
AI: The Doctor That Never Tires?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
AI: The Doctor That Never Tires?
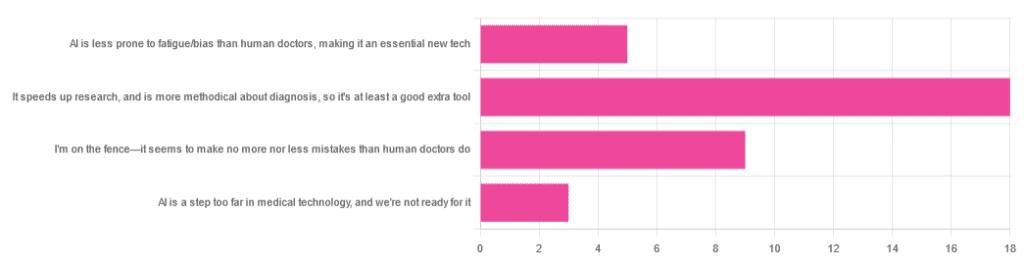
We asked you for your opinion on the use of Artificial Intelligence (AI) in healthcare, and got the above-depicted, below-described set of results:
- A little over half of respondents to the poll voted for “It speeds up research, and is more methodical about diagnosis, so it’s at least a good extra tool”
- A quarter of respondents voted for “I’m on the fence—it seems to make no more nor less mistakes than human doctors do”
- A little under a fifth of respondents voted for “AI is less prone to fatigue/bias than human doctors, making it an essential new tech”
- Three respondents voted for “AI is a step too far in medical technology, and we’re not ready for it”
Writer’s note: I’m a professional writer (you’d never have guessed, right?) and, apparently, I really did write “no more nor less mistakes”, despite the correct grammar being “no more nor fewer mistakes”. Now, I know this, and in fact, people getting less/fewer wrong is a pet hate of mine. Nevertheless, I erred.
Yet, now that I’m writing this out in my usual software, and not directly into the poll-generation software, my (AI!) grammar/style-checker is highlighting the error for me.
Now, an AI could not do my job. ChatGPT would try, and fail miserably. But can technology help me do mine better? Absolutely!
And still, I dismiss a lot of the AI’s suggestions, because I know my field and can make informed choices. I don’t follow it blindly, and I think that’s key.
AI is less prone to fatigue/bias than human doctors, making it an essential new tech: True or False?
True—with one caveat.
First, a quick anecdote from a subscriber who selected this option in the poll:
❝As long as it receives the same data inputs as my doctor (ie my entire medical history), I can see it providing a much more personalised service than my human doctor who is always forgetting what I have told him. I’m also concerned that my doctor may be depressed – not an ailment that ought to affect AI! I recently asked my newly qualified doctor goddaughter whether she would prefer to be treated by a human or AI doctor. No contest, she said – she’d go with AI. Her argument was that human doctors leap to conclusions, rather than properly weighing all the evidence – meaning AI, as long as it receives the same inputs, will be much more reliable❞
Now, an anecdote is not data, so what does the science say?
Well… It says the same:
❝Of 6695 responding physicians in active practice, 6586 provided information on the areas of interest: 3574 (54.3%) reported symptoms of burnout, 2163 (32.8%) reported excessive fatigue, and 427 (6.5%) reported recent suicidal ideation, with 255 of 6563 (3.9%) reporting a poor or failing patient safety grade in their primary work area and 691 of 6586 (10.5%) reporting a major medical error in the prior 3 months. Physicians reporting errors were more likely to have symptoms of burnout (77.6% vs 51.5%; P<.001), fatigue (46.6% vs 31.2%; P<.001), and recent suicidal ideation (12.7% vs 5.8%; P<.001).❞
See the damning report for yourself: Physician Burnout, Well-being, and Work Unit Safety Grades in Relationship to Reported Medical Errors
AI, of course, does not suffer from burnout, fatigue, or suicidal ideation.
So, what was the caveat?
The caveat is about bias. Humans are biased, and that goes for medical practitioners just the same. AI’s machine learning is based on source data, and the source data comes from humans, who are biased.
See: Bias and Discrimination in AI: A Cross-Disciplinary Perspective
So, AI can perpetuate human biases and doesn’t have a special extra strength in this regard.
The lack of burnout, fatigue, and suicidal ideation, however, make a big difference.
AI speeds up research, and is more methodical about diagnosis: True or False?
True! AI is getting more and more efficient at this, and as has been pointed out, doesn’t make errors due to fatigue, and often comes to accurate conclusions near-instantaneously. To give just one example:
❝Deep learning algorithms achieved better diagnostic performance than a panel of 11 pathologists participating in a simulation exercise designed to mimic routine pathology workflow; algorithm performance was comparable with an expert pathologist interpreting whole-slide images without time constraints. The area under the curve was 0.994 (best algorithm) vs 0.884 (best pathologist).❞
About that “getting more and more efficient at this”; it’s in the nature of machine learning that every new piece of data improves the neural net being used. So long as it is getting fed new data, which it can process at rate far exceeding humans’ abilities, it will always be constantly improving.
AI makes no more nor less fewer mistakes than humans do: True or False?
False! AI makes fewer, now. This study is from 2021, and it’s only improved since then:
❝Professionals only came to the same conclusions [as each other] approximately 75 per cent of the time. More importantly, machine learning produced fewer decision-making errors than did all the professionals❞
See: AI can make better clinical decisions than humans: study
All that said, we’re not quite at Star Trek levels of “AI can do a human’s job entirely” just yet:
BMJ | Artificial intelligence versus clinicians: pros and cons
To summarize: medical AI is a powerful tool that:
- Makes healthcare more accessible
- Speeds up diagnosis
- Reduces human error
…and yet, for now at least, still requires human oversights, checks and balances.
Essentially: it’s not really about humans vs machines at all. It’s about humans and machines giving each other information, and catching any mistakes made by the other. That way, humans can make more informed decisions, and still keep a “hand on the wheel”.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
53 Studies Later: The Best Way to Improve VO2 Max
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
VO2 max measures maximum oxygen usage during intense exercise and reflects overall health and performance. To have a high VO2 max, efficient functioning of lungs, heart, red blood cells, muscles, and mitochondria is crucial. So, how to get those?
Let’s HIIT it!
High-Intensity Interval Training (HIIT) outperforms moderate-intensity exercise, by a long way. Further, based on the data from the 53 studies mentioned in the title, we can know which of the protocols tested work best, and they are:
- 15×15 Interval Training: 15 seconds sprint (90–95% max heart rate) + 15 seconds active rest (70% max heart rate), repeated 47 times.
- 4×4 Interval Training: 4 minutes sprint (90–95% max heart rate) + 3 minutes active rest (70% max heart rate), repeated 4 times.
Whichever you choose, it is best to then do that 3x per week.
Note that “sprint” can mean any maximum-effort cardio exercise; it doesn’t have to be running specifically. Cycling or swimming, for example, are fine options too, as is jumping rope.
For more on each of these, plus how the science got there, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
How To Do HIIT (Without Wrecking Your Body)
Take care!
Share This Post
-
Voluntary assisted dying is different to suicide. But federal laws conflate them and restrict access to telehealth
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Voluntary assisted dying is now lawful in every Australian state and will soon begin in the Australian Capital Territory.
However, it’s illegal to discuss it via telehealth. That means people who live in rural and remote areas, or those who can’t physically go to see a doctor, may not be able to access the scheme.
A federal private members bill, introduced to parliament last week, aims to change this. So what’s proposed and why is it needed?
What’s wrong with the current laws?
Voluntary assisted dying doesn’t meet the definition of suicide under state laws.
But the Commonwealth Criminal Code prohibits the discussion or dissemination of suicide-related material electronically.
This opens doctors to the risk of criminal prosecution if they discuss voluntary assisted dying via telehealth.
Successive Commonwealth attorneys-general have failed to address the conflict between federal and state laws, despite persistent calls from state attorneys-general for necessary clarity.
This eventually led to voluntary assistant dying doctor Nicholas Carr calling on the Federal Court of Australia to resolve this conflict. Carr sought a declaration to exclude voluntary assisted dying from the definition of suicide under the Criminal Code.
In November, the court declared voluntary assisted dying was considered suicide for the purpose of the Criminal Code. This meant doctors across Australia were prohibited from using telehealth services for voluntary assisted dying consultations.
Last week, independent federal MP Kate Chaney introduced a private members bill to create an exemption for voluntary assisted dying by excluding it as suicide for the purpose of the Criminal Code. Here’s why it’s needed.
Not all patients can physically see a doctor
Defining voluntary assisted dying as suicide in the Criminal Code disproportionately impacts people living in regional and remote areas. People in the country rely on the use of “carriage services”, such as phone and video consultations, to avoid travelling long distances to consult their doctor.
Other people with terminal illnesses, whether in regional or urban areas, may be suffering intolerably and unable to physically attend appointments with doctors.
The prohibition against telehealth goes against the principles of voluntary assisted dying, which are to minimise suffering, maximise quality of life and promote autonomy.
Some people aren’t able to attend doctors’ appointments in person.
Jeffrey M Levine/ShutterstockDoctors don’t want to be involved in ‘suicide’
Equating voluntary assisted dying with suicide has a direct impact on doctors, who fear criminal prosecution due to the prohibition against using telehealth.
Some doctors may decide not to help patients who choose voluntary assisted dying, leaving patients in a state of limbo.
The number of doctors actively participating in voluntary assisted dying is already low. The majority of doctors are located in metropolitan areas or major regional centres, leaving some locations with very few doctors participating in voluntary assisted dying.
It misclassifies deaths
In state law, people dying under voluntary assisted dying have the cause of their death registered as “the disease, illness or medical condition that was the grounds for a person to access voluntary assisted dying”, while the manner of dying is recorded as voluntary assisted dying.
In contrast, only coroners in each state and territory can make a finding of suicide as a cause of death.
In 2017, voluntary assisted dying was defined in the Coroners Act 2008 (Vic) as not a reportable death, and thus not suicide.
The language of suicide is inappropriate for explaining how people make a decision to die with dignity under the lawful practice of voluntary assisted dying.
There is ongoing taboo and stigma attached to suicide. People who opt for and are lawfully eligible to access voluntary assisted dying should not be tainted with the taboo that currently surrounds suicide.
So what is the solution?
The only way to remedy this problem is for the federal government to create an exemption in the Criminal Code to allow telehealth appointments to discuss voluntary assisted dying.
Chaney’s private member’s bill is yet to be debated in federal parliament.
If it’s unsuccessful, the Commonwealth attorney-general should pass regulations to exempt voluntary assisted dying as suicide.
A cooperative approach to resolve this conflict of laws is necessary to ensure doctors don’t risk prosecution for assisting eligible people to access voluntary assisted dying, regional and remote patients have access to voluntary assisted dying, families don’t suffer consequences for the erroneous classification of voluntary assisted dying as suicide, and people accessing voluntary assisted dying are not shrouded with the taboo of suicide when accessing a lawful practice to die with dignity.
Failure to change this will cause unnecessary suffering for patients and doctors alike.
Michaela Estelle Okninski, Lecturer of Law, University of Adelaide; Marc Trabsky, Associate professor, La Trobe University, and Neera Bhatia, Associate Professor in Law, Deakin University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
16/8 Intermittent Fasting For Beginners
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Health Insider explains in super-simple fashion why and how to do Intermittent Fasting (IF), which is something that can sound complicated at first, but becomes very simple and easy once understood.
What do we need to know?
Intermittent fasting (IF) is a good, well-evidenced way to ease your body’s metabolic load, and
give your organs a chance to recover from the strain of digestion and its effects. That’s not just your gastrointestinal organs! It’s your pancreas and liver too, amongst others—this is about glucose metabolism as much as it is about digestion.This, in turn, allows your body some downtime to do its favorite thing, which is: maintenance!
This maintenance takes the form of enhanced cellular apoptosis and autophagy, helping to keep cells young and cancer-free.
In other words, with well-practised intermittent fasting, we can reduce our risk of metabolic disease (including heart disease and diabetes) as well as cancer and neurodegeneration.
You may be wondering: this sounds miraculous; what’s the catch? There are a couple:
- While fasting from food, the body’s enhanced metabolism requires more water, so you’ll need to take extra care keep on top of your hydration (this is one reason why Ramadan fasting, while healthy for most people, is not as healthy as IF—because Ramadan fasting means abstaining from water, too).
- If you are diabetic, and especially if you have Type 1 Diabetes, fasting may not be a safe option for you, since if you get a hypo in the middle of your fasting period, it’s obviously not a good idea to wait another many hours before fixing it.
Extra note on that last one: it’s easy to think “can’t I just lower my bolus insulin instead of eating?” and while superficially yes that will raise your blood sugar levels, it’s because the sugar will be sticking around in your blood, and not actually getting released into the organs that need it. So while your blood glucose monitor may say you’re fine, you will be starving your organs and if you keep it up they may suffer serious damage.
Disclaimer: our standard legal/medical disclaimer applies, and this is intended for educational purposes only; please do speak with your endocrinologist before changing anything you usually do with regard to your blood sugar maintenance.
Ok, back onto the cheerier topic at hand:
Aside from the above: for most people, IF is a remarkably healthful practice in very many ways.
For more on the science, practicalities, and things to do/avoid, enjoy this short (4:53) video:
Click Here If The Embedded Video Doesn’t Load Automatically
Want to know more?
Check out our previous main feature on this topic:
Intermittent Fasting: Mythbusting Edition
Enjoy!
Share This Post
Related Posts
-
Cranberries vs Goji Berries – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing cranberries to goji berries, we picked the cranberries.
Why?
Both are great! And your priorities may differ. Here’s how they stack up:
In terms of macros, goji berries have more protein, carbs, and fiber. This is consistent with them generally being eaten very dried, whereas cranberries are more often eaten fresh or from frozen, or partially rehydrated. In any case, goji berries are the “more food per food” option, so it wins this category. The glycemic indices are both low, by the way, though goji berries are the lower.
When it comes to vitamins, cranberries have more of vitamins B1, B2, B3, B5, B6, B9, E, K, and choline, while goji berries have more of vitamins A and C. Admittedly it’s a lot more, but still, on strength of overall vitamin coverage, the clear winner here is cranberries.
We see a similar story when it comes to minerals: cranberries have more copper, magnesium, manganese, phosphorus, potassium, selenium, and zinc, while goji berries have (a lot) more calcium and iron. Again, by strength of overall mineral coverage, the clear winner here is cranberries.
Cranberries do also have some extra phytochemical benefits, including their prevention/cure status when it comes to UTIs—see our link below for more on that.
At any rate, enjoy either or both, but those are the strengths and weaknesses of these two berries!
Want to learn more?
You might like to read:
- Health Benefits Of Cranberries (But: You’d Better Watch Out)
- Goji Berries: Which Benefits Do They Really Have?
- The Sugary Food That Lowers Blood Sugars ← this is also about goji berries
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Eat Better, Feel Better – by Giada de Laurentis
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In yesterday’s edition of 10almonds, we reviewed Dr. Aujla’s “The Doctor’s Kitchen“; today we’re reviewing a different book about healing through food—in this case, with a special focus on maintaining energy and good health as we get older.
De Laurentis may not be a medical doctor, but she is a TV chef, and not only holds a lot of influence, but also has access to a lot of celebrity doctors and such; that’s reflected a lot in her style and approach here.
The recipes are clear and easy to follow; well-illustrated and nicely laid-out.
This cookbook’s style is less “enjoy this hearty dish of rice and beans with these herbs and spices” and more “you can serve your steak salad with white beans and sweet shallot dressing on a bed of organic quinoa if you haven’t already had your day’s serving of grains, of course”.
It’s a little fancier, in short, and more focused on what to cut out, than what to include. On account of that, this could make it a good contrast to yesterday’s book, which had the opposite focus.
She also recommends assorted adjuvant practices; some that are evidence-based, like intermittent fasting and meditation, and some that are not, like extreme detox-dieting, and acupuncture (which has no bearing on gut health).
Bottom line: if you like the idea of eating for good health, and prefer a touch of celebrity lifestyle to your meals, this one’s a good book for you.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Insider’s Guide To Making Hospital As Comfortable As Possible
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Nobody Likes Surgery, But Here’s How To Make It Much Less Bad
This is Dr. Chris Bonney. He’s an anesthesiologist. If you have a surgery, he wants you to go in feeling calm, and make a quick recovery afterwards, with minimal suffering in between.
Being a patient in a hospital is a bit like being a passenger in an airplane:
- Almost nobody enjoys the thing itself, but we very much want to get to the other side of the experience.
- We have limited freedoms and comforts, and small things can make a big difference between misery and tolerability.
- There are professionals present to look after us, but they are busy and have a lot of other people to tend to too.
So why is it that there are so many resources available full of “tips for travelers” and so few “tips for hospital patients”?
Especially given the relative risks of each, and likelihood, or even near-certainty of coming to at least some harm… One would think “tips for patients” would be more in demand!
Tips for surgery patients, from an insider expert
First, he advises us: empower yourself.
Empowering yourself in this context means:
- Relax—doctors really want you to feel better, quickly. They’re on your side.
- Research—knowledge is power, so research the procedure (and its risks!). Dr. Bonney, himself an anesthesiologist, particularly recommends you learn what specific anesthetic will be used (there are many, and they’re all a bit different!), and what effects (and/or after-effects) that may have.
- Reframe—you’re not just a patient; you’re a customer/client. Many people suffer from MDeity syndrome, and view doctors as authority figures, rather than what they are: service providers.
- Request—if something would make you feel better, ask for it. If it’s information, they will be not only obliged, but also enthusiastic, to give it. If it’s something else, they’ll oblige if they can, and the worst case scenario is something won’t be possible, but you won’t know if you don’t ask.
Next up, help them to help you
There are various ways you can be a useful member of your own care team:
- Go into surgery as healthy as you can. If there’s ever a time to get a little fitter, eat a little healthier, prioritize good quality sleep more, the time approaching your surgery is the time to do this.
- This will help to minimize complications and maximize recovery.
- Take with you any meds you’re taking, or at least have an up-to-date list of what you’re taking. Dr. Bonney has very many times had patients tell him such things as “Well, let me see. I have two little pink ones and a little white one…” and when asked what they’re for they tell him “I have no idea, you’d need to ask my doctor”.
- Help them to help you; have your meds with you, or at least a comprehensive list (including: medication name, dosage, frequency, any special instructions)
- Don’t stop taking your meds unless told to do so. Many people have heard that one should stop taking meds before a surgery, and sometimes that’s true, but often it isn’t. Keep taking them, unless told otherwise.
- If unsure, ask your surgical team in advance (not your own doctor, who will not be as familiar with what will or won’t interfere with a surgery).
Do any preparatory organization well in advance
Consider the following:
- What do you need to take with you? Medications, clothes, toiletries, phone charger, entertainment, headphones, paperwork, cash for the vending machine?
- Will the surgeons need to shave anywhere, and if so, might you prefer doing some other form of depilation (e.g. waxing etc) yourself in advance?
- Is your list of medications ready?
- Who will take you to the hospital and who will bring you back?
- Who will stay with you for the first 24 hours after you’re sent home?
- Is someone available to look after your kids/pets/plants etc?
Be aware of how you do (and don’t) need to fast before surgery
The American Society of Anesthesiologists gives the following fasting guidelines:
- Non-food liquids: fast for at least 2 hours before surgery
- Food liquids or light snacks: fast for at least 6 hours before surgery
- Fried foods, fatty foods, meat: fast for at least 8 hours before surgery
(see the above link for more details)
Dr. Bonney notes that many times he’s had patients who’ve had the worst thirst, or caffeine headache, because of abstaining unnecessarily for the day of the surgery.
Unless told otherwise by your surgical team, you can have black coffee/tea up until two hours before your surgery, and you can and should have water up until two hours before surgery.
Hydration is good for you and you will feel the difference!
Want to know more?
Dr. Bonney has his own website and blog, where he offers lots of advice, including for specific conditions and specific surgeries, with advice for before/during/after your hospital stay.
He also has a book with many more tips like those we shared today:
Calm For Surgery: Supertips For A Smooth Recovery
Take good care of yourself!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:









