Young Forever – by Dr. Mark Hyman
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A lot of work on the topic of aging looks at dealing with symptoms of aging, rather than the causes. And, that’s worthy too! Those symptoms often do need addressing. But this book is about treating the causes.
Dr. Hyman outlines:
- How and why we age
- The root causes of aging
- The ten hallmarks of aging
From there, we go on to learn about the foundations of longevity, and balancing our seven core biological systems:
- Nutrition, digestion, and the microbiome
- Immune and inflammatory system
- Cellular energy
- Biotransformation and elimination/detoxification*
- Hormones, neurotransmitters, and other signalling molecules
- Circulation and lymphatic flow
- Structural health, from muscle and bones to cells and tissues
*This isn’t about celery juice fasts and the like; this talking about the work your kidneys, liver, and other organs do
The book goes on to detail how, precisely, with practical actionable advices, to optimize and take care of each of those systems.
All in all: if you want a great foundational understanding of aging and how to slow it to increase your healthy lifespan, this is a very respectable option.
Click here to get your copy of “Young Forever” from Amazon today!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Best Form Of Sugar During Exercise
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small 😎
❝What is the best form of sugar for an energy kick during exercise? Both type of sugar eg glicoae fructose dextrose etc and medium, ie drink, gel, solids etc❞
Great question! Let’s be clear first that we’re going to answer this specifically for the context of during exercise.
Because, if you’re not actively exercising strenuously right at the time when you’re taking the various things we’re going to be talking about, the results will not be the same.
For scenarios that are anything less than “I am exercising right now and my muscles (not joints, or anything else) are feeling the burn”, then instead please see this:
Snacks & Hacks: Eating For Energy (In Ways That Actually Work)
Because, to answer your question, we’re going to be going 100% against the first piece of advice in that article, which was “Skip the quasi-injectables”, i.e., anything marketed as very quick release. Those things are useful for diabetics to have handy just in case of needing to urgently correct a hypo, but for most people most of the time, they’re not. See also:
Which Sugars Are Healthier, And Which Are Just The Same?
However…
When strenuously exercising in a way that is taxing our muscles, we do not have to worry about the usual problem of messing up our glucose metabolism by overloading our body with sugars faster than it can use it (thus: it has to hurriedly convert glucose and shove it anywhere it’ll fit to put it away, which is very bad for us), because right now, in the exercise scenario we’re describing, the body is already running its fastest metabolism and is grabbing glucose anywhere it can find it.
Which brings us to our first key: the best type of sugar for this purpose is glucose. Because:
- glucose: the body can use immediately and easily convert whatever’s spare to glycogen (a polysaccharide of glucose) for storage
- fructose: the body cannot use immediately and any conversion of fructose to glycogen has to happen in the liver, so if you take too much fructose (without anything to slow it down, such as the fiber in whole fruit), you’re not only not going to get usable energy (the sugar is just going to be there in your bloodstream, circulating, not getting used, because it doesn’t trigger insulin release and insulin is the gatekeeper that allows sugar to be used), but also, it’s going to tax the liver, which if done to excess, is how we get non-alcoholic fatty liver disease.
- sucrose: is just a disaccharide of glucose and fructose, so it first gets broken down into those, and then its constituent parts get processed as above. Other disaccharides you’ll see mentioned sometimes are maltose and lactose, but again, they’re just an extra step removed from useful metabolism, so to save space, we’ll leave it at that for those today.
- dextrose: is just glucose, but when the labeller is feeling fancy. It’s technically informational because it specifies what isomer of glucose it is, but basically all glucose found in food is d-glucose, i.e. dextrose. Other isomers of glucose can be synthesized (very expensively) in laboratories or potentially found in obscure places (the universe is vast and weird), but in short: unless someone’s going to extreme lengths to get something else, all glucose we encounter is dextrose, and all (absolutely all) dextrose is glucose.
We’d like to show scientific papers contesting these head-to-head for empirical proof, but since the above is basic chemistry and physiology, all we could find is papers taking this for granted and stating in their initial premise that sports drinks, gels, bars usually contain glucose as their main sugar, potentially with some fructose and sucrose. Like this one:
A Comprehensive Study on Sports and Energy Drinks
As for how to take it, again this is the complete opposite of our usual health advice of “don’t drink your calories”, because in this case, for once…
(and again, we must emphasize: only while actively doing strenuous exercise that is making specifically your muscles burn, not your joints or anything else; if your joints are burning you need to rest and definitely don’t spike your blood sugars because that will worsen inflammation)
…just this once, we do want those sugars to be zipping straight into the blood. Which means: liquid is best for this purpose.
And when we say liquid: gel is the same as a drink, so far as the body is concerned, provided the body in question is adequately hydrated (i.e., you are also drinking water).
Here are a pair of studies (by the same team, with the same general methodology), testing things head-to-head, with endurance cyclists on 6-hour stationary cycle rides:
CHO Oxidation from a CHO Gel Compared with a Drink during Exercise
Meanwhile, liquid beat solid, but only significantly so from the 90-minute mark onwards, and even that significant difference was modest (i.e. it’s clinically significant, it’s a statistically reliable result and improbable as random happenstance, but the actual size of the difference was not huge):
Oxidation of Solid versus Liquid CHO Sources during Exercise
We would hypothesize that the reason that liquids only barely outperformed solids for this task is precisely because the solids in question were also designed for the task. When a company makes a fast-release energy bar, they don’t load it with fiber to slow it down. Which differentiates this greatly from, say, getting one’s sugars from whole fruit.
If the study had compared apples to apple juice, we hypothesize the results would have been very different. But alas, if that study has been done, we couldn’t find it.
Today has been all about what’s best during exercise, so let’s quickly finish with a note on what’s best before and after:
Before: What To Eat, Take, And Do Before A Workout
After: Overdone It? How To Speed Up Recovery After Exercise
Take care!
Share This Post
-
An RSV vaccine has been approved for people over 60. But what about young children?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
The Therapeutic Goods Administration (TGA) has approved a vaccine against respiratory syncytial virus (RSV) in Australia for the first time. The shot, called Arexvy and manufactured by GSK, will be available by prescription to adults over 60.
RSV is a contagious respiratory virus which causes an illness similar to influenza, most notably in babies and older adults.
So while it will be good to have an RSV vaccine available for older people, where is protection up to for the youngest children?
A bit about RSV
RSV was discovered in chimpanzees with respiratory illness in 1956, and was soon found to be a common cause of illness in humans.
There are two key groups of people we would like to protect from RSV: babies (up to about one year old) and people older than 60.
Babies tend to fill up hospitals during the RSV season in late spring and winter in large numbers, but severe infection requiring admission to intensive care is less common.
In babies and younger children, RSV generally causes a wheezing asthma-like illness (bronchiolitis), but can also cause pneumonia and croup.
Although there are far fewer hospital admissions among older people, they can develop severe disease and die from an infection.
Babies account for the majority of hospitalisations with RSV.
Prostock-studio/ShutterstockRSV vaccines for older people
For older adults, there are actually several RSV vaccines in the pipeline. The recent Australian TGA approval of Arexvy is likely to be the first of several, with other vaccines from Pfizer and Moderna currently in development.
The GSK and Pfizer RSV vaccines are similar. They both contain a small component of the virus, called the pre-fusion protein, that the immune system can recognise.
Both vaccines have been shown to reduce illness from RSV by more than 80% in the first season after vaccination.
In older adults, side effects following Arexvy appear to be similar to other vaccines, with a sore arm and generalised aches and fatigue frequently reported.
Unlike influenza vaccines which are given each year, it is anticipated the RSV vaccine would be a one-off dose, at least at this stage.
Protecting young children from RSV
Younger babies don’t tend to respond well to some vaccines due to their immature immune system. To prevent other diseases, this can be overcome by giving multiple vaccine doses over time. But the highest risk group for RSV are those in the first few months of life.
To protect this youngest age group from the virus, there are two potential strategies available instead of vaccinating the child directly.
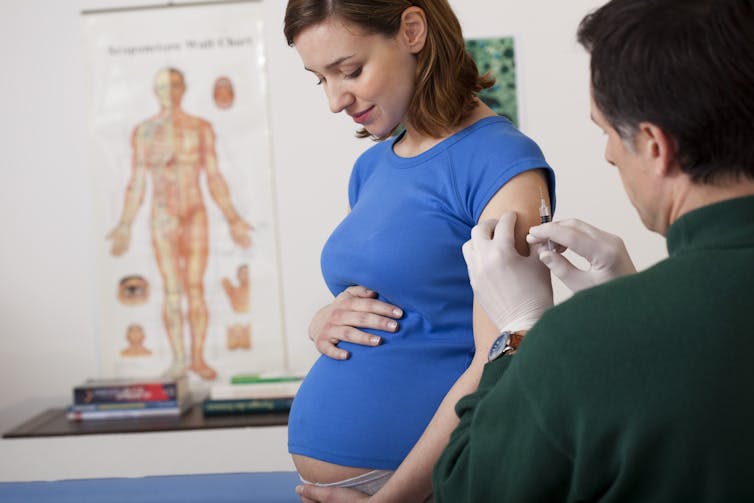
The first is to give a vaccine to the mother and rely on the protective antibodies passing to the infant through the placenta. This is similar to how we protect babies by vaccinating pregnant women against influenza and pertussis (whooping cough).
The second is to give antibodies directly to the baby as an injection. With both these strategies, the protection provided is only temporary as antibodies wane over time, but this is sufficient to protect infants through their highest risk period.
Women could be vaccinated during pregnancy to protect their baby in its first months of life.
Image Point Fr/ShutterstockAbrysvo, the Pfizer RSV vaccine, has been trialled in pregnant women. In clinical trials, this vaccine has been shown to reduce illness in infants for up to six months. It has been approved in pregnant women in the United States, but is not yet approved in Australia.
An antibody product called palivizumab has been available for many years, but is only partially effective and extremely expensive, so has only been given to a small number of children at very high risk.
A newer antibody product, nirsevimab, has been shown to be effective in reducing infections and hospitalisations in infants. It was approved by the TGA in November, but it isn’t yet clear how this would be accessed in Australia.
What now?
RSV, like influenza, is a major cause of respiratory illness, and the development of effective vaccines represents a major advance.
While the approval of the first vaccine for older people is an important step, many details are yet to be made available, including the cost and the timing of availability. GSK has indicated its vaccine should be available soon. While the vaccine will initially only be available on private prescription (with the costs paid by the consumer), GSK has applied for it to be made free under the National Immunisation Program.
In the near future, we expect to hear further news about the other vaccines and antibodies to protect those at higher risk from RSV disease, including young children.
Allen Cheng, Professor of Infectious Diseases, Monash University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Lettuce vs Arugula – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing lettuce to arugula, we picked the arugula.
Why?
These two salad leaves that often fulfil quite similar culinary roles (base of a green salad) are actually of different families, and it shows…
In terms of macros, arugula is lower in carbs, and much higher in protein and fiber—to the point that the protein content in arugula is almost equal to the carb content, which for leaves, is not that common a thing to see.
When it comes to vitamins, things are more even: lettuce has more of vitamins A, B1, B3, B6, and K, while arugula has more of vitamins B5, B9, C, E, and choline. All in all, we can comfortably call it a tie on the vitamin front.
In the category of minerals, things are once again more decided: arugula has more calcium, copper, iron, magnesium, manganese, phosphorus, potassium, and zinc. In contrast, lettuce boasts only more selenium. An easy win for arugula.
Both of these plants have plenty of health-giving phytochemicals, including flavonoids and carotenoids along with other less talked-about things, and while the profiles are quite different for each of them, they stack up about the same in terms of overall benefits in this category.
Taking the various categories into account, this of course adds up to an easy win for arugula, but do enjoy both, especially as lettuce brings benefits that arugula doesn’t in the two categories where they tied!
Want to learn more?
You might like to read:
- How To Avoid Age-Related Macular Degeneration
- Brain Food? The Eyes Have It!
- Spinach vs Kale – Which is Healthier?
Take care!
Share This Post
Related Posts
-
I’m iron deficient. Which supplements will work best for me and how should I take them?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Iron deficiency is common and can be debilitating. It mainly affects women. One in three premenopausal women are low in iron compared to just 5% of Australian men. Iron deficiency particularly affects teenage girls, women who do a lot of exercise and those who are pregnant.
The body needs iron to make new red blood cells, and to support energy production, the immune system and cognitive function. If you’re low, you may experience a range of symptoms including fatigue, weakness, shortness of breath, headache, irregular heartbeat and reduced concentration.
If a blood test shows you’re iron deficient, your doctor may recommend you start taking an oral iron supplement. But should you take a tablet or a liquid? With food or not? And when is the best time of day?
Here are some tips to help you work out how, when and what iron supplement to take.
LittlePigPower/Shutterstock How do I pick the right iron supplement?
The iron in your body is called “elemental iron”. Choosing the right oral supplement and dose will depend on how much elemental iron it has – your doctor will advise exactly how much you need.
The sweet spot is between 60-120 mg of elemental iron. Any less and the supplement won’t be effective in topping up your iron levels. Any higher and you risk gastrointestinal symptoms such as diarrhoea, cramping and stomach pain.
Low iron can especially affect people during pregnancy and women who do a lot of sport. Kamil Macniak/Shutterstock In Australia, iron salts are the most common oral supplements because they are cheap, effective and come in different delivery methods (tablets, capsules, liquid formulas). The iron salts you are most likely to find in your local chemist are ferrous sulfate (~20% elemental iron), ferrous gluconate (~12%) and ferrous fumarate (~33%).
These formulations all work similarly, so your choice should come down to dose and cost.
Many multivitamins may look like an iron supplement, but it’s important to note they usually have too little iron – usually less than 20 mg – to correct an iron deficiency.
Should I take tablets or liquid formulas?
Iron contained within a tablet is just as well absorbed as iron found in a liquid supplement. Choosing the right one usually comes down to personal preference.
The main difference is that liquid formulas tend to contain less iron than tablets. That means you might need to take more of the product to get the right dose, so using a liquid supplement could work out to be more expensive in the long term.
What should I eat with my iron supplement?
Research has shown you will absorb more of the iron in your supplement if you take it on an empty stomach. But this can cause more gastrointestinal issues, so might not be practical for everyone.
If you do take your supplement with meals, it’s important to think about what types of food will boost – rather than limit – iron absorption. For example, taking the supplement alongside vitamin C improves your body’s ability to absorb it.
Some supplements already contain vitamin C. Otherwise you could take the supplement along with a glass of orange juice, or other vitamin C-rich foods.
Taking your supplement alongside foods rich in vitamin C, like orange juice or kiwifruit, can help your body absorb the iron. Anete Lusina/Pexels On the other hand, tea, coffee and calcium all decrease the body’s ability to absorb iron. So you should try to limit these close to the time you take your supplement.
Should I take my supplement in the morning or evening?
The best time of day to take your supplement is in the morning. The body can absorb significantly more iron earlier in the day, when concentrations of hepcidin (the main hormone that regulates iron) are at their lowest.
Exercise also affects the hormone that regulates iron. That means taking your iron supplement after exercising can limit your ability to absorb it. Taking your supplement in the hours following exercise will mean significantly poorer absorption, especially if you take it between two and five hours after you stop.
Our research has shown if you exercise every day, the best time to take your supplement is in the morning before training, or immediately after (within 30 minutes).
My supplements are upsetting my stomach. What should I do?
If you experience gastrointestinal side effects such as diarrhoea or cramps when you take iron supplements, you may want to consider taking your supplement every second day, rather than daily.
Taking a supplement every day is still the fastest way to restore your iron levels. But a recent study has shown taking the same total dose can be just as effective when it’s taken on alternate days. For example, taking a supplement every day for three months works as well as every second day for six months. This results in fewer side effects.
Oral iron supplements can be a cheap and easy way to correct an iron deficiency. But ensuring you are taking the right product, under the right conditions, is crucial for their success.
It’s also important to check your iron levels prior to commencing iron supplementation and do so only under medical advice. In large amounts, iron can be toxic, so you don’t want to be consuming additional iron if your body doesn’t need it.
If you think you may be low on iron, talk to your GP to find out your best options.
Alannah McKay, Postdoctoral Research Fellow, Sports Nutrition, Australian Catholic University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Apples vs Figs – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing apples to figs, we picked the figs.
Why?
These two fruits are both known for being quite rich in sugar (but also rich in fiber, which offsets it metabolically), and indeed their macros are quite similar. That said, figs have slightly more protein, fiber, and carbs. Both are considered low glycemic index foods. We can consider this category a tie, or perhaps a nominal win for apples, whose glycemic index is the lower of the two. But since figs’ GI is also low, it’s really not a deciding factor.
In terms of vitamins, apples have more of vitamins C and E, while figs have more of vitamins A, B1, B2, B3, B5, B6, B9, and choline, with noteworthy margins of difference. A clear for figs here.
When it comes to minerals, apples are not higher in any minerals, while figs are several times higher in calcium, copper, iron, magnesium, manganese, phosphorus, potassium, selenium, and zinc. An overwhelming win for figs.
Of course, enjoy either or both, but if you want nutritional density, apples simply cannot compete with figs.
Want to learn more?
You might like to read:
Which Sugars Are Healthier, And Which Are Just The Same?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Treat Your Own Back – by Robin McKenzie
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
A quick note about the author first: he’s a physiotherapist and not a doctor, but with over 40 years of practice to his name and 33 letters after his name (CNZM OBE FCSP (Hon) FNZSP (Hon) Dip MDT Dip MT), he seems to know his stuff. And certainly, if you visit any physiotherapist, they will probably have some of his books on their own shelves.
This book is intended for the layperson, and as such, explains everything that you need to know, in order to diagnose and treat your back. To this end, he includes assorted tests to perform, a lot of details about various possible back conditions, and then exercises to fix it, i.e. fix whatever you have now learned that the problem is, in your case (if indeed you didn’t know for sure already).
Of course, not everything can be treated by exercises, and he does point to what other things may be necessary in those cases, but for the majority, a significant improvement (if not outright symptom-free status) can be enjoyed by applying the techniques described in this book.
Bottom line: for most people, this book gives you the tools required to do exactly what the title says.
Click here to check out Treat Your Own Back, and treat your own back!
PS: if your issue is not with your back, we recommend you check out his other books in the series (neck, shoulder, hip, knee, ankle) 😎
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: