Anti-Inflammatory Diet 101 (What to Eat to Fight Inflammation)
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Chronic inflammation is a cause and/or exacerbating factor in very many diseases. Arthritis, diabetes, and heart disease are probably top of the list, but there are lots more where they came from. And, it’s good to avoid those things. So, how to eat to avoid inflammation?
Let food be thy medicine
The key things to keep in mind, the “guiding principles” are to prioritize whole, minimally-processed foods, and enjoy foods with plenty of antioxidants. Getting a healthy balance of omega fatty acids is also important, which for most people means getting more omega-3 and less omega-6.
Shopping list (foods to prioritize) includes:
- fruits and vegetables in a variety of colors (e.g. berries, leafy greens, beats)
- whole grains, going for the most fiber-rich options (e.g. quinoa, brown rice, oats)
- healthy fats (e.g. avocados, nuts, seeds)
- fatty fish (e.g. salmon, mackerel, sardines) ← don’t worry about this if you’re vegetarian/vegan though, as the previous category can already cover it
- herbs and spices (e.g. turmeric, garlic, ginger)
Noping list (foods to avoid) includes:
- refined carbohydrates
- highly processed and/or fried foods
- red meats and/or processed meats (yes, that does mean that organic grass-fed farmers’ pinky-promise-certified holistically-raised beef is also off the menu)
- dairy products, especially if unfermented
For more information on each of these, plus advice on transitioning away from an inflammatory diet, enjoy:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
How to Prevent (or Reduce) Inflammation
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
CBD Against Diabetes!
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small
❝CBD for diabetes! I’ve taken CBD for body pain. Did no good. Didn’t pay attention as to diabetes. I’m type 1 for 62 years. Any ideas?❞
Thanks for asking! First up, for reference, here’s our previous main feature on the topic of CBD:
CBD Oil: What Does The Science Say?
There, we touched on CBD’s effects re diabetes:
in mice / in vitro / in humans
In summary, according to the above studies, it…
- lowered incidence of diabetes in non-obese diabetic mice. By this they mean that pancreatic function improved (reduced insulitis and reduced inflammatory Th1-associated cytokine production). Obviously this has strong implications for Type 1 Diabetes in humans—but so far, just that, implications (because you are not a mouse).
- attenuated high glucose-induced endothelial cell inflammatory response and barrier disruption. Again, this is promising, but it was an in vitro study in very controlled lab conditions, and sometimes “what happens in the Petri dish, stays in the Petri dish”—in order words, these results may or may not translate to actual living humans.
- Improved insulin response ← is the main take-away that we got from reading through their numerical results, since there was no convenient conclusion given. Superficially, this may be of more interest to those with type 2 diabetes, but then again, if you have T1D and then acquire insulin resistance on top of that, you stand a good chance of dying on account of your exogenous insulin no longer working. In the case of T2D, “the pancreas will provide” (more or less), T1D, not so much.
So, what else is there out there?
The American Diabetes Association does not give a glowing review:
❝There’s a lot of hype surrounding CBD oil and diabetes. There is no noticeable effect on blood glucose (blood sugar) or insulin levels in people with type 2 diabetes. Researchers continue to study the effects of CBD on diabetes in animal studies. ❞
~ American Diabetes Association
Source: ADA | CBD & Diabetes
Of course, that’s type 2, but most research out there is for type 2, or else have been in vitro or rodent studies (and not many of those, at that).
Here’s a relatively more recent study that echoes the results of the previous mouse study we mentioned; it found:
❝CBD-treated non-obese diabetic mice developed T1D later and showed significantly reduced leukocyte activation and increased FCD in the pancreatic microcirculation.
Conclusions: Experimental CBD treatment reduced markers of inflammation in the microcirculation of the pancreas studied by intravital microscopy. ❞
~ Dr. Christian Lehmann et al.
Read more: Experimental cannabidiol treatment reduces early pancreatic inflammation in type 1 diabetes
…and here’s a 2020 study (so, more recent again) that was this time rats, and/but still more promising, insofar as it was with rats that had full-blown T1D already:
Read in full: Two-weeks treatment with cannabidiol improves biophysical and behavioral deficits associated with experimental type-1 diabetes
Finally, a paper in July 2023 (so, since our previous article about CBD), looked at the benefits of CBD against diabetes-related complications (so, applicable to most people with any kind of diabetes), and concluded:
❝CBDis of great value in the treatment of diabetes and its complications. CBD can improve pancreatic islet function, reduce pancreatic inflammation and improve insulin resistance. For diabetic complications, CBD not only has a preventive effect but also has a therapeutic value for existing diabetic complications and improves the function of target organs❞
…before continuing:
❝However, the safety and effectiveness of CBD are still needed to prove. It should be acknowledged that the clinical application of CBD in the treatment of diabetes and its complications has a long way to go.
The dissecting of the pharmacology and therapeutic role of CBD in diabetes would guide the future development of CBD-based therapeutics for treating diabetes and diabetic complications❞
~ Ibid.
Now, the first part of that is standard ass-covering, and the second part of that is standard “please fund more studies please”. Nevertheless, we must also not fail to take heed—little is guaranteed, especially when it comes to an area of research where the science is still very young.
In summary…
It seems well worth a try, and with ostensibly nothing to lose except the financial cost of the CBD.
If you do, you might want to keep careful track of a) your usual diabetes metrics (blood sugar levels before and after meals, insulin taken), and b) when you took CBD, what dose, etc, so you can do some citizen science here.
Lastly: please remember our standard disclaimer; we are not doctors, let alone your doctors, so please do check with your endocrinologist before undertaking any such changes!
Want to read more?
You might like our previous main feature:
How To Prevent And Reverse Type 2 Diabetes ← obviously this will not prevent or reverse Type 1 Diabetes, but avoiding insulin resistance is good in any case!
If you’re not diabetic and you’ve perhaps been confused throughout this article, then firstly thank you for your patience, and secondly you might like this quick primer:
The Sweet Truth About Diabetes: Debunking Diabetes Myths! ← this gives a simplified but fair overview of types 1 & 2
(for space, we didn’t cover the much less common types 3 & 4; perhaps another time we will)
Meanwhile, take care!
Share This Post
-
Long COVID is real—here’s how patients can get treatment and support
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What you need to know
- There is still no single, FDA-approved treatment for long COVID, but doctors can help patients manage individual symptoms.
- Long COVID patients may be eligible for government benefits that can ease financial burdens.
- Getting reinfected with COVID-19 can worsen existing long COVID symptoms, but patients can take steps to stay protected.
On March 15—Long COVID Awareness Day—patients shared their stories and demanded more funding for long COVID research. Nearly one in five U.S. adults who contract COVID-19 suffer from long COVID, and up to 5.8 million children have the disease.
Anyone who contracts COVID-19 is at risk of developing long-term illness. Long COVID has been deemed by some a “mass-disabling event,” as its symptoms can significantly disrupt patients’ lives.
Fortunately, there’s hope. New treatment options are in development, and there are resources available that may ease the physical, mental, and financial burdens that long COVID patients face.
Read on to learn more about resources for long COVID patients and how you can support the long COVID patients in your life.
What is long COVID, and who is at risk?
Long COVID is a cluster of symptoms that can occur after a COVID-19 infection and last for weeks, months, or years, potentially affecting almost every organ. Symptoms range from mild to debilitating and may include fatigue, chest pain, brain fog, dizziness, abdominal pain, joint pain, and changes in taste or smell.
Anyone who gets infected with COVID-19 is at risk of developing long COVID, but some groups are at greater risk, including unvaccinated people, women, people over 40, and people who face health inequities.
What types of support are available for long COVID patients?
Currently, there is still no single, FDA-approved treatment for long COVID, but doctors can help patients manage individual symptoms. Some options for long COVID treatment include therapies to improve lung function and retrain your sense of smell, as well as medications for pain and blood pressure regulation. Staying up to date on COVID-19 vaccines may also improve symptoms and reduce inflammation.
Long COVID patients are eligible for disability benefits under the Americans with Disabilities Act. The Pandemic Legal Assistance Network provides pro bono support for long COVID patients applying for these benefits.
Long COVID patients may also be eligible for other forms of government assistance, such as Supplemental Nutrition Assistance Program (SNAP), Temporary Assistance for Needy Families (TANF), Medicaid, and rental and utility assistance programs.
How can friends and family of long COVID patients provide support?
Getting reinfected with COVID-19 can worsen existing long COVID symptoms. Wearing a high-quality, well-fitting mask will reduce your risk of contracting COVID-19 and spreading it to long COVID patients and others. At indoor gatherings, improving ventilation by opening doors and windows, using high-efficiency particulate air (HEPA) filters, and building your own Corsi-Rosenthal box can also reduce the spread of the COVID-19 virus.
Long COVID patients may also benefit from emotional and financial support as they manage symptoms, navigate barriers to treatment, and go through the months-long process of applying for and receiving disability benefits.
For more information, talk to your health care provider.
This article first appeared on Public Good News and is republished here under a Creative Commons license.
Share This Post
-
Why rating your pain out of 10 is tricky
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
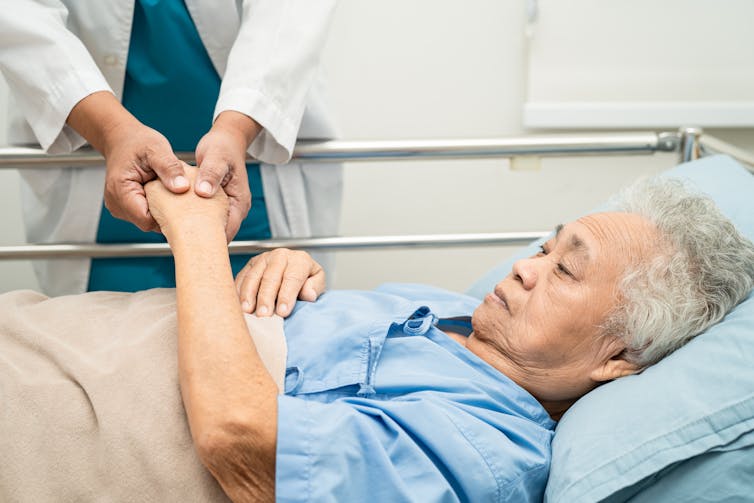
“It’s really sore,” my (Josh’s) five-year-old daughter said, cradling her broken arm in the emergency department.
“But on a scale of zero to ten, how do you rate your pain?” asked the nurse.
My daughter’s tear-streaked face creased with confusion.
“What does ten mean?”
“Ten is the worst pain you can imagine.” She looked even more puzzled.
As both a parent and a pain scientist, I witnessed firsthand how our seemingly simple, well-intentioned pain rating systems can fall flat.
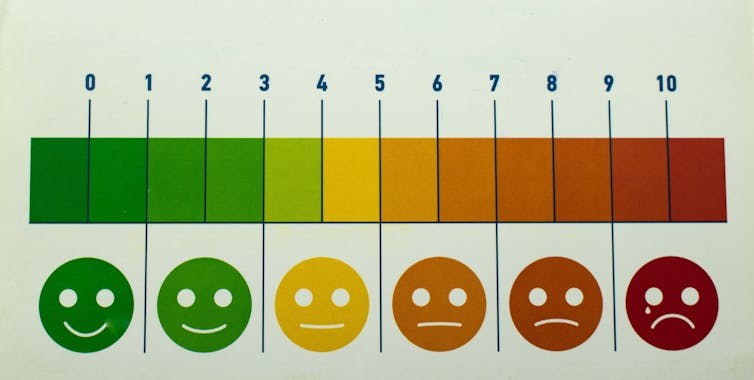
altanaka/Shutterstock What are pain scales for?
The most common scale has been around for 50 years. It asks people to rate their pain from zero (no pain) to ten (typically “the worst pain imaginable”).
This focuses on just one aspect of pain – its intensity – to try and rapidly understand the patient’s whole experience.
How much does it hurt? Is it getting worse? Is treatment making it better?
Rating scales can be useful for tracking pain intensity over time. If pain goes from eight to four, that probably means you’re feeling better – even if someone else’s four is different to yours.
Research suggests a two-point (or 30%) reduction in chronic pain severity usually reflects a change that makes a difference in day-to-day life.
But that common upper anchor in rating scales – “worst pain imaginable” – is a problem.
People usually refer to their previous experiences when rating pain. sasirin pamai/Shutterstock A narrow tool for a complex experience
Consider my daughter’s dilemma. How can anyone imagine the worst possible pain? Does everyone imagine the same thing? Research suggests they don’t. Even kids think very individually about that word “pain”.
People typically – and understandably – anchor their pain ratings to their own life experiences.
This creates dramatic variation. For example, a patient who has never had a serious injury may be more willing to give high ratings than one who has previously had severe burns.
“No pain” can also be problematic. A patient whose pain has receded but who remains uncomfortable may feel stuck: there’s no number on the zero-to-ten scale that can capture their physical experience.
Increasingly, pain scientists recognise a simple number cannot capture the complex, highly individual and multifaceted experience that is pain.
Who we are affects our pain
In reality, pain ratings are influenced by how much pain interferes with a person’s daily activities, how upsetting they find it, their mood, fatigue and how it compares to their usual pain.
Other factors also play a role, including a patient’s age, sex, cultural and language background, literacy and numeracy skills and neurodivergence.
For example, if a clinician and patient speak different languages, there may be extra challenges communicating about pain and care.
Some neurodivergent people may interpret language more literally or process sensory information differently to others. Interpreting what people communicate about pain requires a more individualised approach.
Impossible ratings
Still, we work with the tools available. There is evidence people do use the zero-to-ten pain scale to try and communicate much more than only pain’s “intensity”.
So when a patient says “it’s eleven out of ten”, this “impossible” rating is likely communicating more than severity.
They may be wondering, “Does she believe me? What number will get me help?” A lot of information is crammed into that single number. This patient is most likely saying, “This is serious – please help me.”
In everyday life, we use a range of other communication strategies. We might grimace, groan, move less or differently, use richly descriptive words or metaphors.
Collecting and evaluating this kind of complex and subjective information about pain may not always be feasible, as it is hard to standardise.
As a result, many pain scientists continue to rely heavily on rating scales because they are simple, efficient and have been shown to be reliable and valid in relatively controlled situations.
But clinicians can also use this other, more subjective information to build a fuller picture of the person’s pain.
How can we communicate better about pain?
There are strategies to address language or cultural differences in how people express pain.
Visual scales are one tool. For example, the “Faces Pain Scale-Revised” asks patients to choose a facial expression to communicate their pain. This can be particularly useful for children or people who aren’t comfortable with numeracy and literacy, either at all, or in the language used in the health-care setting.
A vertical “visual analogue scale” asks the person to mark their pain on a vertical line, a bit like imagining “filling up” with pain.
Modified visual scales are sometimes used to try to overcome communication challenges. Nenadmil/Shutterstock What can we do?
Health professionals
Take time to explain the pain scale consistently, remembering that the way you phrase the anchors matters.
Listen for the story behind the number, because the same number means different things to different people.
Use the rating as a launchpad for a more personalised conversation. Consider cultural and individual differences. Ask for descriptive words. Confirm your interpretation with the patient, to make sure you’re both on the same page.
Patients
To better describe pain, use the number scale, but add context.
Try describing the quality of your pain (burning? throbbing? stabbing?) and compare it to previous experiences.
Explain the impact the pain is having on you – both emotionally and how it affects your daily activities.
Parents
Ask the clinician to use a child-suitable pain scale. There are special tools developed for different ages such as the “Faces Pain Scale-Revised”.
Paediatric health professionals are trained to use age-appropriate vocabulary, because children develop their understanding of numbers and pain differently as they grow.
A starting point
In reality, scales will never be perfect measures of pain. Let’s see them as conversation starters to help people communicate about a deeply personal experience.
That’s what my daughter did — she found her own way to describe her pain: “It feels like when I fell off the monkey bars, but in my arm instead of my knee, and it doesn’t get better when I stay still.”
From there, we moved towards effective pain treatment. Sometimes words work better than numbers.
Joshua Pate, Senior Lecturer in Physiotherapy, University of Technology Sydney; Dale J. Langford, Associate Professor of Pain Management Research in Anesthesiology, Weill Cornell Medical College, Cornell University, and Tory Madden, Associate Professor and Pain Researcher, University of Cape Town
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Signs That Are Present When Someone Is Dying
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You’ve probably been there a few times, although given the emotional nature of the thing, it’s likely that you weren’t taking notes. Hospice workers, on the other hand, do take notes, so here are some things you might want to know, and if anything makes the next time even a little easier, that’ll be good:
Last stages
Here are the discussed signs of the “active dying” phase:
- Increasing unconsciousness:
- The person will be mostly unresponsive most of the time.
- Eyes may be open or partially open but not making eye contact.
- Mouth will likely remain open due to muscle relaxation.
- Cessation of food and water intake
- The person will likely not eat or drink for several days.
- This is a natural process and does not cause suffering per se (e.g. thirst, hunger).
- Dryness of mouth, however, can be treated with a little moistening, for comfort.
- Changes in breathing
- Breathing patterns will change and may be irregular.
- This is a natural metabolic response, and is not a sign of distress.
- Terminal secretions (“death rattle”) may occur:
- A gurgling sound caused by saliva buildup due to loss of swallowing reflex.
- Not painful or distressing for the person.
- Can be managed by repositioning or using medication to dry secretions.
- Skin color changes / mottling:
- First appears on fingers and toes (purple or gray discoloration).
- May spread to knees, nose, or other extremities.
- Temperature fluctuations:
- The body loses its ability to regulate temperature.
- Person may feel hot but be cold (or vice versa).
- Fevers are common—cooling measures and/or Tylenol can help.
A person in discomfort may appear restless, have a furrowed brow, or show physical agitation. If on the other hand they appear peaceful and unresponsive, they are almost certainly not in distress. At such times, it’s best to focus on just keeping them clean and comfortable.
For more on all of these, see:
Click Here If The Embedded Video Doesn’t Load Automatically!
Want to learn more?
You might also like to read:
Managing Mortality: When Planning Is a Matter of Life and Death
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
- Increasing unconsciousness:
-
Simple Wall Pilates for Seniors – by Grace Clark
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
While the cover illustration makes this look a little too simple, in fact there’s a lot of value in this book, with exercises ranging from things like that on the cover, to the “wall downward dog”. But the actual exercises (of which there are 29) themselves are only a part of the book (taking about 70 pages of it with clear illustrations).
There’s also a lot about important Pilates principles to apply, such as breathing, correct body alignment (if you don’t already do Pilates, you will not have this, as Pilates alignment is quite specific), flexibility, balance, stability, coordination, range of motion, isometric exercise considerations, endurance, and more.
Unlike a lot of “…for seniors” books, this is not a watered down barely-does-anything version of the “real” exercises, but rather, would present most the same challenges to a 20-year-old reader; it’s just that the focus here is more on matters that tend to concern an older rather than younger demographic. That 20-something may be busy building their butt, for instance, while the 80-year-old is building their bones. No reason both shouldn’t do both, of course, but the focus is age-specific.
The author guides us through working up from easy things to hard, breaking stuff down so that we can progress at our own pace, such that even the most cautious or enthusiastic reader can start at an appropriate point and proceed accordingly.
She also talks us through a 28-day program (as promised by the subtitle), and advice on how to keep it going without plateauing, how to set realistic goals, how to tailor it to our abilities as we go, track our progress, and so forth.
The style is clear and instructional, and one thing that sets this apart from a lot of Pilates books is that the education comes from an angle not of “trust me”, but rather from well-sourced claims with bibliography whose list spans 5 pages at the end.
Bottom line: if you’d like to progressively increase your strength, stability, and more—with no gym equipment, just a wall—then this book will have you see improvements in the 28 days it promises, and thereafter.
Click here to check out Simple Wall Pilates For Seniors, and experience the difference!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Coffee & Your Gut
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Coffee, in moderation, is generally considered a healthful drink—speaking for the drink itself, at least! Because the same cannot be said for added sugar, various sorts of creamers, or iced caramelatte mocha frappucino dessert-style drinks:
The Bitter Truth About Coffee (or is it?)
Caffeine, too, broadly has more pros than cons (again, in moderation):
Caffeine: Cognitive Enhancer Or Brain-Wrecker?
Some people will be concerned about coffee and the heart. Assuming you don’t have a caffeine sensitivity (or you do but you drink decaf), it is heart-neutral in moderation, though there are some ways of preparing it that are better than others:
Make Your Coffee Heart-Healthier!
So, what about coffee and the gut?
The bacteria who enjoy a good coffee
Amongst our trillions of tiny friends, allies, associates, and enemies-on-the-inside, which ones like coffee, and what kind of coffee do they prefer?
A big (n=35,214) international multicohort analysis examined the associations between coffee consumption and very many different gut microbial species, and found:
115 species were positively associated with coffee consumption, mostly of the kind considered “friendly”, including ones often included in probiotic supplements, such as various Bifidobacterium and Lactobacillus species.
The kind that was most strongly associated with coffee consumption, however, was Lawsonibacter asaccharolyticus, a helpful little beast who converts chlorogenic acid (one of the main polyphenols in coffee) into caffeic acid, quinic acid, and various other metabolites that we can use.
More specifically: moderate coffee-drinkers, defined as drinking 1–3 cups per day, enjoyed a 300–400% increase in L. asaccharolyticus, while high coffee-drinkers (no, not that kind of high), defined as drinking 4 or more cups of coffee per day, enjoyed a 400–800% increase, compared to “never/rarely” coffee-drinkers (defined as drinking 2 or fewer cups per month).
Click here to see more data from the study, in a helpful infographic
Things that did not affect the outcome:
- The coffee-making method—it seems the bacteria are not fussy in this regard, as espresso or brewed, and even instant, yielded the same gut microbiome benefits
- The caffeine content—as both caffeinated and decaffeinated yielded the same gut microbiome benefits
You can read the paper itself in full for here:
Want to enjoy coffee, but not keen on the effects of caffeine or the taste of decaffeinated?
Taking l-theanine alongside coffee flattens the curve of caffeine metabolism, and means one can get the benefits without unwanted jitteriness:
Enjoy!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: