
Feminist narratives are being hijacked to market medical tests not backed by evidence
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Corporations have used feminist language to promote their products for decades. In the 1980s, companies co-opted messaging about female autonomy to encourage women’s consumption of unhealthy commodities, such as tobacco and alcohol.
Today, feminist narratives around empowerment and women’s rights are being co-opted to market interventions that are not backed by evidence across many areas of women’s health. This includes by commercial companies, industry, mass media and well-intentioned advocacy groups.
Some of these health technologies, tests and treatments are useful in certain situations and can be very beneficial to some women.
However, promoting them to a large group of asymptomatic healthy women that are unlikely to benefit, or without being transparent about the limitations, runs the risk of causing more harm than good. This includes inappropriate medicalisation, overdiagnosis and overtreatment.
In our analysis published today in the BMJ, we examine this phenomenon in two current examples: the anti-mullerian hormone (AMH) test and breast density notification.
The AMH test
The AMH test is a blood test associated with the number of eggs in a woman’s ovaries and is sometimes referred to as the “egg timer” test.
Although often used in fertility treatment, the AMH test cannot reliably predict the likelihood of pregnancy, timing to pregnancy or specific age of menopause. The American College of Obstetricians and Gynaecologists therefore strongly discourages testing for women not seeking fertility treatment.

Anastasia Vityukova/Unsplash
Despite this, several fertility clinics and online companies market the AMH test to women not even trying to get pregnant. Some use feminist rhetoric promising empowerment, selling the test as a way to gain personalised insights into your fertility. For example, “you deserve to know your reproductive potential”, “be proactive about your fertility” and “knowing your numbers will empower you to make the best decisions when family planning”.
The use of feminist marketing makes these companies appear socially progressive and champions of female health. But they are selling a test that has no proven benefit outside of IVF and cannot inform women about their current or future fertility.
Our recent study found around 30% of women having an AMH test in Australia may be having it for these reasons.
Misleading women to believe that the test can reliably predict fertility can create a false sense of security about delaying pregnancy. It can also create unnecessary anxiety, pressure to freeze eggs, conceive earlier than desired, or start fertility treatment when it may not be needed.
While some companies mention the test’s limitations if you read on, they are glossed over and contradicted by the calls to be proactive and messages of empowerment.
Breast density notification
Breast density is one of several independent risk factors for breast cancer. It’s also harder to see cancer on a mammogram image of breasts with high amounts of dense tissue than breasts with a greater proportion of fatty tissue.
While estimates vary, approximately 25–50% of women in the breast screening population have dense breasts.
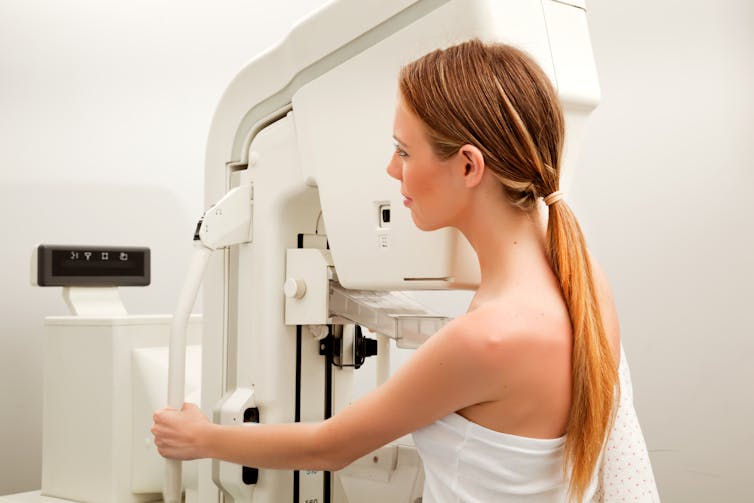
Tyler Olsen/Shutterstock
Stemming from valid concerns about the increased risk of cancer, advocacy efforts have used feminist language around women’s right to know such as “women need to know the truth” and “women can handle the truth” to argue for widespread breast density notification.
However, this simplistic messaging overlooks that this is a complex issue and that more data is still needed on whether the benefits of notifying and providing additional screening or tests to women with dense breasts outweigh the harms.
Additional tests (ultrasound or MRI) are now being recommended for women with dense breasts as they have the ability to detect more cancer. Yet, there is no or little mention of the lack of robust evidence showing that it prevents breast cancer deaths. These extra tests also have out-of-pocket costs and high rates of false-positive results.
Large international advocacy groups are also sponsored by companies that will financially benefit from women being notified.
While stronger patient autonomy is vital, campaigning for breast density notification without stating the limitations or unclear evidence of benefit may go against the empowerment being sought.
Ensuring feminism isn’t hijacked
Increased awareness and advocacy in women’s health are key to overcoming sex inequalities in health care.
But we need to ensure the goals of feminist health advocacy aren’t undermined through commercially driven use of feminist language pushing care that isn’t based on evidence. This includes more transparency about the risks and uncertainties of health technologies, tests and treatments and greater scrutiny of conflicts of interests.
Health professionals and governments must also ensure that easily understood, balanced information based on high quality scientific evidence is available. This will enable women to make more informed decisions about their health.
Brooke Nickel, NHMRC Emerging Leader Research Fellow, University of Sydney and Tessa Copp, NHMRC Emerging Leader Research Fellow, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Heal & Reenergize Your Brain With Optimized Sleep Cycles
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Sometimes 8 hours sleep can result in grogginess while 6 hours can result in waking up fresh as a daisy, so what gives? Dr. Tracey Marks explains, in this short video.
Getting more than Zs in
Sleep involves 90-minute cycles, usually in 4 stages:
- Stage 1: (drowsy state): brief muscle jerks; lasts a few minutes.
- Stage 2: (light sleep): sleep spindles for memory consolidation; 50% of total sleep.
- Stage 3 (deep sleep): tissue repair, immune support, brain toxin removal via the glymphatic system.
- Stage 4 (REM sleep): emotional processing, creativity, problem-solving, and dreaming.
Some things can disrupt some or all of those. To give a few common examples:
- Alcohol: impairs REM sleep.
- Caffeine: hinders deep sleep even if consumed hours before bed.
- Screentime: delays sleep onset due to blue light (but not by much); the greater problem is that it can also disrupt REM sleep due to mental stimulation.
To optimize things, Dr. Marks recommends:
- 90-minute rule: plan sleep to align with full cycles (e.g: 22:30 to 06:00 = 7½ hours, which is 5x 90-minute cycles).
- Smart alarms: use sleep-tracking apps with built-in alarm, to wake you up during light sleep phases.
- Strategic naps: keep naps to 20 minutes or a full 90-minute cycle.
- Pink noise: improves deep sleep.
- Meal timing: avoid eating within 3 hours of bedtime.
- Natural light: get morning light exposure in the morning to strengthen circadian rhythm.
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Calculate (And Enjoy) The Perfect Night’s Sleep
Take care!
Share This Post
-
Vegan Eager for Milk Alternatives
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Q: Thanks for the info about dairy. As a vegan, I look forward to a future comment about milk alternatives
Thanks for bringing it up! What we research and write about is heavily driven by subscriber feedback, so notes like this really help us know there’s an audience for a given topic!
We’ll do a main feature on it, to do it justice. Watch out for Research Review Monday!
Share This Post
-
Fasting Without Crashing?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Intermittent Fasting: What’s the truth?
Before we get to facts and fictions, let’s quickly cover:
What is Intermittent Fasting?
Intermittent Fasting (IF) is an umbrella term for various kinds of time-restricted fasting, based on a schedule. Types include:
Time-restricted IF, for example:
- 16:8—Fast for 16 hours, eat during an 8-hour window
- 18:6–Fast for 18 hours, eat during a 6-hour window
- 20:4—Fast for 20 hours, eat during a 4-hour window
24hr fasting, including:
- Eat Stop Eat—basically, take a day off from eating once a week
- Alternate Day Fasting—a more extreme version of the above; it is what it sounds like; eat one day, fast the next, repeat
Non-fast fasting, e.g:
- 5:2—Eat normally for 5 days, have a very reduced calorie intake (⅓ of normal intake) for the other 2 days
- Fruit Fasting—have a small amount of fruit on “fast” days, but no other food
- The Warrior Diet—as above, but include a small amount of non-starchy vegetables
Why IF?
While IF is perhaps most commonly undertaken as a means of fat loss or fat management (i.e., keeping fat down when it is already low), others cite different reasons, such as short term cognitive performance or long-term longevity.
But… Does it work?
Here we get into the myth-busting bit!
“IF promotes weight loss”
Mix of True and False. It can! But it also doesn’t have to. If you’re a bodybuilder who downs 4,000 calories in your 4hr eating window, you’re probably not going to lose weight! For such people, this is of course “a feature, not a bug” of IF—especially as it has been found that, in an acute study, IF did not adversely impact muscle protein synthesis.
“IF promotes fat loss, without eating less”
Broadly True. IF was found to be potentially equal to, but not necessarily better than, eating less.
“IF provides metabolic benefits for general health”
Broadly True. IF (perhaps counterintuitively) decreases the risk of insulin resistance, and also has anti-inflammatory effects, benefits a healthy gut microbiome, and promotes healthy autophagy (which as we noted in a previous edition of 10almonds, is important against both aging and cancer)
However, results vary according to which protocol you’re observing…
For what it’s worth, 16:8 is perhaps the most-studied protocol. Because such studies tend to have the eating window from midday to 8pm, this means that—going against popular wisdom—part of the advice here is basically “skip breakfast”.
“Unlike caloric restriction, IF is sustainable and healthy as a long-term protocol”
Broadly True. Of course, there’s a slight loophole here in that IF is loosely defined—technically everyone fasts while they’re sleeping, at the very least!
However, for the most commonly-studied IF method (16:8), this is generally very sustainable and healthy and for most people.
On the other hand, a more extreme method such as Alternate Day Fasting, may be trickier to sustain (even if it remains healthy to do so), because it’s been found that hunger does not decrease on fasting days—ie, the body does not “get used to it”.
The American Journal of Clinical Nutrition wrote:
❝Alternate-day fasting was feasible in nonobese subjects, and fat oxidation increased. However, hunger on fasting days did not decrease, perhaps indicating the unlikelihood of continuing this diet for extended periods of time. Adding one small meal on a fasting day may make this approach to dietary restriction more acceptable.❞
“IF improves mood and cognition”
Mix of True and False (plus an honest “We Don’t Know” from researchers).
Many studies have found benefits to both mood and cognition, but in the short-term, fasting can make people “hangry” (or: “experience irritability due to low blood sugar levels”, as the scientists put it), and in the long term, it can worsen symptoms of depression for those who already experience such—although some studies have found it can help alleviate depressive symptoms.
Basically this is one where researchers typically append the words “more research is needed” to their summaries.
“Anyone can do IF”
Definitely False, unless going by the absolute broadest possible interpretation of what constitutes “Intermittent Fasting” to the point of disingenuity.
For example, if you are Type 1 Diabetic, and your blood sugars are hypo, and you wait until tomorrow to correct that, you will stand a good chance of going into a coma instead. So please don’t.
(On the other hand, IF may help achieve remission of type 2 diabetes)
Lastly, IF is broadly not recommend to children and adolescents, anyone pregnant or breastfeeding, and certain underlying health conditions not mentioned above (we’re not going to try to give an exhaustive list here, but basically, if you have a chronic health condition, we recommend you check with your doctor first).
WHICH APP?
Choosing a fasting app
Thinking of giving IF a try and would like a little extra help? We’ve got you covered!
Check out: Livewire’s 7 Best Intermittent Fasting Apps of 2023
Prefer to just trust us with a recommendation?
We like BodyFast—it’s #2 on Lifewire’s list, but it has an array of pre-set plans to choose from (unlike Lifewire’s #1, Zero), and plenty of clear tracking, scheduling help, and motivational features.
Both are available on both iOS and Android:
Share This Post
Related Posts
-
Cranberry juice really can help with UTIs – and reduce reliance on antibiotics
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Cranberry juice has been used medicinally for centuries. Our new research indicates it should be a normal aspect of urinary tract infection (UTI) management today.
While some benefits of cranberry compounds for the prevention of UTIs have been suspected for some time, it hasn’t been clear whether the benefits from cranberry juice were simply from drinking more fluid, or something in the fruit itself.
For our study, published this week, we combined and collectively assessed 3,091 participants across more than 20 clinical trials.
Our analysis indicates that increasing liquids reduces the rate of UTIs compared with no treatment, but cranberry in liquid form is even better at reducing UTIs and antibiotic use.
Julie Falk/Flickr, CC BY-NC-ND Are UTIs really that bad?
Urinary tract infections affect more than 50% of women and 20% of men in their lifetime.
Most commonly, UTIs are caused from the bug called Escherichia coli (E.coli). This bug lives harmlessly in our intestines, but can cause infection in the urinary tract. This is why, particularly for women, it is recommended people wipe from front to back after using the toilet.
An untreated UTI can move up to the kidneys and cause even more serious illness.
Even when not managing infection, many people are anxious about contracting a UTI. Sexually active women, pregnant women and older women may all be at increased risk.
Why cranberries?
To cause a UTI, the bacteria need to attach to the wall of the urinary bladder. Increasing fluids helps to flush out bacteria before it attaches (or makes its way up into the bladder).
Some beneficial compounds in cranberry, such as proanthocyanidins (also called condensed tannins), prevent the bacteria from attaching to the wall itself.
While there are treatments, over 90% of the bugs that cause UTIs exhibit some form of microbial resistance. This suggests that they are rapidly changing and some cases of UTI might be left untreatable.
The juice of cranberries has long been thought to have infection-fighting properties. duckeesue/Shutterstock What we found
Our analysis showed a 54% lower rate of UTIs from cranberry juice consumption compared to no treatment. This means that significantly fewer participants who regularly consumed cranberry juice (most commonly around 200 millilitres each day) reported having a UTI during the periods assessed in the studies we analysed.
Cranberry juice was also linked to a 49% lower rate of antibiotic use than placebo liquid and a 59% lower rate than no treatment, based on analysis of indirect and direct effects across six studies. The use of cranberry compounds, whether in drinks or tablet form, also reduced the prevalence of symptoms associated with UTIs.
While some studies we included presented conflicts of interest (such as receiving funding from cranberry companies), we took this “high risk of bias” into account when analysing the data.
The study found extra hydration helped but not to the same extent as cranberry juice. Pixelshot/Shutterstock So, when can cranberry juice help?
We found three main benefits of cranberry juice for UTIs.
1. Reduced rates of infections
Increasing fluids (for example, drinking more water) reduced the prevalence of UTIs, and taking cranberry compounds (such as tablets) was also beneficial. But the most benefits were identified from increasing fluids and taking cranberry compounds at the same time, such as with cranberry juice.
2. Reduced use of antibiotics
The data shows cranberry juice lowers the need to use antibiotics by 59%. This was identified as fewer participants in randomised cranberry juice groups required antibiotics.
Increasing fluid intake also helped reduce antibiotic use (by 25%). But this was not as useful as increasing fluids at the same time as using cranberry compounds.
Cranberry compounds alone (such as tablets without associated increases in fluid intake) did not affect antibiotic use.
3. Reducing symptoms
Taking cranberry compounds (in any form, liquid or tablet) reduced the symptoms of UTIs, as measured in the overall data, by more than five times.
Take home advice
While cranberry juice cannot treat a UTI, it can certainly be part of UTI management.
If you suspect that you have a UTI, see your GP as soon as possible.
Christian Moro, Associate Professor of Science & Medicine, Bond University and Charlotte Phelps, Senior Teaching Fellow, Medical Program, Bond University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Pain Doesn’t Belong on a Scale of Zero to 10
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Over the past two years, a simple but baffling request has preceded most of my encounters with medical professionals: “Rate your pain on a scale of zero to 10.”
I trained as a physician and have asked patients the very same question thousands of times, so I think hard about how to quantify the sum of the sore hips, the prickly thighs, and the numbing, itchy pain near my left shoulder blade. I pause and then, mostly arbitrarily, choose a number. “Three or four?” I venture, knowing the real answer is long, complicated, and not measurable in this one-dimensional way.
Pain is a squirrely thing. It’s sometimes burning, sometimes drilling, sometimes a deep-in-the-muscles clenching ache. Mine can depend on my mood or how much attention I afford it and can recede nearly entirely if I’m engrossed in a film or a task. Pain can also be disabling enough to cancel vacations, or so overwhelming that it leads people to opioid addiction. Even 10+ pain can be bearable when it’s endured for good reason, like giving birth to a child. But what’s the purpose of the pains I have now, the lingering effects of a head injury?
The concept of reducing these shades of pain to a single number dates to the 1970s. But the zero-to-10 scale is ubiquitous today because of what was called a “pain revolution” in the ’90s, when intense new attention to addressing pain — primarily with opioids — was framed as progress. Doctors today have a fuller understanding of treating pain, as well as the terrible consequences of prescribing opioids so readily. What they are learning only now is how to better measure pain and treat its many forms.
About 30 years ago, physicians who championed the use of opioids gave robust new life to what had been a niche specialty: pain management. They started pushing the idea that pain should be measured at every appointment as a “fifth vital sign.” The American Pain Society went as far as copyrighting the phrase. But unlike the other vital signs — blood pressure, temperature, heart rate, and breathing rate — pain had no objective scale. How to measure the unmeasurable? The society encouraged doctors and nurses to use the zero-to-10 rating system. Around that time, the FDA approved OxyContin, a slow-release opioid painkiller made by Purdue Pharma. The drugmaker itself encouraged doctors to routinely record and treat pain, and aggressively marketed opioids as an obvious solution.
To be fair, in an era when pain was too often ignored or undertreated, the zero-to-10 rating system could be regarded as an advance. Morphine pumps were not available for those cancer patients I saw in the ’80s, even those in agonizing pain from cancer in their bones; doctors regarded pain as an inevitable part of disease. In the emergency room where I practiced in the early ’90s, prescribing even a few opioid pills was a hassle: It required asking the head nurse to unlock a special prescription pad and making a copy for the state agency that tracked prescribing patterns. Regulators (rightly) worried that handing out narcotics would lead to addiction. As a result, some patients in need of relief likely went without.
After pain doctors and opioid manufacturers campaigned for broader use of opioids — claiming that newer forms were not addictive, or much less so than previous incarnations — prescribing the drugs became far easier and were promoted for all kinds of pain, whether from knee arthritis or back problems. As a young doctor joining the “pain revolution,” I probably asked patients thousands of times to rate their pain on a scale of zero to 10 and wrote many scripts each week for pain medication, as monitoring “the fifth vital sign” quickly became routine in the medical system. In time, a zero-to-10 pain measurement became a necessary box to fill in electronic medical records. The Joint Commission on the Accreditation of Healthcare Organizations made regularly assessing pain a prerequisite for medical centers receiving federal health care dollars. Medical groups added treatment of pain to their list of patient rights, and satisfaction with pain treatment became a component of post-visit patient surveys. (A poor showing could mean lower reimbursement from some insurers.)
But this approach to pain management had clear drawbacks. Studies accumulated showing that measuring patients’ pain didn’t result in better pain control. Doctors showed little interest in or didn’t know how to respond to the recorded answer. And patients’ satisfaction with their doctors’ discussion of pain didn’t necessarily mean they got adequate treatment. At the same time, the drugs were fueling the growing opioid epidemic. Research showed that an estimated 3% to 19% of people who received a prescription for pain medication from a doctor developed an addiction.
Doctors who wanted to treat pain had few other options, though. “We had a good sense that these drugs weren’t the only way to manage pain,” Linda Porter, director of the National Institutes of Health’s Office of Pain Policy and Planning, told me. “But we didn’t have a good understanding of the complexity or alternatives.” The enthusiasm for narcotics left many varietals of pain underexplored and undertreated for years. Only in 2018, a year when nearly 50,000 Americans died of an overdose, did Congress start funding a program — the Early Phase Pain Investigation Clinical Network, or EPPIC-Net — designed to explore types of pain and find better solutions. The network connects specialists at 12 academic specialized clinical centers and is meant to jump-start new research in the field and find bespoke solutions for different kinds of pain.
A zero-to-10 scale may make sense in certain situations, such as when a nurse uses it to adjust a medication dose for a patient hospitalized after surgery or an accident. And researchers and pain specialists have tried to create better rating tools — dozens, in fact, none of which was adequate to capture pain’s complexity, a European panel of experts concluded. The Veterans Health Administration, for instance, created one that had supplemental questions and visual prompts: A rating of 5 correlated with a frown and a pain level that “interrupts some activities.” The survey took much longer to administer and produced results that were no better than the zero-to-10 system. By the 2010s, many medical organizations, including the American Medical Association and the American Academy of Family Physicians, were rejecting not just the zero-to-10 scale but the entire notion that pain could be meaningfully self-reported numerically by a patient.
In the years that opioids had dominated pain remedies, a few drugs — such as gabapentin and pregabalin for neuropathy, and lidocaine patches and creams for musculoskeletal aches — had become available. “There was a growing awareness of the incredible complexity of pain — that you would have to find the right drugs for the right patients,” Rebecca Hommer, EPPIC-Net’s interim director, told me. Researchers are now looking for biomarkers associated with different kinds of pain so that drug studies can use more objective measures to assess the medications’ effect. A better understanding of the neural pathways and neurotransmitters that create different types of pain could also help researchers design drugs to interrupt and tame them.
Any treatments that come out of this research are unlikely to be blockbusters like opioids; by design, they will be useful to fewer people. That also makes them less appealing prospects to drug companies. So EPPIC-Net is helping small drug companies, academics, and even individual doctors design and conduct early-stage trials to test the safety and efficacy of promising pain-taming molecules. That information will be handed over to drug manufacturers for late-stage trials, all with the aim of getting new drugs approved by the FDA more quickly.
The first EPPIC-Net trials are just getting underway. Finding better treatments will be no easy task, because the nervous system is a largely unexplored universe of molecules, cells, and electronic connections that interact in countless ways. The 2021 Nobel Prize in Physiology or Medicine went to scientists who discovered the mechanisms that allow us to feel the most basic sensations: cold and hot. In comparison, pain is a hydra. A simple number might feel definitive. But it’s not helping anyone make the pain go away.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Best Foods For Collagen Production
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Andrea Suarez gives us the low-down on collagen synthesis and maintenance. Collagen is the most abundant protein in our body, and it can be fairly described as “the stuff that holds us together”. It’s particularly important for joints and bones too, though many people’s focus on it is for the skin. Whatever your priorities, collagen levels are something it pays to be mindful of, as they usually drop quite sharply after a certain age. What certain age? Well, that depends a lot on you, and your diet and lifestyle. But it can start to decline from the age of 30 with often noticeable drop-offs in one’s mid-40s and again in one’s mid-60s.
Showing us what we’re made of
There’s a lot more to having good collagen levels than just how much collagen we consume (which for vegetarians/vegans, will be “none”, unless using the “except if for medical reasons” exemption, which is probably a little tenuous in the case of collagen but nevertheless it’s a possibility; this exemption is usually one that people use for, say, a nasal spray vaccine that contains gelatine, or a medicinal tablet that contains lactose, etc).
Rather, having good collagen levels is also a matter of what we eat that allows us to synthesize our own collagen (which includes: its ingredients, and various “helper” nutrients), as well as what dietary adjustments we make to avoid our extant collagen getting broken down, degraded, and generally lost.
Here’s what Dr. Suarez recommends:
Protein-rich foods (but watch out)
- Protein is essential for collagen production.
- Sources: fish, soy, lean meats (but not red meats, which—counterintuitively—degrade collagen), eggs, lentils.
- Egg whites are high in lysine, vital for collagen synthesis.
- Bone broth is a natural source of collagen.
Omega-3 fatty acids
- Omega-3s are anti-inflammatory and protect skin collagen.
- Sources: walnuts, chia seeds, flax seeds, fatty fish (e.g. mackerel, sardines).
Leafy greens
- Leafy dark green vegetables (e.g. kale, spinach) are rich in vitamins C and B9.
- Vitamin C is crucial for collagen synthesis and acts as an antioxidant.
- Vitamin B9 supports skin cell division and DNA repair.
Red fruits & vegetables
- Red fruits/vegetables (e.g. tomatoes, red bell peppers) contain lycopene, an antioxidant that protects collagen from UV damage (so, that aspect is mostly relevant for skin, but antioxidants are good things to have in all of the body in any case).
Orange-colored vegetables
- Carrots and sweet potatoes are rich in vitamin A, which helps in collagen repair and synthesis.
- Vitamin A is best from food, not supplements, to avoid potential toxicity.
Fruits rich in vitamin C
- Citrus fruits, kiwi, and berries are loaded with vitamin C and antioxidants, essential for collagen synthesis and skin health.
Soy
- Soy products (e.g. tofu, soybeans) contain isoflavones, which reduce inflammation and inhibit enzymes that degrade collagen.
- Soy is associated with lower risks of chronic diseases.
Garlic
- Garlic contains sulfur, taurine, and lipoic acid, important for collagen production and repair.
What to avoid:
- Reduce foods high in advanced glycation end products (AGEs), which damage collagen and promote inflammation.
- AGEs are found in fried, roasted, or grilled fatty proteinous foods (e.g. meat, including synthetic meat, and yes, including grass-fed nicely marketed meat—although processed meat such as bacon and sausages are even worse than steaks etc).
- Switch to cooking methods like boiling or steaming to reduce AGE levels.
- Processed foods, sugary pastries, and red meats contribute to collagen degradation.
General diet tips:
- Incorporate more plant-based, antioxidant-rich foods.
- Opt for slow cooking to reduce AGEs.
- Since sustainability is key, choose foods you enjoy for a collagen-boosting diet that you won’t seem like a chore a month later.
For more on all of this, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
We Are Such Stuff As Fish Are Made Of ← our main feature research review about collagen
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:










