6 Signs Of A Heart Attack… A Month In Advance
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Many people know the signs of a heart attack when it’s happening, but how about before it’s too late to avoid it?
The signs
- Unusual fatigue: persistent tiredness that doesn’t improve with rest
- Shortness of breath: unexplained breathlessness during light activities or rest, which can be caused by fluid buildup in the lungs (because the heart isn’t circulating blood as well as it should)
- Chest discomfort: pain, pressure, tightness, or aching in the chest due to reduced blood flow to the heart muscle—often occurring during physical exertion or emotional stress
- Frequent indigestion: means that heartburn could be heart-related! This is about persistently reoccurring discomfort or pain in the upper abdomen
- Sleep disturbances: difficulties falling asleep, staying asleep, or waking up abruptly
- Excessive sweating: unexplained cold sweats or sudden sweating without physical exertion or excessive heat, can be a response to the decreased oxygen levels caused by less efficient blood flow
Note: this is a list of warning signs, not a diagnostic tool. Any or even all of these could be caused by something else. Just, don’t ignore the signs and do get yourself checked out.
For more details on each of these, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Come Together – by Dr. Emily Nagoski
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
From Dr. Emily Nagoski, author of the bestseller “Come As You Are” (which we reviewed very favorably before) we now present: Come Together.
What it is not about: simultaneous orgasms. The title is just a play on words.
What it is about: improving sexual wellbeing, particularly in long-term relationships where one or more partner(s) may be experiencing low desire.
Hence: come together, in the closeness sense.
A lot of books (or advice articles) out there take the Cosmo approach of “spicing things up”, and that can help for a night perhaps, but relying on novelty is not a sustainable approach.
Instead, what Dr. Nagoski outlines here is a method for focusing on shared comfort and pleasure over desire, creating the right state of mind that’s more conducive to sexuality, and reducing things that put the brakes on sexuality.
She also covers things whereby sexuality can often be obliged to change (for example, with age and/or disability), but that with the right attitude, change can sometimes just be growth in a different way, as you explore the new circumstances together, and continue to find shared pleasure in the ways that best suit your changing circumstances,
Bottom line: if you and/or your partner(s) would like to foster and maintain intimacy and pleasure, then this is a top-tier book for you.
Click here to check out Come Together, and, well, come together!
Share This Post
-
Gut-Positive Pot Noodles
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Everything we consume either improves our health a little or worsens it. Pot noodles aren’t generally the healthiest foods, but these ones sure are! There’s quite a range of fiber in this, including the soluble fiber of the noodles themselves (which are, in fact, mostly fiber and water). As a bonus, the glucomannan in the noodles promotes feelings of fullness, notwithstanding its negligible carb count. Of course, the protein in the edamame beans also counts for satiety!
You will need
- ½ cup konjac noodles (also called shirataki), tossed in 1 tsp avocado oil (or sesame oil, if you don’t have avocado)
- 2 oz mangetout, thinly sliced
- 1 oz edamame beans
- ¼ carrot, grated
- 2 baby sweetcorn, cut in half lengthways
- 1 scallion, finely diced
- 1 heaped tsp crunchy peanut butter (omit if allergic)
- 1 tsp miso paste
- 1 tsp chili oil
- 1 tsp black pepper, coarse ground
- 1 tsp peeled-and-grated ginger
Method
(we suggest you read everything at least once before doing anything)
1) Layer a heat-resistant jar (mason jars are usually quite resistant to temperature changes) with the noodles and vegetables.
2) Combine the peanut butter, miso paste, and chili oil, black pepper, and ginger in a small bowl. Pour this dressing over the layered vegetables and noodles, and screw the lid on. Refrigerate until needed.
3) Add hot water to the jar and stir, to serve. If you prefer the vegetables to be more cooked, you can microwave (without the lid!) for a minute or two.
Enjoy!
Want to learn more?
For those interested in some of the science of what we have going on today:
- Making Friends With Your Gut (You Can Thank Us Later)
- Why You’re Probably Not Getting Enough Fiber (And How To Fix It)
- 10 Ways To Balance Blood Sugars ← today’s recipe makes a perfect high-fiber, low-carb starter, per the hacks here
- Capsaicin For Weight Loss And Against Inflammation
- Black Pepper’s Impressive Anti-Cancer Arsenal (And More)
- Ginger Does A Lot More Than You Think
Take care!
Share This Post
-
Try This At Home: ABI Test For Clogged Arteries
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Arterial plaque is a big deal, and statistically it’s more of a risk as we get older, often coming to a head around age 72 for women and 65 for men—these are the median ages at which people who are going to get heart attacks, get them. Or get it, because sometimes one is all it takes.
The Ankle-Brachial Index Test
Dr. Brewer recommends a home test for detecting arterial plaque called the Ankle-Brachial Index (ABI), which uses a blood pressure monitor. The test involves measuring blood pressure in both the arms and ankles, then calculating the ratio of these measurements:
- A healthy ABI score is between 1.0 and 1.4; anything outside this range may indicate arterial problems.
- Low ABI scores (below 0.8) suggest plaque is likely obstructing blood flow
- High ABI scores (above 1.4) may indicate artery hardening
Peripheral Artery Disease (PAD), associated with poor ABI results (be they high or low), can cause a whole lot of problems that are definitely better tackled sooner rather than later—remember that atherosclerosis is a self-worsening thing once it gets going, because narrower walls means it’s even easier for more stuff to get stuck in there (and thus, the new stuff that got stuck also becomes part of the walls, and the problem gets worse).
If you need a blood pressure monitor, by the way, here’s an example product on Amazon.
Do note also that yes, if you have plaque obstructing blood flow and hardened arteries, your scores may cancel out and give you a “healthy” score, despite your arteries being very much not healthy. For this reason, this test can be used to raise the alarm, but not to give the “all clear”.
For more on all of the above, plus a demonstration and more in-depth explanation of the test, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Take care!
Share This Post
Related Posts
-
Counterclockwise – by Dr. Ellen Langer
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve written previously about Dr. Langer’s famous “Counterclockwise” study that saw reversals in biological markers of aging after a one-week intervention that consisted only of a (albeit rather intensive) mental reframe with regard to their age.
This book, as you might expect from the title, refers to that experiment a lot—but it doesn’t stop there. While the Counterclockwise experiment remains Dr. Langer’s most well-known, it’s not her most recent, and she draws from a wealth of research (her own and that of her colleagues in the field) to show the extent and limit of psychosomatic effect on aging.
Note:
- psychosomatic effect does not mean: “imagining it”
- psychosomatic effect means: “your brain regulates almost everything else in your body, directly or indirectly, including your autonomic functions, which includes immune function, tissue replacement, and more”
And as for when it comes to aging? Aging, like cancer, is in large part a problem of immune dysfunction; in both cases cells (be they senescent or cancerous, respectively) are not being killed when they are supposed to be, and in both cases, better instructions will improve the matter.
Many larger-scale markers of aging, such as mobility, are a case of the body only being able to do what the tissues allow, and the tissues are being constantly rebuilt (for better or for worse) according to autonomically-implemented specifications, and cells’ ability to carry out those orders.
Beyond the cellular physiology, this book discusses (a lot) the brain-down mechanisms by which the most powerful organ in our body can tell the rest of the body how old to be.
Dr. Langer also discusses the matter of “priming”, that is to say, how external factors prime us to believe certain things about our age and, with it, our health. These things can include popular media, conversations with friends and family, and healthcare providers’ framing of certain issues.
For example, a person just under a certain age and a person just over a certain age could both go to the doctor with the same complaint—a pain in a certain joint, let’s say. The doctor may refer the slightly younger patient for an x-ray because “let’s see what’s going on here”, and prescribe the slightly older patient some painkillers because “this is perfectly normal at your age”. One resultant problem is obvious: a difference in the standard of care. But the other resultant problem is less obvious: the older patient has now been primed to believe, by a confident authority figure, “it is natural for my body to be in a state of decline now, and this is what to expect”.
Thus, Dr. Langer prescribes mindfulness, not in the mindfulness meditation sense (though sure, do that too), but rather in the sense of consciously interacting with the world and making our own decisions about our own health and, yes, our own age. Because after all, our body neither knows nor cares how many times it has flown around the sun, and merely responds to physiological stimuli—including those we can influence with psychological reframing.
The book is not, per se, a “how-to” guide, rather it is an explanatory treatise, but it contains more than enough information to put it into practice, and indeed, she does also provide some exercises to do along the way.
The style is… Vivacious, without being especially upbeat. Dr. Langer is enthused about her work, yes, but she’s also angry at how many people are having their health sabotaged on the daily, and calls for a more health-first approach (as opposed to illness-first).
Bottom line: this is the book on our brain’s power over aging, so if that topic interests you, this book absolutely belongs on your bookshelf. Well, in your hands, and then on the bookshelf, and then back in your hands from time to time.
Click here to check out Counterclockwise, and age counterclockwise as her experimental subjects did!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Kidney Beans vs Fava Beans – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing kidney beans to fava beans, we picked the kidney beans.
Why?
It’s a simple and straightforward one today!
The macronutrient profiles are mostly comparable, but kidney beans do have a little more protein and a little more fiber.
In the category of vitamins, kidney beans have more of vitamins B1, B5, B6, B9, C, E, & K, while fava beans boast only more of vitamins B2 and B3. They are both equally good sources of choline, but the general weight of vitamins is very much in kidney beans’ favor, with a 7:2 lead, most of which have generous margins.
When it comes to minerals, kidney beans have more iron, phosphorus, and potassium, while fava beans have more copper and selenium. They’re both equally good sources of other minerals they both contain. Still, a 3:2 victory for kidney beans on the mineral front.
Adding up the moderate victory on macros, the strong victory on vitamins, and the slight victory on minerals, all in all makes for a clear win for kidney beans.
Still, enjoy both! Diversity is healthy.
Want to learn more?
You might like to read:
Chickpeas vs Black Beans – Which is Healthier?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Getting antivirals for COVID too often depends on where you live and how wealthy you are
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Medical experts recommend antivirals for people aged 70 and older who get COVID, and for other groups at risk of severe illness and hospitalisation from COVID.
But many older Australians have missed out on antivirals after getting sick with COVID. It is yet another way the health system is failing the most vulnerable.
CGN089/Shutterstock Who missed out?
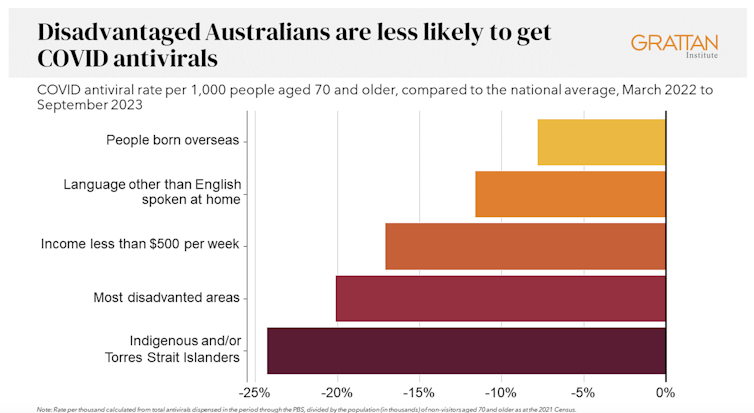
We analysed COVID antiviral uptake between March 2022 and September 2023. We found some groups were more likely to miss out on antivirals including Indigenous people, people from disadvantaged areas, and people from culturally and linguistically diverse backgrounds.
Some of the differences will be due to different rates of infection. But across this 18-month period, many older Australians were infected at least once, and rates of infection were higher in some disadvantaged communities.
How stark are the differences?
Compared to the national average, Indigenous Australians were nearly 25% less likely to get antivirals, older people living in disadvantaged areas were 20% less likely to get them, and people with a culturally or linguistically diverse background were 13% less likely to get a script.
People in remote areas were 37% less likely to get antivirals than people living in major cities. People in outer regional areas were 25% less likely.
Dispensing rates by group. Grattan Institute Even within the same city, the differences are stark. In Sydney, people older than 70 in the affluent eastern suburbs (including Vaucluse, Point Piper and Bondi) were nearly twice as likely to have had an antiviral as those in Fairfield, in Sydney’s south-west.
Older people in leafy inner-eastern Melbourne (including Canterbury, Hawthorn and Kew) were 1.8 times more likely to have had an antiviral as those in Brimbank (which includes Sunshine) in the city’s west.
Why are people missing out?
COVID antivirals should be taken when symptoms first appear. While awareness of COVID antivirals is generally strong, people often don’t realise they would benefit from the medication. They wait until symptoms get worse and it is too late.
Frequent GP visits make a big difference. Our analysis found people 70 and older who see a GP more frequently were much more likely to be dispensed a COVID antiviral.
Regular visits give an opportunity for preventive care and patient education. For example, GPs can provide high-risk patients with “COVID treatment plans” as a reminder to get tested and seek treatment as soon as they are unwell.
Difficulty seeing a GP could help explain low antiviral use in rural areas. Compared to people in major cities, people in small rural towns have about 35% fewer GPs, see their GP about half as often, and are 30% more likely to report waiting too long for an appointment.
Just like for vaccination, a GP’s focus on antivirals probably matters, as does providing care that is accessible to people from different cultural backgrounds.
Care should go those who need it
Since the period we looked at, evidence has emerged that raises doubts about how effective antivirals are, particularly for people at lower risk of severe illness. That means getting vaccinated is more important than getting antivirals.
But all Australians who are eligible for antivirals should have the same chance of getting them.
These drugs have cost more than A$1.7 billion, with the vast majority of that money coming from the federal government. While dispensing rates have fallen, more than 30,000 packs of COVID antivirals were dispensed in August, costing about $35 million.
Such a huge investment shouldn’t be leaving so many people behind. Getting treatment shouldn’t depend on your income, cultural background or where you live. Instead, care should go to those who need it the most.
Getting antivirals shouldn’t depend on who your GP is. National Cancer Institute/Unsplash People born overseas have been 40% more likely to die from COVID than those born here. Indigenous Australians have been 60% more likely to die from COVID than non-Indigenous people. And the most disadvantaged people have been 2.8 times more likely to die from COVID than those in the wealthiest areas.
All those at-risk groups have been more likely to miss out on antivirals.
It’s not just a problem with antivirals. The same groups are also disproportionately missing out on COVID vaccination, compounding their risk of severe illness. The pattern is repeated for other important preventive health care, such as cancer screening.
A 3-step plan to meet patients’ needs
The federal government should do three things to close these gaps in preventive care.
First, the government should make Primary Health Networks (PHNs) responsible for reducing them. PHNs, the regional bodies responsible for improving primary care, should share data with GPs and step in to boost uptake in communities that are missing out.
Second, the government should extend its MyMedicare reforms. MyMedicare gives general practices flexible funding to care for patients who live in residential aged care or who visit hospital frequently. That approach should be expanded to all patients, with more funding for poorer and sicker patients. That will give GP clinics time to advise patients about preventive health, including COVID vaccines and antivirals, before they get sick.
Third, team-based pharmacist prescribing should be introduced. Then pharmacists could quickly dispense antivirals for patients if they have a prior agreement with the patient’s GP. It’s an approach that would also work for medications for chronic diseases, such as cardiovascular disease.
COVID antivirals, unlike vaccines, have been keeping up with new variants without the need for updates. If a new and more harmful variant emerges, or when a new pandemic hits, governments should have these systems in place to make sure everyone who needs treatment can get it fast.
In the meantime, fairer access to care will help close the big and persistent gaps in health between different groups of Australians.
Peter Breadon, Program Director, Health and Aged Care, Grattan Institute
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: