The Brain Fog Fix – by Dr. Mike Dow
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The three weeks mentioned in the subtitle is in fact a week-by-week plan:
- Adjusting diet (inclusions and exclusions) and cognitive strategies
- Focusing on sleep, exercise, and memory-boosting “brain games”
- Bringing in the social aspect, and connection to something larger than oneself
In this reviewer’s opinion, a week is too short a time to completely overhaul one’s diet; most changes need to be gradual, so doing several at once in a week is quite extreme. But, even if it takes a month for each stage instead of a week, the method is reasonable.
The nutritional advice is good, and consistent with current best science on the topic. There’s a lot about keeping even blood sugars and improving insulin sensitivity, as well as doing what is best for the heart and blood in general (e.g. fiber, managing triglycerides, doing the right kinds of exercise, etc).
As a psychotherapist, he also talks a fair bit about neurotransmitters, and making sure one’s gut and brain are fed appropriately to keep the correct balance (remembering for example that serotonin is made in the gut, and dopamine is made in the brain). Unlike many of his colleagues, he’s not a fan of medicating beyond absolute necessity.
The style is a little salesy for this reviewer’s personal taste—but then again, perhaps he made the reasonable assumption that a person reading a book entitled “the brain fog fix” needs their attention grabbing and re-grabbing every paragraph or so. As such, maybe it’s not a bad call.
Bottom line: if you have brain fog and would like to not have brain fog, this book offers a scientifically sound, evidence-based, holistic approach that can certainly improve things.
Click here to check out The Brain Fog Fix, and fix your brain fog!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
As Nuns Disappear, Many Catholic Hospitals Look More Like Megacorporations
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
ST. LOUIS — Inside the more than 600 Catholic hospitals across the country, not a single nun can be found occupying a chief executive suite, according to the Catholic Health Association.
Nuns founded and led those hospitals in a mission to treat sick and poor people, but some were also shrewd business leaders. Sister Irene Kraus, a former chief executive of Daughters of Charity National Health System, was famous for coining the phrase “no margin, no mission.” It means hospitals must succeed — generating enough revenue to exceed expenses — to fulfill their original mission.
The Catholic Church still governs the care that can be delivered to millions in those hospitals each year, using religious directives to ban abortions and limit contraceptives, in vitro fertilization, and medical aid in dying.
But over time, that focus on margins led the hospitals to transform into behemoths that operate for-profit subsidiaries and pay their executives millions, according to hospital tax filings. These institutions, some of which are for-profit companies, now look more like other megacorporations than like the charities for the destitute of yesteryear.
The absence of nuns in the top roles raises the question, said M. Therese Lysaught, a Catholic moral theologist and professor at Loyola University Chicago: “What does it mean to be a Catholic hospital when the enterprise has been so deeply commodified?”
The St. Louis area serves as the de facto capital of Catholic hospital systems. Three of the largest are headquartered here, along with the Catholic hospital lobbying arm. Catholicism is deeply rooted in the region’s culture. During Pope John Paul II’s only U.S. stop in 1999, he led Mass downtown in a packed stadium of more than 100,000 people.
For a quarter century, Sister Mary Jean Ryan led SSM Health, one of those giant systems centered on St. Louis. Now retired, the 86-year-old said she was one of the last nuns in the nation to lead a Catholic hospital system.
Ryan grew up Catholic in Wisconsin and joined a convent while in nursing school in the 1960s, surprising her family. She admired the nuns she worked alongside and felt they were living out a higher purpose.
“They were very impressive,” she said. “Not that I necessarily liked all of them.”
Indeed, the nuns running hospitals defied the simplistic image often ascribed to them, wrote John Fialka in his book “Sisters: Catholic Nuns and the Making of America.”
“Their contributions to American culture are not small,” he wrote. “Ambitious women who had the skills and the stamina to build and run large institutions found the convent to be the first and, for a long time, the only outlet for their talents.”
This was certainly true for Ryan, who climbed the ranks, working her way from nurse to chief executive of SSM Health, which today has hospitals in Illinois, Missouri, Oklahoma, and Wisconsin.
The system was founded more than a century ago when five German nuns arrived in St. Louis with $5. Smallpox swept through the city and the Sisters of St. Mary walked the streets offering free care to the sick.
Their early foray grew into one of the largest Catholic health systems in the country, with annual revenue exceeding $10 billion, according to its 2023 audited financial report. SSM Health treats patients in 23 hospitals and co-owns a for-profit pharmacy benefit manager, Navitus, that coordinates prescriptions for 14 million people.
But Ryan, like many nuns in leadership roles in recent decades, found herself confronted with an existential crisis. As fewer women became nuns, she had to ensure the system’s future without them.
When Ron Levy, who is Jewish, started at SSM as an administrator, he declined to lead a prayer in a meeting, Ryan recounted in her book, “On Becoming Exceptional.”
“Ron, I’m not asking you to be Catholic,” she recalled telling him. “And I know you’ve only been here two weeks. So, if you’d like to make it three, I suggest you be prepared to pray the next time you’re asked.”
Levy went on to serve SSM for more than 30 years — praying from then on, Ryan wrote.
In Catholic hospitals, meetings are still likely to start with a prayer. Crucifixes often adorn buildings and patient rooms. Mission statements on the walls of SSM facilities remind patients: “We reveal the healing presence of God.”
Above all else, the Catholic faith calls on its hospitals to treat everyone regardless of race, religion, or ability to pay, said Diarmuid Rooney, a vice president of the Catholic Health Association. No nuns run the trade group’s member hospitals, according to the lobbying group. But the mission that compelled the nuns is “what compels us now,” Rooney said. “It’s not just words on a wall.”
The Catholic Health Association urges its hospitals to evaluate themselves every three years on whether they’re living up to Catholic teachings. It created a tool that weighs seven criteria, including how a hospital acts as an extension of the church and cares for poor and marginalized patients.
“We’re not relying on hearsay that the Catholic identity is alive and well in our facilities and hospitals,” Rooney said. “We can actually see on a scale where they are at.”
The association does not share the results with the public.
At SSM Health, “our Catholic identity is deeply and structurally ingrained” even with no nun at the helm, spokesperson Patrick Kampert said. The system reports to two boards. One functions as a typical business board of directors while the other ensures the system abides by the rules of the Catholic Church. The church requires the majority of that nine-member board to be Catholic. Three nuns currently serve on it; one is the chair.
Separately, SSM also is required to file an annual report with the Vatican detailing the ways, Kampert said, “we deepen our Catholic identity and further the healing ministry of Jesus.” SSM declined to provide copies of those reports.
From a business perspective, though, it’s hard to distinguish a Catholic hospital system like SSM from a secular one, said Ruth Hollenbeck, a former Anthem insurance executive who retired in 2018 after negotiating Missouri hospital contracts. In the contracts, she said, the difference amounted to a single paragraph stating that Catholic hospitals wouldn’t do anything contrary to the church’s directives.
To retain tax-exempt status under Internal Revenue Service rules, all nonprofit hospitals must provide a “benefit” to their communities such as free or reduced-price care for patients with low incomes. But the IRS provides a broad definition of what constitutes a community benefit, which gives hospitals wide latitude to justify not needing to pay taxes.
On average, the nation’s nonprofit hospitals reported that 15.5% of their total annual expenses were for community benefits in 2020, the latest figure available from the American Hospital Association.
SSM Health, including all of its subsidiaries, spent proportionately far less than the association’s average for individual hospitals, allocating roughly the same share of its annual expenses to community efforts over three years: 5.1% in 2020, 4.5% in 2021, and 4.9% in 2022, according to a KFF Health News analysis of its most recent publicly available IRS filings and audited financial statements.
A separate analysis from the Lown Institute think tank placed five Catholic systems — including the St. Louis region’s Ascension — on its list of the 10 health systems with the largest “fair share” deficits, which means receiving more in tax breaks than what they spent on the community. And Lown said three St. Louis-area Catholic health systems — Ascension, SSM Health, and Mercy — had fair share deficits of $614 million, $235 million, and $92 million, respectively, in the 2021 fiscal year.
Ascension, Mercy, and SSM disputed Lown’s methodology, arguing it doesn’t take into account the gap between the payments they receive for Medicaid patients and the cost of delivering their care. The IRS filings do.
But, Kampert said, many of the benefits SSM provides aren’t reflected in its IRS filings either. The forms reflect “very simplistic calculations” and do not accurately represent the health system’s true impact on the community, he said.
Today, SSM Health is led by longtime business executive Laura Kaiser. Her compensation in 2022 totaled $8.4 million, including deferred payments, according to its IRS filing. Kampert defended the amount as necessary “to retain and attract the most qualified” candidate.
By contrast, SSM never paid Ryan a salary, giving instead an annual contribution to her convent of less than $2 million a year, according to some tax filings from her long tenure. “I didn’t join the convent to earn money,” Ryan said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
This article first appeared on KFF Health News and is republished here under a Creative Commons license.
Share This Post
-
No-Frills, Evidence-Based Mindfulness
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What’s on your mind, really?
We hear a lot about “the evidence-based benefits of mindfulness”, but what actually are they? And what is the evidence? And, perhaps most importantly: how do we do it?
What are the benefits?
The benefits of mindfulness are many, and include:
- reducing stress
- reducing pain
- improving quality of life
- reducing fatigue
- providing relief from digestive disorders
- reducing symptoms of sleep disorders
- improving immune response
- providing support for caregivers
The evidence is also abundant, and includes:
- Effects of mindfulness exercises as stand-alone intervention on symptoms of anxiety and depression: Systematic review and meta-analysis
- Fusing character strengths and mindfulness interventions: Benefits for satisfaction and performance
- Evidence for the Role of Mindfulness in Cancer: Benefits and Techniques
- Effects of mindfulness-based stress reduction on anxiety symptoms: A systematic review and meta-analysis
- The benefits of meditation and mindfulness practices during times of crisis such as COVID-19
Sounds great… What actually is it, though?
Mindfulness is the state of being attentive to one’s mind. This is at its heart a meditative practice, but that doesn’t necessarily mean you have to be sitting in the lotus position with candles—mindfulness can be built into any daily activity, or even no activity at all.
An exercise you can try right now:
Take a moment to notice everything you can hear. For this writer, that includes:
- The noise of my keystrokes as I type
- The ticking of the clock on the wall
- The gentle humming of my computer’s processor
- The higher-pitched noise of my computer’s monitor
- Birdsong outside
- Traffic further away
- My own breathing
- The sound of my eyelids as I blink
Whatever it is for you, notice how much you can notice that you had previously taken for granted.
You can repeat this exercise with other senses, by the way! For example:
- Notice five things you can see in your immediate environment that you’ve never noticed before. If you’re at home reading this, you probably think you’re very familiar with everything around you, but now see that mark on the wall you’d never noticed before, or a quirk of some electrical wiring, or the stitching on some furnishing, for example.
- Notice the textures of your clothes, or your face, or perhaps an object you’ve never paid attention to touching before. Your fingertips, unless you have some special reason this doesn’t apply to you, are far more sensitive than you probably give them credit for, and can notice the tiniest differentiation in textures, so take a moment to do that now.
- Mindful eating can be an especially healthful practice because it requires that we pay every attention to what we’re putting in our mouth, tasting, chewing, swallowing. No more thoughtlessly downing a box of cookies; every bite is now an experience. On the one hand, you’ll probably eat less at a sitting. On the other hand, what a sensory experience! It really reminds one that life is for living, not just for zipping through at a speed-run pace!
What about mindfulness as a meditative practice?
Well, those are meditative practices! But yes, mindfulness goes for more formal meditation too. For example:
Sit comfortably, with good posture, whatever that means to you. No need to get too caught up in the physical mechanics here—it’d take a whole article. For now, if you’re sitting and comfortable, that’s enough.
Notice your breathing. No need to try to control it—that’s not what this is about today. Just notice it. The in, the out, whether you breathe to your chest or abdomen, through your nose or mouth, don’t worry about doing it “right”, just notice what you are doing. Observe without judgement.
Notice your thoughts—no need to try to stop them. Notice noticing your thoughts, and again, observe without judgement. Notice your feelings; are you angry, hopeful, stressed, serene? There are no wrong answers here, and there’s nothing you should try to “correct”. Just observe. No judgement, only observe. Watch your thoughts, and watch your thoughts go.
Did you forget about your breathing while watching your thoughts? Don’t worry about that either if so, just notice that it happened. If you have any feelings about that, notice them too, and carry on observing.
We go through so much of our lives in “autopilot”, that it can be an amazing experience to sometimes just “be”—and be aware of being.
Share This Post
-
Pistachios vs Walnuts – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing pistachios to walnuts, we picked the pistachios.
Why?
Pistachios have more protein and fiber, while walnuts have more fat (though the fats are famously healthy, the same is true of the fats in pistachios).
In the category of vitamins, pistachios have several times more* of vitamins A, B1, B6, C, and E, while walnuts boast only a little more of vitamin B9. They are approximately equal on other vitamins they both contain.
*actually 25x more vitamin A, but the others are 2x, 3x, 4x more.
When it comes to minerals, things are more even; pistachios have more iron, phosphorus, potassium, and selenium, while walnuts have more copper, magnesium, manganese, and zinc. So this category’s a tie.
So given two clear wins for pistachios, and one tie, it’s evident that pistachios win the day.
However! Do enjoy both of these nuts; we often mention that diversity is good in general, and in this case, it’s especially true because of the different mineral profiles, and also because in terms of the healthy fats that they offer, pistachios offer more monounsaturated fats and walnuts offer more polyunsaturated fats; both are healthy, just different.
They’re about equal on saturated fat, in case you were wondering, as it makes up about 6% of the total fats in both cases.
Want to learn more?
You might like to read:
Why You Should Diversify Your Nuts
Take care!
Share This Post
Related Posts
-
Dr. Kim Foster’s Method For Balancing Hormones Naturally
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Not just sex hormones, but also hormones like cortisol (the stress hormone), and thyroid hormones (for metabolism regulation) too! The body is most of the time self-regulating when it comes to hormones, but there are things that we can do to help our body look after us correctly.
In short, if we give our body what it needs, it will (usually, barring serious illness!) give us what we need.
Dr. Foster recommends…
Foods:
- Healthy fats (especially avocados and nuts)
- Lean proteins (especially poultry, fish, and legumes)
- Fruits & vegetables (especially colorful ones)
- Probiotics (especially fermented foods like sauerkraut, kimchi, etc)
- Magnesium-rich foods (especially dark leafy greens, nuts, and yes, dark chocolate)
Teas:
- Camomile tea (especially beneficial against cortisol overproduction)
- Nettle tea (especially beneficial for estrogen production)
- Peppermint tea (especially beneficial for gut health, thus indirect hormone benefits)
Stress reduction:
- Breathing exercises (especially mindfulness exercises)
- Yoga (especially combining exercise with stretches)
- Spending time in nature (especially green spaces)
Dr. Foster explains more about all of these things, along with more illustrative examples, so if you can, do enjoy her video:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to read more about this topic?
You might like our main feature: What Does “Balance Your Hormones” Even Mean?
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Feminist narratives are being hijacked to market medical tests not backed by evidence
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Corporations have used feminist language to promote their products for decades. In the 1980s, companies co-opted messaging about female autonomy to encourage women’s consumption of unhealthy commodities, such as tobacco and alcohol.
Today, feminist narratives around empowerment and women’s rights are being co-opted to market interventions that are not backed by evidence across many areas of women’s health. This includes by commercial companies, industry, mass media and well-intentioned advocacy groups.
Some of these health technologies, tests and treatments are useful in certain situations and can be very beneficial to some women.
However, promoting them to a large group of asymptomatic healthy women that are unlikely to benefit, or without being transparent about the limitations, runs the risk of causing more harm than good. This includes inappropriate medicalisation, overdiagnosis and overtreatment.
In our analysis published today in the BMJ, we examine this phenomenon in two current examples: the anti-mullerian hormone (AMH) test and breast density notification.
The AMH test
The AMH test is a blood test associated with the number of eggs in a woman’s ovaries and is sometimes referred to as the “egg timer” test.
Although often used in fertility treatment, the AMH test cannot reliably predict the likelihood of pregnancy, timing to pregnancy or specific age of menopause. The American College of Obstetricians and Gynaecologists therefore strongly discourages testing for women not seeking fertility treatment.
The AMH test can’t predict your chance of getting pregnant.
Anastasia Vityukova/UnsplashDespite this, several fertility clinics and online companies market the AMH test to women not even trying to get pregnant. Some use feminist rhetoric promising empowerment, selling the test as a way to gain personalised insights into your fertility. For example, “you deserve to know your reproductive potential”, “be proactive about your fertility” and “knowing your numbers will empower you to make the best decisions when family planning”.
The use of feminist marketing makes these companies appear socially progressive and champions of female health. But they are selling a test that has no proven benefit outside of IVF and cannot inform women about their current or future fertility.
Our recent study found around 30% of women having an AMH test in Australia may be having it for these reasons.
Misleading women to believe that the test can reliably predict fertility can create a false sense of security about delaying pregnancy. It can also create unnecessary anxiety, pressure to freeze eggs, conceive earlier than desired, or start fertility treatment when it may not be needed.
While some companies mention the test’s limitations if you read on, they are glossed over and contradicted by the calls to be proactive and messages of empowerment.
Breast density notification
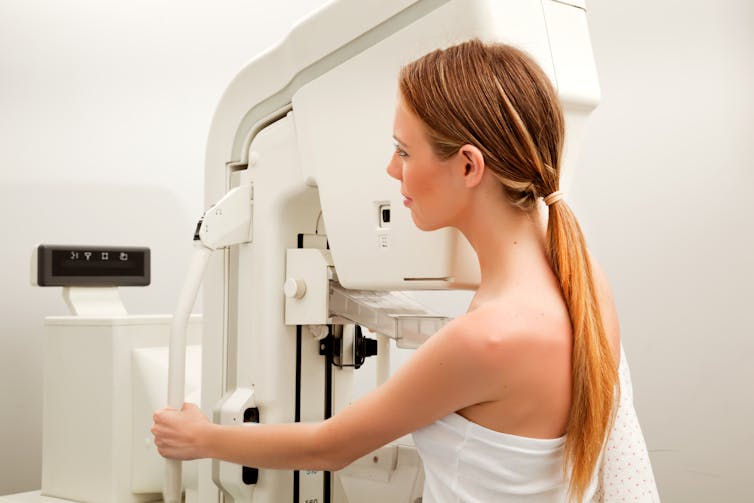
Breast density is one of several independent risk factors for breast cancer. It’s also harder to see cancer on a mammogram image of breasts with high amounts of dense tissue than breasts with a greater proportion of fatty tissue.
While estimates vary, approximately 25–50% of women in the breast screening population have dense breasts.
Dense breasts can make it harder to detect cancer.
Tyler Olsen/ShutterstockStemming from valid concerns about the increased risk of cancer, advocacy efforts have used feminist language around women’s right to know such as “women need to know the truth” and “women can handle the truth” to argue for widespread breast density notification.
However, this simplistic messaging overlooks that this is a complex issue and that more data is still needed on whether the benefits of notifying and providing additional screening or tests to women with dense breasts outweigh the harms.
Additional tests (ultrasound or MRI) are now being recommended for women with dense breasts as they have the ability to detect more cancer. Yet, there is no or little mention of the lack of robust evidence showing that it prevents breast cancer deaths. These extra tests also have out-of-pocket costs and high rates of false-positive results.
Large international advocacy groups are also sponsored by companies that will financially benefit from women being notified.
While stronger patient autonomy is vital, campaigning for breast density notification without stating the limitations or unclear evidence of benefit may go against the empowerment being sought.
Ensuring feminism isn’t hijacked
Increased awareness and advocacy in women’s health are key to overcoming sex inequalities in health care.
But we need to ensure the goals of feminist health advocacy aren’t undermined through commercially driven use of feminist language pushing care that isn’t based on evidence. This includes more transparency about the risks and uncertainties of health technologies, tests and treatments and greater scrutiny of conflicts of interests.
Health professionals and governments must also ensure that easily understood, balanced information based on high quality scientific evidence is available. This will enable women to make more informed decisions about their health.
Brooke Nickel, NHMRC Emerging Leader Research Fellow, University of Sydney and Tessa Copp, NHMRC Emerging Leader Research Fellow, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Almond Butter vs Cashew Butter – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing almond butter to cashew butter, we picked the almond.
Why?
They’re both good! But, our inherent pro-almond bias notwithstanding, the almond butter does have a slightly better spread of nutrients.
In terms of macros, almond butter has more protein while cashew butter has more carbs, and of their fats, they’re broadly healthy in both cases, but almond butter does have less saturated fat.
In the category of vitamins, both are good sources of vitamin E, but almond butter has about 4x more. The rest of the vitamins they both contain aren’t too dissimilar, aside from some different weightings of various different B-vitamins, that pretty much balance out across the two nut butters. The only noteworthy point in cashew butter’s favor here is that it is a good source of vitamin K, which almond butter doesn’t have.
When it comes to minerals, both are good sources of lots of minerals, but most significantly, almond butter has a lot more calcium and quite a bit more potassium. In contrast, cashew butter has more selenium.
In short, they’re both great, but almond butter has more relative points in its favor than cashew butter.
Here are the two we depicted today, by the way, in case you’d like to try them:
Want to learn more?
You might like to read:
Why You Should Diversify Your Nuts
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: