
Why it’s a bad idea to mix alcohol with some medications
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Anyone who has drunk alcohol will be familiar with how easily it can lower your social inhibitions and let you do things you wouldn’t normally do.
But you may not be aware that mixing certain medicines with alcohol can increase the effects and put you at risk.
When you mix alcohol with medicines, whether prescription or over-the-counter, the medicines can increase the effects of the alcohol or the alcohol can increase the side-effects of the drug. Sometimes it can also result in all new side-effects.
How alcohol and medicines interact
The chemicals in your brain maintain a delicate balance between excitation and inhibition. Too much excitation can lead to convulsions. Too much inhibition and you will experience effects like sedation and depression.
Alcohol works by increasing the amount of inhibition in the brain. You might recognise this as a sense of relaxation and a lowering of social inhibitions when you’ve had a couple of alcoholic drinks.
With even more alcohol, you will notice you can’t coordinate your muscles as well, you might slur your speech, become dizzy, forget things that have happened, and even fall asleep.

Jonathan Kemper/Unsplash
Medications can interact with alcohol to produce different or increased effects. Alcohol can interfere with the way a medicine works in the body, or it can interfere with the way a medicine is absorbed from the stomach. If your medicine has similar side-effects as being drunk, those effects can be compounded.
Not all the side-effects need to be alcohol-like. Mixing alcohol with the ADHD medicine ritalin, for example, can increase the drug’s effect on the heart, increasing your heart rate and the risk of a heart attack.
Combining alcohol with ibuprofen can lead to a higher risk of stomach upsets and stomach bleeds.
Alcohol can increase the break-down of certain medicines, such as opioids, cannabis, seizures, and even ritalin. This can make the medicine less effective. Alcohol can also alter the pathway of how a medicine is broken down, potentially creating toxic chemicals that can cause serious liver complications. This is a particular problem with paracetamol.
At its worst, the consequences of mixing alcohol and medicines can be fatal. Combining a medicine that acts on the brain with alcohol may make driving a car or operating heavy machinery difficult and lead to a serious accident.
Who is at most risk?
The effects of mixing alcohol and medicine are not the same for everyone. Those most at risk of an interaction are older people, women and people with a smaller body size.
Older people do not break down medicines as quickly as younger people, and are often on more than one medication.
Older people also are more sensitive to the effects of medications acting on the brain and will experience more side-effects, such as dizziness and falls.

Alfonso Scarpa/Unsplash
Women and people with smaller body size tend to have a higher blood alcohol concentration when they consume the same amount of alcohol as someone larger. This is because there is less water in their bodies that can mix with the alcohol.
What drugs can’t you mix with alcohol?
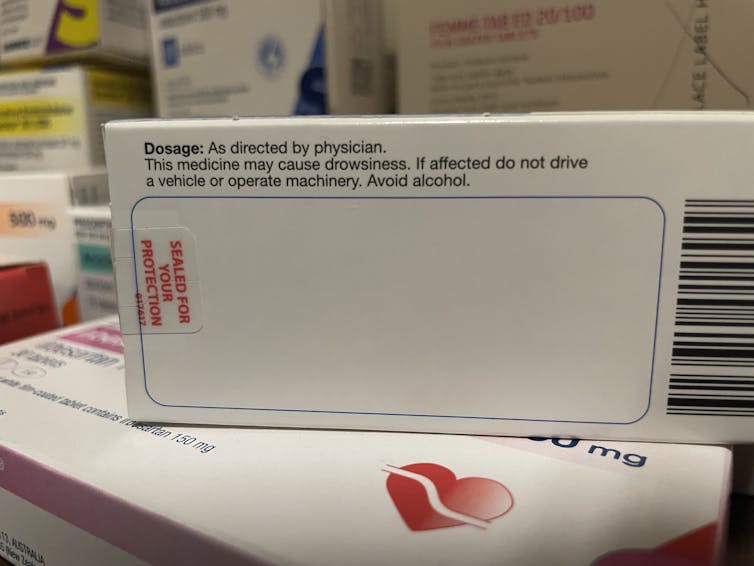
You’ll know if you can’t take alcohol because there will be a prominent warning on the box. Your pharmacist should also counsel you on your medicine when you pick up your script.
The most common alcohol-interacting prescription medicines are benzodiazepines (for anxiety, insomnia, or seizures), opioids for pain, antidepressants, antipsychotics, and some antibiotics, like metronidazole and tinidazole.
Nial Wheate
It’s not just prescription medicines that shouldn’t be mixed with alcohol. Some over-the-counter medicines that you shouldn’t combine with alcohol include medicines for sleeping, travel sickness, cold and flu, allergy, and pain.
Next time you pick up a medicine from your pharmacist or buy one from the local supermarket, check the packaging and ask for advice about whether you can consume alcohol while taking it.
If you do want to drink alcohol while being on medication, discuss it with your doctor or pharmacist first.
Nial Wheate, Associate Professor of the School of Pharmacy, University of Sydney; Jasmine Lee, Pharmacist and PhD Candidate, University of Sydney; Kellie Charles, Associate Professor in Pharmacology, University of Sydney, and Tina Hinton, Associate Professor of Pharmacology, University of Sydney
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
The Diabetes Code – by Dr. Jason Fung
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Cure this serious disease with diet!” is often a bold-claim that overreaches scientific rigor, but in this case, it’s well-established as scientifically valid.
Caveat up-front: the only known circumstance in which this won’t work is if you have comorbidities that prevent you from following the advice.
You may be wondering: is this just the Mediterranean diet again? The answer is that the Mediterreanean diet (or similar) is part of it. But there’s a lot more to this book than that.
Dr. Fung explains to us a lot of the physiology of type 2 diabetes; how insulin resistance occurs, how it becomes a vicious cycle that we get locked into, and how to escape it.
- We learn about the role of fructose, and why fruit is very healthful whereas high-fructose corn syrup and similars are very much not.
- We learn about the role of the liver in glycogen metabolism, and how to un-fatty a fatty liver. Good news: the liver has famously strong self-regenerative abilities, if we give it a break to allow it to do so!
- We learn why portion control doesn’t work, and why intermittent fasting does (here be science).
Dr. Fung’s very readable explanations are free from needless jargon while not dumbing down. The writing style is clear and direct: “this happens this way”, “do this, not that”, etc.
Bottom line: if you have type 2 diabetes and would like to not have that (or if you are pre-diabetic and would like to avoid diabetes) this is a book for you. If you are in great metabolic health and would like to stay that way as you get older, then this is a book for you too.
Click here to check out The Diabetes Code, and get/keep your metabolic health in order!
Share This Post
-
Hate salad or veggies? Just keep eating them. Here’s how our tastebuds adapt to what we eat
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Do you hate salad? It’s OK if you do, there are plenty of foods in the world, and lots of different ways to prepare them.
But given almost all of us don’t eat enough vegetables, even though most of us (81%) know eating more vegetables is a simple way to improve our health, you might want to try.
If this idea makes you miserable, fear not, with time and a little effort you can make friends with salad.
Why don’t I like salads?
It’s an unfortunate quirk of evolution that vegetables are so good for us but they aren’t all immediately tasty to all of us. We have evolved to enjoy the sweet or umami (savoury) taste of higher energy foods, because starvation is a more immediate risk than long-term health.
Vegetables aren’t particularly high energy but they are jam-packed with dietary fibre, vitamins and minerals, and health-promoting compounds called bioactives.
Those bioactives are part of the reason vegetables taste bitter. Plant bioactives, also called phytonutrients, are made by plants to protect themselves against environmental stress and predators. The very things that make plant foods bitter, are the things that make them good for us.
Unfortunately, bitter taste evolved to protect us from poisons, and possibly from over-eating one single plant food. So in a way, plant foods can taste like poison.
For some of us, this bitter sensing is particularly acute, and for others it isn’t so bad. This is partly due to our genes. Humans have at least 25 different receptors that detect bitterness, and we each have our own genetic combinations. So some people really, really taste some bitter compounds while others can barely detect them.
This means we don’t all have the same starting point when it comes to interacting with salads and veggies. So be patient with yourself. But the steps toward learning to like salads and veggies are the same regardless of your starting point.
It takes time
We can train our tastes because our genes and our receptors aren’t the end of the story. Repeat exposures to bitter foods can help us adapt over time. Repeat exposures help our brain learn that bitter vegetables aren’t posions.
And as we change what we eat, the enzymes and other proteins in our saliva change too. This changes how different compounds in food are broken down and detected by our taste buds. How exactly this works isn’t clear, but it’s similar to other behavioural cognitive training.
Add masking ingredients
The good news is we can use lots of great strategies to mask the bitterness of vegetables, and this positively reinforces our taste training.
Salt and fat can reduce the perception of bitterness, so adding seasoning and dressing can help make salads taste better instantly. You are probably thinking, “but don’t we need to reduce our salt and fat intake?” – yes, but you will get more nutritional bang-for-buck by reducing those in discretionary foods like cakes, biscuits, chips and desserts, not by trying to avoid them with your vegetables.
Adding heat with chillies or pepper can also help by acting as a decoy to the bitterness. Adding fruits to salads adds sweetness and juiciness, this can help improve the overall flavour and texture balance, increasing enjoyment.
Pairing foods you are learning to like with foods you already like can also help.
The options for salads are almost endless, if you don’t like the standard garden salad you were raised on, that’s OK, keep experimenting.
Experimenting with texture (for example chopping vegetables smaller or chunkier) can also help in finding your salad loves.
Challenge your biases
Challenging your biases can also help the salad situation. A phenomenon called the “unhealthy-tasty intuition” makes us assume tasty foods aren’t good for us, and that healthy foods will taste bad. Shaking that assumption off can help you enjoy your vegetables more.
When researchers labelled vegetables with taste-focused labels, priming subjects for an enjoyable taste, they were more likely to enjoy them compared to when they were told how healthy they were.
The bottom line
Vegetables are good for us, but we need to be patient and kind with ourselves when we start trying to eat more.
Try working with biology and brain, and not against them.
And hold back from judging yourself or other people if they don’t like the salads you do. We are all on a different point of our taste-training journey.
Emma Beckett, Senior Lecturer (Food Science and Human Nutrition), School of Environmental and Life Sciences, University of Newcastle
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Why do I need to take some medicines with food?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Have you ever been instructed to take your medicine with food and wondered why? Perhaps you’ve wondered if you really need to?
There are varied reasons, and sometimes complex science and chemistry, behind why you may be advised to take a medicine with food.
To complicate matters, some similar medicines need to be taken differently. The antibiotic amoxicillin with clavulanic acid (sold as Amoxil Duo Forte), for example, is recommended to be taken with food, while amoxicillin alone (sold as Amoxil), can be taken with or without food.
Different brands of the same medicine may also have different recommendations when it comes to taking it with food.
Ron Lach/Pexels Food impacts drug absorption
Food can affect how fast and how much a drug is absorbed into the body in up to 40% of medicines taken orally.
When you have food in your stomach, the makeup of the digestive juices change. This includes things like the fluid volume, thickness, pH (which becomes less acidic with food), surface tension, movement and how much salt is in your bile. These changes can impair or enhance drug absorption.
Eating a meal also delays how fast the contents of the stomach move into the small intestine – this is known as gastric emptying. The small intestine has a large surface area and rich blood supply – and this is the primary site of drug absorption.
Eating a meal with medicine will delay its onset. Farhad/Pexels Eating a larger meal, or one with lots of fibre, delays gastric emptying more than a smaller meal. Sometimes, health professionals will advise you to take a medicine with food, to help your body absorb the drug more slowly.
But if a drug can be taken with or without food – such as paracetamol – and you want it to work faster, take it on an empty stomach.
Food can make medicines more tolerable
Have you ever taken a medicine on an empty stomach and felt nauseated soon after? Some medicines can cause stomach upsets.
Metformin, for example, is a drug that reduces blood glucose and treats type 2 diabetes and polycystic ovary syndrome. It commonly causes gastrointestinal symptoms, with one in four users affected. To combat these side effects, it is generally recommended to be taken with food.
The same advice is given for corticosteroids (such as prednisolone/prednisone) and certain antibiotics (such as doxycycline).
Taking some medicines with food makes them more tolerable and improves the chance you’ll take it for the duration it’s prescribed.
Can food make medicines safer?
Ibuprofen is one of the most widely used over-the-counter medicines, with around one in five Australians reporting use within a two-week period.
While effective for pain and inflammation, ibuprofen can impact the stomach by inhibiting protective prostaglandins, increasing the risk of bleeding, ulceration and perforation with long-term use.
But there isn’t enough research to show taking ibuprofen with food reduces this risk.
Prolonged use may also affect kidney function, particularly in those with pre-existing conditions or dehydration.
The Australian Medicines Handbook, which guides prescribers about medicine usage and dosage, advises taking ibuprofen (sold as Nurofen and Advil) with a glass of water – or with a meal if it upsets your stomach.
If it doesn’t upset your stomach, ibuprofen can be taken with water. Tbel Abuseridze/Unsplash A systematic review published in 2015 found food delays the transit of ibuprofen to the small intestine and absorption, which delays therapeutic effect and the time before pain relief. It also found taking short courses of ibuprofen without food reduced the need for additional doses.
To reduce the risk of ibuprofen causing damage to your stomach or kidneys, use the lowest effective dose for the shortest duration, stay hydrated and avoid taking other non-steroidal anti-inflammatory medicines at the same time.
For people who use ibuprofen for prolonged periods and are at higher risk of gastrointestinal side effects (such as people with a history of ulcers or older adults), your prescriber may start you on a proton pump inhibitor, a medicine that reduces stomach acid and protects the stomach lining.
How much food do you need?
When you need to take a medicine with food, how much is enough?
Sometimes a full glass of milk or a couple of crackers may be enough, for medicines such as prednisone/prednisolone.
However, most head-to-head studies that compare the effects of a medicine “with food” and without, usually use a heavy meal to define “with food”. So, a cracker may not be enough, particularly for those with a sensitive stomach. A more substantial meal that includes a mix of fat, protein and carbohydrates is generally advised.
Your health professional can advise you on which of your medicines need to be taken with food and how they interact with your digestive system.
Mary Bushell, Clinical Associate Professor in Pharmacy, University of Canberra
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
Related Posts
-
Is chocolate milk a good recovery drink after a workout? A dietitian reviews the evidence
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Whether you enjoy chocolate milk regularly, as a weekend treat, or as an occasional dose of childhood nostalgia, it probably wouldn’t be the first option you think of for post-workout recovery.
Unless you’re on TikTok, perhaps. According to many people on the social media platform, chocolate milk is not only delicious, but it offers benefits comparable to sports drinks after a workout.
So is there any evidence to support this? Let’s take a look.
eldar nurkovic/Shutterstock Rehydrating after a workout is important
Water accounts for somewhere between 50% and 60% of our body weight. Water has many important functions in the body, including helping to keep our body at the right temperature through sweating.
We lose water naturally from our bodies when we sweat, as well as through our breathing and when we go to the toilet. So it’s important to stay hydrated to replenish the water we lose.
When we don’t, we become dehydrated, which can put a strain on our bodies. Signs and symptoms of dehydration can range from thirst and dizziness to low blood pressure and confusion.
Athletes, because of their higher levels of exertion, lose more water through sweating and from respiration (when their breathing rate gets faster). If they’re training or competing in hot or humid environments they will sweat even more.
Dehydration impacts athletes’ performance and like for all of us, can affect their health.
So finding ways to ensure athletes rehydrate quickly during and after they train or compete is important. Fortunately, sports scientists and dietitians have done research looking at the composition of different fluids to understand which ones rehydrate athletes most effectively.
The beverage hydration index
The best hydrating drinks are those the body retains the most of once they’ve been consumed. By doing studies where they give people different drinks in standardised conditions, scientists have been able to determine how various options stack up.
To this end, they’ve developed something called the beverage hydration index, which measures to what degree different fluids hydrate a person compared to still water.
According to this index beverages with similar fluid retention to still water include sparkling water, sports drinks, cola, diet cola, tea, coffee, and beer below 4% alcohol. That said, alcohol is probably best avoided when recovering from exercise.
Beverages with superior fluid retention to still water include milk (both full-fat and skim), soy milk, orange juice and oral rehydration solutions.
This body of research indicates that when it comes to rehydration after exercise, unflavoured milk (full fat, skim or soy) is better than sports drinks.
But what about chocolate milk?
A small study looked at the effects of chocolate milk compared to plain milk on rehydration and exercise performance in futsal players (futsal is similar to soccer but played on a court indoors). The researchers found no difference in rehydration between the two. There’s no other published research to my knowledge looking at how chocolate milk compares to regular milk for rehydration during or after exercise.
But rehydration isn’t the only thing athletes look for in sports drinks. In the same study, drinking chocolate milk after play (referred to as the recovery period) increased the time it took for the futsal players to become exhausted in further exercise (a shuttle run test) four hours later.
This was also shown in a review of several clinical trials. The analysis found that, compared to different placebos (such as water) or other drinks containing fat, protein and carbohydrates, chocolate milk lengthened the time to exhaustion during exercise.
What’s in chocolate milk?
Milk contains protein, carbohydrates and electrolytes, each of which can affect hydration, performance, or both.
Protein is important for building muscle, which is beneficial for performance. The electrolytes in milk (including sodium and potassium) help to replace electrolytes lost through sweating, so can also be good for performance, and aid hydration.
Compared to regular milk, chocolate milk contains added sugar. This provides extra carbohydrates, which are likewise beneficial for performance. Carbohydrates provide an immediate source of energy for athletes’ working muscles, where they’re stored as glycogen. This might contribute to the edge chocolate milk appears to have over plain milk in terms of athletic endurance.
The added sugar in chocolate milk provides extra carbohydrates. Brent Hofacker/Shutterstock Coffee-flavoured milk has an additional advantage. It contains caffeine, which can improve athletic performance by reducing the perceived effort that goes into exercise.
One study showed that a frappe-type drink prepared with filtered coffee, skim milk and sugar led to better muscle glycogen levels after exercise compared to plain milk with an equivalent amount of sugar added.
So what’s the verdict?
Evidence shows chocolate milk can rehydrate better than water or sports drinks after exercise. But there isn’t evidence to suggest it can rehydrate better than plain milk. Chocolate milk does appear to improve athletic endurance compared to plain milk though.
Ultimately, the best drink for athletes to consume to rehydrate is the one they’re most likely to drink.
While many TikTok trends are not based on evidence, it seems chocolate milk could actually be a good option for recovery from exercise. And it will be cheaper than specialised sports nutrition products. You can buy different brands from the supermarket or make your own at home with a drinking chocolate powder.
This doesn’t mean everyone should look to chocolate milk when they’re feeling thirsty. Chocolate milk does have more calories than plain milk and many other drinks because of the added sugar. For most of us, chocolate milk may be best enjoyed as an occasional treat.
Evangeline Mantzioris, Program Director of Nutrition and Food Sciences, Accredited Practising Dietitian, University of South Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Stretching for 50+ – by Dr. Karl Knopf
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Dr. Knopf explores in this book the two-way relationship between aging and stretching (i.e., each can have a large impact on the other). Thinking about stretching in those terms is an important reframe for going into any stretching program. We’d say “after the age of 50”, but honestly, at any age. But this book is written with over-50s in mind, as the title goes.
There’s an extensive encyclopedic section on stretches per body part, which is exactly as you might expect from any book of this kind. There is also a flexibility self-assessment, so that progress can be measured easily, and so that the reader knows where might need more improvement.
Perhaps this book’s greatest strength is the section on specialized programs based on things ranging from working to improve symptoms of any chronic conditions you may have (or at least working around them, if outright improvement is not possible by stretching), to your recreational activities of importance to you—so, what kinds of flexibilities will be important to you, and also, what kinds of injury you are most likely to need to avoid.
Bottom line: if you’re 50 and would like to do more stretching and less aging, then this book can help with that.
Click here to check out Stretching for 50+, and extend your healthspan!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
If I’m diagnosed with one cancer, am I likely to get another?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Receiving a cancer diagnosis is life-changing and can cause a range of concerns about ongoing health.
Fear of cancer returning is one of the top health concerns. And managing this fear is an important part of cancer treatment.
But how likely is it to get cancer for a second time?
Why can cancer return?
While initial cancer treatment may seem successful, sometimes a few cancer cells remain dormant. Over time, these cancer cells can grow again and may start to cause symptoms.
This is known as cancer recurrence: when a cancer returns after a period of remission. This period could be days, months or even years. The new cancer is the same type as the original cancer, but can sometimes grow in a new location through a process called metastasis.
Actor Hugh Jackman has gone public about his multiple diagnoses of basal cell carcinoma (a type of skin cancer) over the past decade.
The exact reason why cancer returns differs depending on the cancer type and the treatment received. Research is ongoing to identify genes associated with cancers returning. This may eventually allow doctors to tailor treatments for high-risk people.
What are the chances of cancer returning?
The risk of cancer returning differs between cancers, and between sub-types of the same cancer.
New screening and treatment options have seen reductions in recurrence rates for many types of cancer. For example, between 2004 and 2019, the risk of colon cancer recurring dropped by 31-68%. It is important to remember that only someone’s treatment team can assess an individual’s personal risk of cancer returning.
For most types of cancer, the highest risk of cancer returning is within the first three years after entering remission. This is because any leftover cancer cells not killed by treatment are likely to start growing again sooner rather than later. Three years after entering remission, recurrence rates for most cancers decrease, meaning that every day that passes lowers the risk of the cancer returning.
Every day that passes also increases the numbers of new discoveries, and cancer drugs being developed.
What about second, unrelated cancers?
Earlier this year, we learned Sarah Ferguson, Duchess of York, had been diagnosed with malignant melanoma (a type of skin cancer) shortly after being treated for breast cancer.
Although details have not been confirmed, this is likely a new cancer that isn’t a recurrence or metastasis of the first one.
Australian research from Queensland and Tasmania shows adults who have had cancer have around a 6-36% higher risk of developing a second primary cancer compared to the risk of cancer in the general population.
Who’s at risk of another, unrelated cancer?
With improvements in cancer diagnosis and treatment, people diagnosed with cancer are living longer than ever. This means they need to consider their long-term health, including their risk of developing another unrelated cancer.
Reasons for such cancers include different types of cancers sharing the same kind of lifestyle, environmental and genetic risk factors.
The increased risk is also likely partly due to the effects that some cancer treatments and imaging procedures have on the body. However, this increased risk is relatively small when compared with the (sometimes lifesaving) benefits of these treatment and procedures.
While a 6-36% greater chance of getting a second, unrelated cancer may seem large, only around 10-12% of participants developed a second cancer in the Australian studies we mentioned. Both had a median follow-up time of around five years.
Similarly, in a large US study only about one in 12 adult cancer patients developed a second type of cancer in the follow-up period (an average of seven years).
The kind of first cancer you had also affects your risk of a second, unrelated cancer, as well as the type of second cancer you are at risk of. For example, in the two Australian studies we mentioned, the risk of a second cancer was greater for people with an initial diagnosis of head and neck cancer, or a haematological (blood) cancer.
People diagnosed with cancer as a child, adolescent or young adult also have a greater risk of a second, unrelated cancer.
What can I do to lower my risk?
Regular follow-up examinations can give peace of mind, and ensure any subsequent cancer is caught early, when there’s the best chance of successful treatment.
Maintenance therapy may be used to reduce the risk of some types of cancer returning. However, despite ongoing research, there are no specific treatments against cancer recurrence or developing a second, unrelated cancer.
But there are things you can do to help lower your general risk of cancer – not smoking, being physically active, eating well, maintaining a healthy body weight, limiting alcohol intake and being sun safe. These all reduce the chance of cancer returning and getting a second cancer.
Sarah Diepstraten, Senior Research Officer, Blood Cells and Blood Cancer Division, Walter and Eliza Hall Institute and Terry Boyle, Senior Lecturer in Cancer Epidemiology, University of South Australia
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:












