Dealing With Hearing Loss
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Hearing is important, not only for convenience, but also for cognitive health—as an inability to participate in what for most people is an important part of social life, has been shown to accelerate cognitive decline:
14 Powerful Strategies To Prevent Dementia ← one of them is looking after your hearing
To this end, we’ve written before about ways to retain (or at least slow the loss of) your hearing, here:
But, what if, despite our best efforts, your hearing is declining regardless, or is already impaired in some way?
Working with the hand we’ve been dealt
So, your hearing is bad and/or deteriorating. Assuming you’ve ruled out possibilities of fixing it, the next step is how to manage this new state of affairs.
One thing to seriously consider, sooner than you think you need to, is using hearing aids. This is because they will not only help you in the obvious practical way, but also, they will slow the associated decline of the parts of your brain that process the language you hear:
ACHIEVE study finds hearing aids cut cognitive decline by 48%
…and here’s the paper itself:
Furthermore, hearing aid use can significantly reduce all-cause mortality:
Your ears are not the only organs
Remember, today’s about dealing with hearing loss, not preventing it (for preventing it, see the second link we dropped up top).
With this in mind: do not underestimate the usefulness of learning to lipread.
Lipreading is not a panacea; it has its limitations:
- You can’t lipread an audio-only phonecall, or a podcast, or the radio
- You can’t lipread a video call if the video quality is poor
- You can’t lipread if someone is wearing a mask (as in many healthcare settings)
- You can’t lipread multiple people at once; you have to choose whose mouth to watch (or at least, you will miss the first word(s) each time while switching)
- You can’t lipread during sex if your/their face is somewhere else (may seem like a silly example, but actually communication can be important in sex, and the number of times this writer has had to say “Say again?” in intimate moments is ridiculous)
However, it can also make a huge difference the rest of the time, and can even be a superpower in times/places when other people’s hearing is nullified, such as a noisy environment, or a video call in which someone’s mic isn’t working.
The good news is, it’s really very easy to learn to lipread. There are many valid ways (often involving consciously memorizing mouth-shapes from charts, and then putting them together one by one to build a vocabulary), but this writer recommends a more organic, less effort-intensive approach:
- Choose a video of someone who speaks clearly, and for which video you already know what is being said (such as by using subtitles first, or a transcript, or perhaps the person is delivering a famous speech or reciting a poem that you know well, or it’s your favorite movie that you’ve watched many times).
- Now watch it with the sound off (assuming you do normally have some hearing; if you don’t, then you’re probably ahead of the game here) and just pay close attention to the lips. Do this on repeat; soon you’ll be able to “hear” the sounds as you see them made.
- Now choose a video of someone who speaks clearly, for which video you do not already know what is being said. You’ll probably only get parts of it at first; that’s ok.
- Now learn the rest of what they said in that video (by reading a transcript or such), and use it like you used the first video.
- Now repeat steps 3 and 4 until you are lipreading most people easily unless there is some clear obfuscation preventing you.
This process should not take long, as there are only about 44 phonemes (distinct sounds) in English, and once you’ve learned them, you’re set. If you speak more languages, those same 44 phonemes should cover most of most of them, but if not, just repeat the above process with the next language.
Remember, if you have at least some hearing, then most of the time your lipreading and your hearing are going to be working together, and neither will be as strong without the other—but if necessary, well-practised lipreading can indeed often stand in for hearing when hearing isn’t available.
A note on sign language:
Sign language is great, and cool, and useful. However, it’s only as useful as the people who know it, which means that it’s top-tier in the Deaf community (where people will dodge hearing-related cognitive decline entirely, because their social interaction is predominantly signed rather than spoken), and can be useful with close friends or family members who learn it (or at least learn some), but isn’t as useful in most of the wider world when people don’t know it. But if you do want to learn it, don’t let that hold you back—be the change you want to see!
Most of our readers are American, so here’s a good starting place for American Sign Language ← this is a list of mostly-free resources
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Women Rowing North – by Dr. Mary Pipher
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Ageism is rife, as is misogyny. And those can be internalized too, and compounded as they intersect.
Clinical psychologist Dr. Mary Pipher, herself 75, writes for us a guidebook of, as the subtitle goes, “navigating life’s currents and flourishing as we age”.
The book does assume, by the way, that the reader is…
- a woman, and
- getting old (if not already old)
However, the lessons the book imparts are vital for women of any age, and valuable as a matter of insight and perspective for any reader.
Dr. Pipher takes us on a tour of aging as a woman, and what parts of it we can make our own, do things our way, and take what joy we can from it.
Nor is the book given to “toxic positivity” though—it also deals with themes of hardship, frustration, and loss.
When it comes to those elements, the book is… honest, human, and raw. But also, an exhortation to hope, beauty, and a carpe diem attitude.
Bottom line: this book is highly recommendable to anyone of any age; life is precious and can be short. And be we blessed with many long years, this book serves as a guide to making each one of them count.
Click here to check out Women Rowing North—it really is worth it
Share This Post
-
Good news: midlife health is about more than a waist measurement. Here’s why
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You’re not in your 20s or 30s anymore and you know regular health checks are important. So you go to your GP. During the appointment they measure your waist. They might also check your weight. Looking concerned, they recommend some lifestyle changes.
GPs and health professionals commonly measure waist circumference as a vital sign for health. This is a better indicator than body mass index (BMI) of the amount of intra-abdominal fat. This is the really risky fat around and within the organs that can drive heart disease and metabolic disorders such as type 2 diabetes.
Men are at greatly increased risk of health issues if their waist circumference is greater than 102 centimetres. Women are considered to be at greater risk with a waist circumference of 88 centimetres or more. More than two-thirds of Australian adults have waist measurements that put them at an increased risk of disease. An even better indicator is waist circumference divided by height or waist-to-height ratio.
But we know people (especially women) have a propensity to gain weight around their middle during midlife, which can be very hard to control. Are they doomed to ill health? It turns out that, although such measurements are important, they are not the whole story when it comes to your risk of disease and death.
How much is too much?
Having a waist circumference to height ratio larger than 0.5 is associated with greater risk of chronic disease as well as premature death and this applies in adults of any age. A healthy waist-to-height ratio is between 0.4 to 0.49. A ratio of 0.6 or more places a person at the highest risk of disease.
Some experts recommend waist circumference be routinely measured in patients during health appointments. This can kick off a discussion about their risk of chronic diseases and how they might address this.
Excessive body fat and the associated health problems manifest more strongly during midlife. A range of social, personal and physiological factors come together to make it more difficult to control waist circumference as we age. Metabolism tends to slow down mainly due to decreasing muscle mass because people do less vigorous physical activity, in particular resistance exercise.
For women, hormone levels begin changing in mid-life and this also stimulates increased fat levels particularly around the abdomen. At the same time, this life phase (often involving job responsibilities, parenting and caring for ageing parents) is when elevated stress can lead to increased cortisol which causes fat gain in the abdominal region.
Midlife can also bring poorer sleep patterns. These contribute to fat gain with disruption to the hormones that control appetite.
Finally, your family history and genetics can make you predisposed to gaining more abdominal fat.
Why the waist?
This intra-abdominal or visceral fat is much more metabolically active (it has a greater impact on body organs and systems) than the fat under the skin (subcutaneous fat).
Visceral fat surrounds and infiltrates major organs such as the liver, pancreas and intestines, releasing a variety of chemicals (hormones, inflammatory signals, and fatty acids). These affect inflammation, lipid metabolism, cholesterol levels and insulin resistance, contributing to the development of chronic illnesses.
Exercise can limit visceral fat gains in mid-life. Shutterstock/Zamrznuti tonovi The issue is particularly evident during menopause. In addition to the direct effects of hormone changes, declining levels of oestrogen change brain function, mood and motivation. These psychological alterations can result in reduced physical activity and increased eating – often of comfort foods high in sugar and fat.
But these outcomes are not inevitable. Diet, exercise and managing mental health can limit visceral fat gains in mid-life. And importantly, the waist circumference (and ratio to height) is just one measure of human health. There are so many other aspects of body composition, exercise and diet. These can have much larger influence on a person’s health.
Muscle matters
The quantity and quality of skeletal muscle (attached to bones to produce movement) a person has makes a big difference to their heart, lung, metabolic, immune, neurological and mental health as well as their physical function.
On current evidence, it is equally or more important for health and longevity to have higher muscle mass and better cardiorespiratory (aerobic) fitness than waist circumference within the healthy range.
So, if a person does have an excessive waist circumference, but they are also sedentary and have less muscle mass and aerobic fitness, then the recommendation would be to focus on an appropriate exercise program. The fitness deficits should be addressed as priority rather than worry about fat loss.
Conversely, a person with low visceral fat levels is not necessarily fit and healthy and may have quite poor aerobic fitness, muscle mass, and strength. The research evidence is that these vital signs of health – how strong a person is, the quality of their diet and how well their heart, circulation and lungs are working – are more predictive of risk of disease and death than how thin or fat a person is.
For example, a 2017 Dutch study followed overweight and obese people for 15 years and found people who were very physically active had no increased heart disease risk than “normal weight” participants.
Getting moving is important advice
Physical activity has many benefits. Exercise can counter a lot of the negative behavioural and physiological changes that are occurring during midlife including for people going through menopause.
And regular exercise reduces the tendency to use food and drink to help manage what can be a quite difficult time in life.
Measuring your waist circumference and monitoring your weight remains important. If the measures exceed the values listed above, then it is certainly a good idea to make some changes. Exercise is effective for fat loss and in particular decreasing visceral fat with greater effectiveness when combined with dietary restriction of energy intake. Importantly, any fat loss program – whether through drugs, diet or surgery – is also a muscle loss program unless resistance exercise is part of the program. Talking about your overall health with a doctor is a great place to start.
Accredited exercise physiologists and accredited practising dietitians are the most appropriate allied health professionals to assess your physical structure, fitness and diet and work with you to get a plan in place to improve your health, fitness and reduce your current and future health risks.
Rob Newton, Professor of Exercise Medicine, Edith Cowan University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Pasteurization: What It Does And Doesn’t Do
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Pasteurization’s Effect On Risks & Nutrients
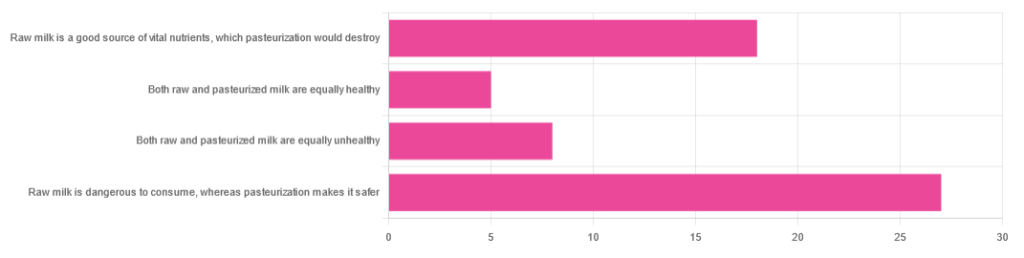
In Wednesday’s newsletter, we asked you for your health-related opinions of raw (cow’s) milk, and got the above-depicted, below-described, set of responses:
- About 47% said “raw milk is dangerous to consume, whereas pasteurization makes it safer”
- About 31% said “raw milk is a good source of vital nutrients which pasteurization would destroy”
- About 14% said “both raw milk and pasteurized milk are equally unhealthy”
- About 9% said “both raw milk and pasteurized milk are equally healthy”
Quite polarizing! So, what does the science say?
“Raw milk is dangerous to consume, whereas pasteurization makes it safer: True or False?”
True! Coincidentally, the 47% who voted for this are mirrored by the 47% of the general US population in a similar poll, deciding between the options of whether raw milk is less safe to drink (47%), just as safe to drink (15%), safer to drink (9%), or not sure (30%):
Public Fails to Appreciate Risk of Consuming Raw Milk, Survey Finds
As for what those risks are, by the way, unpasteurized dairy products are estimated to cause 840x more illness and 45x more hospitalizations than pasteurized products.
This is because unpasteurized milk can (and often does) contain E. coli, Listeria, Salmonella, Cryptosporidium, and other such unpleasantries, which pasteurization kills.
Source for both of the above claims:
(we know the title sounds vague, but all this information is easily visible in the abstract, specifically, the first two paragraphs)
Raw milk is a good source of vital nutrients which pasteurization would destroy: True or False?
False! Whether it’s a “good” source can be debated depending on other factors (e.g., if we considered milk’s inflammatory qualities against its positive nutritional content), but it’s undeniably a rich source. However, pasteurization doesn’t destroy or damage those nutrients.
Incidentally, in the same survey we linked up top, 16% of the general US public believed that pasteurization destroys nutrients, while 41% were not sure (and 43% knew that it doesn’t).
Note: for our confidence here, we are skipping over studies published by, for example, dairy farming lobbies and so forth. Those do agree, by the way, but nevertheless we like sources to be as unbiased as possible. The FDA, which is not completely unbiased, has produced a good list of references for this, about half of which we would consider biased, and half unbiased; the clue is generally in the journal names. For example, Food Chemistry and the Journal of Food Science and Journal of Nutrition are probably less biased than the International Dairy Association and the Journal of Dairy Science:
FDA | Raw Milk Misconceptions and the Danger of Raw Milk Consumption
this page covers a lot of other myths too, more than we have room to “bust” here, but it’s very interesting reading and we recommend to check it out!
Notably, we also weren’t able to find any refutation by counterexample on PubMed, with the very slight exception that some studies sometimes found that in the case of milks that were of low quality, pasteurization can reduce the vitamin E content while increasing the vitamin A content. For most milks however, no significant change was found, and in all cases we looked at, B-vitamins were comparable and vitamin D, popularly touted as a benefit of cow’s milk, is actually added later in any case. And, importantly, because this is a common argument, no change in lipid profiles appears to be findable either.
In science, when something has been well-studied and there aren’t clear refutations by counterexample, and the weight of evidence is clearly very much tipped into one camp, that usually means that camp has it right.
Milk generally is good/bad for the health: True or False?
True or False, depending on what we want to look at. It’s definitely not good for inflammation, but the whole it seems to be cancer-neutral and only increases heart disease risk very slightly:
- Keep Inflammation At Bay ← short version is milk is bad, fermented milk products are fine in moderation
- Is Dairy Scary? ← short version is that milk is neither good nor terrible; fermented dairy products however are health-positive in numerous ways when consumed in moderation
You may be wondering…
…how this goes for the safety of dairy products when it comes to the bird flu currently affecting dairy cows, so:
Take care!
Share This Post
Related Posts
-
I’ve been given opioids after surgery to take at home. What do I need to know?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Opioids are commonly prescribed when you’re discharged from hospital after surgery to help manage pain at home.
These strong painkillers may have unwanted side effects or harms, such as constipation, drowsiness or the risk of dependence.
However, there are steps you can take to minimise those harms and use opioids more safely as you recover from surgery.
Flystock/Shutterstock Which types of opioids are most common?
The most commonly prescribed opioids after surgery in Australia are oxycodone (brand names include Endone, OxyNorm) and tapentadol (Palexia).
In fact, about half of new oxycodone prescriptions in Australia occur after a recent hospital visit.
Most commonly, people will be given immediate-release opioids for their pain. These are quick-acting and are used to manage short-term pain.
Because they work quickly, their dose can be easily adjusted to manage current pain levels. Your doctor will provide instructions on how to adjust the dosage based on your pain levels.
Then there are slow-release opioids, which are specially formulated to slowly release the dose over about half to a full day. These may have “sustained-release”, “controlled-release” or “extended-release” on the box.
Slow-release formulations are primarily used for chronic or long-term pain. The slow-release form means the medicine does not have to be taken as often. However, it takes longer to have an effect compared with immediate-release, so it is not commonly used after surgery.
Controlling your pain after surgery is important. This allows you get up and start moving sooner, and recover faster. Moving around sooner after surgery prevents muscle wasting and harms associated with immobility, such as bed sores and blood clots.
Everyone’s pain levels and needs for pain medicines are different. Pain levels also decrease as your surgical wound heals, so you may need to take less of your medicine as you recover.
But there are also risks
As mentioned above, side effects of opioids include constipation and feeling drowsy or nauseous. The drowsiness can also make you more likely to fall over.
Opioids prescribed to manage pain at home after surgery are usually prescribed for short-term use.
But up to one in ten Australians still take them up to four months after surgery. One study found people didn’t know how to safely stop taking opioids.
Such long-term opioid use may lead to dependence and overdose. It can also reduce the medicine’s effectiveness. That’s because your body becomes used to the opioid and needs more of it to have the same effect.
Dependency and side effects are also more common with slow-release opioids than immediate-release opioids. This is because people are usually on slow-release opioids for longer.
Then there are concerns about “leftover” opioids. One study found 40% of participants were prescribed more than twice the amount they needed.
This results in unused opioids at home, which can be dangerous to the person and their family. Storing leftover opioids at home increases the risk of taking too much, sharing with others inappropriately, and using without doctor supervision.
Don’t stockpile your leftover opioids in your medicine cupboard. Take them to your pharmacy for safe disposal. Archer Photo/Shutterstock How to mimimise the risks
Before using opioids, speak to your doctor or pharmacist about using over-the-counter pain medicines such as paracetamol or anti-inflammatories such as ibuprofen (for example, Nurofen, Brufen) or diclofenac (for example, Voltaren, Fenac).
These can be quite effective at controlling pain and will lessen your need for opioids. They can often be used instead of opioids, but in some cases a combination of both is needed.
Other techniques to manage pain include physiotherapy, exercise, heat packs or ice packs. Speak to your doctor or pharmacist to discuss which techniques would benefit you the most.
However, if you do need opioids, there are some ways to make sure you use them safely and effectively:
- ask for immediate-release rather than slow-release opioids to lower your risk of side effects
- do not drink alcohol or take sleeping tablets while on opioids. This can increase any drowsiness, and lead to reduced alertness and slower breathing
- as you may be at higher risk of falls, remove trip hazards from your home and make sure you can safely get up off the sofa or bed and to the bathroom or kitchen
- before starting opioids, have a plan in place with your doctor or pharmacist about how and when to stop taking them. Opioids after surgery are ideally taken at the lowest possible dose for the shortest length of time.
A heat pack may help with pain relief, so you end up using fewer painkillers. New Africa/Shutterstock If you’re concerned about side effects
If you are concerned about side effects while taking opioids, speak to your pharmacist or doctor. Side effects include:
- constipation – your pharmacist will be able to give you lifestyle advice and recommend laxatives
- drowsiness – do not drive or operate heavy machinery. If you’re trying to stay awake during the day, but keep falling asleep, your dose may be too high and you should contact your doctor
- weakness and slowed breathing – this may be a sign of a more serious side effect such as respiratory depression which requires medical attention. Contact your doctor immediately.
If you’re having trouble stopping opioids
Talk to your doctor or pharmacist if you’re having trouble stopping opioids. They can give you alternatives to manage the pain and provide advice on gradually lowering your dose.
You may experience withdrawal effects, such as agitation, anxiety and insomnia, but your doctor and pharmacist can help you manage these.
How about leftover opioids?
After you have finished using opioids, take any leftovers to your local pharmacy to dispose of them safely, free of charge.
Do not share opioids with others and keep them away from others in the house who do not need them, as opioids can cause unintended harms if not used under the supervision of a medical professional. This could include accidental ingestion by children.
For more information, speak to your pharmacist or doctor. Choosing Wisely Australia also has free online information about managing pain and opioid medicines.
Katelyn Jauregui, PhD Candidate and Clinical Pharmacist, School of Pharmacy, Faculty of Medicine and Health, University of Sydney; Asad Patanwala, Professor, Sydney School of Pharmacy, University of Sydney; Jonathan Penm, Senior lecturer, School of Pharmacy, University of Sydney, and Shania Liu, Postdoctoral Research Fellow, Faculty of Medicine and Dentistry, University of Alberta
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Chorus or Cacophony? Cicada Song Hits Some Ears Harder Than Others
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
ST. LOUIS — Shhhooo. Wee-uuu. Chick, chick, chick. That’s the sound of three different cicada species. For some people, those sounds are the song of the summer. Others wish the insects would turn it down. The cacophony can be especially irritating for people on the autism spectrum who have hearing sensitivity.
Warren Rickly, 14, lives in suburban south St. Louis County, Missouri. Warren, who has autism, was at the bus stop recently waiting for his younger brother when the sound of cicadas became too much to bear.
“He said it sounds like there’s always a train running next to him,” his mother, Jamie Reed, said.
Warren told her the noise hurt.
Starting this spring, trillions of the red-eyed insects crawled their way out of the ground across the Midwest and Southeast. It’s part of a rare simultaneous emergence of two broods — one that appears every 13 years, the other every 17.
The noisy insects can be stressful. People with autism can have a sensitivity to texture, brightness, and sound.
“I think the difference for individuals with autism is the level of intensity or how upsetting some of these sensory differences are,” said Rachel Follmer, a developmental and behavioral pediatrician at Lurie Children’s Hospital in Chicago.
“It can get to the extreme where it can cause physical discomfort,” she said.
When a large group of cicadas starts to sing, the chorus can be as loud as a motorcycle. Researchers at the University of Missouri-St. Louis this year crowdsourced cicada noise levels as high as 86 decibels, about as loud as a food blender.
That can be stressful, not melodic, Follmer said.
To help children cope, she suggests giving them a primer before they encounter a noisy situation. For cicadas, that could mean explaining what they are, that they don’t bite or sting, and that they’ll be here for just a short time.
“When something is uncomfortable, not having power in that situation can be very scary for a lot of individuals, whether you’re on the spectrum or not,” Follmer said.
Jamie Reed’s family has been using this and other strategies to help her son. Warren wears noise-canceling headphones, listens to music, and has been teaching himself about cicadas.
“For him, researching it and looking into it I think grounds him a little bit,” Reed said.
Fatima Husain is a professor and neuroscientist at the University of Illinois Urbana-Champaign and studies how the brain processes sound. She said people with tinnitus may also struggle with cicada song.
Tinnitus, a ringing or other noise in the ears, is a person’s perception of sound without an external source.
“Some people say it sounds like buzzing, like wind blowing through trees, and ironically, quite a few people say it sounds like cicadas,” Husain said.
For most people with tinnitus the cicada’s song is harmless background noise, according to Husain, but for others the ringing can prevent easy conversation or sleep. Those with tinnitus are also more likely to have anxiety or depression. A loud persistent sound, like singing cicadas, can make someone’s tinnitus worse, Husain said.
It’s not always bad, though. The cicada’s song can also be a relief.
For some, tinnitus gets worse in a quiet environment. Husain said she’s seen reports this year of patients saying the cicadas’ song has been like soothing white noise.
“The sound is loud enough that in some ways it’s drowning their internal tinnitus,” Husain said.
As loud as the cicadas can be, they won’t necessarily damage anyone’s hearing, according to the Centers for Disease Control and Prevention. Hearing loss builds up over time from repeated exposure to loud sounds. Cicadas aren’t loud enough for long enough to do lasting damage, Husain said.
Everyday sources of noise come with a higher risk. Husain said constant exposure to loud highways, an airport, industrial sites, or household appliances like blenders and hair dryers can be a concern. And they can take a toll on someone’s emotional well-being.
“If you are being exposed to very loud sounds for a part of your school day or your working day, it may make you more stressed out; it may make you more angry about things,” she said.
Unlike the highway or an airport, cicadas won’t be around long. Most of the current brood will be gone in the next few weeks. Just in time for another noisy summer event: the Fourth of July.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
For Many Rural Women, Finding Maternity Care Outweighs Concerns About Abortion Access
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
BAKER CITY, Ore. — In what has become a routine event in rural America, a hospital maternity ward closed in 2023 in this small Oregon town about an hour from the Idaho border.
For Shyanne McCoy, 23, that meant the closest hospital with an obstetrician on staff when she was pregnant was a 45-mile drive away over a mountain pass.
When McCoy developed symptoms of preeclampsia last January, she felt she had the best chance of getting the care she needed at a larger hospital in Boise, Idaho, two hours away. She spent the final week of her pregnancy there, too far from home to risk leaving, before giving birth to her daughter.
Six months later, she said it seems clear to her that the health care needs of rural young women like her are largely ignored.
For McCoy and others, figuring out how to obtain adequate care to safely have a baby in Baker City has quickly eclipsed concerns about another medical service lacking in the area: abortion. But in Oregon and elsewhere in the country, progressive lawmakers’ attempts to expand abortion access sometimes clash with rural constituencies.
Oregon is considered one of the most protective states in the country when it comes to abortion. There are no legal limits on when someone can receive an abortion in the state, and the service is covered by its Medicaid system. Still, efforts to expand access in the rural, largely conservative areas that cover most of the state have encountered resistance and incredulity.
It’s a divide that has played out in elections in such states as Nevada, where voters passed a ballot measure in November that seeks to codify abortion protections in the state constitution. Residents in several rural counties opposed the measure.
In Oregon, during the months just before the Baker City closure was announced, Democratic state lawmakers were focused on a proposed pilot program that would launch two mobile reproductive health care clinics in rural areas. The bill specified that the van-based clinics would include abortion services.
State Rep. Christine Goodwin, a Republican from a southwestern Oregon district, called the proposal the “latest example” of urban legislators telling rural leaders what their communities need.
The mobile health clinic pilot was eventually removed from the bill that was under discussion. That means no new abortion options in Oregon’s Baker County — and no new state-funded maternity care either.
“I think if you expanded rural access in this community to abortions before you extended access to maternal health care, you would have an uprising on your hands,” said Paige Witham, 27, a member of the Baker County health care steering committee and the mother of two children, including an infant born in October.
A study published in JAMA in early December that examined nearly 5,000 acute care hospitals found that by 2022, 52% of rural hospitals lacked obstetrics care after more than a decade of unit closures. The health implications of those closures for young women, the population most likely to need pregnancy care, and their babies can be significant. Research has shown that added distance between a patient and obstetric care increases the likelihood the baby will be admitted to a neonatal intensive care unit, or NICU.
Witham said that while she does not support abortion, she believes the government should not “legislate it away completely.” She said that unless the government provides far more support for young families, like free child care and better mental health care, abortion should remain legal.
Conversations with a liberal school board member, a moderate owner of a timber company, members of Baker City’s Republican Party chapter, a local doula, several pregnant women, and the director of the Baker County Health Department — many of whom were not rigidly opposed to abortion — all turned up the same answer: No mobile clinics offering abortions here, please.
Kelle Osborn, a nurse supervisor for the Baker County Health Department, loved the idea of a mobile clinic that would provide education and birth control services to people in outlying areas. She was less thrilled about including abortion services in a clinic on wheels.
“It’s not something that should just be handed out from a mobile van,” she said of abortion services. She said people in her conservative rural county would probably avoid using the clinics for anything if they were understood to provide abortion services.
Both Osborn and Meghan Chancey, the health department’s director, said they would rank many health care priorities higher, including the need for a general surgeon, an ICU, and a dialysis clinic.
Nationally, reproductive health care services of all types tend to be limited for people in rural areas, even within states that protect abortion access. More than two-thirds of people in “maternity care deserts” — all of which are in rural counties — must drive more than a half-hour to get obstetric care, according to a 2024 March of Dimes report. For people in the Southern states where lawmakers installed abortion bans, abortion care can be up to 700 miles away, according to a data analysis by Axios.
Nathan Defrees grew up in Baker City and has practiced medicine here since 2017. He works for a family medicine clinic. If a patient asks about abortion, he provides information about where and how one can be obtained, but he doesn’t offer abortions himself.
“There’s not a lot of anonymity in small towns for physicians who provide that care,” he said. “Many of us aren’t willing to sacrifice the rest of our career for that.”
He also pointed to the small number of patients requesting the service locally. Just six people living in Baker County had an abortion in 2023, according to data from the Oregon Department of Public Health. Meanwhile, 125 residents had a baby that year.
A doctor with obstetric training living in another rural part of the state has chosen to quietly provide early-stage abortions when asked. The doctor, concerned for their family’s safety in the small, conservative town where they live, asked not to be identified.
The idea that better access to abortion is not needed in rural areas seems naive, the doctor said. People most in need of abortion often don’t have access to any medical service not already available in town, the doctor pointed out. The first patient the doctor provided an abortion for at the clinic was a meth user with no resources to travel or to manage an at-home medication abortion.
“It seemed entirely inappropriate for me to turn her away for care I had the training and the tools to do,” the doctor said.
Defrees said it has been easier for Baker County residents to get an abortion since the U.S. Supreme Court overturned Roe v. Wade.
A new Planned Parenthood clinic in Ontario, Oregon, 70 miles away in neighboring Malheur County, was built primarily to provide services to people from the Boise metro area, but it also created an option for many living in rural eastern Oregon.
Idaho is one of the 16 states with near-total bans on abortion. Like many states with bans, Idaho has struggled to maintain its already small fleet of fetal medicine doctors. The loss of regional expertise touches Baker City, too, Defrees said.
For example, he said, the treatment plan for women who have a desired pregnancy but need a termination for medical reasons is now far less clear. “It used to be those folks could go to Boise,” he said. “Now they can’t. That does put us in a bind.”
Portland is the next closest option for that type of care, and that means a 300-mile drive along a set of highways that can be treacherous in winter.
“It’s a lot scarier to be pregnant now in Baker City than it ever has been,” Defrees said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
This article first appeared on KFF Health News and is republished here under a Creative Commons license.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: