Heart Healthy Diet Plan – by Stephen William
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve covered heart-healthy cooking books before, but variety is good, and boredom is an enemy of health, so let’s shake it up with a fresh stack of recipes!
After a brief overview of the relevant science (which if you’re a regular 10almonds reader, probably won’t be new to you), the author takes the reader on a 28-day journey. Yes, we know the subtitle says 30 days, but unless they carefully hid the other two days somewhere we didn’t find, there are “only” 28 inside. Perhaps the publisher heard it was a month and took creative license. Or maybe there’s a different edition. Either way…
Rather than merely giving a diet plan (though yes, he also does that), he gives a wide range of “spotlight ingredients”, such that many of the recipes, while great in and of themselves, can also be jumping-off points for those of us who like to take recipes and immediately do our own things to them.
Each day gets a breakfast, lunch, dinner, and he also covers drinks, desserts, and such like.
Notwithstanding the cover art being a lot of plants, the recipes are not entirely plant-based; there are a selection of fish dishes (and other seafood, e.g. shrimp) and also some dairy products (e.g. Greek yoghurt). The recipes are certainly very “plant-forward” though and many are just plants. If you’re a strict vegan though, this probably isn’t the book for you.
Bottom line: if you’d like to cook heart-healthy but are often stuck wondering “aaah, what to cook again today?”, then this is the book to get you out of any culinary creative block!
Click here to check out the Heart Healthy Diet Plan, and widen your heart-healthy repertoire!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Best Workouts for Women Over 40 To Give Your Metabolism A Makeover
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
After 40, the usual course of events goes: your lean muscle mass decreases, which slows your metabolism and makes it easier to gain fat. At the same time, bone density decreases, increasing the risk of osteoporosis and frailty. This leads to lower mobility, flexibility, and overall frustration.
But it doesn’t have to be that way! Fitness coach Jessica Cooke explains how:
It all depends on this
Strength training helps counteract these effects by increasing lean muscle mass, which boosts metabolism and fat burning. It also improves bone density, reducing the risk of osteoporosis. Plus, it builds strength, fitness, and a toned physique.
The best part? It doesn’t require long workouts—short, effective sessions work best.
While walking is very beneficial for general health, it doesn’t provide the resistance needed to build muscle. Without resistance, your body composition won’t change, and so your metabolism will remain the same. Strength training is essential for burning fat at rest and improving overall fitness.
You don’t have to do high-impact exercises or jumping to see results. Low-impact strength training is effective and gentle on the joints. Lifting weights or using your body weight in a controlled manner will help build muscle and improve strength.
Many women only do cardio and neglect strength training, leading to minimal progress. Another common mistake is overcomplicating workouts—simple, consistent strength training is all you need.
Aim to strength train three times per week for 20 minutes. Focus on compound movements that work multiple muscle groups, such as:
- squats
- lunges
- deadlifts
- press-ups
- shoulder presses
- upright rows
- planks
- glute bridges
- sit-ups
- Russian twists
Start with light (e.g. 2-3 kg) weights and maintain proper form.
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like:
Don’t Let Menopause Run You Down: 4 Critical Things Female Runners Should Know
Take care!
Share This Post
-
Paulina Porizkova (Former Supermodel) Talks Menopause, Aging, & Appearances
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Are supermodels destined to all eventually become “Grizabella the Glamor Cat”, a washed-up shell of their former glory? Is it true that “men grow cold as girls grow old, and we all lose our charms in the end”? And what—if anything—can we do about it?
Insights from a retired professional
Paulina Porizkova is 56, and she looks like she’s… 56, maybe? Perhaps a little younger or a bit older depending on the camera and lighting and such.
It’s usually the case, on glossy magazine covers and YouTube thumbnails, that there’s a 20-year difference between appearance and reality, but not here. Why’s that?
Porizkova noted that many celebrities of a similar age look younger, and felt bad. But then she noted that they’d all had various cosmetic work done, and looked for images of “real” women in their mid-50s, and didn’t find them.
Note: we at 10almonds do disagree with one thing here: we say that someone who has had cosmetic work done is no less real for it; it’s a simple matter of personal choice and bodily autonomy. She is, in our opinion, making the same mistake as people make when they say such things as “real people, rather than models”, as though models are not also real people.
Porizkova found modelling highly lucrative but dehumanizing, and did not enjoy the objectification involved—and she enjoyed even less, when she reached a certain age, negative comments about aging, and people being visibly wrong-footed when meeting her, as they had misconceptions based on past images.
As a child and younger adult through her modelling career, she felt very much “seen and not heard”, and these days, she realizes she’s more interesting now but feels less seen. Menopause coincided with her marriage ending, and she felt unattractive and ignored by her husband; she questioned her self-worth, and felt very bad about it. Then her husband (they had separated, but had not divorced) died, and she felt even more isolated—but it heightened her sensitivity to life.
In her pain and longing for recognition, she reached out through her Instagram, crying, and received positive feedback—but still she struggles with expressing needs and feeling worthy.
And yet, when it comes to looks, she embraces her wrinkles as a form of expression, and values her natural appearance over cosmetic alterations.
She describes herself as a work in progress—still broken, still needing cleansing and healing, but proud of how far she’s come so far, and optimistic with regard to the future.
For all this and more in her own words, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
The Many Faces Of Cosmetic Surgery
Take care!
Share This Post
-
Edamame vs Soybeans – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing edamame to soybeans, we picked the soybeans.
Why?
You may be thinking: aren’t edamame soybeans? And yes, yes they are. But just like our many instances of pitting Brassica oleracea vs Brassica oleracea (one species, many cultivars e.g. broccoli, cauliflower, kale, cabbage, Brussels sprouts, etc), there are still differences. In this case, edamame and soybeans aren’t even different cultivars, what are conventionally called edamame are just the young beans of the plant, while what are conventionally called soybeans are the mature beans of the plant.
The main nutritional difference is: as they get older, they lose vitamins and gain minerals. More on that later. But first, “main difference” isn’t “only difference”, so…
In terms of macros, edamame have more carbs, while soybeans have a little more fiber and a lot more protein. An easy win for the mature soybeans.
In the category of vitamins, edamame have more of vitamins A, B1, B3, B5, B9, C, E, K, and choline, while soybeans have more of vitamins B2 and B6. A clear win for edamame, this time.
When it comes to minerals, the nutritional tables are turned, and edamame have more manganese and zinc, while soybeans have more calcium, copper, iron, magnesium, phosphorus, potassium, and selenium. An easy win for soybeans.
Adding up the sections makes for a two-to-one victory for soybeans, but by all means enjoy either or both; diversity is good!
Want to learn more?
You might like to read:
What’s Your Plant Diversity Score?
Enjoy!
Share This Post
Related Posts
-
No, your aches and pains don’t get worse in the cold. So why do we think they do?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s cold and wet outside. As you get out of bed, you can feel it in your bones. Your right knee is flaring up again. That’ll make it harder for you to walk the dog or go to the gym. You think it must be because of the weather.
It’s a common idea, but a myth.
When we looked at the evidence, we found no direct link between most common aches and pains and the weather. In the first study of its kind, we found no direct link between the temperature or humidity with most joint or muscle aches and pains.
So why are so many of us convinced the weather’s to blame? Here’s what we think is really going on.
fongbeerredhot/Shutterstock Weather can be linked to your health
The weather is often associated with the risk of new and ongoing health conditions. For example, cold temperatures may worsen asthma symptoms. Hot temperatures increase the risk of heart problems, such as arrhythmia (irregular heartbeat), cardiac arrest and coronary heart disease.
Many people are also convinced the weather is linked to their aches and pains. For example, two in every three people with knee, hip or hand osteoarthritis say cold temperatures trigger their symptoms.
Musculoskeletal conditions affect more than seven million Australians. So we set out to find out whether weather is really the culprit behind winter flare-ups.
What we did
Very few studies have been specifically and appropriately designed to look for any direct link between weather changes and joint or muscle pain. And ours is the first to evaluate data from these particular studies.
We looked at data from more than 15,000 people from around the world. Together, these people reported more than 28,000 episodes of pain, mostly back pain, knee or hip osteoarthritis. People with rheumatoid arthritis and gout were also included.
We then compared the frequency of those pain reports between different types of weather: hot or cold, humid or dry, rainy, windy, as well as some combinations (for example, hot and humid versus cold and dry).
Bad back on a cold day? We wanted to know if the weather was really to blame. Pearl PhotoPix/Shutterstock What we found
We found changes in air temperature, humidity, air pressure and rainfall do not increase the risk of knee, hip or lower back pain symptoms and are not associated with people seeking care for a new episode of arthritis.
The results of this study suggest we do not experience joint or muscle pain flare-ups as a result of changes in the weather, and a cold day will not increase our risk of having knee or back pain.
In order words, there is no direct link between the weather and back, knee or hip pain, nor will it give you arthritis.
It is important to note, though, that very cold air temperatures (under 10°C) were rarely studied so we cannot make conclusions about worsening symptoms in more extreme changes in the weather.
The only exception to our findings was for gout, an inflammatory type of arthritis that can come and go. Here, pain increased in warmer, dry conditions.
Gout has a very different underlying biological mechanism to back pain or knee and hip osteoarthritis, which may explain our results. The combination of warm and dry weather may lead to increased dehydration and consequently increased concentration of uric acid in the blood, and deposition of uric acid crystals in the joint in people with gout, resulting in a flare-up.
Why do people blame the weather?
The weather can influence other factors and behaviours that consequently shape how we perceive and manage pain.
For example, some people may change their physical activity routine during winter, choosing the couch over the gym. And we know prolonged sitting, for instance, is directly linked to worse back pain. Others may change their sleep routine or sleep less well when it is either too cold or too warm. Once again, a bad night’s sleep can trigger your back and knee pain.
Likewise, changes in mood, often experienced in cold weather, trigger increases in both back and knee pain.
So these changes in behaviour over winter may contribute to more aches and pains, and not the weather itself.
Believing our pain will feel worse in winter (even if this is not the case) may also make us feel worse in winter. This is known as the nocebo effect.
When it’s cold outside, we may be less active. Anna Nass/Shutterstock What to do about winter aches and pains?
It’s best to focus on risk factors for pain you can control and modify, rather than ones you can’t (such as the weather).
You can:
- become more physically active. This winter, and throughout the year, aim to walk more, or talk to your health-care provider about gentle exercises you can safely do at home, with a physiotherapist, personal trainer or at the pool
- lose weight if obese or overweight, as this is linked to lower levels of joint pain and better physical function
- keep your body warm in winter if you feel some muscle tension in uncomfortably cold conditions. Also ensure your bedroom is nice and warm as we tend to sleep less well in cold rooms
- maintain a healthy diet and avoid smoking or drinking high levels of alcohol. These are among key lifestyle recommendations to better manage many types of arthritis and musculoskeletal conditions. For people with back pain, for example, a healthy lifestyle is linked with higher levels of physical function.
Manuela Ferreira, Professor of Musculoskeletal Health, Head of Musculoskeletal Program, George Institute for Global Health and Leticia Deveza, Rheumatologist and Research Fellow, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Red Light, Go!
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Casting Yourself In A Healthier Light
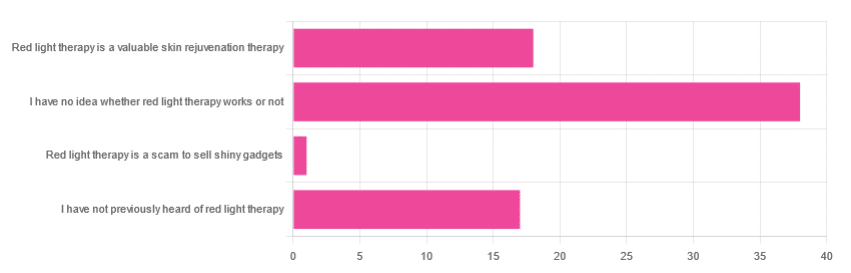
In Tuesday’s newsletter, we asked you for your opinion of red light therapy (henceforth: RLT), and got the above-depicted, below-described, set of responses:
- About 51% said “I have no idea whether light therapy works or not”
- About 24% said “Red light therapy is a valuable skin rejuvenation therapy”
- About 23% said “I have not previously heard of red light therapy”
- One (1) person said: “Red light therapy is a scam to sell shiny gadgets”
A number of subscribers wrote with personal anecdotes of using red light therapy to beneficial effect, for example:
❝My husband used red light therapy after surgery on his hand. It did seem to speed healing of the incision and there is very minimal scarring. I would like to know if the red light really helped or if he was just lucky❞
~ 10almonds subscriber
And one wrote to report having observed mixed results amongst friends, per:
❝Some people it works, others I’ve seen it breaks them out❞
~ 10almonds subscriber
So, what does the science say?
RLT rejuvenates skin, insofar as it reduces wrinkles and fine lines: True or False?
True! This one’s pretty clear-cut, so we’ll just give one example study of many, which found:
❝The treated subjects experienced significantly improved skin complexion and skin feeling, profilometrically assessed skin roughness, and ultrasonographically measured collagen density.
The blinded clinical evaluation of photographs confirmed significant improvement in the intervention groups compared with the control❞
~ Dr. Alexander Wunsch & Dr. Karsten Matuschka
RLT helps speed up healing of wounds: True or False?
True! There is less science for this than the above claim, but the studies that have been done are quite compelling, for example this NASA technology study found that…
❝LED produced improvement of greater than 40% in musculoskeletal training injuries in Navy SEAL team members, and decreased wound healing time in crew members aboard a U.S. Naval submarine.❞
Read more: Effect of NASA light-emitting diode irradiation on wound healing
RLT’s benefits are only skin-deep: True or False?
False, probably, but we’d love to see more science for this, to be sure.
However, it does look like wavelengths in the near-infrared spectrum reduce the abnormal tau protein and neurofibrillary tangles associated with Alzheimer’s disease, resulting in increased blood flow to the brain, and a decrease in neuroinflammation:
Therapeutic Potential of Photobiomodulation In Alzheimer’s Disease: A Systematic Review
Would you like to try RLT for yourself?
There are some contraindications, for example:
- if you have photosensitivity (for obvious reasons)
- if you have Lupus (mostly because of the above)
- if you have hyperthyroidism (because if you use RLT to your neck as well as face, it may help stimulate thyroid function, which in your case is not what you want)
As ever, please check with your own doctor if you’re not completely sure; we can’t cover all bases here, and cannot speak for your individual circumstances.
For most people though, it’s very safe, and if you’d like to try it, here’s an example product on Amazon, and by all means do read reviews and shop around for the ideal device for you
Take care! 😎
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What’s the difference between autism and Asperger’s disorder?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Swedish climate activist Greta Thunberg describes herself as having Asperger’s while others on the autism spectrum, such as Australian comedian Hannah Gatsby, describe themselves as “autistic”. But what’s the difference?
Today, the previous diagnoses of “Asperger’s disorder” and “autistic disorder” both fall within the diagnosis of autism spectrum disorder, or ASD.
Autism describes a “neurotype” – a person’s thinking and information-processing style. Autism is one of the forms of diversity in human thinking, which comes with strengths and challenges.
When these challenges become overwhelming and impact how a person learns, plays, works or socialises, a diagnosis of autism spectrum disorder is made.
Where do the definitions come from?
The Diagnostic and Statistical Manual of Mental Disorders (DSM) outlines the criteria clinicians use to diagnose mental illnesses and behavioural disorders.
Between 1994 and 2013, autistic disorder and Asperger’s disorder were the two primary diagnoses related to autism in the fourth edition of the manual, the DSM-4.
In 2013, the DSM-5 collapsed both diagnoses into one autism spectrum disorder.
How did we used to think about autism?
The two thinkers behind the DSM-4 diagnostic categories were Baltimore psychiatrist Leo Kanner and Viennese paediatrician Hans Asperger. They described the challenges faced by people who were later diagnosed with autistic disorder and Asperger’s disorder.
Kanner and Asperger observed patterns of behaviour that differed to typical thinkers in the domains of communication, social interaction and flexibility of behaviour and thinking. The variance was associated with challenges in adaptation and distress.
Kanner and Asperger described different thinking patterns in children with autism.
Roman Nerud/ShutterstockBetween the 1940s and 1994, the majority of those diagnosed with autism also had an intellectual disability. Clinicians became focused on the accompanying intellectual disability as a necessary part of autism.
The introduction of Asperger’s disorder shifted this focus and acknowledged the diversity in autism. In the DSM-4 it superficially looked like autistic disorder and Asperger’s disorder were different things, with the Asperger’s criteria stating there could be no intellectual disability or delay in the development of speech.
Today, as a legacy of the recognition of the autism itself, the majority of people diagnosed with autism spectrum disorder – the new term from the DSM-5 – don’t a have an accompanying intellectual disability.
What changed with ‘autism spectrum disorder’?
The move to autism spectrum disorder brought the previously diagnosed autistic disorder and Asperger’s disorder under the one new diagnostic umbrella term.
It made clear that other diagnostic groups – such as intellectual disability – can co-exist with autism, but are separate things.
The other major change was acknowledging communication and social skills are intimately linked and not separable. Rather than separating “impaired communication” and “impaired social skills”, the diagnostic criteria changed to “impaired social communication”.
The introduction of the spectrum in the diagnostic term further clarified that people have varied capabilities in the flexibility of their thinking, behaviour and social communication – and this can change in response to the context the person is in.
Why do some people prefer the old terminology?
Some people feel the clinical label of Asperger’s allowed a much more refined understanding of autism. This included recognising the achievements and great societal contributions of people with known or presumed autism.
The contraction “Aspie” played an enormous part in the shift to positive identity formation. In the time up to the release of the DSM-5, Tony Attwood and Carol Gray, two well known thinkers in the area of autism, highlighted the strengths associated with “being Aspie” as something to be proud of. But they also raised awareness of the challenges.
What about identity-based language?
A more recent shift in language has been the reclamation of what was once viewed as a slur – “autistic”. This was a shift from person-first language to identity-based language, from “person with autism spectrum disorder” to “autistic”.
The neurodiversity rights movement describes its aim to push back against a breach of human rights resulting from the wish to cure, or fundamentally change, people with autism.
Autism is one of the forms of diversity in human thinking, which comes with strengths and challenges.
Alex and Maria photo/ShutterstockThe movement uses a “social model of disability”. This views disability as arising from societies’ response to individuals and the failure to adjust to enable full participation. The inherent challenges in autism are seen as only a problem if not accommodated through reasonable adjustments.
However the social model contrasts itself against a very outdated medical or clinical model.
Current clinical thinking and practice focuses on targeted supports to reduce distress, promote thriving and enable optimum individual participation in school, work, community and social activities. It doesn’t aim to cure or fundamentally change people with autism.
A diagnosis of autism spectrum disorder signals there are challenges beyond what will be solved by adjustments alone; individual supports are also needed. So it’s important to combine the best of the social model and contemporary clinical model.
Andrew Cashin, Professor of Nursing, School of Health and Human Sciences, Southern Cross University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: