Oat Milk vs Almond Milk – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing oat milk to almond milk, we picked the almond milk.
Why?
This one’s quite straightforward, and no, it’s not just our bias for almonds
Rather, almonds contain a lot more vitamins and minerals, all of which usually make it into the milk.
Oat milk is still a fine choice though, and has a very high soluble fiber content, which is great for your heart.
Just make sure you get versions without added sugar or other unpleasantries! You can always make your own at home, too.
You can read a bit more about the pros and cons of various plant milks here:
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The 5 Love Languages Gone Wrong
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Levelling up the 5 love languages
The saying “happy wife; happy life” certainly goes regardless of gender, and if we’re partnered, it’s difficult to thrive in our individual lives if we’re not thriving as a couple. So, with the usual note that mental health is also just health, let’s take a look at getting beyond the basics of a well-known, often clumsily-applied model:
The 5 love languages
You’re probably familiar with “the 5 love languages”, as developed by Dr. Gary Chapman. If not, they are:
- Acts of Service
- Gift-Giving
- Physical Touch
- Quality Time
- Words of Affirmation
The idea is that we each weight these differently, and problems can arise when a couple are “speaking a different language”.
So, is this a basic compatibility test?
It doesn’t have to be!
We can, if we’re aware of each other’s primary love languages, make an effort to do a thing we wouldn’t necessarily do automatically, to ensure they’re loved the way they need to be.
But…
What a lot of people overlook is that we can also have different primary love languages for giving and for receiving. And, missing that can mean that even taking each other’s primarily love languages into account, efforts to make a partner feel loved, or to feel loved oneself, can miss 50% of the time.
For example, I (your writer here today, hi) could be asked my primary love language and respond without hesitation “Acts of Service!” because that’s my go-to for expressing love.
I’m the person who’ll run around bringing drinks, do all the housework, and without being indelicate, will tend towards giving in the bedroom. But…
A partner trying to act on that information to make me feel loved by giving Acts of Service would be doomed to catastrophic failure, because my knee-jerk reaction would be “No, here, let me do that for you!”
So it’s important for partners to ask each other…
- Not: “what’s your primary love language?” ❌
- But: “what’s your primary way of expressing love?” ✅
- And: “which love language makes you feel most loved?” ✅
For what it’s worth, I thrive on Words of Affirmation, so thanks again to everyone who leaves kind feedback on our articles! It lets me know I provided a good Act of Service
So far, so simple, right? You and your partner (or: other person! Because as we’ve just seen, these go for all kinds of dynamics, not just romantic partnerships) need to be aware of each other’s preferred love languages for giving and receiving.
But…
There’s another pitfall that many fall into, and that’s assuming that the other person has the same idea about what a given love language means, when there’s more to clarify.
For example:
- Acts of Service: is it more important that the service be useful, or that it took effort?
- Gift-Giving: is it better that a gift be more expensive, or more thoughtful and personal?
- Physical Touch: what counts here? If we’re shoulder-to-shoulder on the couch, is that physical touch or is something more active needed?
- Quality Time: does it count if we’re both doing our own thing but together in the same room, comfortable in silence together? Or does it need to be a more active and involved activity together? And is it quality time if we’re at a social event together, or does it need to be just us?
- Words of Affirmation: what, exactly, do we need to hear? For romantic partners, “I love you” can often be important, but is there something else we need to hear? Perhaps a “because…”, or perhaps a “so much that…”, or perhaps something else entirely? Does it no longer count if we have to put the words in our partner’s mouth, or is that just good two-way communication?
Bottom line:
There’s a lot more to this than a “What’s your love language?” click-through quiz, but with a little application and good communication, this model can really resolve a lot of would-be problems that can grow from feeling unappreciated or such. And, the same principles go just the same for friends and others as they do for romantic partners.
In short, it’s one of the keys to good interpersonal relationships in general—something critical for our overall well-being!
Share This Post
-
‘Disease X’: What it is (and isn’t)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What you need to know
- In January 2024, the World Economic Forum hosted an event called Preparing for Disease X to discuss strategies to improve international pandemic response.
- Disease X is a term used in epidemiology to refer to potential disease threats. It is not a real disease or a global conspiracy.
- Preparation to prevent and respond to future pandemics is a necessary part of global health to keep us all safer.
During the World Economic Forum’s 54th annual meeting in Davos, Switzerland, global health experts discussed ways to strengthen health care systems in preparation for future pandemics. Conspiracy theories quickly began circulating posts about the event and the fictional disease at its center, so-called Disease X.
What is Disease X?
In 2018, the World Health Organization added Disease X to its list of Blueprint Priority Diseases that are public health risks. But, unlike the other diseases on the list, Disease X doesn’t exist. The term represents a hypothetical human disease capable of causing a pandemic. Although experts don’t know what the next Disease X will be, they can make educated guesses about where and how it may emerge—and how we can prepare for it.
Why are we hearing about Disease X now?
COVID-19 has been the deadliest infectious disease outbreak of the 21st century. It’s also an example of a Disease X: a previously unknown pathogen that spreads rapidly around the world, claiming millions of lives.
When the WEF hosted a panel of experts to discuss Disease X, it was the first exposure that many people had to a concept that global health experts have been discussing since 2018.
Even before the routine pandemic preparedness event took place, online conspiracy theorists began circulating false claims that those discussing and preparing for Disease X had sinister motives, underscoring how widespread distrust of global health entities has become in the wake of the COVID-19 pandemic.
Why does Disease X matter?
Epidemiologists use concepts like Disease X to plan for future outbreaks and avoid the mistakes of past outbreaks. The COVID-19 pandemic and the recent non-endemic outbreak of mpox highlight the importance of global coordination to efficiently prevent and respond to disease outbreaks.
Pandemics are inevitable, but the scale of their destruction doesn’t have to be. Major disease outbreaks are likely to become more frequent due to the impacts of climate change. Preparing for a pandemic now helps ensure that the world is better equipped to handle the next one.
This article first appeared on Public Good News and is republished here under a Creative Commons license.
Share This Post
-
WHO Overturns Dogma on Airborne Disease Spread. The CDC Might Not Act on It.
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The World Health Organization has issued a report that transforms how the world understands respiratory infections like covid-19, influenza, and measles.
Motivated by grave missteps in the pandemic, the WHO convened about 50 experts in virology, epidemiology, aerosol science, and bioengineering, among other specialties, who spent two years poring through the evidence on how airborne viruses and bacteria spread.
However, the WHO report stops short of prescribing actions that governments, hospitals, and the public should take in response. It remains to be seen how the Centers for Disease Control and Prevention will act on this information in its own guidance for infection control in health care settings.
The WHO concluded that airborne transmission occurs as sick people exhale pathogens that remain suspended in the air, contained in tiny particles of saliva and mucus that are inhaled by others.
While it may seem obvious, and some researchers have pushed for this acknowledgment for more than a decade, an alternative dogma persisted — which kept health authorities from saying that covid was airborne for many months into the pandemic.
Specifically, they relied on a traditional notion that respiratory viruses spread mainly through droplets spewed out of an infected person’s nose or mouth. These droplets infect others by landing directly in their mouth, nose, or eyes — or they get carried into these orifices on droplet-contaminated fingers. Although these routes of transmission still happen, particularly among young children, experts have concluded that many respiratory infections spread as people simply breathe in virus-laden air.
“This is a complete U-turn,” said Julian Tang, a clinical virologist at the University of Leicester in the United Kingdom, who advised the WHO on the report. He also helped the agency create an online tool to assess the risk of airborne transmission indoors.
Peg Seminario, an occupational health and safety specialist in Bethesda, Maryland, welcomed the shift after years of resistance from health authorities. “The dogma that droplets are a major mode of transmission is the ‘flat Earth’ position now,” she said. “Hurray! We are finally recognizing that the world is round.”
The change puts fresh emphasis on the need to improve ventilation indoors and stockpile quality face masks before the next airborne disease explodes. Far from a remote possibility, measles is on the rise this year and the H5N1 bird flu is spreading among cattle in several states. Scientists worry that as the H5N1 virus spends more time in mammals, it could evolve to more easily infect people and spread among them through the air.
Traditional beliefs on droplet transmission help explain why the WHO and the CDC focused so acutely on hand-washing and surface-cleaning at the beginning of the pandemic. Such advice overwhelmed recommendations for N95 masks that filter out most virus-laden particles suspended in the air. Employers denied many health care workers access to N95s, insisting that only those routinely working within feet of covid patients needed them. More than 3,600 health care workers died in the first year of the pandemic, many due to a lack of protection.
However, a committee advising the CDC appears poised to brush aside the updated science when it comes to its pending guidance on health care facilities.
Lisa Brosseau, an aerosol expert and a consultant at the Center for Infectious Disease Research and Policy in Minnesota, warns of a repeat of 2020 if that happens.
“The rubber hits the road when you make decisions on how to protect people,” Brosseau said. “Aerosol scientists may see this report as a big win because they think everything will now follow from the science. But that’s not how this works and there are still major barriers.”
Money is one. If a respiratory disease spreads through inhalation, it means that people can lower their risk of infection indoors through sometimes costly methods to clean the air, such as mechanical ventilation and using air purifiers, and wearing an N95 mask. The CDC has so far been reluctant to press for such measures, as it updates foundational guidelines on curbing airborne infections in hospitals, nursing homes, prisons, and other facilities that provide health care. This year, a committee advising the CDC released a draft guidance that differs significantly from the WHO report.
Whereas the WHO report doesn’t characterize airborne viruses and bacteria as traveling short distances or long, the CDC draft maintains those traditional categories. It prescribes looser-fitting surgical masks rather than N95s for pathogens that “spread predominantly over short distances.” Surgical masks block far fewer airborne virus particles than N95s, which cost roughly 10 times as much.
Researchers and health care workers have been outraged about the committee’s draft, filing letters and petitions to the CDC. They say it gets the science wrong and endangers health. “A separation between short- and long-range distance is totally artificial,” Tang said.
Airborne viruses travel much like cigarette smoke, he explained. The scent will be strongest beside a smoker, but those farther away will inhale more and more smoke if they remain in the room, especially when there’s no ventilation.
Likewise, people open windows when they burn toast so that smoke dissipates before filling the kitchen and setting off an alarm. “You think viruses stop after 3 feet and drop to the ground?” Tang said of the classical notion of distance. “That is absurd.”
The CDC’s advisory committee is comprised primarily of infection control researchers at large hospital systems, while the WHO consulted a diverse group of scientists looking at many different types of studies. For example, one analysis examined the puff clouds expelled by singers, and musicians playing clarinets, French horns, saxophones, and trumpets. Another reviewed 16 investigations into covid outbreaks at restaurants, a gym, a food processing factory, and other venues, finding that insufficient ventilation probably made them worse than they would otherwise be.
In response to the outcry, the CDC returned the draft to its committee for review, asking it to reconsider its advice. Meetings from an expanded working group have since been held privately. But the National Nurses United union obtained notes of the conversations through a public records request to the agency. The records suggest a push for more lax protection. “It may be difficult as far as compliance is concerned to not have surgical masks as an option,” said one unidentified member, according to notes from the committee’s March 14 discussion. Another warned that “supply and compliance would be difficult.”
The nurses’ union, far from echoing such concerns, wrote on its website, “The Work Group has prioritized employer costs and profits (often under the umbrella of ‘feasibility’ and ‘flexibility’) over robust protections.” Jane Thomason, the union’s lead industrial hygienist, said the meeting records suggest the CDC group is working backward, molding its definitions of airborne transmission to fit the outcome it prefers.
Tang expects resistance to the WHO report. “Infection control people who have built their careers on this will object,” he said. “It takes a long time to change people’s way of thinking.”
The CDC declined to comment on how the WHO’s shift might influence its final policies on infection control in health facilities, which might not be completed this year. Creating policies to protect people from inhaling airborne viruses is complicated by the number of factors that influence how they spread indoors, such as ventilation, temperature, and the size of the space.
Adding to the complexity, policymakers must weigh the toll of various ailments, ranging from covid to colds to tuberculosis, against the burden of protection. And tolls often depend on context, such as whether an outbreak happens in a school or a cancer ward.
“What is the level of mortality that people will accept without precautions?” Tang said. “That’s another question.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Share This Post
Related Posts
-
Healthy Harissa Falafel Patties
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You can make these as regular falafel balls if you prefer, but patties are quicker and easier to cook, and are great for popping in a pitta.
You will need
For the falafels:
- 1 can chickpeas, drained, keep the chickpea water (aquafaba)
- 1 red onion, roughly chopped
- 2 tbsp chickpea flour (also called gram flour or garbanzo bean flour)
- 1 bunch parsley
- 1 tbsp harissa paste
- Extra virgin olive oil for frying
For the harissa sauce:
- ½ cup crème fraîche or plant-based equivalent (you can use our Plant-Based Healthy Cream Cheese recipe and add the juice of 1 lemon)*
- 1 tbsp harissa paste (or adjust this quantity per your heat preference)
*if doing this, rather than waste the zest of the lemon, you can add the zest to the falafels if you like, but it’s by no means necessary, just an option
For serving:
- Wholegrain pitta or other flatbread (you can use our Healthy Homemade Flatbreads recipe)
- Salad (your preference; we recommend some salad leaves, sliced tomato, sliced cucumber, maybe some sliced onion, that sort of thing)
Method
(we suggest you read everything at least once before doing anything)
1) Blend the chickpeas, 1 oz of the aquafaba, the onion, the parsley, and the harissa paste, until smooth. Then add in the chickpea flour until you get a thick batter. If you overdo it with the chickpea flour, add a little more of the aquafaba to equalize. Refrigerate the mixture for at least 30 minutes.
2) Heat some oil in a skillet, and spoon the falafel mixture into the pan to make the patties, cooking on both sides (you can use a spatula to gently turn them), and set them aside.
3) Mix the harissa sauce ingredients in a small bowl.
4) Assemble; best served warm, but enjoy it however you like!
Enjoy!
Want to learn more?
For those interested in more of what we have going on today:
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
- Capsaicin For Weight Loss And Against Inflammation
- Hero Homemade Hummus ← another great option
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What is ‘double pneumonia’, the condition that’s put Pope Francis in hospital?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Pope Francis has been in hospital for more than a week with what some media reports are now calling “double pneumonia”.
The Vatican released a statement on Tuesday evening saying
laboratory tests, chest X-rays, and the clinical condition of the Holy Father continue to present a complex picture.
The 88-year-old Catholic leader has a long history of respiratory illness.
So, what makes this bout of pneumonia – a severe lung infection – so “complex”? And how will it be treated?
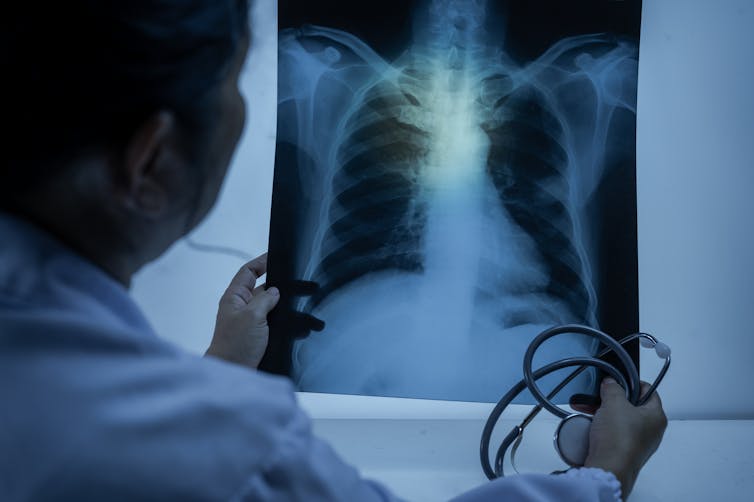
Marco Iaccobucci Epp/Shutterstock What is double pneumonia?
Pneumonia is a serious infection that fills the lungs with liquid or pus and can make it difficult to breathe. People may also have chest pain, cough up green mucus and have a fever.
“Double pneumonia” is not an official medical term. It may be being used to describe two different aspects of Pope Francis’s condition.
1. A bilateral infection
Pope Francis has pneumonia in both lungs. This is known as “bilateral pneumonia”.
An infection in both lungs doesn’t necessarily mean it’s more severe, but location is important. It can make a difference which parts of the lung are affected.
When just one part of the lung or one lung is affected, the person can continue to breathe using the other lung while their body fights the infection.
However when both lungs are compromised, the person will be receiving very little oxygen.
2. A polymicrobial infection
The Vatican has also said the infection affecting Pope Francis’s lungs is “polymicrobial”.
This means the infection is being caused by more than one kind of microorganism (or “pathogen”).
So, the cause could be two (or more) different kinds of bacteria, or any combination of bacteria, virus and fungus. It’s vital to know what’s causing the infection to effectively treat it.
How is it diagnosed?
Usually, when someone presents with suspected pneumonia the hospital will sample their lungs with a sputum test or swab.
They will often also undergo an X-ray, usually to confirm which parts of the lung are involved.
Healthy lungs look “empty” on an X-ray, because they are filled with air. But pneumonia fills the lungs with fluid.
This means it’s usually very easy to see where pneumonia is affecting them, because the infection shows up as solid white mass on the scan.
Lungs infected with pneumonia will have solid white areas on an X-ray. Komsan Loonprom/Shutterstock How is it treated?
The sputum or swab helps detect what is causing the infection and determine treatment. For example, a specific antibiotic will be used to target a certain bacterium.
Usually this works well. But if the infection is polymicrobial, the normal treatment might not be effective.
For example, the antibiotics may work on the bacteria. But if there’s also a virus – which can’t be treated with antibiotics – it may become the dominant pathogen driving the infection.
As a result, the patient may initially respond well to medication and then begin deteriorating again.
If the infection is caused by multiple bacteria, the patient might be given a broad-spectrum antibiotic rather than a single targeted drug.
A viral infection is harder to treat, as the anti-viral drugs that are available aren’t very effective or targeted.
In severe cases, a patient will also need to be in intensive care on a breathing machine because they can’t breathe alone. This helps make sure they receive enough oxygen while their body fights the infection.
Who is most susceptible?
It’s possible to recover, even from severe infections. However having pneumonia can damage the lungs, and this can make a repeat infection more likely.
Most people will never have a severe infection from these same pathogens. They may only experience a minor cold or flu, because their immune system can adequately fight the infection.
However, certain groups are much more vulnerable to developing a serious case of pneumonia.
Risk factors include:
- age: babies under two, whose immune systems are still developing, and adults over 65, who tend to have weakened immune systems
- lung damage: previous infections can cause scarring
- lung disease: for example, if you have emphysema or chronic obstructive pulmonary disease
- being a smoker
- immunosuppression: if your immune system is weakened, for example by medication you take after a transplant or during cancer treatment.
Pope Francis has a number of these risk factors. The pontiff is 88 years old and has a history of respiratory illness.
He also had pleurisy (a condition that inflames the lungs) as a young adult. As a result, he had part of one lung removed, making him susceptible to lung infections.
On Tuesday, the Vatican said Pope Francis remains “in good spirits” while he receives medical care and is grateful for the support he has received.
Brian Oliver, Professor, School of Life Sciences, University of Technology Sydney and Min Feng, PhD Candidate in Respiratory Disease, University of Technology Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Dental Diet – by Dr. Steven Lin
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
As it turns out, there’s a lot more to healthy teeth than skipping the sugar and getting some calcium.
The author’s journey started with the realization that most of his work as a dentist should be unnecessary, and not just in the “you should have been flossing” sense. Rather, he came to the same conclusions as his fellow dentist Weston Price before him, and this time (unlike Price) he stuck to his own field, dentistry—meaning that the conclusions he kept were the more valid ones.
Another thing he does better than Price is that he contextualizes the information—we don’t need, for example, to be eating seal fat as a main component of our diet, but we do need to be getting sufficient amounts of certain fat-soluble vitamins. And most people aren’t. Same with what’s good or bad for our oral microbiome, and by extension, our saliva, and by extension, our teeth and gums.
There’s a lot of nutritional information in here; macros and micronutrients alike, but the book goes further than that, to also recommend minimally-processed food that requires more chewing, for example. Not just for its nutritional content, but because that helps our teeth move to (and then stay) where they are ideally supposed to be. No amount of perfectly-blended nutritional supplement drink will align your maxilla for you, say. But chomping on raw carrots? Different story.
Dr. Lin offers a 40-day meal plan, but aware that if you’re vegetarian or vegan you’re probably going to have to rethink it yourself using the information he gives, because his meal plan includes animal products.
Bottom line: if you’d like to eat for better oral health (nutritionally, physically, and for your oral microbiome), this book has all the information you’ll need.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: