Asbestos in mulch? Here’s the risk if you’ve been exposed
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Mulch containing asbestos has now been found at 41 locations in New South Wales, including Sydney parks, schools, hospitals, a supermarket and at least one regional site. Tests are under way at other sites.
As a precautionary measure, some parks have been cordoned off and some schools have closed temporarily. Fair Day – a large public event that traditionally marks the start of Mardi Gras – was cancelled after contaminated mulch was found at the site.
The New South Wales government has announced a new taskforce to help investigate how the asbestos ended up in the mulch.
Here’s what we know about the risk to public health of mulch contaminated with asbestos, including “friable” asbestos, which has been found in one site (Harmony Park in Surry Hills).
What are the health risks of asbestos?
Asbestos is a naturally occurring, heat-resistant fibre that was widely used in building materials from the 1940s to the 1980s. It can be found in either a bonded or friable form.
Bonded asbestos means the fibres are bound in a cement matrix. Asbestos sheeting that was used for walls, fences, roofs and eaves are examples of bonded asbestos. The fibres don’t escape this matrix unless the product is severely damaged or worn.
A lot of asbestos fragments from broken asbestos products are still considered bonded as the fibres are not released as they lay on the ground.

Tomas Regina/Shutterstock
Friable asbestos, in contrast, can be easily crumbled by touch. It will include raw asbestos fibres and previously bonded products that have worn to the point that they crumble easily.
The risk of disease from asbestos exposure is due to the inhalation of fibres. It doesn’t matter if those fibres are from friable or bonded sources.
However, fibres can more easily become airborne, and therefore inhalable, if the asbestos is friable. This means there is more of a risk of exposure if you are disturbing friable asbestos than if you disturb fragments of bonded asbestos.
Who is most at risk from asbestos exposure?
The most important factor for disease risk is exposure – you actually have to inhale fibres to be at risk of disease.
Just being in the vicinity of asbestos, or material containing asbestos, does not put you at risk of asbestos-related disease.
For those who accessed the contaminated areas, the level of exposure will depend on disturbing the asbestos and how many fibres become airborne due to that disturbance.
However, if you have been exposed to, and inhaled, asbestos fibres it does not mean you will get an asbestos-related disease. Exposure levels from the sites across Sydney will be low and the chance of disease is highly unlikely.
The evidence for disease risk from ingestion remains highly uncertain, although you are not likely to ingest sufficient fibres from the air, or even the hand to mouth activities that may occur with playing in contaminated mulch, for this to be a concern.
The risk of disease from exposure depends on the intensity, frequency and duration of that exposure. That is, the more you are exposed to asbestos, the greater the risk of disease.
Most asbestos-related disease has occurred in people who work with raw asbestos (for example, asbestos miners) or asbestos-containing products (such as building tradespeople). This has been a tragedy and fortunately asbestos is now banned.
There have been cases of asbestos-related disease, most notably mesothelioma – a cancer of the lining of the lung (mostly) or peritoneum – from non-occupational exposures. This has included people who have undertaken DIY home renovations and may have only had short-term exposures. The level of exposure in these cases is not known and it is also impossible to determine if those activities have been the only exposure.
There is no known safe level of exposure – but this does not mean that one fibre will kill. Asbestos needs to be treated with caution.
As far as we are aware, there have been no cases of mesothelioma, or other asbestos-related disease, that have been caused by exposure from contaminated soils or mulch.
Has asbestos been found in mulch before?
Asbestos contamination of mulch is, unfortunately, not new. Environmental and health agencies have dealt with these situations in the past. All jurisdictions have strict regulations about removing asbestos products from the green waste stream but, as is happening in Sydney now, this does not always happen.

gibleho/Shutterstock
What if I’ve been near contaminated mulch?
Exposure from mulch contamination is generally much lower than from current renovation or construction activities and will be many orders of magnitude lower than past occupational exposures.
Unlike activities such as demolition, construction and mining, the generation of airborne fibres from asbestos fragments in mulch will be very low. The asbestos contamination will be sparsely spread throughout the mulch and it is unlikely there will be sufficient disturbance to generate large quantities of airborne fibres.
Despite the low chance of exposure, if you’re near contaminated mulch, do not disturb it.
If, by chance, you have had an exposure, or think you have had an exposure, it’s highly unlikely you will develop an asbestos-related disease in the future. If you’re worried, the Asbestos Safety and Eradication Agency is a good source of information.
Peter Franklin, Associate Professor and Director, Occupational Respiratory Epidemiology, The University of Western Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Yes, you still need to use sunscreen, despite what you’ve heard on TikTok
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Summer is nearly here. But rather than getting out the sunscreen, some TikTokers are urging followers to chuck it out and go sunscreen-free.
They claim it’s healthier to forgo sunscreen to get the full benefits of sunshine.
Here’s the science really says.
Karolina Grabowska/Pexels How does sunscreen work?
Because of Australia’s extreme UV environment, most people with pale to olive skin or other risk factors for skin cancer need to protect themselves. Applying sunscreen is a key method of protecting areas not easily covered by clothes.
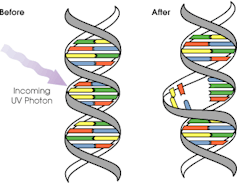
Sunscreen works by absorbing or scattering UV rays before they can enter your skin and damage DNA or supportive structures such as collagen.
When UV particles hit DNA, the excess energy can damage our DNA. This damage can be repaired, but if the cell divides before the mistake is fixed, it causes a mutation that can lead to skin cancers.
The energy from a particle of UV (a photon) causes DNA strands to break apart and reconnect incorrectly. This causes a bump in the DNA strand that makes it difficult to copy accurately and can introduce mutations. NASA/David Herring The most common skin cancers are basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Melanoma is less common, but is the most likely to spread around the body; this process is called metastasis.
Two in three Australians will have at least one skin cancer in their lifetime, and they make up 80% of all cancers in Australia.
Around 99% of skin cancers in Australia are caused by excessive exposure to UV radiation.
Excessive exposure to UV radiation also affects the appearance of your skin. UVA rays are able to penetrate deep into the skin, where they break down supportive structures such as elastin and collagen.
This causes signs of premature ageing, such as deep wrinkling, brown or white blotches, and broken capillaries.
Sunscreen can help prevent skin cancers
Used consistently, sunscreen reduces your risk of skin cancer and slows skin ageing.
In a Queensland study, participants either used sunscreen daily for almost five years, or continued their usual use.
At the end of five years, the daily-use group had reduced their risk of squamous cell carcinoma by 40% compared to the other group.
Ten years later, the daily use group had reduced their risk of invasive melanoma by 73%
Does sunscreen block the health-promoting properties of sunlight?
The answer is a bit more complicated, and involves personalised risk versus benefit trade-offs.
First, the good news: there are many health benefits of spending time in the sun that don’t rely on exposure to UV radiation and aren’t affected by sunscreen use.
Sunscreen only filters UV rays, not all light. Ron Lach/Pexels Sunscreen only filters UV rays, not visible light or infrared light (which we feel as heat). And importantly, some of the benefits of sunlight are obtained via the eyes.
Visible light improves mood and regulates circadian rhythm (which influences your sleep-wake cycle), and probably reduces myopia (short-sightedness) in children.
Infrared light is being investigated as a treatment for several skin, neurological, psychiatric and autoimmune disorders.
So what is the benefit of exposing skin to UV radiation?
Exposing the skin to the sun produces vitamin D, which is critical for healthy bones and muscles.
Vitamin D deficiency is surprisingly common among Australians, peaking in Victoria at 49% in winter and being lowest in Queensland at 6% in summer.
Luckily, people who are careful about sun protection can avoid vitamin D deficiency by taking a supplement.
Exposing the skin to UV radiation might have benefits independent of vitamin D production, but these are not proven. It might reduce the risk of autoimmune diseases such as multiple sclerosis or cause release of a chemical that could reduce blood pressure. However, there is not enough detail about these benefits to know whether sunscreen would be a problem.
What does this mean for you?
There are some benefits of exposing the skin to UV radiation that might be blunted by sunscreen. Whether it’s worth foregoing those benefits to avoid skin cancer depends on how susceptible you are to skin cancer.
If you have pale skin or other factors that increase you risk of skin cancer, you should aim to apply sunscreen daily on all days when the UV index is forecast to reach 3.
If you have darker skin that rarely or never burns, you can go without daily sunscreen – although you will still need protection during extended times outdoors.
For now, the balance of evidence suggests it’s better for people who are susceptible to skin cancer to continue with sun protection practices, with vitamin D supplementation if needed.
Katie Lee, PhD Candidate, Dermatology Research Centre, The University of Queensland and Rachel Neale, Principal research fellow, QIMR Berghofer Medical Research Institute
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
What’s the difference between a food allergy and an intolerance?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
At one time or another, you’ve probably come across someone who is lactose intolerant and might experience some unpleasant gut symptoms if they have dairy. Maybe it’s you – food intolerances are estimated to affect up to 25% of Australians.
Meanwhile, cow’s milk allergy is one of the most common food allergies in infants and young children, affecting around one in 100 infants.
But what’s the difference between food allergies and food intolerances? While they might seem alike, there are some fundamental differences between the two.
Feel good studio/Shutterstock What is an allergy?
Australia has one of the highest rates of food allergies in the world. Food allergies can develop at any age but are more common in children, affecting more than 10% of one-year-olds and 6% of children at age ten.
A food allergy happens when the body’s immune system mistakenly reacts to certain foods as if they were dangerous. The most common foods that trigger allergies include eggs, peanuts and other nuts, milk, shellfish, fish, soy and wheat.
Mild to moderate signs of food allergy include a swollen face, lips or eyes; hives or welts on your skin; or vomiting. A severe allergic reaction (called anaphylaxis) can cause trouble breathing, persistent dizziness or collapse.
What is an intolerance?
Food intolerances (sometimes called non-allergic reactions) are also reactions to food, but they don’t involve your immune system.
For example, lactose intolerance is a metabolic condition that happens when the body doesn’t produce enough lactase. This enzyme is needed to break down the lactose (a type of sugar) in dairy products.
Food intolerances can also include reactions to natural chemicals in foods (such as salicylates, found in some fruits, vegetables, herbs and spices) and problems with artificial preservatives or flavour enhancers.
Lactose intolerance is caused by a problem with breaking down lactose in milk. Pormezz/Shutterstock Symptoms of food intolerances can include an upset stomach, headaches and fatigue, among others.
Food intolerances don’t cause life-threatening reactions (anaphylaxis) so are less dangerous than allergies in the short term, although they can cause problems in the longer term such as malnutrition.
We don’t know a lot about how common food intolerances are, but they appear to be more commonly reported than allergies. They can develop at any age.
It can be confusing
Some foods, such as peanuts and tree nuts, are more often associated with allergy. Other foods or ingredients, such as caffeine, are more often associated with intolerance.
Meanwhile, certain foods, such as cow’s milk and wheat or gluten (a protein found in wheat, rye and barley), can cause both allergic and non-allergic reactions in different people. But these reactions, even when they’re caused by the same foods, are quite different.
For example, children with a cow’s milk allergy can react to very small amounts of milk, and serious reactions (such as throat swelling or difficulty breathing) can happen within minutes. Conversely, many people with lactose intolerance can tolerate small amounts of lactose without symptoms.
There are other differences too. Cow’s milk allergy is more common in children, though many infants will grow out of this allergy during childhood.
Lactose intolerance is more common in adults, but can also sometimes be temporary. One type of lactose intolerance, secondary lactase deficiency, can be caused by damage to the gut after infection or with medication use (such as antibiotics or cancer treatment). This can go away by itself when the underlying condition resolves or the person stops using the relevant medication.
Whether an allergy or intolerance is likely to be lifelong depends on the food and the reason that the child or adult is reacting to it.
Allergies to some foods, such as milk, egg, wheat and soy, often resolve during childhood, whereas allergies to nuts, fish or shellfish, often (but not always) persist into adulthood. We don’t know much about how likely children are to grow out of different types of food intolerances.
How do you find out what’s wrong?
If you think you may have a food allergy or intolerance, see a doctor.
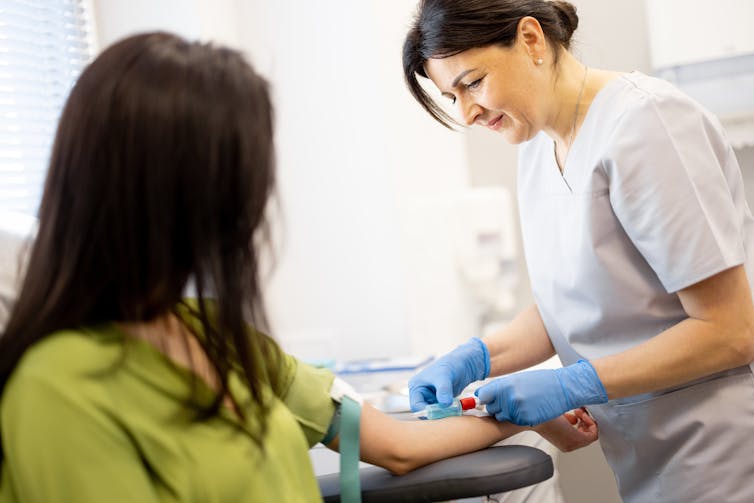
Allergy tests help doctors find out which foods might be causing your allergic reactions (but can’t diagnose food intolerances). There are two common types: skin prick tests and blood tests.
In a skin prick test, doctors put tiny amounts of allergens (the things that can cause allergies) on your skin and make small pricks to see if your body reacts.
A blood test checks for allergen-specific immunoglobulin E (IgE) antibodies in your blood that show if you might be allergic to a particular food.
Blood tests can help diagnose allergies. RossHelen/Shutterstock Food intolerances can be tricky to figure out because the symptoms depend on what foods you eat and how much. To diagnose them, doctors look at your health history, and may do some tests (such as a breath test). They may ask you to keep a record of foods you eat and timing of symptoms.
A temporary elimination diet, where you stop eating certain foods, can also help to work out which foods you might be intolerant to. But this should only be done with the help of a doctor or dietitian, because eliminating particular foods can lead to nutritional deficiencies, especially in children.
Is there a cure?
There’s currently no cure for food allergies or intolerances. For allergies in particular, it’s important to strictly avoid allergens. This means reading food labels carefully and being vigilant when eating out.
However, researchers are studying a treatment called oral immunotherapy, which may help some people with food allergies become less sensitive to certain foods.
Whether you have a food allergy or intolerance, your doctor or dietitian can help you to make sure you’re eating the right foods.
Victoria Gibson, a Higher Degree by Research student and Research Officer at the School of Nursing, Midwifery and Social Work at the University of Queensland, and Rani Scott-Farmer, a Senior Research Assistant at the University of Queensland, contributed to this article.
Jennifer Koplin, Group Leader, Childhood Allergy & Epidemiology, The University of Queensland and Desalegn Markos Shifti, Postdoctoral Research Fellow, Child Health Research Centre, Faculty of Medicine, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
The Mindful Body – by Dr. Ellen Langer
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Fear not, this is not a “think healing thoughts” New Age sort of book. In fact, it’s quite the contrary.
The most common negative reviews for this on Amazon are that it is too densely packed with scientific studies, and some readers found it hard to get through since they didn’t find it “light reading”.
Counterpoint: this reviewer found it very readable. A lot of it is as accessible as 10almonds content, and a lot is perhaps halfway between 10almonds content in readability, and the studies we cite. So if you’re at least somewhat comfortable reading academic literature, you should be fine.
The author, a professor of psychology (tenured at Harvard since 1981), examines a lot of psychosomatic effect. Psychosomatic effect is often dismissed as “it’s all in your head”, but it means: what’s in your head has an effect on your body, because your brain talks to the rest of the body and directs bodily responses and actions/reactions.
An obvious presentation of this in medicine is the placebo/nocebo effect, but Dr. Langer’s studies (indeed, many of the studies she cites are her own, from over the course of her 40-year career) take it further and deeper, including her famous “Counterclockwise” study in which many physiological markers of aging were changed (made younger) by changing the environment that people spent time in, to resemble their youth, and giving them instructions to act accordingly while there.
In the category of subjective criticism: the book is not exceptionally well-organized, but if you read for example a chapter a day, you’ll get all the ideas just fine.
Bottom line: if you want a straightforward hand-holding “how-to” guide, this isn’t it. But it is very much information-packed with a lot of ideas and high-quality science that’s easily applicable to any of us.
Click here to check out The Mindful Body, and indeed grow your chronic good health!
Share This Post
Related Posts
-
It’s Not Fantastic To Be Plastic
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We Are Such Stuff As Bottles Are Made Of
We’ve written before about PFAS, often found in non-stick coatings and the like:
PFAS Exposure & Cancer: The Numbers Are High
Today we’re going to be talking about microplastics & nanoplastics!
What are microplastics and nanoplastics?
Firstly, they’renot just the now-banned plastic microbeads that have seen some use is toiletries (although those are classified as microplastics too).
Many are much smaller than that, and if they get smaller than a thousandth of a millimeter, then they get the additional classification of “nanoplastic”.
In other words: not something that can be filtered even if you were to use a single-micron filter. The microplastics would still get through, for example:
Scientists find about a quarter million invisible nanoplastic particles in a liter of bottled water
And unfortunately, that’s bad:
❝What’s disturbing is that small particles can appear in different organs and may cross membranes that they aren’t meant to cross, such as the blood-brain barrier❞
Note: they’re crossing the same blood-brain barrier that many of our nutrients and neurochemicals are too big to cross.
These microplastics are also being found in arterial plaque
What makes arterial plaque bad for the health is precisely its plasticity (the arterial walls themselves are elastic), so you most certainly do not want actual plastic being used as part of the cement that shouldn’t even be lining your arteries in the first place:
Microplastics found in artery plaque linked with higher risk of heart attack, stroke and death
❝In this study, patients with carotid artery plaque in which MNPs were detected had a higher risk of a composite of myocardial infarction, stroke, or death from any cause at 34 months of follow-up than those in whom MNPs were not detected❞
~ Dr. Raffaele Marfella et al.
(MNP = Micro/Nanoplastics)
Source: Microplastics and Nanoplastics in Atheromas and Cardiovascular Events
We don’t know how bad this is yet
There are various ways this might not be as bad as it looks (the results may not be repeated, the samples could have been compromised, etc), but also, perhaps cynically but nevertheless honestly, it could also be worse than we know yet—only more experiments being done will tell us which.
In the meantime, here’s a rundown of what we do and don’t know:
Study links microplastics with human health problems—but there’s still a lot we don’t know
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Cold Truth About Respiratory Infections
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The Pathogens That Came In From The Cold
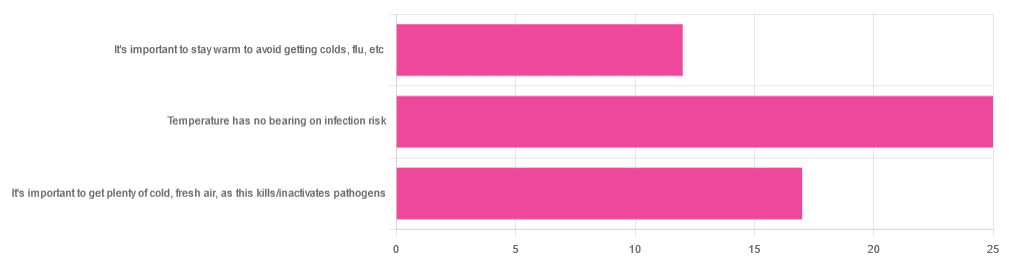
Yesterday, we asked you about your climate-themed policy for avoiding respiratory infections, and got the above-depicted, below-described, set of answers:
- About 46% of respondents said “Temperature has no bearing on infection risk”
- About 31% of respondents said “It’s important to get plenty of cold, fresh air, as this kills/inactivates pathogens”
- About 22% of respondents said “It’s important to stay warm to avoid getting colds, flu, etc”
Some gave rationales, including…
For “stay warm”:
❝Childhood lessons❞
For “get cold, fresh air”:
❝I just feel that it’s healthy to get fresh air daily. Whether it kills germs, I don’t know❞
For “temperature has no bearing”:
❝If climate issue affected respiratory infections, would people in the tropics suffer more than those in colder climates? Pollutants may affect respiratory infections, but I doubt just temperature would do so.❞
So, what does the science say?
It’s important to stay warm to avoid getting colds, flu, etc: True or False?
False, simply. Cold weather does increase the infection risk, but for reasons that a hat and scarf won’t protect you from. More on this later, but for now, let’s lay to rest the idea that bodily chilling will promote infection by cold, flu, etc.
In a small-ish but statistically significant study (n=180), it was found that…
❝There was no evidence that chilling caused any acute change in symptom scores❞
Read more: Acute cooling of the feet and the onset of common cold symptoms
Note: they do mention in their conclusion that chilling the feet “causes the onset of cold symptoms in about 10% of subjects who are chilled”, but the data does not support that conclusion, and the only clear indicator is that people who are more prone to colds generally, were more prone to getting a cold after a cold water footbath.
In other words, people who were more prone to colds remained more prone to colds, just the same.
It’s important to get plenty of cold, fresh air, as this kills/inactivates pathogens: True or False?
Broadly False, though most pathogens do have an optimal operating temperature that (for obvious reasons) is around normal human body temperature.
However, given that they don’t generally have to survive outside of a host body for long to get passed on, the fact that the pathogens may be a little sluggish in the great outdoors will not change the fact that they will be delighted by the climate in your respiratory tract as soon as you get back into the warm.
With regard to the cold air not being a reliable killer/inactivator of pathogens, we call to the witness stand…
Polar Bear Dies From Bird Flu As H5N1 Spreads Across Globe
(it was found near Utqiagvik, one of the northernmost communities in Alaska)
Because pathogens like human body temperature, raising the body temperature is a way to kill/inactivate them: True or False?
True! Unfortunately, it’s also a way to kill us. Because we, too, cannot survive for long above our normal body temperature.
So, for example, bundling up warmly and cranking up the heating won’t necessarily help, because:
- if the temperature is comfortable for you, it’s comfortable for the pathogen
- if the temperature is dangerous to the pathogen, it’s dangerous to you too
This is why the fever response evolved, and/but why many people with fevers die anyway. It’s the body’s way of playing chicken with the pathogen, challenging “guess which of us can survive this for longer!”
Temperature has no bearing on infection risk: True or False?
True and/or False, circumstantially. This one’s a little complex, but let’s break it down to the essentials.
- Temperature has no direct effect, for the reasons we outlined above
- Temperature is often related to humidity, which does have an effect
- Temperature does tend to influence human behavior (more time spent in open spaces with good ventilation vs more time spent in closed quarters with poor ventilation and/or recycled air), which has an obvious effect on transmission rates
The first one we covered, and the third one is self-evident, so let’s look at the second one:
Temperature is often related to humidity, which does have an effect
When the environmental temperature is warmer, water droplets in the air will tend to be bigger, and thus drop to the ground much more quickly.
When the environmental temperature is colder, water droplets in the air will tend to be smaller, and thus stay in the air for longer (along with any pathogens those water droplets may be carrying).
Some papers on the impact of this:
- Cold temperature and low humidity are associated with increased occurrence of respiratory tract infections
- A Decrease in Temperature and Humidity Precedes Human Rhinovirus Infections in a Cold Climate
So whatever temperature you like to keep your environment, humidity is a protective factor against respiratory infections, and dry air is a risk factor.
So, for example:
- If the weather doesn’t suit having good ventilation, a humidifier is a good option
- Being in an airplane is one of the worst places to be for this, outside of a hospital
Don’t have a humidifier? Here’s an example product on Amazon, but by all means shop around.
A crock pot with hot water in and the lid off is also a very workable workaround too
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
How Beneficial Is MCT Oil, Really?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Often derived from coconuts (though it doesn’t have to be), medium-chain triglycerides (MCTs) are trendy… But does the science back the hype?
First, the principle
MCTs are commonly enjoyed because unlike short- or long-chain fatty acids, they can be quickly broken down and either immediately converted quickly and easily into energy, or turned into ketones in the case of a surplus (in the case of true excess, however, it’ll simply be stored as fat).
Most of that involves the liver, so for anyone who wants a refresher on liver health:
How To Unfatty A Fatty Liver ← notwithstanding the title, this is also important knowledge even if your liver is healthy now—if you’d like it to stay healthy, anyway!
You can also read about the ins and outs of glycogen metabolism and the body’s energy-based metabolic processes in general (including the body’s energy processes that go on in the liver), here:
From Apples to Bees, and High-Fructose Cs: Which Sugars Are Healthier, And Which Are Just The Same?
If the liver turns the MCTs into ketones, those ketones will then be used for energy if there is insufficient glucose available (as the body will always use glucose from the blood first, if available, before moving to alternative energy sources such as ketones and/or fat reserves.)
Thus, many people look to ketones as a solution for having enough energy to function while on a very low-carb diet such as the ketogenic diet:
Ketogenic Diet: Burning Fat Or Burning Out?
…which as you’ll recall, does work for short-term weight loss, but brings long-term health risks, so should not be undertaken for long periods of time.
So, does MCT Oil help?
With regard to weight loss, the research is weak and mixed:
- Weak, because often the methodology was shoddy, often there are many factors not controlled-for, and often the sample sizes were small (and also, RCTs by their very nature tend to be quite short-term (often 6, 8, or 12 weeks), whereas heavy reliance on ketones from MCTs may fall into the same long-term problems as the ketogenic diet in general).
- Mixed, because the results varied widely (probably because of the aforementioned problems).
Rather than pick at individual studies, let’s look at this review and meta-analysis of 13 studies, with a combined sample size of 749 people (so you can imagine how small the individual RCTs were):
❝Compared with LCTs, MCTs decreased body weight (-0.51 kg [95% CI-0.80 to -0.23 kg]; P<0.001; I(2)=35%); waist circumference (-1.46 cm [95% CI -2.04 to -0.87 cm]; P<0.001; I(2)=0%), hip circumference (-0.79 cm [95% CI -1.27 to -0.30 cm]; P=0.002; I(2)=0%), total body fat (standard mean difference -0.39 [95% CI -0.57 to -0.22]; P<0.001; I(2)=0%), total subcutaneous fat (standard mean difference -0.46 [95% CI -0.64 to -0.27]; P<0.001; I(2)=20%), and visceral fat (standard mean difference -0.55 [95% CI -0.75 to -0.34]; P<0.001; I(2)=0%).
No differences were seen in blood lipid levels.
Many trials lacked sufficient information for a complete quality assessment, and commercial bias was detected.❞
So, if we’re going to take those numbers at face value, that means a net weight loss, over the course of the trial period, was…
*drumroll*
0.51kg (that’s about 1 lb).
To put that into perspective, if you did nothing else but pee 1 cup of urine before getting weighed, you’d register as having lost 0.25kg (or about ½ lb) by virtue of the bathroom trip alone.
Here’s the paper:
What about cholesterol and heart health?
With regard to cholesterol, MCT oil is touted as improving blood lipids, which means lowering LDL and increasing HDL (within a safe range, anyway).
You’ll remember that the above review concluded “No differences were seen in blood lipid levels”.
It may again be a case of individual studies cancelling each other out. For example…
This study found that it improved lipids in 40 young women as part of a calorie-controlled interventional diet:
This study found that it worsened lipids in 17 young men, worse even than taking an equivalent amount of sunflower oil:
In short, it’s a gamble.
It may be good for insulin sensitivity, though
This one seems to be specific to people with type 2 diabetes. The paper heading says it all, but we include the link in case you want to know the details (the short version is, it improved insulin sensitivity in diabetic subjects only (not others), and didn’t affect anything else that was measured:
The sample size was small (20 people total, of whom 10 had diabetes), and the next study was with 40 people, this time moderately overweight and all with type 2 diabetes:
Want to try some?
We don’t sell it, but here for your convenience is an example product on Amazon 😎
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: