Seniors: Improve Blood Flow & Circulation In Your Legs
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Doug Weiss, a physiotherapist (and thus: a doctor of physical therapy), has advice on how and why to increase blood flow and circulation in your legs, keeping yourself healthier for longer and avoiding a lot of potential unpleasantries.
The exercises
The exercises here are not complex; they are as follows, and he suggests 3 sets of 10 reps of each, daily:
- Sitting ankle pumps: sitting on a chair or the edge of a bed, lift the toes up, then heels up, squeezing the muscles.
- Sitting knee extensions: sitting as before, kick one leg up until knee is straight, then switch legs.
- Heel raises: standing this time, with a sturdy support such as a countertop, raise on toes as high as possible, then lower heels back to the ground
- Pillow squats: placing pillows on a chair, cross hands on chest, and simply stand up and sit down—similar to the “getting up off the floor without using your hands” exercise, but an easier version.
For visuals on these, and more details including the specific benefits of each, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like:
4 Tips To Stand Without Using Hands ← this time it’s the full movement, from the floor, and this is a really important movement to be able to do, as it’s a big indicator of healthy longevity
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
When the Body Says No – by Dr. Gabor Maté
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We know that chronic stress is bad for us because of what it does to our cortisol levels, so what is the rest of this book about?
Dr. Gabor Maté is a medical doctor, heavily specialized in the impact of psychological trauma on long term physical health.
Here, he examies—as the subtitle promises—the connection between stress and disease. As it turns out, it’s not that simple.
We learn not just about the impact that stress has on our immune system (including increasing the risk of autoimmune disorders like rheumatoid arthritis), the cardiovascular system, and various other critical systems fo the body… But also:
- how environmental factors and destructive coping styles contribute to the onset of disease, and
- how traumatic events can warp people’s physical perception of pain
- how certain illnesses are associated with particular personality types.
This latter is not “astrology for doctors”, by the way. It has more to do with what coping strategies people are likely to employ, and thus what diseases become more likely to take hold.
The book has practical advice too, and it’s not just “reduce your stress”. Ideally, of course, indeed reduce your stress. But that’s a) obvious b) not always possible. Rather, Dr. Maté explains which coping strategies result in the least prevalence of disease.
In terms of writing style, the book is very much easy-reading, but be warned that (ironically) this isn’t exactly a feel-good book. There are lot of tragic stories in it. But, even those are very much well-worth reading.
Bottom line: if you (and/or a loved one) are suffering from stress, this book will give you the knowledge and understanding to minimize the harm that it will otherwise do.
Click here to check out When The Body Says No, and take good care of yourself; you’re important!
Share This Post
-
The Herbal Supplement That Rivals Prozac
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Flower Power: St. John’s Wort’s Drug-Level Effectiveness
St. John’s wort is a small yellow flower, extract of which can be bought inexpensively off-the-shelf in pretty much any pharmacy in most places.
It’s sold and used as a herbal mood-brightener.
Does it work?
Yes! It’s actually very effective. This is really uncontroversial, so we’ll keep it brief.
The main findings of studies are that St. John’s wort not only gives significant benefits over placebo, but also works about as well as prescription anti-depressants:
A systematic review of St. John’s wort for major depressive disorder
They also found that fewer people stop taking it, compared to how many stop taking antidepressants. It’s not known how much of this is because of its inexpensive, freely-accessible nature, and how much might be because it gave them fewer adverse side effects:
Clinical use of Hypericum perforatum (St John’s wort) in depression: A meta-analysis
How does it work?
First and foremost, it’s an SSRI—a selective serotonin reuptake inhibitor. Basically, it doesn’t add serotonin, but it makes whatever serotonin you have, last longer. Same as most prescription antidepressants. It also affects adenosine and GABA pathways, which in lay terms, means it promotes feelings of relaxation, in a similar way to many prescription antianxiety medications.
Mechanism of action of St John’s wort in depression: what is known?
Any problems we should know about?
Yes, definitely. To quote directly from the National Center for Complementary and Integrative Health:
St. John’s wort can weaken the effects of many medicines, including crucially important medicines such as:
- Antidepressants
- Birth control pills
- Cyclosporine, which prevents the body from rejecting transplanted organs
- Some heart medications, including digoxin and ivabradine
- Some HIV drugs, including indinavir and nevirapine
- Some cancer medications, including irinotecan and imatinib
- Warfarin, an anticoagulant (blood thinner)
- Certain statins, including simvastatin
I’ve read all that, and want to try it!
As ever, we don’t sell it (or anything else), but here’s an example product on Amazon.
Please be safe and do check with your doctor and/or pharmacist, though!
Share This Post
-
The No-Nonsense Meditation Book – by Dr. Steven Laureys
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve reviewed books about meditation before, and when we review books, we try to pick ones that have something that make them stand out from the others. So, what stands out in this case?
The author is a medical doctor and neurologist, with decades of experience focusing on neuronal plasticity and multimodel neural imaging. So, a little beyond “think happy thoughts”-style woo.
The style of the book is pop-science in tone, but with a lot of hard clinical science underpinning it and referenced throughout, as one would expect of a scientist of Dr. Laurey’s stature (with hundreds of peer-reviewed papers in top-level journals).
You may be wondering: is this a “how-to” book or a “why-to” book or a “what-happens” book? It’s all three.
The “how-to” is also, as the title suggests, no-nonsense. We are talking maximum results for minimum mystery here.
Bottom line: if you’d like to be able to take up a meditative practice and know exactly what it’s doing to your brain (quietening these parts, stimulating and physically growing those parts, etc) then this is the book for you.
Share This Post
Related Posts
-
Vision for Life, Revised Edition – by Dr. Meir Schneider
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The “ten steps” would be better called “ten exercises”, as they’re ten things that one can (and should) continue to do on an ongoing basis, rather than steps to progress through and then forget about.
We can’t claim to have tested the ten exercises for improvement (this reviewer has excellent eyesight and merely hopes to maintain such as she gets older) but the rationale is compelling, and the public testimonials abundant.
Dr. Schneider also talks about improving and correcting errors of refraction—in other words, doing the job of any corrective lenses you may currently be using. While he doesn’t claim miracles, it turns out there is a lot that can be done for common issues such as near-sightedness and far-sightedness, amongst others.
There’s a large section on managing more chronic pathological eye conditions than this reviewer previously knew existed; in some cases it’s a matter of making sure things don’t get worse, but in many others, there’s a recurring of theme of “and here’s an exercise for correcting that”.
The writing style is a little more “narrative prose” than we’d have liked, but the quality of the content more than makes up for any style preference issues.
Bottom line: the human body is a highly adaptive organism, and sometimes it just needs a little help to correct itself. This book can help with that.
Click here to check out Vision for Life, and take good care of yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Toe-Tapping Tip For Better Balance
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Balance is critical for health especially in older age, since it’s amazing how much else can go dramatically and suddenly wrong after a fall. So, here’s an exercise to give great balance and stability:
How to do it
You will need:
- Something to hold onto, such as a countertop
- A target on the floor, such as a mark or a coin
The steps:
- Lift one leg up, bring your foot forward, and tap the object in front of you.
- Then, bring that foot back to where it started.
- Next, switch to the other leg and tap.
- Alternate between your right and left legs, shifting back and forth.
- Your goal is to do this for 10 repetitions on each leg without holding on.
How it works:
Whenever you tap, you have to lift one leg up and reach it out in front of you. Doing this requires you to stand on one leg while moving a weight (namely: your other leg), which is something many people, especially upon getting older, are hesitant to do. If you’re unable to stand on one leg, let alone move your center of gravity (per the counterbalance of the other leg) while doing so, you may end up shuffling and walking with your feet sliding across the ground—something you really want to avoid.
For more on all of this plus a visual demonstration, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Fall Special ← this is about not falling, or, failing that, minimizing injury if you do
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What’s the difference between a food allergy and an intolerance?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
At one time or another, you’ve probably come across someone who is lactose intolerant and might experience some unpleasant gut symptoms if they have dairy. Maybe it’s you – food intolerances are estimated to affect up to 25% of Australians.
Meanwhile, cow’s milk allergy is one of the most common food allergies in infants and young children, affecting around one in 100 infants.
But what’s the difference between food allergies and food intolerances? While they might seem alike, there are some fundamental differences between the two.
Feel good studio/Shutterstock What is an allergy?
Australia has one of the highest rates of food allergies in the world. Food allergies can develop at any age but are more common in children, affecting more than 10% of one-year-olds and 6% of children at age ten.
A food allergy happens when the body’s immune system mistakenly reacts to certain foods as if they were dangerous. The most common foods that trigger allergies include eggs, peanuts and other nuts, milk, shellfish, fish, soy and wheat.
Mild to moderate signs of food allergy include a swollen face, lips or eyes; hives or welts on your skin; or vomiting. A severe allergic reaction (called anaphylaxis) can cause trouble breathing, persistent dizziness or collapse.
What is an intolerance?
Food intolerances (sometimes called non-allergic reactions) are also reactions to food, but they don’t involve your immune system.
For example, lactose intolerance is a metabolic condition that happens when the body doesn’t produce enough lactase. This enzyme is needed to break down the lactose (a type of sugar) in dairy products.
Food intolerances can also include reactions to natural chemicals in foods (such as salicylates, found in some fruits, vegetables, herbs and spices) and problems with artificial preservatives or flavour enhancers.
Lactose intolerance is caused by a problem with breaking down lactose in milk. Pormezz/Shutterstock Symptoms of food intolerances can include an upset stomach, headaches and fatigue, among others.
Food intolerances don’t cause life-threatening reactions (anaphylaxis) so are less dangerous than allergies in the short term, although they can cause problems in the longer term such as malnutrition.
We don’t know a lot about how common food intolerances are, but they appear to be more commonly reported than allergies. They can develop at any age.
It can be confusing
Some foods, such as peanuts and tree nuts, are more often associated with allergy. Other foods or ingredients, such as caffeine, are more often associated with intolerance.
Meanwhile, certain foods, such as cow’s milk and wheat or gluten (a protein found in wheat, rye and barley), can cause both allergic and non-allergic reactions in different people. But these reactions, even when they’re caused by the same foods, are quite different.
For example, children with a cow’s milk allergy can react to very small amounts of milk, and serious reactions (such as throat swelling or difficulty breathing) can happen within minutes. Conversely, many people with lactose intolerance can tolerate small amounts of lactose without symptoms.
There are other differences too. Cow’s milk allergy is more common in children, though many infants will grow out of this allergy during childhood.
Lactose intolerance is more common in adults, but can also sometimes be temporary. One type of lactose intolerance, secondary lactase deficiency, can be caused by damage to the gut after infection or with medication use (such as antibiotics or cancer treatment). This can go away by itself when the underlying condition resolves or the person stops using the relevant medication.
Whether an allergy or intolerance is likely to be lifelong depends on the food and the reason that the child or adult is reacting to it.
Allergies to some foods, such as milk, egg, wheat and soy, often resolve during childhood, whereas allergies to nuts, fish or shellfish, often (but not always) persist into adulthood. We don’t know much about how likely children are to grow out of different types of food intolerances.
How do you find out what’s wrong?
If you think you may have a food allergy or intolerance, see a doctor.
Allergy tests help doctors find out which foods might be causing your allergic reactions (but can’t diagnose food intolerances). There are two common types: skin prick tests and blood tests.
In a skin prick test, doctors put tiny amounts of allergens (the things that can cause allergies) on your skin and make small pricks to see if your body reacts.
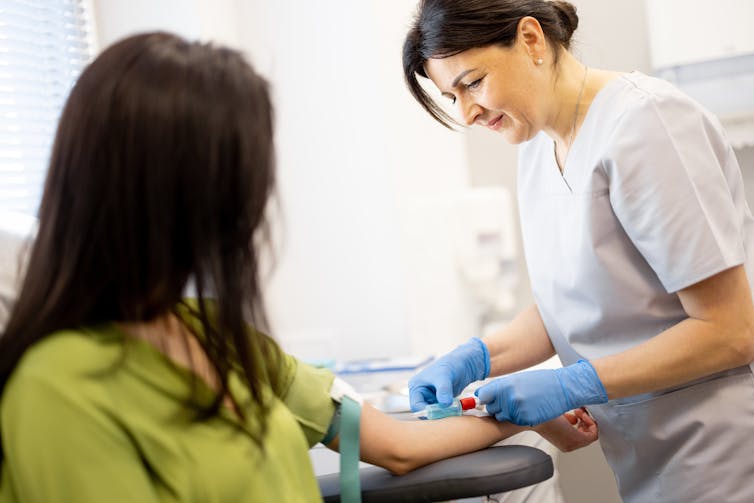
A blood test checks for allergen-specific immunoglobulin E (IgE) antibodies in your blood that show if you might be allergic to a particular food.
Blood tests can help diagnose allergies. RossHelen/Shutterstock Food intolerances can be tricky to figure out because the symptoms depend on what foods you eat and how much. To diagnose them, doctors look at your health history, and may do some tests (such as a breath test). They may ask you to keep a record of foods you eat and timing of symptoms.
A temporary elimination diet, where you stop eating certain foods, can also help to work out which foods you might be intolerant to. But this should only be done with the help of a doctor or dietitian, because eliminating particular foods can lead to nutritional deficiencies, especially in children.
Is there a cure?
There’s currently no cure for food allergies or intolerances. For allergies in particular, it’s important to strictly avoid allergens. This means reading food labels carefully and being vigilant when eating out.
However, researchers are studying a treatment called oral immunotherapy, which may help some people with food allergies become less sensitive to certain foods.
Whether you have a food allergy or intolerance, your doctor or dietitian can help you to make sure you’re eating the right foods.
Victoria Gibson, a Higher Degree by Research student and Research Officer at the School of Nursing, Midwifery and Social Work at the University of Queensland, and Rani Scott-Farmer, a Senior Research Assistant at the University of Queensland, contributed to this article.
Jennifer Koplin, Group Leader, Childhood Allergy & Epidemiology, The University of Queensland and Desalegn Markos Shifti, Postdoctoral Research Fellow, Child Health Research Centre, Faculty of Medicine, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: