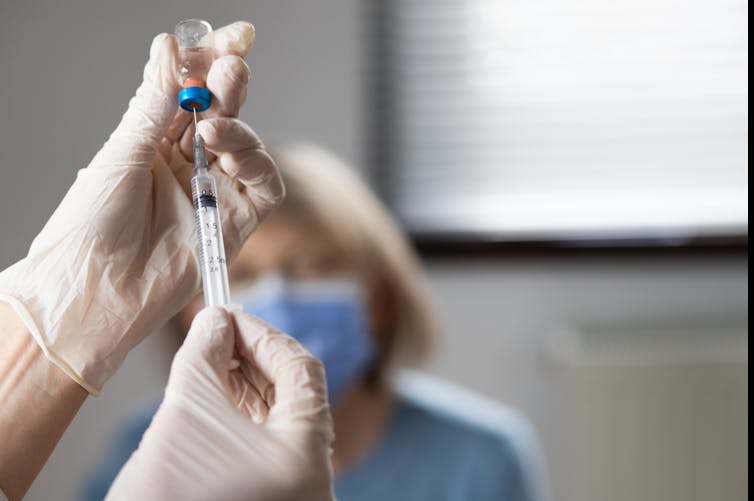
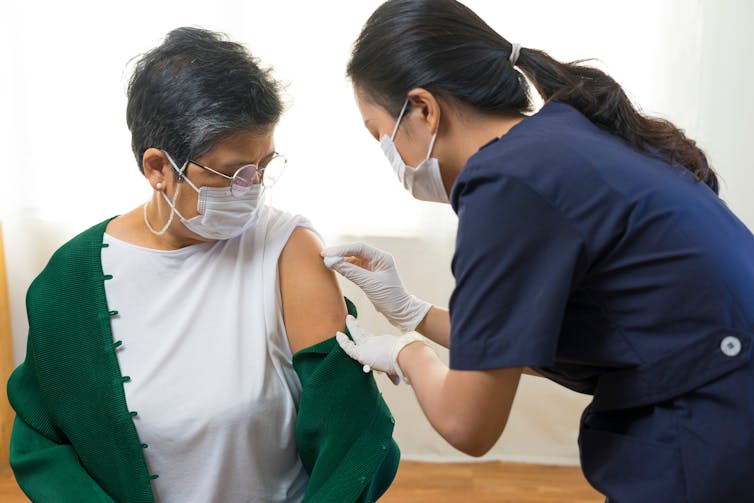
Asbestos in mulch? Here’s the risk if you’ve been exposed
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Mulch containing asbestos has now been found at 41 locations in New South Wales, including Sydney parks, schools, hospitals, a supermarket and at least one regional site. Tests are under way at other sites.
As a precautionary measure, some parks have been cordoned off and some schools have closed temporarily. Fair Day – a large public event that traditionally marks the start of Mardi Gras – was cancelled after contaminated mulch was found at the site.
The New South Wales government has announced a new taskforce to help investigate how the asbestos ended up in the mulch.
Here’s what we know about the risk to public health of mulch contaminated with asbestos, including “friable” asbestos, which has been found in one site (Harmony Park in Surry Hills).
What are the health risks of asbestos?
Asbestos is a naturally occurring, heat-resistant fibre that was widely used in building materials from the 1940s to the 1980s. It can be found in either a bonded or friable form.
Bonded asbestos means the fibres are bound in a cement matrix. Asbestos sheeting that was used for walls, fences, roofs and eaves are examples of bonded asbestos. The fibres don’t escape this matrix unless the product is severely damaged or worn.
A lot of asbestos fragments from broken asbestos products are still considered bonded as the fibres are not released as they lay on the ground.

Tomas Regina/Shutterstock
Friable asbestos, in contrast, can be easily crumbled by touch. It will include raw asbestos fibres and previously bonded products that have worn to the point that they crumble easily.
The risk of disease from asbestos exposure is due to the inhalation of fibres. It doesn’t matter if those fibres are from friable or bonded sources.
However, fibres can more easily become airborne, and therefore inhalable, if the asbestos is friable. This means there is more of a risk of exposure if you are disturbing friable asbestos than if you disturb fragments of bonded asbestos.
Who is most at risk from asbestos exposure?
The most important factor for disease risk is exposure – you actually have to inhale fibres to be at risk of disease.
Just being in the vicinity of asbestos, or material containing asbestos, does not put you at risk of asbestos-related disease.
For those who accessed the contaminated areas, the level of exposure will depend on disturbing the asbestos and how many fibres become airborne due to that disturbance.
However, if you have been exposed to, and inhaled, asbestos fibres it does not mean you will get an asbestos-related disease. Exposure levels from the sites across Sydney will be low and the chance of disease is highly unlikely.
The evidence for disease risk from ingestion remains highly uncertain, although you are not likely to ingest sufficient fibres from the air, or even the hand to mouth activities that may occur with playing in contaminated mulch, for this to be a concern.
The risk of disease from exposure depends on the intensity, frequency and duration of that exposure. That is, the more you are exposed to asbestos, the greater the risk of disease.
Most asbestos-related disease has occurred in people who work with raw asbestos (for example, asbestos miners) or asbestos-containing products (such as building tradespeople). This has been a tragedy and fortunately asbestos is now banned.
There have been cases of asbestos-related disease, most notably mesothelioma – a cancer of the lining of the lung (mostly) or peritoneum – from non-occupational exposures. This has included people who have undertaken DIY home renovations and may have only had short-term exposures. The level of exposure in these cases is not known and it is also impossible to determine if those activities have been the only exposure.
There is no known safe level of exposure – but this does not mean that one fibre will kill. Asbestos needs to be treated with caution.
As far as we are aware, there have been no cases of mesothelioma, or other asbestos-related disease, that have been caused by exposure from contaminated soils or mulch.
Has asbestos been found in mulch before?
Asbestos contamination of mulch is, unfortunately, not new. Environmental and health agencies have dealt with these situations in the past. All jurisdictions have strict regulations about removing asbestos products from the green waste stream but, as is happening in Sydney now, this does not always happen.

gibleho/Shutterstock
What if I’ve been near contaminated mulch?
Exposure from mulch contamination is generally much lower than from current renovation or construction activities and will be many orders of magnitude lower than past occupational exposures.
Unlike activities such as demolition, construction and mining, the generation of airborne fibres from asbestos fragments in mulch will be very low. The asbestos contamination will be sparsely spread throughout the mulch and it is unlikely there will be sufficient disturbance to generate large quantities of airborne fibres.
Despite the low chance of exposure, if you’re near contaminated mulch, do not disturb it.
If, by chance, you have had an exposure, or think you have had an exposure, it’s highly unlikely you will develop an asbestos-related disease in the future. If you’re worried, the Asbestos Safety and Eradication Agency is a good source of information.
Peter Franklin, Associate Professor and Director, Occupational Respiratory Epidemiology, The University of Western Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Watch Out For Lipedema
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Lipedema occurs mostly in women, mostly in times of hormonal change, with increasing risk as time goes by (so for example, puberty yields a lower risk than pregnancy, which yields a lower risk than menopause).
Its name literally means “fat swelling”, and can easily be mistaken for obesity or, in its earlier stages, just pain old cellulite.
Cellulite, by the way, is completely harmless and is also not, per se, an indicator of bad health. But if you have it and don’t like it, you can reduce it:
Obesity is more of a complex matter, and one that we’ve covered here:
Lipedema is actively harmful
Lipedema can become a big problem, because lifestyle change does not reduce lipedema fat, the fat is painful, can lead to obesity if one was not already obese, causes gait and joint abnormalities, causes fatigue, can lead to lymphedema (beyond the scope of today’s article—perhaps another time!) and very much psychosocial distress.
Like many conditions that mostly affect women, the science is… Well, here’s a recent example review that was conducted and published:
Fun fact: in Romanian there is an expression “one eye is laughing; the other is crying”, and it seems appropriate here.
Spot the signs
Because it’s most readily mistaken for cellulite in first presentation, let’s look at the differences between them:
- Cellulite is characterized by dimpled, bumpy, or even skin; lipedema is the same but with swelling too.
- Cellulite is a connective tissue condition; lipedema is too (at least in part), but also involves the abnormal accumulation and deposition of fat cells, rather than just pulling some down a bit.
- Cellulite has no additional symptoms; lipedema soon also brings swollen limbs, joint pain, and/or skin that’s “spongy” and easily bruised.
What to do about it
First, get it checked out by a doctor.
If the doctor says it is just cellulite or obesity, ask them what difference(s) they are basing that on, and ask that they confirm in writing having dismissed your concerns (having this will be handy later if it turns out to be lipedema after all).
If it is lipedema, you will want to catch it early; there is no known cure, but advanced symptoms are a lot easier to keep at bay than they are to reverse once they’ve shown up.
Weight maintenance, skin care (including good hydration), and compression therapy have all been shown to help slow the progression.
If it is allowed to progress unhindered, that’s when a lot more fat accumulation and joint pain is likely to occur. Liposuction and surgery are options, but even they are only a temporary solution, and are obviously not fun things to have to go through.
Prevention is, as ever, much better than
curetreatment ← because there is no known cureOne last thing
Lipedema’s main risk factor is genetic. The bad news is, there’s not much that can be done about that for now, but the good news is, you can at least get the heads-up about whether you are at increased risk or not, and be especially vigilant if you’re in the increased risk group. See also:
One Test, Many Warnings: The Real Benefit Of Genetic Testing
Take care!
Share This Post
-
Vegetarian & Vegan Diets: Good Or Bad For Brain Health?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s well-established that most people should eat more plants, and generally speaking, less meat. But what about abstaining from meat completely? And what about abstaining from all animal products?
For a more general overview (rather than specifically brain health), check out: Do We Need Animal Products To Be Healthy?
Now, about brains…
Before Homo sapiens was a thing, our precursors such as Homo habilis developed language (thus: greatly enhanced collaborative teamwork) and cooking, resulting in Homo ergaster (who came approximately next in line, give or take taxonomical quibbles) having twice the cranial capacity, generally attributed to being able to acquire and—where appropriate—cook calorie-dense food, which included meat, and also tubers that can’t be safely eaten raw. It’s estimated (based on forensic examination of tooth wear, mineralization, microdeposits of various kinds, etc) that our consumption of animal products in that era was around 10% of our diet (fluctuating by region, of course), but it likely was an important one.
By the time we got to Homo erectus, our skulls (including our cranial cavities, and thus it is presumed, our brains) were actually larger than in Homo sapiens. You may be wondering about Homo neanderthalensis; our cousins (or in some cases, ancestors—but that is beyond the scope of today’s article) also had larger cranial cavities than us, and certainly enjoyed comparatively advanced culture, arts, religion, etc.
Fast-forward to the present day. Nothing is going to meaningfully change our skull size, as individuals. Brain size? Well, keep hydrated or it’ll shrink. Don’t overhydrate or it’ll swell. Neuroplasticity means we can increase (or lose) volume in specific areas of the brain, according to what we do most of. For example, if you were to scan this writer’s brain, you’d probably find overdevelopment in the various areas pertaining to language and memory, as that’s been “my thing” for as long as I can remember (which is a long way). See also: An Underrated Tool Against Alzheimer’s
The impact of diet in the modern day
Unlike our distant ancestors, if we want a high-calorie snack we can buy some nuts from the supermarket, and if anything, this can be a problem (as many people’s go-to high-calorie snack may be a lot less healthy than that), and in turn cause problems for the brain, because too many pizzas, cheeseburgers, tater tots, and so forth cause chronic inflammation, and thus, neuroinflammation.
See also: 6 Worst Foods That Cause Dementia
So much for “calories for the brain”. Yes, the brain definitely needs calories (it expends a very large portion of our daily calorie intake), but you can have too much of a good thing.
In any case, the brain needs more than just calories!
For example, you may remember the “6 Pillars Of Nutritional Psychiatry”, which are:
- Be whole; eat whole
- Eat the rainbow
- The greener, the better
- Tap into your body intelligence
- Consistency & balance are key
- Avoid anxiety-triggering foods
For more on all of those, see Dr. Uma Naidoo’s 6 Pillars Of Nutritional Psychiatry ← She’s a Harvard-trained psychiatrist, professional chef graduating with her culinary school’s most coveted award, and a trained nutritionist. Between those three qualifications, she knows her stuff when it comes to the niche that is nutritional psychiatry.
When it comes to any potential nutritional deficiencies of a vegetarian or vegan diet, it’s a matter of planning.
Properly planned vegetarian diets are rich in essential nutrients like carbohydrates, fiber, magnesium, potassium, folate, vitamins C and E, and an abundance of phytochemicals, which support brain health (and overall health too, but today is about brain health).
However, if not well-planned, they can indeed lack certain nutrients such as vitamin B12, iron, and omega-3 fatty acids, which are critical for brain function.
In essence, there’s a difference between a “whole foods plant-based diet” and junk food that just happens to be vegetarian or vegan.
Vitamin B12 is usually supplemented by vegans, but it can also be enjoyed from nutritional yeast used in cooking (it adds a cheesy flavor to dishes for which that’d be appropriate).
Iron is a fascinating beast, because while everyone thinks of red meat (which is indeed rich in iron), not only are there good plant-based sources of iron, but there are important considerations when it comes to bioavailability differences between heme and non-heme iron. In few words, heme iron (from blood etc) is more bioavailable by 1.8x, but all iron, including non-heme iron (from beans, greens, etc) can have its bioavailability multiplied by 5x just by having it with vitamin C:
Avoiding Anemia (More Than Just “Get More Iron”)
Omega-3 fatty acids, for vegetarians that mostly means eggs. See: Eggs: All Things In Moderation?
For vegans, we must look to nuts and seeds, for the most part. Or supplement—many omega 3 supplements are vegan, made from algae, or seaweed (that in turn is composed partially or entirely of algae):
So really, it comes down to “make sure you still get these things”, and once you’re used to it, it’s easy.
For those who prefer to keep some meat in their diet
Our summary in our top-linked article (Do We Need Animal Products To Be Healthy?) concluded:
- Most of us can live healthily and happily on just plants if we so choose.
- Some people cannot, and will require varying kinds (and quantities) of animal products.
- As for red and/or processed meats, we’re not the boss of you, but from a health perspective, the science is clear: unless you have a circumstance that really necessitates it, just don’t.
- Same goes for pork, which isn’t red and may not be processed, but metabolically it’s associated with the same problems.
- The jury is out on poultry, but it strongly appears to be optional, healthwise, without making much of a difference either way
- Fish is roundly considered healthful in moderation. Enjoy it if you want, don’t if you don’t.
And the paper from which we’ve largely been working from today included such comments as:
❝ Evidence suggests that vegan and vegetarian diets, when well planned, can be rich in phytonutrients and antioxidants, which have been associated with lower levels of inflammatory markers, such as C-reactive protein (CRP) and interleukin-6 (IL-6). These findings indicate a potential role in reducing systemic inflammation and oxidative stress, both of which are linked to neurodegenerative diseases.
However, deficiencies in critical nutrients such as vitamin B12, DHA, EPA, and iron have been consistently associated with an increased risk of cognitive decline, mood disturbances, and neurodegenerative disorders.
While plant-based diets provide anti-inflammatory and antioxidant benefits, their neurological implications depend on nutrient adequacy. Proper planning, supplementation, and food preparation techniques are essential to mitigate risks and enhance cognitive health.❞
Source: Impact of Vegan and Vegetarian Diets on Neurological Health: A Critical Review ← you can see that they also cover the same nutrients that we do
One final note, not discussed above
We often say “what’s good for your heart is good for your brain”, because the former feeds the latter (with oxygen and nutrients) and assists in cleanup (of detritus that otherwise brings about cognitive decline).
So with that in mind…
What Matters Most For Your Heart? ← hint: it’s fiber. So whether you eat animal products or not, please do eat plenty of plants!
Take care!
Share This Post
-
Could the shingles vaccine lower your risk of dementia?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A recent study has suggested Shingrix, a relatively new vaccine given to protect older adults against shingles, may delay the onset of dementia.
This might seem like a bizarre link, but actually, research has previously shown an older version of the shingles vaccine, Zostavax, reduced the risk of dementia.
In this new study, published last week in the journal Nature Medicine, researchers from the United Kingdom found Shingrix delayed dementia onset by 17% compared with Zostavax.
So how did the researchers work this out, and how could a shingles vaccine affect dementia risk?
Melinda Nagy/Shutterstock From Zostavax to Shingrix
Shingles is a viral infection caused by the varicella-zoster virus. It causes painful rashes, and affects older people in particular.
Previously, Zostavax was used to vaccinate against shingles. It was administered as a single shot and provided good protection for about five years.
Shingrix has been developed based on a newer vaccine technology, and is thought to offer stronger and longer-lasting protection. Given in two doses, it’s now the preferred option for shingles vaccination in Australia and elsewhere.
In November 2023, Shingrix replaced Zostavax on the National Immunisation Program, making it available for free to those at highest risk of complications from shingles. This includes all adults aged 65 and over, First Nations people aged 50 and older, and younger adults with certain medical conditions that affect their immune systems.
What the study found
Shingrix was approved by the US Food and Drugs Administration in October 2017. The researchers in the new study used the transition from Zostavax to Shingrix in the United States as an opportunity for research.
They selected 103,837 people who received Zostavax (between October 2014 and September 2017) and compared them with 103,837 people who received Shingrix (between November 2017 and October 2020).
By analysing data from electronic health records, they found people who received Shingrix had a 17% increase in “diagnosis-free time” during the follow-up period (up to six years after vaccination) compared with those who received Zostavax. This was equivalent to an average of 164 extra days without a dementia diagnosis.
The researchers also compared the shingles vaccines to other vaccines: influenza, and a combined vaccine for tetanus, diphtheria and pertussis. Shingrix and Zostavax performed around 14–27% better in lowering the risk of a dementia diagnosis, with Shingrix associated with a greater improvement.
The benefits of Shingrix in terms of dementia risk were significant for both sexes, but more pronounced for women. This is not entirely surprising, because we know women have a higher risk of developing dementia due to interplay of biological factors. These include being more sensitive to certain genetic mutations associated with dementia and hormonal differences.
Why the link?
The idea that vaccination against viral infection can lower the risk of dementia has been around for more than two decades. Associations have been observed between vaccines, such as those for diphtheria, tetanus, polio and influenza, and subsequent dementia risk.
Research has shown Zostavax vaccination can reduce the risk of developing dementia by 20% compared with people who are unvaccinated.
But it may not be that the vaccines themselves protect against dementia. Rather, it may be the resulting lack of viral infection creating this effect. Research indicates bacterial infections in the gut, as well as viral infections, are associated with a higher risk of dementia.
Notably, untreated infections with herpes simplex (herpes) virus – closely related to the varicella-zoster virus that causes shingles – can significantly increase the risk of developing dementia. Research has also shown shingles increases the risk of a later dementia diagnosis.
This isn’t the first time research has suggested a vaccine could reduce dementia risk. ben bryant/Shutterstock The mechanism is not entirely clear. But there are two potential pathways which may help us understand why infections could increase the risk of dementia.
First, certain molecules are produced when a baby is developing in the womb to help with the body’s development. These molecules have the potential to cause inflammation and accelerate ageing, so the production of these molecules is silenced around birth. However, viral infections such as shingles can reactivate the production of these molecules in adult life which could hypothetically lead to dementia.
Second, in Alzheimer’s disease, a specific protein called Amyloid-β go rogue and kill brain cells. Certain proteins produced by viruses such as COVID and bad gut bacteria have the potential to support Amyloid-β in its toxic form. In laboratory conditions, these proteins have been shown to accelerate the onset of dementia.
What does this all mean?
With an ageing population, the burden of dementia is only likely to become greater in the years to come. There’s a lot more we have to learn about the causes of the disease and what we can potentially do to prevent and treat it.
This new study has some limitations. For example, time without a diagnosis doesn’t necessarily mean time without disease. Some people may have underlying disease with delayed diagnosis.
This research indicates Shingrix could have a silent benefit, but it’s too early to suggest we can use antiviral vaccines to prevent dementia.
Overall, we need more research exploring in greater detail how infections are linked with dementia. This will help us understand the root causes of dementia and design potential therapies.
Ibrahim Javed, Enterprise and NHMRC Emerging Leadership Fellow, UniSA Clinical & Health Sciences, University of South Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
The Mindful Body – by Dr. Ellen Langer
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fear not, this is not a “think healing thoughts” New Age sort of book. In fact, it’s quite the contrary.
The most common negative reviews for this on Amazon are that it is too densely packed with scientific studies, and some readers found it hard to get through since they didn’t find it “light reading”.
Counterpoint: this reviewer found it very readable. A lot of it is as accessible as 10almonds content, and a lot is perhaps halfway between 10almonds content in readability, and the studies we cite. So if you’re at least somewhat comfortable reading academic literature, you should be fine.
The author, a professor of psychology (tenured at Harvard since 1981), examines a lot of psychosomatic effect. Psychosomatic effect is often dismissed as “it’s all in your head”, but it means: what’s in your head has an effect on your body, because your brain talks to the rest of the body and directs bodily responses and actions/reactions.
An obvious presentation of this in medicine is the placebo/nocebo effect, but Dr. Langer’s studies (indeed, many of the studies she cites are her own, from over the course of her 40-year career) take it further and deeper, including her famous “Counterclockwise” study in which many physiological markers of aging were changed (made younger) by changing the environment that people spent time in, to resemble their youth, and giving them instructions to act accordingly while there.
In the category of subjective criticism: the book is not exceptionally well-organized, but if you read for example a chapter a day, you’ll get all the ideas just fine.
Bottom line: if you want a straightforward hand-holding “how-to” guide, this isn’t it. But it is very much information-packed with a lot of ideas and high-quality science that’s easily applicable to any of us.
Click here to check out The Mindful Body, and indeed grow your chronic good health!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How To Kill Laziness
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Laziness Is A Scooby-Doo Villain.
Which means: to tackle it requires doing a Scooby-Doo unmasking.
You know, when the mystery-solving gang has the “ghost” or “monster” tied to a chair, and they pull the mask off, to reveal that there was no ghost etc, and in fact it was a real estate scammer or somesuch.
Social psychologist Dr. Devon Price wrote about this (not with that metaphor though) in a book we haven’t reviewed yet, but will one of these days:
Laziness Does Not Exist – by Dr. Devon Price (book)
In the meantime, and perhaps more accessibly, he gave a very abridged summary for Medium:
Medium | Laziness Does Not Exist… But unseen barriers do (11mins read)
Speaking of barriers, Medium added a paywall to that (the author did not, in fact, arrange the paywall as Medium claim), so in case you don’t have an account, he kindly made the article free on its own website, here:
Devon Price | Laziness Does Not Exist… But unseen barriers do (same article; no paywall)
He details problems that people get into (ranging from missed deadlines to homelessness), that are easily chalked up to laziness, but in fact, these people are not lazily choosing to suffer, and are usually instead suffering from all manner of unchosen things, ranging from…
- imposter syndrome / performance anxiety,
- perfectionism (which can overlap a lot with the above),
- social anxiety and/or depression (these also can overlap for some people),
- executive dysfunction in the brain, and/or
- just plain weathering “the slings and arrows of outrageous fortune [and] the heartache and the thousand natural shocks that flesh is heir to”, to borrow from Shakespeare, in ways that aren’t always obviously connected—these things can be great or small, it could be a terminal diagnosis of some terrible disease, or it could be a car breakdown, but the ripples spread.
And nor are you, dear reader, choosing to suffer (even if sometimes it appears otherwise)
Unless you’re actually a masochist, at least, in which case, you do you. But for most of us, what can look like laziness or “doing it to oneself” is usually a case of just having one or more of the above-mentioned conditions in place.
Which means…
That grace we just remembered above to give to other people?
Yep, we should give that to ourselves too.
Not as a free pass, but in the same way we (hopefully) would with someone else, and ask: is there some problem I haven’t considered, and is there something that would make this easier?
Here are some tools to get you started:
- Imposter Syndrome (And Why Almost Everyone Has It)
- Perfectionism, And How To Make Yours Work For You
- How To Set Anxiety Aside
- Mental Health First-Aid (To Get Yourself Or A Loved One Through Depression)
- Procrastination, And How To Pay Off The To-Do List Debt
- Take This Two-Minute Executive Dysfunction Test
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Sweet Truth About Diabetes
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
There’s A Lot Of Confusion About Diabetes!
For those readers who are not diabetic, nor have a loved one who is diabetic, nor any other pressing reason to know these things, first a quick 101 rundown of some things to understand the rest of today’s main feature:
- Blood sugar levels: how much sugar is in the blood, measured in mg/dL or mmol/L
- Hyperglycemia or “hyper” for short: too much sugar in the blood
- Hypoglycemia or “hypo” for short: too little sugar in the blood
- Insulin: a hormone that acts as a gatekeeper to allow sugar to pass, or not pass, into various parts of the body
- Type 1 diabetes (sometimes capitalized, and/or abbreviated to “T1D”) is an autoimmune disorder that prevents the pancreas from being able to supply the body with insulin. This means that taking insulin consistently is necessary for life.
- Type 2 diabetes is a matter of insulin resistance. The pancreas produces plenty of insulin, but the body has become desensitized to it, so it doesn’t work properly. Taking extra insulin may sometimes be necessary, but for many people, it can be controlled by means of a careful diet and other lifestyle factors.
With that in mind, on to some very popular myths…
Diabetes is caused by having too much sugar
While sugar is not exactly a health food, it’s not the villain of this story either.
- Type 1 diabetes has a genetic basis, triggered by epigenetic factors unrelated to sugar.
- Type 2 diabetes comes from a cluster of risk factors which, together, can cause a person to go through pre-diabetes and acquire type 2 diabetes.
- Those risk factors include:
- A genetic predisposition
- A large waist circumference
- (this is more relevant than BMI or body fat percentage)
- High blood pressure
- A sedentary lifestyle
- Age (the risk starts rising at 35, rises sharply at 45, and continues upwards with increasing age)
- Those risk factors include:
Read more: Risk Factors for Type 2 Diabetes
Diabetics can’t have sugar
While it’s true that diabetics must be careful about sugar (and carbs in general), it’s not to say that they can’t have them… just: be mindful and intentional about it.
- Type 1 diabetics will need to carb-count in order to take the appropriate insulin bolus. Otherwise, too little insulin will result in hyperglycemia, or too much insulin will result in hypoglycemia.
- Type 2 diabetics will often be able to manage their blood sugar levels with diet alone, and slow-release carbs will make this easier.
In either case, having quick release sugars will increase blood sugar levels (what a surprise), and sometimes (such as when experiencing a hypo), that’s what’s needed.
Also, when it comes to sugar, a word on fruit:
Not all fruits are equal, and some fruits can help maintain stable blood sugar levels! Read all about it:
Fruit Intake to Prevent and Control Hypertension and Diabetes
Artificial sweeteners are must-haves for diabetics
Whereas sugar is a known quantity to the careful diabetic, some artificial sweeteners can impact insulin sensitivity, causing blood sugars to behave in unexpected ways. See for example:
The Impact of Artificial Sweeteners on Body Weight Control and Glucose Homeostasis
If a diabetic person is hyper, they should exercise to bring their blood sugar levels down
Be careful with this!
- In the case of type 2 diabetes, it may (or may not) help, as the extra sugar may be used up.
- Type 1 diabetes, however, has a crucial difference. Because the pancreas isn’t making insulin, a hyper (above a certain level, anyway) means more insulin is needed. Exercising could do more harm than good, as unlike in type 2 diabetes, the body has no way to use that extra sugar, without the insulin to facilitate it. Exercising will just pump the syrupy hyperglycemic blood around the body, potentially causing damage as it goes (all without actually being able to use it).
There are other ways this can be managed that are outside of the scope of this newsletter, but “be careful” is rarely a bad approach.
Read more, from the American Diabetes Association:
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: