The Real Benefit Of Genetic Testing
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Genetic Testing: Health Benefits & Methods
Genetic testing is an oft-derided American pastime, but there’s a lot more to it than finding out about your ancestry!
Note: because there are relatively few companies offering health-related genetic testing services, and we are talking about the benefits of those services, some of this main feature may seem like an advert.
It’s not; none of those companies are sponsoring us, and if any of them become a sponsor at some point, we’ll make it clear and put it in the clearly-marked sponsor segment.
As ever, our only goal here is to provide science-backed information, to enable you to make your own, well-informed, decisions.
Health genomics & genetic testing
The basic goal of health genomics and genetic testing is to learn:
- What genetic conditions you have
- Clearcut genetic conditions, such as Fragile X syndrome, or Huntington’s disease
- What genetic predispositions you have
- Such as an increased/decreased risk for various kinds of cancer, diabetes, heart conditions, and so forth
- What genetic traits you have
- These may range from “blue eyes” to “superathlete muscle type”
- More specifically, pharmacogenomic information
- For example, “fast caffeine metabolizer” or “clopidogrel (Plavix) non-responder” (i.e., that drug simply will not work for you)
Wait, what’s the difference between health genomics and genetic testing?
- Health genomics is the science of how our genes affect our health.
- Genetic testing can be broadly defined as the means of finding out which genes we have.
A quick snippet…
More specifically, a lot of these services look at which single nucleotide polymorphisms (SNPs, pronounced “snips”) we have. While we share almost all of our DNA with each other (and indeed, with most vertebrates), our polymorphisms are the bits that differ, and are the bits that, genetically speaking, make us different.
So, by looking just at the SNPs, it means we “only” need to look at about 3,000,000 DNA positions, and not our entire genome. For perspective, those 3,000,000 DNA positions make up about 0.1% of our whole genome, so without focusing on SNPs, the task would be 1000x harder.
For example, the kind of information that this sort of testing may give you, includes (to look at some “popular” SNPs):
- rs53576 in the oxytocin receptor influences social behavior and personality
- rs7412 and rs429358 can raise the risk of Alzheimer’s disease by more than 10x
- rs6152 can influence baldness
- rs333 resistance to HIV
- rs1800497 in a dopamine receptor may influence the sense of pleasure
- rs1805007 determines red hair and sensitivity to anesthetics
- rs9939609 triggers obesity and type-2 diabetes
- rs662799 prevents weight gain from high fat diets
- rs12255372 linked to type-2 diabetes and breast cancer
- rs1799971 makes alcohol cravings stronger
- rs17822931 determines earwax, sweating and body odor
- rs1333049 coronary heart disease
- rs1051730 and rs3750344 nicotine dependence
- rs4988235 lactose intolerance
(You can learn about these and more than 100,000 other SNPs at SNPedia.com)
I don’t know what SNPs I have, and am disinclined to look them up one by one!
The first step to knowing, is to get your DNA out of your body and into a genetic testing service. This is usually done by saliva or blood sample. This writer got hers done many years ago by 23andMe and was very happy with that service, but there are plenty of other options.
Healthline did an independent review of the most popular companies, so you might like to check out:
Healthline: Best DNA Testing Kits of 2023
Those companies will give you some basic information, such as “6x higher breast cancer risk” or “3x lower age-related macular degeneration risk” etc.
However, to really get bang-for-buck, what you want to do next is:
- Get your raw genetic data (the companies above should provide it); this will probably look like a big text file full of As, Cs, Gs, and Ts, but it make take another form.
- Upload it to Promethease. When this writer got hers done , the cost was $2; that price has now gone up to a whopping $12.
- You will then get a report that will cross-reference your data with everything known about SNPs, and give a supremely comprehensive, readable-to-the-human-eye, explanation of what it all means for you—from much more specific health risk prognostics, to more trivial things like whether you can roll your tongue or smell decomposed asparagus metabolites in urine.
A note on privacy: anything you upload to Promethease will be anonymized, and/but in doing so, you consent to it going into the grand scientific open-source bank of “things we know about the human genome”, and thus contribute to the overall sample size of genetic data.
In our opinion, it means you’re doing your bit for science, without personal risk. But your opinion may differ, and that’s your decision to make.
Lastly, on the pros and cons of pharmacogenetic testing specifically:
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Link Between Introversion & Sensory Processing
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve talked before about how to beat loneliness and isolation, and how that’s important for all of us, including those of us on the less social end of the scale.
However, while we all need at least the option of social contact in order to be at our best, there’s a large portion of the population who also need to be able to retreat to somewhere quiet to recover from too much social goings-on.
Clinically speaking, this sometimes gets called introversion, or at least a negative score for extroversion on the “Big Five Inventory”, the only personality-typing system that actually gets used in science. Today we’re going to be focusing on a term that typically gets applied to those generally considered introverts:
The “highly sensitive person”
This makes it sound like a very rare snowflake condition, when in fact the diagnostic criteria yield a population bell curve of 30:40:30, whereupon 30% are in the band of “high sensitivity”, 40% “normal sensitivity” and the remaining 30% “low sensitivity”.
You may note that “high” and “low” together outnumber “normal”, but statistics is like that. It is interesting to note, though, that this statistical spread renders it not a disorder, so much as simply a description.
You can read more about it here:
Sensory-processing sensitivity and its relation to introversion and emotionality
What it means in practical terms
Such a person will generally seek solitude more frequently during the day than others will, and it’s not because of misanthropy (at least, statistically speaking it’s not; can’t speak for individuals!), but rather, it’s about needing downtime after what has felt like too much sensory processing resulting:
If this need for solitude is not met (sometimes it’s simply not practicable), then it can lead to overwhelm.
Sidenote about overwhelm: pick your battles! No, pick fewer than that. Put some back. That’s still too many 😜
Back to seriousness: if you’re the sort of person to walk into a room and immediately do the Sherlock Holmes thing of noticing everything about everyone, who is doing what, what has changed about the room since last time you were there, etc… Then that’s great; it’s a sign of a sharp mind, but it’s also a lot of information to process and you’re probably going to need a little decompression afterwards:
This is the biological equivalent of needing to let an overworked computer or phone cool down after excessive high-intensity use of its CPU.
The same goes if you’re the sort of person who goes into “performance mode” when in company, is “the life and soul of the party” etc, and/or perhaps “the elegant hostess”, but needs to then collapse afterwards because it’s more of a role you play than your natural inclination.
Take care of your battery
To continue the technological metaphor from earlier, if you repeatedly overuse a device without allowing it cooldown periods, it will break down (and if it’s a certain generation of iPhone, it might explode).
Similarly, if you repeatedly overuse your own highly sensitive senses (such as being often in social environment where there’s a lot going on) without allowing yourself adequate cooldown periods, you will break down (or indeed, explode: not literally, but some people are prone to emotional outbursts after bottling things up).
None of this is good for the health, not in the short term and not in the long term, either:
With that in mind, take care to take care of yourself, meeting your actual needs instead of just those that get socially assumed.
Want to take the test?
Here’s a two-minute test (results available immediately right there on-screen; no need to give your email or anything) 😎
Want to know more?
We reviewed this book about playing to one’s strengths in the context of sensitivity, a while back, and highly recommend it:
Sensitive – by Jenn Granneman and Andre Sólo
Enjoy!
Share This Post
-
Daily, Weekly, Monthly: Habits Against Aging
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Anil Rajani has advice on restoring/retaining youthfulness. Two out of three of the sections are on skincare specifically, which may seem a vanity, but it’s also worth remembering that our skin is a very large and significant organ, and makes a big difference for the rest of our physical health, as well as our mental health. So, it’s worthwhile to look after it:
The recommendations
Daily: meditation practice
Meditation reduces stress, which reduction in turn protects telomere length, slowing the overall aging process in every living cell of the body.
Weekly: skincare basics
Dr. Rajani recommends a combination of retinol and glycolic acid. The former to accelerate cell turnover, stimulate collagen production, and reduce wrinkles; the latter, to exfoliate dead cells, allowing the retinol to do its job more effectively.
We at 10almonds would like to add: wearing sunscreen with SPF50 is a very good thing to do on any day that your phone’s weather app says the UV index is “moderate” or higher.
Monthly: skincare extras
Here are the real luxuries; spa visits, microneedling (stimulates collagen production), and non-ablative laser therapy. He recommends creating a home spa if possible for monthly skincare treatments, investing in high-quality devices for long-term benefits.
For more on all of these things, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
- Age & Aging: What Can (And Can’t) We Do About It?
- No-Frills, Evidence-Based Mindfulness
- The Evidence-Based Skincare That Beats Product-Specific Hype
Take care!
Share This Post
-
‘Emergency’ or Not, Covid Is Still Killing People. Here’s What Doctors Advise to Stay Safe.
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
With around 20,000 people dying of covid in the United States since the start of October, and tens of thousands more abroad, the covid pandemic clearly isn’t over. However, the crisis response is, since the World Health Organization and the Biden administration ended their declared health emergencies last year.
Let’s not confuse the terms “pandemic” and “emergency.” As Abraar Karan, an infectious disease physician and researcher at Stanford University, said, “The pandemic is over until you are scrunched in bed, feeling terrible.”
Pandemics are defined by neither time nor severity, but rather by large numbers of ongoing infections worldwide. Emergencies are acute and declared to trigger an urgent response. Ending the official emergency shifted the responsibility for curbing covid from leaders to the public. In the United States, it meant, for example, that the government largely stopped covering the cost of covid tests and vaccines.
But the virus is still infecting people; indeed, it is surging right now.
With changes in the nature of the pandemic and the response, KFF Health News spoke with doctors and researchers about how to best handle covid, influenza, and other respiratory ailments spreading this season.
A holiday wave of sickness has ensued as expected. Covid infections have escalated nationwide in the past few weeks, with analyses of virus traces in wastewater suggesting infection rates as high as last year’s. More than 73,000 people died of covid in the U.S. in 2023, meaning the virus remains deadlier than car accidents and influenza. Still, compared with last year’s seasonal surge, this winter’s wave of covid hospitalizations has been lower and death rates less than half.
“We’re seeing outbreaks in homeless shelters and in nursing homes, but hospitals aren’t overwhelmed like they have been in the past,” said Salvador Sandoval, a doctor and health officer at the Merced County public health department in California. He attributes that welcome fact to vaccination, covid treatments like Paxlovid, and a degree of immunity from prior infections.
While a new coronavirus variant, JN.1, has spread around the world, the current vaccines and covid tests remain effective.
Other seasonal illnesses are surging, too, but rates are consistent with those of previous years. Between 9,400 and 28,000 people died from influenza from Oct. 1 to Jan. 6, estimates the Centers for Disease Control and Prevention, and millions felt so ill from the flu that they sought medical care. Cases of pneumonia — a serious condition marked by inflamed lungs that can be triggered by the flu, covid, or other infections — also predictably rose as winter set in. Researchers are now less concerned about flare-ups of pneumonia in China, Denmark, and France in November and December, because they fit cyclical patterns of the pneumonia-causing bacteria Mycoplasma pneumoniae rather than outbreaks of a dangerous new bug.
Public health researchers recommend following the CDC guidance on getting the latest covid and influenza vaccines to ward off hospitalization and death from the diseases and reduce chances of getting sick. A recent review of studies that included 614,000 people found that those who received two covid vaccines were also less likely to develop long covid; often involving fatigue, cognitive dysfunction, and joint pain, the condition is marked by the development or continuation of symptoms a few months after an infection and has been debilitating for millions of people. Another analysis found that people who had three doses of covid vaccines were much less likely to have long covid than those who were unvaccinated. (A caveat, however, is that those with three doses might have taken additional measures to avoid infections than those who chose to go without.)
It’s not too late for an influenza vaccine, either, said Helen Chu, a doctor and epidemiologist at the University of Washington in Seattle. Influenza continues to rise into the new year, especially in Southern states and California. Last season’s shot appeared to reduce adults’ risk of visits to the emergency room and urgent care by almost half and hospitalization by more than a third. Meanwhile, another seasonal illness with a fresh set of vaccines released last year, respiratory syncytial virus, appears to be waning this month.
Another powerful way to prevent covid, influenza, common colds, and other airborne infections is by wearing an N95 mask. Many researchers say they’ve returned to socializing without one but opt for the masks in crowded, indoor places when wearing one would not be particularly burdensome. Karan, for example, wears his favorite N95 masks on airplanes. And don’t forget good, old-fashioned hand-washing, which helps prevent infections as well.
If you do all that and still feel sick? Researchers say they reach for rapid covid tests. While they’ve never been perfect, they’re often quite helpful in guiding a person’s next steps.
When President Joe Biden declared the end of the public health emergency last year, many federally funded testing sites that sent samples to laboratories shut their doors. As a result, people now mainly turn to home covid tests that signal an infection within 15 minutes and cost around $6 to $8 each at many pharmacies. The trick is to use these tests correctly by taking more than one when there’s reason for concern. They miss early infections more often than tests processed in a lab, because higher levels of the coronavirus are required for detection — and the virus takes time to multiply in the body. For this reason, Karan considers other information. “If I ran into someone who turned out to be sick, and then I get symptoms a few days later,” he said, “the chance is high that I have whatever they had, even if a test is negative.”
A negative result with a rapid test might mean simply that an infection hasn’t progressed enough to be detected, that the test had expired, or that it was conducted wrong. To be sure the culprit behind symptoms like a sore throat isn’t covid, researchers suggest testing again in a day or two. It often takes about three days after symptoms start for a test to register as positive, said Karan, adding that such time estimates are based on averages and that individuals may deviate from the norm.
If a person feels healthy and wants to know their status because they were around someone with covid, Karan recommends testing two to four days after the exposure. To protect others during those uncertain days, the person can wear an N95 mask that blocks the spread of the virus. If tests remain negative five days after an exposure and the person still feels fine, Chu said, they’re unlikely to be infected — and, if they are, viral levels would be so low that they would be unlikely to pass the disease to others.
Positive tests, on the other hand, reliably flag an infection. In this case, people can ask a doctor whether they qualify for the antiviral drug Paxlovid. The pills work best when taken immediately after symptoms begin so that they slash levels of the virus before it damages the body. Some studies suggest the medicine reduces a person’s risk of long covid, too, but the evidence is mixed. Another note on tests: Don’t worry if they continue to turn out positive for longer than symptoms last; the virus may linger even if it’s no longer replicating. After roughly a week since a positive test or symptoms, studies suggest, a person is unlikely to pass the virus to others.
If covid is ruled out, Karan recommends tests for influenza because they can guide doctors on whether to prescribe an antiviral to fight it — or if instead it’s a bacterial infection, in which case antibiotics may be in order. (One new home test diagnoses covid and influenza at the same time.) Whereas antivirals and antibiotics target the source of the ailment, over-the-counter medications may soothe congestion, coughs, fevers, and other symptoms. That said, the FDA recently determined that a main ingredient in versions of Sudafed, NyQuil, and other decongestants, called phenylephrine, is ineffective.
Jobs complicate a personal approach to staying healthy. Emergency-era business closures have ended, and mandates on vaccination and wearing masks have receded across the country. Some managers take precautions to protect their staff. Chu, for example, keeps air-purifying devices around her lab, and she asks researchers to stay home when they feel sick and to test themselves for covid before returning to work after a trip.
However, occupational safety experts note that many employees face risks they cannot control because decisions on if and how to protect against outbreaks, such as through ventilation, testing, and masking, are left to employers. Notably, people with low-wage and part-time jobs — occupations disproportionately held by people of color — are often least able to control their workplace environments.
Jessica Martinez, co-executive director of the National Council for Occupational Safety and Health, said the lack of national occupational standards around airborne disease protection represents a fatal flaw in the Biden administration’s decision to relinquish its control of the pandemic.
“Every workplace needs to have a plan for reducing the threat of infectious disease,” she said. “If you only focus on the individual, you fail workers.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Share This Post
Related Posts
-
Addiction Myths That Are Hard To Quit
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Which Addiction-Quitting Methods Work Best?
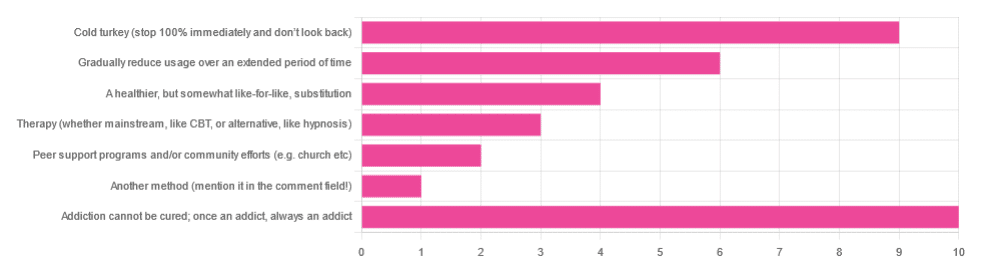
In Tuesday’s newsletter we asked you what, in your opinion, is the best way to cure an addiction. We got the above-depicted, below-described, interesting distribution of responses:
- About 29% said: “Addiction cannot be cured; once an addict, always an addict”
- About 26% said “Cold turkey (stop 100% and don’t look back)”
- About 17% said “Gradually reduce usage over an extended period of time”
- About 11% said “A healthier, but somewhat like-for-like, substitution”
- About 9% said “Therapy (whether mainstream, like CBT, or alternative, like hypnosis)”
- About 6% said “Peer support programs and/or community efforts (e.g. church etc)”
- About 3% said “Another method (mention it in the comment field)” and then did not mention it in the comment field
So what does the science say?
Addiction cannot be cured; once an addict, always an addict: True or False?
False, which some of the people who voted for it seemed to know, as some went on to add in the comment field what they thought was the best way to overcome the addiction.
The widespread belief that “once an addict, always an addict” is a “popular truism” in the same sense as “once a cheater, always a cheater”. It’s an observation of behavioral probability phrased as a strong generalization, but it’s not actually any kind of special unbreakable law of the universe.
And, certainly the notion that one cannot be cured keeps membership in many 12-step programs and similar going—because if you’re never cured, then you need to stick around.
However…
❝What is the definition of addiction?
Addiction is a treatable, chronic medical disease involving complex interactions among brain circuits, genetics, the environment, and an individual’s life experiences. People with addiction use substances or engage in behaviors that become compulsive and often continue despite harmful consequences.
Prevention efforts and treatment approaches for addiction are generally as successful as those for other chronic diseases.❞
~ American Society of Addiction Medicine
Or if we want peer-reviewed source science, rather than appeal to mere authority as above, then:
❝What is drug addiction?
Addiction is defined as a chronic, relapsing disorder characterized by compulsive drug seeking and use despite adverse consequences. It is considered a brain disorder, because it involves functional changes to brain circuits involved in reward, stress, and self-control. Those changes may last a long time after a person has stopped taking drugs.
Addiction is a lot like other diseases, such as heart disease. Both disrupt the normal, healthy functioning of an organ in the body, both have serious harmful effects, and both are, in many cases, preventable and treatable.❞
~ Nora D. Volkow (Director, National Institute of Drug Abuse)
Read more: Drugs, Brains, and Behavior: The Science of Addiction
In short: part of the definition of addiction is the continued use; if the effects of the substance are no longer active in your physiology, and you are no longer using, then you are not addicted.
Just because you would probably become addicted again if you used again does not make you addicted when neither the substance nor its after-effects are remaining in your body. Otherwise, we could define all people as addicted to all things based on “well if they use in the future they will probably become addicted”.
This means: the effects of addiction can and often will last for long after cessation of use, but ultimately, addiction can be treated and cured.
(yes, you should still abstain from the thing to which you were formerly addicted though, or you indeed most probably will become addicted again)
Cold turkey is best: True or False?
True if and only if certain conditions are met, and then only for certain addictions. For all other situations… False.
To decide whether cold turkey is a safe approach (before even considering “effective”), the first thing to check is how dangerous the withdrawal symptoms are. In some cases (e.g. alcohol, cocaine, heroin, and others), the withdrawal symptoms can kill.
That doesn’t mean they will kill, so knowing (or being!) someone who quit this way does not refute this science by counterexample. The mortality rates that we saw while researching varied from 8% to 37%, so most people did not die, but do you really want (yourself or a loved one) to play those odds unnecessarily?
See also: Detoxification and Substance Abuse Treatment
Even in those cases where it is considered completely safe for most people to quit cold turkey, such as smoking, it is only effective when the quitter has appropriate reliable medical support, e.g.
- Without support: 3–5% success rate
- With support: 22% success rate
And yes, that 22% was for the “abrupt cessation” group; the “gradual cessation” group had a success rate of 15.5%. On which note…
Gradual reduction is the best approach: True or False?
False based on the above data, in the case of addictions where abrupt cessation is safe. True in other cases where abrupt cessation is not safe.
Because if you quit abruptly and then die from the withdrawal symptoms, then well, technically you did stay off the substance for the rest of your life, but we can’t really claim that as a success!
A healthier, but somewhat like-for-like substitution is best: True or False?
True where such is possible!
This is why, for example, medical institutions recommend the use of buprenorphine (e.g. Naloxone) in the case of opioid addiction. It’s a partial opioid receptor agonist, meaning it does some of the job of opioids, while being less dangerous:
It’s also why vaping—despite itself being a health hazard—is recommended as a method of quitting smoking:
Similarly, “zero alcohol drinks that seem like alcohol” are a popular way to stop drinking alcohol, alongside other methods:
This is also why it’s recommended that if you have multiple addictions, to quit one thing at a time, unless for example multiple doctors are telling you otherwise for some specific-to-your-situation reason.
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Health Fix – by Dr. Ayan Panja
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The book is divided into three main sections:
- The foundations
- The aspirations
- The fixes
The foundations are an overview of the things you’re going to need to know, about biology, behaviors, and being human.
The aspirations are research-generated common hopes, desires, dreams and goals of patients who have come to Dr. Panja for help.
The fixes are exactly what you’d hope them to be. They’re strategies, tools, hacks, tips, tricks, to get you from where you are now to where you want to be, health-wise.
The book is well-structured, with deep-dives, summaries, and practical advice of how to make sure everything you’re doing works together as part of the big picture that you’re building for your health.
All in all, a fantastic catch-all book, whatever your health goals.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Sun, Sea, And Sudden Killers To Avoid
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Stay Safe From Heat Exhaustion & Heatstroke!
For most of us, summer is upon us now. Which can be lovely… and also bring new, different health risks. Today we’re going to talk about heat exhaustion and heatstroke.
What’s the difference?
Heat exhaustion is a milder form of heatstroke, but the former can turn into the latter very quickly if left untreated.
Symptoms of heat exhaustion include:
- Headache
- Nausea
- Cold sweats
- Light-headedness
Symptoms of heatstroke include the above and also:
- Red/flushed-looking skin
- High body temperature (104ºF / 40ºC)
- Disorientation/confusion
- Accelerated heart rate
Click here for a handy downloadable infographic you can keep on your phone
What should we do about it?
In the case of heatstroke, call 911 or the equivalent emergency number for the country where you are.
Hopefully we can avoid it getting that far, though:
Prevention first
Here are some top tips to avoid heat exhaustion and thus also avoid heatstroke. Many are common sense, but it’s easy to forget things—especially in the moment, on a hot sunny day!
- Hydrate, hydrate, hydrate
- (Non-sugary) iced teas, fruit infusions, that sort of thing are more hydrating than water alone
- Avoid alcohol
- If you really want to imbibe, rehydrate between each alcoholic drink
- Time your exercise with the heat in mind
- In other words, make any exercise session early or late in the day, not during the hottest period
- Use sunscreen
- This isn’t just for skin health (though it is important for that); it will also help keep you cooler, as it blocks the UV rays that literally cook your cells
- Keep your environment cool
- Shade is good, air conditioning / cooling fans can help.
- A wide-brimmed hat is portable shade just for you
- Wear loose, breathable clothing
- We write about health, not fashion, but: light breathable clothes that cover more of your body are generally better healthwise in this context, than minimal clothes that don’t, if you’re in the sun.
- Be aware of any medications you’re taking that will increase your sensitivity to heat.
- This includes medications that are dehydrating, and includes most anti-depressants, many anti-nausea medications, some anti-allergy medications, and more.
- Check your labels/leaflets, look up your meds online, or ask your pharmacist.
Treatment
If prevention fails, treatment is next. Again, in the case of heatstroke, it’s time for an ambulance.
If symptoms are “only” of heat exhaustion and are more mild, then:
- Move to a cooler location
- Rehydrate again
- Remove clothing that’s confining or too thick
- What does confining mean? Clothing that’s tight and may interfere with the body’s ability to lose heat.
- For example, you might want to lose your sports bra, but there is no need to lose a bikini, for instance.
- What does confining mean? Clothing that’s tight and may interfere with the body’s ability to lose heat.
- Use ice packs or towels soaked in cold water, applied to your body, especially wear circulation is easiest to affect, e.g. forehead, wrists, back of neck, under the arms, or groin.
- A cool bath or shower, or a dip in the pool may help cool you down, but only do this if there’s someone else around and you’re not too dizzy.
- This isn’t a good moment to go in the sea, no matter how refreshing it would be. You do not want to avoid heatstroke by drowning instead.
If full recovery doesn’t occur within a couple of hours, seek medical help.
Stay safe and have fun!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: