctor asked if he had any health concerns, he mentioned that he was having digestive problems but had already made an appointment with his gastroenterologist. So, the office explained, his visit was billed as both a preventive physical and a consultation. “Next year,” Opasker said in an interview, if he’s asked about health concerns, “I’ll say ‘no,’ even if I have a gunshot wound.”
Kevin Lin, a technology specialist in Virginia in his 30s, went to a new primary care provider to take advantage of the preventive care benefit when he got insurance; he had no physical complaints. He said he was assured at check-in that he wouldn’t be charged. His insurer paid $174 for the checkup, but he was billed an additional $132.29 for a “new patient visit.” He said he has made many calls to fight the bill, so far with no luck.
Finally, there’s Yoori Lee, 46, of Minnesota, herself a colorectal surgeon, who was shocked when her first screening colonoscopy yielded a bill for $450 for a biopsy of a polyp — a bill she knew was illegal. Federal regulations issued in 2022 to clarify the matter are very clear that biopsies during screening colonoscopies are included in the no-cost promise. “I mean, the whole point of screening is to find things,” she said, stating, perhaps, the obvious.
Though these patient bills defy common sense, room for creative exploitation has been provided by the complex regulatory language surrounding the ACA. Consider this from Ellen Montz, deputy administrator and director of the Center for Consumer Information and Insurance Oversight at the Centers for Medicare & Medicaid Services, in an emailed response to queries and an interview request on this subject: “If a preventive service is not billed separately or is not tracked as individual encounter data separately from an office visit and the primary purpose of the office visit is not the delivery of the preventive item or service, then the plan issuer may impose cost sharing for the office visit.”
So, if the doctor decides that a patient’s mention of stomach pain does not fall under the umbrella of preventive care, then that aspect of the visit can be billed separately, and the patient must pay?
And then there’s this, also from Montz: “Whether a facility fee is permitted to be charged to a consumer would depend on whether the facility usage is an integral part of performing the mammogram or an integral part of any other preventive service that is required to be covered without cost sharing under federal law.”
But wait, how can you do a mammogram or colonoscopy without a facility?
Unfortunately, there is no federal enforcement mechanism to catch individual billing abuses. And agencies’ remedies are weak — simply directing insurers to reprocess claims or notifying patients they can resubmit them.
In the absence of stronger enforcement or remedies, CMS could likely curtail these practices and give patients the tools to fight back by offering the sort of clarity the agency provided a few years ago regarding polyp biopsies — spelling out more clearly what comes under the rubric of preventive care, what can be billed, and what cannot.
The stories KFF Health News and NPR receive are likely just the tip of an iceberg. And while each bill might be relatively small compared with the stunning $10,000 hospital bills that have become all too familiar in the United States, the sorry consequences are manifold. Patients pay bills they do not owe, depriving them of cash they could use elsewhere. If they can’t pay, those bills might end up with debt-collection agencies and, ultimately, harm their credit score.
Perhaps most disturbing: These unexpected bills might discourage people from seeking preventive screenings that could be lifesaving, which is why the ACA deemed them “essential health benefits” that should be free.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
10 Lessons For A Healthy Mind & Body
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sadia Badiei, food scientist of “Pick Up Limes” culinary fame, has advice in and out of the kitchen:
Pick up a zest for life
Here’s what she picked up, and we all can too:
- “I can’t do it… yet”: it’s never too late to adopt a growth mindset by adding “yet” to your self-doubt, focusing on progress and the possibility of improvement.
- The spotlight effect: people are generally too absorbed in their own lives to focus on you, so don’t worry too much about others’ perceptions.
- Nutrition by addition: focus on adding healthier foods to your diet rather than eliminating the less healthy ones to avoid restrictive mindsets. You can still eliminate the less healthy ones if you want to! It just shouldn’t be the primary focus. Focusing on a conceptually negative thing is rarely helpful.
- It’s ok to change: embrace change as a sign of growth and evolution, rather than seeing it as a failure or waste of time.
- The way you do one thing is the way you do everything: be mindful of how you approach small tasks, regular tasks, boring tasks, unwanted tasks—you can either create a habit of enthusiasm or a habit of suffering (it’s entirely your choice which)
- Setting goals for success: set goals based on actions you can control (inputs) rather than outcomes that are uncertain. Less “lose 10 lbs”, and more “eat fiber before starch”, for example.
- You probably can’t have it all at once: you can achieve all your dreams, but often not simultaneously; goals and desires unfold in stages over time.
- The five-year rule: before adopting a new lifestyle or habit, ask yourself if you can realistically sustain it for five years to ensure it’s not just a short-term fix. If you struggle with this prognostic, look backwards first instead. Which healthy habits have you maintained for decades, and which were you never able to make stick?
- Are you afraid or excited?: reframe fear as excitement, as both emotions share similar physical sensations and signify that you care about the outcome.
- The voice you hear most: speak kindly to yourself in self-talk to create a softer, more compassionate tone. Your subconscious is always listening, so reinforce healthy rather than unhealthy thought patterns.
For more on each of these, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
80-Year-Olds Share Their Biggest Regrets
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: