What you need to know about PCOS
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In 2008, microbiologist Sasha Ottey saw her OB-GYN because she had missed some periods. The doctor ran blood tests and gave her an ultrasound, diagnosing her with polycystic ovary syndrome (PCOS). She also told her not to worry, referred her to an endocrinologist (a doctor who specializes in hormones), and told her to come back when she wanted to get pregnant.
“I found [that] quite dismissive because that was my reason for presenting to her,” Ottey tells PGN. “I felt that she was missing an opportunity to educate me on PCOS, and that was just not an accurate message: Missing periods can lead to other serious, life-threatening health conditions.”
During the consultation with the endocrinologist, Ottey was told to lose weight and come back in six months. “Again, I felt dismissed and left up to my own devices to understand this condition and how to manage it,” she says.
Following that experience, Ottey began researching and found that thousands of people around the world had similar experiences with their PCOS diagnoses, which led her to start and lead the advocacy and support organization PCOS Challenge.
PCOS is the most common hormonal condition affecting people with ovaries of reproductive age. In the United States, one in 10 women of childbearing age have the condition, which affects the endocrine and reproductive systems and is a common cause of infertility. Yet, the condition is significantly underdiagnosed—especially among people of color—and under-researched.
Read on to find out more about PCOS, what symptoms to look out for, what treatments are available, and useful resources.
What is PCOS, and what are its most common symptoms?
PCOS is a chronic hormonal condition that affects how the ovaries work. A hormonal imbalance causes people with PCOS to have too much testosterone, the male sex hormone, which can make their periods irregular and cause hirsutism (extra hair), explains Dr. Melanie Cree, associate professor at the University of Colorado School of Medicine and director of the Multi-Disciplinary PCOS clinic at Children’s Hospital Colorado.
This means that people can have excess facial or body hair or experience hair loss.
PCOS also impacts the relationship between insulin—the hormone released when we eat—and testosterone.
“In women with PCOS, it seems like their ovaries are sensitive to insulin, and so when their ovaries see insulin, [they] make extra testosterone,” Cree adds. “So things that affect insulin levels [like sugary drinks] can affect testosterone levels.”
Other common symptoms associated with PCOS include:
- Acne
- Thinning hair
- Skin tags or excess skin in the armpits or neck
- Ovaries with many cysts
- Infertility
- Anxiety, depression, and other mental health conditions
- Sleep apnea, a condition where breathing stops and restarts while sleeping
What causes PCOS?
The cause is still unknown, but researchers have found that the condition is genetic and can be inherited. Experts have found that exposure to harmful chemicals like PFAs, which can be present in drinking water, and BPA, commonly used in plastics, can also increase the risk for PCOS.
Studies have shown that “BPA can change how the endocrine system develops in a developing fetus … and that women with PCOS tend to also have more BPA in their bodies,” adds Dr. Felice Gersh, an OB-GYN and founder and director of the Integrative Medical Group of Irvine, which treats patients with PCOS.
How is PCOS diagnosed?
PCOS is diagnosed through a physical exam; a conversation with your health care provider about your symptoms and medical history; a blood test to measure your hormone levels; and, in some cases, an ultrasound to see your ovaries.
PCOS is what’s known as a “diagnosis of exclusion,” Ottey says, meaning that the provider must rule out other conditions, such as thyroid disease, before diagnosing it.
Why isn’t more known about PCOS?
Research on PCOS has been scarce, underfunded, and narrowly focused. Research on the condition has largely focused on the reproductive system, Ottey says, even though it also affects many aspects of a person’s life, including their mental health, appearance, metabolism, and weight.
“There is the point of getting pregnant, and the struggle to get pregnant for so many people,” Ottey adds. “[And] once that happens, [the condition] also impacts your ability to carry a healthy pregnancy, to have healthy babies. But outside of that, your metabolic health is at risk from having PCOS, your mental health is at risk, [and] overall health and quality of life, they’re all impacted by PCOS.”
People with PCOS are more likely to develop other serious health issues, like high blood pressure, heart problems, high cholesterol, uterine cancer, and diabetes. Cree says that teenagers with PCOS and obesity have “an 18-fold higher risk of type 2 diabetes” in their teens and that teenagers who get type 2 diabetes are starting to die in their late 20s and early 30s.
What are some treatments for PCOS?
There is still no single medication approved by the Food and Drug Administration specifically for PCOS, though advocacy groups like PCOS Challenge are working with the agency to incorporate patient experiences and testimonials into a possible future treatment. Treatment depends on what symptoms you experience and what your main concerns are.
For now, treatment options include the following:
- Birth control: Your provider may prescribe birth control pills to lower testosterone levels and regulate your menstrual cycle.
- Lifestyle changes: Because testosterone can affect insulin levels, Cree explains that regardless of a patient’s weight, a diet with lower simple carbohydrates (such as candy, sugar, sweets, juices, sodas, and coffee drinks) is recommended.
“When you have a large amount of sugar like that, especially as a liquid, it gets into your bloodstream very quickly,” adds Cree. “And so you then release a ton of insulin that goes to the ovary, and you make a bunch of testosterone.”
More exercise is also recommended for both weight loss and weight maintenance, Cree says: “Food changes and better activity work directly to lower insulin, to lower testosterone.”
- Metformin: Even though it’s a medication for type 2 diabetes, it’s used in patients with PCOS because it can reduce insulin levels, and as a result, lower testosterone levels.
What should I keep in mind if I have (or think I may have) PCOS?
If your periods are irregular or you have acne, facial hair, or hair loss, tell your provider—it could be a sign that you have PCOS or another condition. And ask questions.
“I call periods a vital sign for women, if you’re not taking hormones,” Cree says. “Our bodies are really smart: Periods are to get pregnant, and if our body senses that we’re not healthy enough to get pregnant, then we don’t have periods. That means we’ve got to figure out why.”
Once you’re diagnosed, Ottey recommends that you “don’t go through extremes, yo-yo dieting, or trying to achieve massive weight loss—it only rebounds.”
She adds that “when you get this diagnosis, [there’s] a lot that might feel like it’s being taken away from you: ‘Don’t do this. Don’t eat this. Don’t do that.’ But what I want everyone to think of is what brings you joy, and do more of that and incorporate a lot of healthy activities into your life.”
Resources for PCOS patients:
- AskPCOS: A guide designed by experts on the condition that helps answer all your questions about it and how to manage it.
- PCOS Challenge: An advocacy and support organization for people with PCOS.
- PCOS Patient Communication Guide: A tool for better communication with your health care providers.
- Polycystic Ovary Syndrome Question Prompt List: Questions you can ask your provider about PCOS.
For more information, talk to your health care provider.
This article first appeared on Public Good News and is republished here under a Creative Commons license.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Coconut & Lemongrass Protein Soup
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The main protein here is pea protein, but the soup’s health benefits don’t stop there. With healthy MCTs from the coconut, as well as phytochemical benefits from the ginger and chili, this wonderfully refreshing soup has a lot to offer.
You will need
- 1 can coconut milk
- 1 cup vegetable stock (making your own, or buying a low-sodium option)
- 1 cup frozen petits pois
- 1 oz fresh ginger, roughly chopped
- ½ oz lemongrass stalk, crumpled without being broken into multiple pieces
- 1 red chili, roughly chopped
- 1 tbsp white miso paste
- zest and juice of 1 lime
- Optional: garnish of your choice
Method
(we suggest you read everything at least once before doing anything)
1) Mix the coconut milk, vegetable stock, ginger, and chili in a saucepan, and simmer for 15 minutes
2) Remove the lemongrass and ginger (and the chili if you don’t want more heat), and add the petit pois. Bring back to a simmer for about 2 minutes more, stir in the miso paste and lime, then take off the heat.
3) Blend the soup to a smooth purée. Since it is hot, you will need to either use a stick blender, or else a food processor that is ok with blending hot liquids (many are not, so don’t use yours unless you’re sure, as it might explode if it’s not made for that). Alternatively, you can let it cool, blend it, and then reheat it.
4) Serve, adding a garnish if you so wish:
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Can Saturated Fats Be Healthy?
- Ginger Does A Lot More Than You Think
- Capsaicin For Weight Loss And Against Inflammation
Take care!
Share This Post
-
Nutrivore – by Dr. Sarah Ballantyne
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The core idea of this book is that foods can be assigned a numerical value according to their total nutritional value, and that this number can be used to guide a person’s diet such that we will eat, in aggregate, a diet that is more nutritious. So far, so simple.
What Dr. Ballantyne also does, besides explaining and illustrating this system (there are chapters explaining the calculation system, and appendices with values), is also going over what to consider important and what we can let slide, and what things we might need more of to address a wide assortment of potential health concerns. And yes, this is definitely a “positive diet” approach, i.e. it focuses on what to add in, not what to cut out.
The premise of the “positive diet” approach is simple, by the way: if we get a full set of good nutrients, we will be satisfied and not crave unhealthy food.
She also offers a lot of helpful “rules of thumb”, and provides a variety of cheat-sheets and suchlike to make things as easy as possible.
There’s also a recipes section! Though, it’s not huge and it’s probably not necessary, but it’s just one more “she’s thinking of everything” element.
Bottom line: if you’d like a single-volume “Bible of” nutrition-made-easy, this is a very usable tome.
Click here to check out Nutrivore, and start filling up your diet!
Share This Post
-
What Teas To Drink Before Bed (By Science!)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Which Sleepy Tea?
Herbal “tea” preparations (henceforth we will write it without the quotation marks, although these are not true teas) are popular for winding down at the end of a long day ready for a relaxing sleep.
Today we’ll look at the science for them! We’ll be brief for each, because we’ve selected five and have only so much room, but here goes:
Camomile
Simply put, it works and has plenty of good science for it. Here’s just one example:
❝Noteworthy, our meta-analysis showed a significant improvement in sleep quality after chamomile administration❞
Also this writer’s favourite relaxation drink!
(example on Amazon if you want some)
Lavender
We didn’t find robust science for its popularly-claimed sedative properties, but it does appear to be anxiolytic, and anxiety gets in the way of sleep, so while lavender may not be a sedative, it may calm a racing mind all the same, thus facilitating better sleep:
(example on Amazon if you want some)
Magnolia
Animal study for the mechanism:
Human study for “it is observed to help humans sleep better”:
As you can see from the title, its sedative properties weren’t the point of the study, but if you click through to read it, you can see that they found (and recorded) this benefit anyway
(example on Amazon if you want some)
Passionflower
There’s not a lot of evidence for this one, but there is some. Here’s a small study (n=41) that found:
❝Of six sleep-diary measures analysed, sleep quality showed a significantly better rating for passionflower compared with placebo (t(40) = 2.70, p < 0.01). These initial findings suggest that the consumption of a low dose of Passiflora incarnata, in the form of tea, yields short-term subjective sleep benefits for healthy adults with mild fluctuations in sleep quality.❞
So, that’s not exactly a huge body of evidence, but it is promising.
(example on Amazon if you want some)
Valerian
We’ll be honest, the science for this one is sloppy. It’s very rare to find Valerian tested by itself (or sold by itself; we had to dig a bit to find one for the Amazon link below), and that skews the results of science and renders any conclusions questionable.
And the studies that were done? Dubious methods, and inconclusive results:
Nevertheless, if you want to try it for yourself, you can do a case study (i.e., n=1 sample) if not a randomized controlled trial, and let us know how it goes 🙂
(example on Amazon if you want some)
Summary
- Valerian we really don’t have the science to say anything about it
- Passionflower has some nascent science for it, but not much
- Lavender is probably not soporific, but it is anxiolytic
- Magnolia almost certainly helps, but isn’t nearly so well-backed as…
- Camomile comes out on top, easily—by both sheer weight of evidence, and by clear conclusive uncontroversial results.
Enjoy!
Share This Post
Related Posts
-
Just One Heart – by Dr. Jonathan Fisher
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
First, what this is not: a book to say eat fiber, go easy on the salt, get some exercise, and so forth.
What this rather is: a book about the connection between the heart and mind; often written poetically, the simple biological reality is that our emotional state does have a genuine impact on our heart health, and as such, any effort to look after our heart (healthwise) would be incomplete without an effort to look after our heart (emotionally).
Dr. Fisher talks about the impact of stress and uncertainty, as well as peace and security, on heart health—and then, having sorted emotional states into “heart breakers” and “heart wakers”, he goes about laying out a plan for what is, emotionally and thus also physiologically, good for our heart.
Chapter by chapter, he walks us through the 7 principles to live by:
- Steadiness: how to steady your heart amid chaos
- Wisdom: how to develop a wise heart in uncertain times
- Openness: how to safely open your heart in a threatening world
- Wholeness: how to show up with your whole heart without going to pieces
- Courage: how to lead with a courageous heart when fear surrounds you
- Lightness: how to live with a light heart in a heavy world
- Warmth: how to love with a warm heart when life feels cold
The style is anything but clinical; it’s well-written, certainly, and definitely informed in part by his medical understanding of the heart, but it’s entirely the raw human element that shines throughout, and that makes the ideas a lot more tangible.
Bottom line: if you’d like your heart to be healthy (cardiac health) and your heart to be healthy (emotional health), this book is a very worthwhile read.
Click here to check out Just One Heart, and take care of yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Ear Candling: Is It Safe & Does It Work?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Does This Practice Really Hold A Candle To Evidence-Based Medicine?
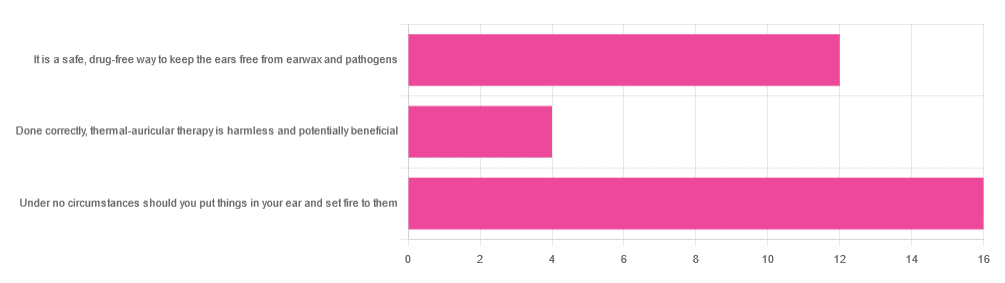
In Tuesday’s newsletter, we asked you your opinion of ear candling, and got the above-depicted, below-described set of responses:
- Exactly 50% said “Under no circumstances should you put things in your ear and set fire to them”
- About 38% said “It is a safe, drug-free way to keep the ears free from earwax and pathogens”
- About 13% said “Done correctly, thermal-auricular therapy is harmless and potentially beneficial”
This means that if we add the two positive-to-candling answers together, it’s a perfect 50:50 split between “do it” and “don’t do it”.
(Yes, 38%+13%=51%, but that’s because we round to the nearest integer in these reports, and more precisely it was 37.5% and 12.5%)
So, with the vote split, what does the science say?
First, a quick bit of background: nobody seems keen to admit to having invented this. One of the major manufacturers of ear candles refers to them as “Hopi” candles, which the actual Hopi tribe has spent a long time asking them not to do, as it is not and never has been used by the Hopi people. Other proposed origins offered by advocates of ear candling include Traditional Chinese Medicine (not used), Ancient Egypt (no evidence of such whatsoever), and Atlantis:
Quackwatch | Why Ear Candling Is Not A Good Idea
It is a safe, drug-free way to keep the ears free from earwax and pathogens: True or False?
False! In a lot of cases of alternative therapy claims, there’s an absence of evidence that doesn’t necessarily disprove the treatment. In this case, however, it’s not even an open matter; its claims have been actively disproven by experimentation:
- It doesn’t remove earwax; on the contrary, experimentation “showed no removal of cerumen from the external auditory canal. Candle wax was actually deposited in some“
- It doesn’t remove pathogens, and the proposed mechanism of action for removing pathogens, that of the “chimney effect”: the idea that the burning candle creates a vacuum that draws wax out of the ear along with debris and bacteria, simply does not work; on the contrary, “Tympanometric measurements in an ear canal model demonstrated that ear candles do not produce negative pressure”.
- It isn’t safe; on the contrary, “Ear candles have no benefit in the management of cerumen and may result in serious injury”
In a medium-sized survey (n=122), the following injuries were reported:
- 13 x burns
- 7 x occlusion of the ear canal
- 6 x temporary hearing loss
- 3 x otitis externa (this also called “swimmer’s ear”, and is an inflammation of the ear, accompanied by pain and swelling)
- 1 x tympanic membrane perforation
Indeed, authors of one paper concluded:
❝Ear candling appears to be popular and is heavily advertised with claims that could seem scientific to lay people. However, its claimed mechanism of action has not been verified, no positive clinical effect has been reliably recorded, and it is associated with considerable risk.
No evidence suggests that ear candling is an effective treatment for any condition. On this basis, we believe it can do more harm than good and we recommend that GPs discourage its use❞
Source: Canadian Family Physician | Ear Candling
Under no circumstances should you put things in your ear and set fire to them: True or False?
True! It’s generally considered good advice to not put objects in general in your ears.
Inserting flaming objects is a definite no-no. Please leave that for the Cirque du Soleil.
You may be thinking, “but I have done this and suffered no ill effects”, which seems reasonable, but is an example of survivorship bias in action—it doesn’t make the thing in question any safer, it just means you were one of the one of the ones who got away unscathed.
If you’re wondering what to do instead… Ear oils can help with the removal of earwax (if you don’t want to go get it sucked out at a clinic—the industry standard is to use a suction device, which actually does what ear candles claim to do). For information on safely getting rid of earwax, see our previous article:
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
SMOL Bowl With Sautéed Greens
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Whole grains are good, and gluten is bad for some people. Today’s dish has four whole grains, and no gluten (assuming no cross-contamination, so look for the gluten-free label if that’s important to you). Breafast? Brunch? Lunch? Supper, even? This is good at any time of day, packed with nutrients and full of flavor!
You will need (per person)
- 1 cup mixed cooked grains of equal parts sorghum, millet, oats, lentils (SMOL)—these can be cooked in bulk in advance and frozen in portions, as it’s often good to used mixed grains, and these four are a great combination for many purposes.
- ½ cup low sodium vegetable stock (ideally you made this yourself from vegetable offcuts you kept in the freezer until you had enough for this purpose, but failing that, low-sodium stock cubes can be bought at most large supermarkets).
- ½ cup finely chopped red onion
- 6 oz cavolo nero, finely chopped
- 1 small carrot, finely chopped
- 3 cloves garlic, finely chopped
- 1 tbsp nutritional yeast
- 1 tsp black pepper, coarse ground
- 1 tsp white miso paste
- To serve: 1 lemon wedge
Method
(we suggest you read everything at least once before doing anything)
1) Add the stock to a sauté pan over a medium heat, and add the onion, garlic, and carrot. Stir frequently for about 7 minutes.
2) Add the cavolo nero and miso paste, stirring for another 4 minutes. If there is any liquid remaining, drain it off now.
3) Warm the SMOL mixture (microwave is fine) and spoon it into a bowl, topping with the nutritional yeast and black pepper. Finally, add the hot cavolo nero mixture.
4) Serve with the lemon wedge on the side, to add a dash of lemon at will.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: