Thinking of trying a new diet? 4 questions to ask yourself before you do
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We live in a society that glorifies dieting, with around 42% of adults globally having tried to lose weight. Messages about dieting and weight loss are amplified on social media, with a never-ending cycle of weight loss fads and diet trends.
Amid often conflicting messages and misinformation, if you’re looking for diet advice online, it’s easy to become confused and overwhelmed.
So before diving into the latest weight loss trend or extreme diet, consider these four questions to help you make a more informed decision.

1. Is the diet realistic?
Have you considered the financial cost of maintaining the diet or lifestyle, and the time and resources that would be required? For example, do you need to purchase specific products, supplements, or follow a rigid meal plan?
If the diet is coming from someone who is trying to sell you something – such as a particular weight-loss product you need in order to follow the diet – this could be a particular red flag.
Many extreme diet recommendations come from a place of privilege and overlook food access, affordability, cooking skills, where you live, or even your culture and ethics.
If the diet has these sorts of issues it can lead to frustration, stress, stigmatisation and feelings of failure for the person trying to adhere to the diet. But the problem may be with the diet itself – not with you.

2. Is there evidence to support this diet?
Self-proclaimed “experts” online will often make claims focused on specific groups, known as target populations. This might be 30- to 50-year-old men with diabetes, for example.
In some cases, evidence for claims made may come from animal studies, which might not be applicable to humans at all.
So be aware that if research findings are for a group that doesn’t match your profile, then the results might not be relevant to you.
It takes time and a lot of high-quality studies to tell us a “diet” is safe and effective, not just one study. Ask yourself, is it supported by multiple studies in humans? Be critical and question the claims before you accept them.
For accurate information look for government websites, or ask your GP or dietitian.
3. How will this diet affect my life?
Food is much more than calories and nutrients. It plays many roles in our lives, and likewise diets can influence our lives in ways we often overlook.
Socially and culturally, food can be a point of connection and celebration. It can be a source of enjoyment, a source of comfort, or even a way to explore new parts of the world.
So when you’re considering a new diet, think about how it might affect meaningful moments for you. For example, if you’re going travelling, will your diet influence the food choices you make? Will you feel that you can’t sample the local cuisine? Or would you be deterred from going out for dinner with friends because of their choice of restaurant?
4. Will this diet make me feel guilty or affect my mental health?
What is your favourite meal? Does this diet “allow” you to eat it? Imagine visiting your mum who has prepared your favourite childhood meal. How will the diet affect your feelings about these special foods? Will it cause you to feel stressed or guilty about enjoying a birthday cake or a meal cooked by a loved one?
Studies have shown that dieting can negatively impact our mental health, and skipping meals can increase symptoms of depression and anxiety.
Many diets fail to consider the psychological aspects of eating, even though our mental health is just as important as physical health. Eating should not make you feel stressed, anxious, or guilty.
So before starting another diet, consider how it might affect your mental health.
Moving away from a dieting mindset
We’re frequently told that weight loss is the path to better health. Whereas, we can prioritise our health without focusing on our weight. Constant messages about the need to lose weight can also be harmful to mental health, and not necessarily helpful for physical health.
Our research has found eating in a way that prioritises health over weight loss is linked to a range of positive outcomes for our health and wellbeing. These include a more positive relationship with food, and less guilt and stress.
Our research also indicates mindful and intuitive eating practices – which focus on internal cues, body trust, and being present and mindful when eating – are related to lower levels of depression and stress, and greater body image and self-compassion.
But like anything, it takes practice and time to build a positive relationship with food. Be kind to yourself, seek out weight-inclusive health-care professionals, and the changes will come. Finally, remember you’re allowed to find joy in food.
Melissa Eaton, Accredited Practising Dietitian; PhD Candidate, University of Wollongong; Verena Vaiciurgis, Accredited Practising Dietitian; PhD Candidate, University of Wollongong, and Yasmine Probst, Associate Professor, School of Medical, Indigenous and Health Sciences, University of Wollongong
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
I lost weight and my period stopped. How are weight and menstruation linked?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
You may have noticed that changes in weight are sometimes accompanied by changes in your period.
But what does one really have to do with the other?
Maintaining a healthy weight is key to regular menstruation. Here’s why – and when to talk to your doctor.
The role of hormones
The menstrual cycle – including when you bleed and ovulate – is regulated by a balance of hormones, particularly oestrogen.
The ovaries are connected to the brain through a hormonal signalling system. This acts as a kind of “chain of command” of hormones controlling the menstrual cycle.
The brain produces a key hormone, called the gonadotropin-releasing hormone, in the hypothalamus. It stimulates the release of other hormones which tell the ovaries to produce oestrogen and release a mature egg (ovulation).
But the release of the gonadotropin-releasing hormone depends on oestrogen levels and how much energy is available to the body. Both of these are closely related to body weight.
Oestrogen is primarily produced in the ovaries, but fat cells also produce oestrogen. This is why weight – and more specifically body fat – can affect menstruation.
Fat cells produce oestrogen, a hormone with a key role in the menstrual cycle. Halfpoint/Shutterstock Can being underweight affect my period?
The body prioritises conserving energy. When reserves are low it stops anything non-essential, such as reproduction.
This can happen when you are underweight, or suddenly lose weight. It can also happen to people who undertake intense exercise or have inadequate nutrition.
The stress sends the hypothalamus into survival mode. As a result, the body lowers its production of the hormones important to ovulation, including oestrogen, and stops menstruation.
Being chronically underweight means not having enough energy available to support reproduction, which can lead to menstrual irregularities including amenorrhea (no periods at all).
This results in very low oestrogen levels and can cause potentially serious health risks, including infertility and bone loss.
Missing periods is not always a cause for concern. But a chronic lack of energy availability can be, if not addressed. The two are linked, meaning understanding your period and being aware of any prolonged changes is important.
How about being overweight?
Higher body fat can elevate oestrogen levels.
When you’re overweight your body stores extra energy in fat cells, which produce oestrogen and other hormones and can cause inflammation in the body. So, if you have a lot of fat cells, your body produces an excess of these hormones. This can affect normal functioning of the uterus lining (endometrium).
Excess oestrogen and inflammation can interfere in the feedback system to the brain and stop ovulation. As a result, you may have irregular or missed periods.
It can also lead to pain (dysmenorrhea) and heavier bleeding (menorrhagia).
Being overweight can sometimes worsen premenstrual syndrome as well. One study found for every 1 kg increase in height (m²) in body mass index (BMI), the risk of premenstrual syndrome went up by 3%. Women with a BMI over 27.5 kg/m² had a much higher risk than those with a BMI under 20 kg/m².
What else might be going on?
Sometimes weight changes are linked to hormonal balances that indicate an underlying condition.
For example, people with polycystic ovary syndrome may gain weight or find it hard to lose weight because they have a hormonal imbalance, including higher levels of testosterone.
The syndrome is also associated with irregular periods and heavy bleeding. So, if you notice these symptoms, it’s a good idea to talk to your doctor.
Similarly, weight changes and irregular periods in midlife might signal the start of perimenopause, the period before menopause (when your periods stop altogether).
Changes in weight and your period could be a sign of menopause approaching. Sabrina Bracher/Shutterstock When should I worry?
Small changes in when your period comes or how long it lasts are usually harmless.
Similarly, slight fluctuations in weight won’t usually have a significant impact on your period – or the changes may be so subtle you don’t notice them.
But regular menstruation is an important marker of female health. Sometimes changes in flow, regularity or the pain you experience can indicate there’s something else going on.
If you notice changes and they don’t feel right to you, speak to a health care provider.
Mia Schaumberg, Associate Professor in Physiology, School of Health, University of the Sunshine Coast and Laura Pernoud, PhD Candidate in Women’s Health, School of Health, University of the Sunshine Coast
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Glycemic Index vs Glycemic Load vs Insulin Index
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
How To Actually Use Those Indices
Carbohydrates are essential for our life, and/but often bring about our early demise. It would be a very conveniently simple world if it were simply a matter of “enjoy in moderation”, but the truth is, it’s not that simple.
To take an extreme example, for the sake of clearest illustration: The person who eats an 80% whole fruit diet (and makes up the necessary protein and fats etc in the other 20%) will probably be healthier than the person who eats a “standard American diet”, despite not practising moderation in their fruit-eating activities. The “standard American diet” has many faults, and one of those faults is how it promotes sporadic insulin spikes leading to metabolic disease.
If your breakfast is a glass of orange juice, this is a supremely “moderate” consumption, but an insulin spike is an insulin spike.
Quick sidenote: if you’re wondering why eating immoderate amounts of fruit is unlikely to cause such spikes, but a single glass of orange juice is, check out:
Which Sugars Are Healthier, And Which Are Just The Same?
Glycemic Index
The first tool in our toolbox here is glycemic index, or GI.
GI measures how much a carb-containing food raises blood glucose levels, also called blood sugar levels, but it’s just glucose that’s actually measured, bearing in mind that more complex carbs will generally get broken down to glucose.
Pure glucose has a GI of 100, and other foods are ranked from 0 to 100 based on how they compare.
Sometimes, what we do to foods changes its GI.
- Some is because it changed form, like the above example of whole fruit (low GI) vs fruit juice (high GI).
- Some is because of more “industrial” refinement processes, such as whole grain wheat (medium GI) vs white flour and white flour products (high GI)
- Some is because of other changes, like starches that were allowed to cool before being reheated (or eaten cold).
Broadly speaking, a daily average GI of 45 is considered great.
But that’s not the whole story…
Glycemic Load
Glycemic Load, or GL, takes the GI and says “ok, but how much of it was there?”, because this is often relevant information.
Refined sugar may have a high GI, but half a teaspoon of sugar in your coffee isn’t going to move your blood sugar levels as much as a glass of Coke, say—the latter simply has more sugar in, and just the same zero fiber.
GL is calculated by (grams of carbs / 100) x GI, by the way.
But it still misses some important things, so now let’s look at…
Insulin Index
Insulin Index, which does not get an abbreviation (probably because of the potentially confusing appearance of “II”), measures the rise in insulin levels, regardless of glucose levels.
This is important, because a lot of insulin response is independent of blood glucose:
- Some is because of other sugars, some some is in response to fats, and yes, even proteins.
- Some is a function of metabolic base rate.
- Some is a stress response.
- Some remains a mystery!
Another reason it’s important is that insulin drives weight gain and metabolic disorders far more than glucose.
Note: the indices of foods are calculated based on average non-diabetic response. If for example you have Type 1 Diabetes, then when you take a certain food, your rise in insulin is going to be whatever insulin you then take, because your body’s insulin response is disrupted by being too busy fighting a civil war in your pancreas.
If your diabetes is type 2, or you are prediabetic, then a lot of different things could happen depending on the stage and state of your diabetes, but the insulin index is still a very good thing to be aware of, because you want to resensitize your body to insulin, which means (barring any urgent actions for immediate management of hyper- or hypoglycemia, obviously) you want to eat foods with a low insulin index where possible.
Great! What foods have a low insulin index?
Many factors affect insulin index, but to speak in general terms:
- Whole plant foods are usually top-tier options
- Lean and/or white meats generally have lower insulin index than red and/or fatty ones
- Unprocessed is generally lower than processed
- The more solid a food is, generally the lower its insulin index compared to a less solid version of the same food (e.g. baked potatoes vs mashed potatoes; cheese vs milk, etc)
But do remember the non-food factors too! This means where possible:
- reducing/managing stress
- getting frequent exercise
- getting good sleep
- practising intermittent fasting
See for example (we promise you it’s relevant):
Fix Chronic Fatigue & Regain Your Energy, By Science
…as are (especially recommendable!) the two links we drop at the bottom of that page; do check them out if you can
Take care!
Share This Post
-
Detox: What’s Real, What’s Not, What’s Useful, What’s Dangerous?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
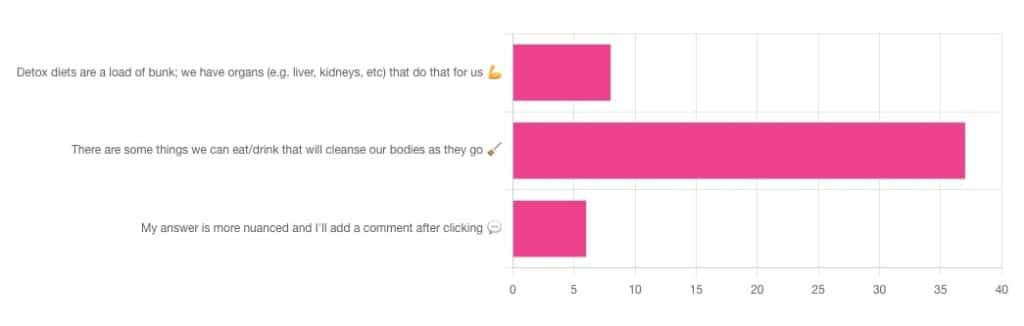
Detox: What’s Real, What’s Not, What’s Useful, What’s Dangerous?
Out of the subscribers who engaged in the poll, it looks like we have a lot of confidence in at least some detox approaches being useful!
Celery juice is most people’s go-to, and indeed it was the only one to get mentioned in the comments added. So let’s take a look at that first…
Celery juice
Celery juice is enjoyed by many people, with many health benefits in mind, including to:
- reduce inflammation
- lower blood pressure
- heal the liver
- fight cancer
- reduce bloating
- support the digestive system
- increase energy
- support weight loss
- promote good mental health
An impressive list! With such an impressive list, we would hope for an impressive weight of evidence, so regular readers might be wondering why those bullet-pointed items aren’t all shiny hyperlinks to studies backing those claims. The reason is…
There aren’t any high-quality studies that back any of those claims.
We found one case study (so, a study with a sample size of one; not amazing) that observed a blood pressure change in an elderly man after drinking celery juice.
Rather than trawl up half of PubMed to show the lacklustre results in a way more befitting of Research Review Monday, though, here’s a nice compact article detailing the litany of disappointment that is science’s observations regards celery juice:
Why Are People Juicing Their Celery? – by Allison Webster, PhD, RD
A key take-away is: juicing destroys the fiber that is celery’s biggest benefit, and its phytochemicals are largely unproven to be of use.
If you enjoy celery, great! It (when not juiced) is a great source of fiber and water. If you juice it, it’s a great source of water.
Activated Charcoal
Unlike a lot of greenery—whose “cleansing” benefits mostly come from fiber and disappear when juiced—activated charcoal has a very different way of operating.
Activated charcoal is negatively charged on a molecular level*, and that—along with its porous nature—traps toxins. It really is a superpowered detox that actually works very well indeed.
But…
It works very well indeed. It will draw out toxins so well, that it’s commonly used to treat poisonings. “Wait”, we hear you say, “why was that a but”?
It doesn’t know what a toxin is. It just draws out all of the things. You took medicine recently? Not any more you didn’t. You didn’t even take that medication orally, you took it some other way? Activated charcoal does not care:
- The effect of activated charcoal on drug exposure following intravenous administration: A meta-analysis
- Activated charcoal for acute overdose: a reappraisal
Does this mean that activated charcoal can be used to “undo” a night of heavy drinking?
Sadly not. That’s one of the few things it just doesn’t work for. It won’t work for alcohol, salts, or metals:
The Use of Activated Charcoal to Treat Intoxications
*Fun chemistry mnemonic about ions:
Cations are pussitive
Anions (by process of elimination) are negative
Onions taste good in salad (remember also: Cole’s Law)
Bottom line on detox foods/drinks:
- Fiber is great; juicing removes fiber. Eat your greens (don’t drink them)!
- Activated charcoal is the heavy artillery of detoxing
- Sometimes it will remove things you didn’t want removed, though
- It also won’t help against alcohol, sadly
Share This Post
Related Posts
-
New research suggests intermittent fasting increases the risk of dying from heart disease. But the evidence is mixed
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Kaitlin Day, RMIT University and Sharayah Carter, RMIT University
Intermittent fasting has gained popularity in recent years as a dietary approach with potential health benefits. So you might have been surprised to see headlines last week suggesting the practice could increase a person’s risk of death from heart disease.
The news stories were based on recent research which found a link between time-restricted eating, a form of intermittent fasting, and an increased risk of death from cardiovascular disease, or heart disease.
So what can we make of these findings? And how do they measure up with what else we know about intermittent fasting and heart disease?
The study in question
The research was presented as a scientific poster at an American Heart Association conference last week. The full study hasn’t yet been published in a peer-reviewed journal.
The researchers used data from the National Health and Nutrition Examination Survey (NHANES), a long-running survey that collects information from a large number of people in the United States.
This type of research, known as observational research, involves analysing large groups of people to identify relationships between lifestyle factors and disease. The study covered a 15-year period.
It showed people who ate their meals within an eight-hour window faced a 91% increased risk of dying from heart disease compared to those spreading their meals over 12 to 16 hours. When we look more closely at the data, it suggests 7.5% of those who ate within eight hours died from heart disease during the study, compared to 3.6% of those who ate across 12 to 16 hours.
We don’t know if the authors controlled for other factors that can influence health, such as body weight, medication use or diet quality. It’s likely some of these questions will be answered once the full details of the study are published.
It’s also worth noting that participants may have eaten during a shorter window for a range of reasons – not necessarily because they were intentionally following a time-restricted diet. For example, they may have had a poor appetite due to illness, which could have also influenced the results.
Other research
Although this research may have a number of limitations, its findings aren’t entirely unique. They align with several other published studies using the NHANES data set.
For example, one study showed eating over a longer period of time reduced the risk of death from heart disease by 64% in people with heart failure.
Another study in people with diabetes showed those who ate more frequently had a lower risk of death from heart disease.
A recent study found an overnight fast shorter than ten hours and longer than 14 hours increased the risk dying from of heart disease. This suggests too short a fast could also be a problem.
But I thought intermittent fasting was healthy?
There are conflicting results about intermittent fasting in the scientific literature, partly due to the different types of intermittent fasting.
There’s time restricted eating, which limits eating to a period of time each day, and which the current study looks at. There are also different patterns of fast and feed days, such as the well-known 5:2 diet, where on fast days people generally consume about 25% of their energy needs, while on feed days there is no restriction on food intake.
Despite these different fasting patterns, systematic reviews of randomised controlled trials (RCTs) consistently demonstrate benefits for intermittent fasting in terms of weight loss and heart disease risk factors (for example, blood pressure and cholesterol levels).
RCTs indicate intermittent fasting yields comparable improvements in these areas to other dietary interventions, such as daily moderate energy restriction.
There are a variety of intermittent fasting diets. Fauxels/Pexels So why do we see such different results?
RCTs directly compare two conditions, such as intermittent fasting versus daily energy restriction, and control for a range of factors that could affect outcomes. So they offer insights into causal relationships we can’t get through observational studies alone.
However, they often focus on specific groups and short-term outcomes. On average, these studies follow participants for around 12 months, leaving long-term effects unknown.
While observational research provides valuable insights into population-level trends over longer periods, it relies on self-reporting and cannot demonstrate cause and effect.
Relying on people to accurately report their own eating habits is tricky, as they may have difficulty remembering what and when they ate. This is a long-standing issue in observational studies and makes relying only on these types of studies to help us understand the relationship between diet and disease challenging.
It’s likely the relationship between eating timing and health is more complex than simply eating more or less regularly. Our bodies are controlled by a group of internal clocks (our circadian rhythm), and when our behaviour doesn’t align with these clocks, such as when we eat at unusual times, our bodies can have trouble managing this.
So, is intermittent fasting safe?
There’s no simple answer to this question. RCTs have shown it appears a safe option for weight loss in the short term.
However, people in the NHANES dataset who eat within a limited period of the day appear to be at higher risk of dying from heart disease. Of course, many other factors could be causing them to eat in this way, and influence the results.
When faced with conflicting data, it’s generally agreed among scientists that RCTs provide a higher level of evidence. There are too many unknowns to accept the conclusions of an epidemiological study like this one without asking questions. Unsurprisingly, it has been subject to criticism.
That said, to gain a better understanding of the long-term safety of intermittent fasting, we need to be able follow up individuals in these RCTs over five or ten years.
In the meantime, if you’re interested in trying intermittent fasting, you should speak to a health professional first.
Kaitlin Day, Lecturer in Human Nutrition, RMIT University and Sharayah Carter, Lecturer Nutrition and Dietetics, RMIT University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What Doctors Feel – by Dr. Danielle Ofri
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This book discusses how feelings such as shame, fear, anger, empathy, and even love influence patient care. Dr. Ofri notes early on:
❝One might reasonably say, I don’t give a damn how my doctor feels as long as she gets me better. In straightforward medical cases, this line of thinking is probably valid. Doctors who are angry, nervous, jealous, burned out, terrified, or ashamed can usually still treat bronchitis or ankle sprains competently.
The problems arise when clinical situations are convoluted, unyielding, or overlaid with unexpected complications, medical errors, or psychological components. This is where factors other than clinical competency come into play.❞
~ Dr. Danielle Ofri
What then follows is very much a no-holds-barred account of the emotional side of medicine.
Not portraying doctors as heroes or martyrs, just as people. Indeed, she even talks about an early, abject failure of hers as a medical student, literally hiding from a patient who badly needed attention and to whom she had been assigned.
We learn not just about the mistakes of doctors, but also the mistakes of patients that lead to mistakes by doctors. For example, emphasizing the severity of your symptom(s) can sometimes be useful to ensure they get attention, but if your regular doctor has heard you rating every symptom always as a 10 every appointment for the past many years, then the end result is that they don’t have information to work from, and will—at best—become frustrated, which will not work out well for you.
Mostly, though, it’s about what goes on behind that calm collected professional exterior that most doctors show most of the time.
The style is a fascinating blend of well-researched science (there’s an extensive bibliography) and very human tales of suffering, compassion, hope, loss, isolation, connection, and more.
Bottom line: if you want to understand your doctor(s), then you want to read this book.
Click here to check out What Doctors Feel, and learn how emotions affect the practice of medicine!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
A short history of sunscreen, from basting like a chook to preventing skin cancer
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Australians have used commercial creams, lotions or gels to manage our skin’s sun exposure for nearly a century.
But why we do it, the preparations themselves, and whether they work, has changed over time.
In this short history of sunscreen in Australia, we look at how we’ve slathered, slopped and spritzed our skin for sometimes surprising reasons.
At first, suncreams helped you ‘tan with ease’
This early sunscreen claimed you could ‘tan with ease’.
Trove/NLASunscreens have been available in Australia since the 30s. Chemist Milton Blake made one of the first.
He used a kerosene heater to cook batches of “sunburn vanishing cream”, scented with French perfume.
His backyard business became H.A. Milton (Hamilton) Laboratories, which still makes sunscreens today.
Hamilton’s first cream claimed you could “
Sunbathe in Comfort and TAN with ease”. According to modern standards, it would have had an SPF (or sun protection factor) of 2.The mirage of ‘safe tanning’
A tan was considered a “modern complexion” and for most of the 20th century, you might put something on your skin to help gain one. That’s when “safe tanning” (without burning) was thought possible.
This 1967 Coppertone advertisement urged you to ‘tan, not burn’.
SenseiAlan/Flickr, CC BY-SASunburn was known to be caused by the UVB component of ultraviolet (UV) light. UVA, however, was thought not to be involved in burning; it was just thought to darken the skin pigment melanin. So, medical authorities advised that by using a sunscreen that filtered out UVB, you could “safely tan” without burning.
But that was wrong.
From the 70s, medical research suggested UVA penetrated damagingly deep into the skin, causing ageing effects such as sunspots and wrinkles. And both UVA and UVB could cause skin cancer.
Sunscreens from the 80s sought to be “broad spectrum” – they filtered both UVB and UVA.
Researchers consequently recommended sunscreens for all skin tones, including for preventing sun damage in people with dark skin.
Delaying burning … or encouraging it?
Up to the 80s, sun preparations ranged from something that claimed to delay burning, to preparations that actively encouraged it to get that desirable tan – think, baby oil or coconut oil. Sun-worshippers even raided the kitchen cabinet, slicking olive oil on their skin.
One manufacturer’s “sun lotion” might effectively filter UVB; another’s merely basted you like a roast chicken.
Since labelling laws before the 80s didn’t require manufacturers to list the ingredients, it was often hard for consumers to tell which was which.
At last, SPF arrives to guide consumers
In the 70s, two Queensland researchers, Gordon Groves and Don Robertson, developed tests for sunscreens – sometimes experimenting on students or colleagues. They printed their ranking in the newspaper, which the public could use to choose a product.
An Australian sunscreen manufacturer then asked the federal health department to regulate the industry. The company wanted standard definitions to market their products, backed up by consistent lab testing methods.
In 1986, after years of consultation with manufacturers, researchers and consumers, Australian Standard AS2604 gave a specified a testing method, based on the Queensland researchers’ work. We also had a way of expressing how well sunscreens worked – the sun protection factor or SPF.
This is the ratio of how long it takes a fair-skinned person to burn using the product compared with how long it takes to burn without it. So a cream that protects the skin sufficiently so it takes 40 minutes to burn instead of 20 minutes has an SPF of 2.
Manufacturers liked SPF because businesses that invested in clever chemistry could distinguish themselves in marketing. Consumers liked SPF because it was easy to understand – the higher the number, the better the protection.
Australians, encouraged from 1981 by the Slip! Slop! Slap! nationwide skin cancer campaign, could now “slop” on a sunscreen knowing the degree of protection it offered.
How about skin cancer?
It wasn’t until 1999 that research proved that using sunscreen prevents skin cancer. Again, we have Queensland to thank, specifically the residents of Nambour. They took part in a trial for nearly five years, carried out by a research team led by Adele Green of the Queensland Institute of Medical Research. Using sunscreen daily over that time reduced rates of squamous cell carcinoma (a common form of skin cancer) by about 60%.
Follow-up studies in 2011 and 2013 showed regular sunscreen use almost halved the rate of melanoma and slowed skin ageing. But there was no impact on rates of basal cell carcinoma, another common skin cancer.
By then, researchers had shown sunscreen stopped sunburn, and stopping sunburn would prevent at least some types of skin cancer.
What’s in sunscreen today?
An effective sunscreen uses one or more active ingredients in a cream, lotion or gel. The active ingredient either works:
-
“chemically” by absorbing UV and converting it to heat. Examples include PABA (para-aminobenzoic acid) and benzyl salicylate, or
-
“physically” by blocking the UV, such as zinc oxide or titanium dioxide.
Physical blockers at first had limited cosmetic appeal because they were opaque pastes. (Think cricketers with zinc smeared on their noses.)
With microfine particle technology from the 90s, sunscreen manufacturers could then use a combination of chemical absorbers and physical blockers to achieve high degrees of sun protection in a cosmetically acceptable formulation.
Where now?
Australians have embraced sunscreen, but they still don’t apply enough or reapply often enough.
Although some people are concerned sunscreen will block the skin’s ability to make vitamin D this is unlikely. That’s because even SPF50 sunscreen doesn’t filter out all UVB.
There’s also concern about the active ingredients in sunscreen getting into the environment and whether their absorption by our bodies is a problem.
Sunscreens have evolved from something that at best offered mild protection to effective, easy-to-use products that stave off the harmful effects of UV. They’ve evolved from something only people with fair skin used to a product for anyone.
Remember, slopping on sunscreen is just one part of sun protection. Don’t forget to also slip (protective clothing), slap (hat), seek (shade) and slide (sunglasses).
Laura Dawes, Research Fellow in Medico-Legal History, Australian National University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-