Lost Connections – by Johann Hari
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Johann Hari had a long journey through (and out of!) depression, and shares his personal findings, including his disappointment with medical options, and a focus on the external factors that lead to depression.
And that’s key to this book—while he acknowledges later in the book that there are physiological factors involved in depression, he wants to look past things we can’t change (like genes accounting for 37% of depression) or things that there may be unwanted side-effects to changing (as in the case of antidepressants, for many people), to things we genuinely can choose.
And no, it’s not a “think yourself happy” book either; rather, it looks at nine key external factorsthat a) influence depression b) can mostly be changed.
If the book has a downside, it’s that the author does tend to extrapolate his own experience a lot more than might be ideal. If SSRIs didn’t help him, they are useless, and also the only kind of antidepressant. If getting into a green space helped him, a Londoner, someone who lives in the countryside will not be depressed in the first place. And so forth. It can also be argued that he cherry-picked data to arrive at some of his pre-decided conclusions. He also misinterprets data sometimes; which is understandable; he is after all a journalist, not a scientist.
Nevertheless, he offers a fresh perspective with a lot of ideas, and whether or not we agree with them all, new ideas tend to be worth reading. And if even one of his nine ideas helps you, that’s a win.
Bottom line: if you’d like to explore the treatment of depression from a direction other than medicalization or psychotherapy, then this is will be a good book for you.
Click here to check out Lost Connections, and reforge yours!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
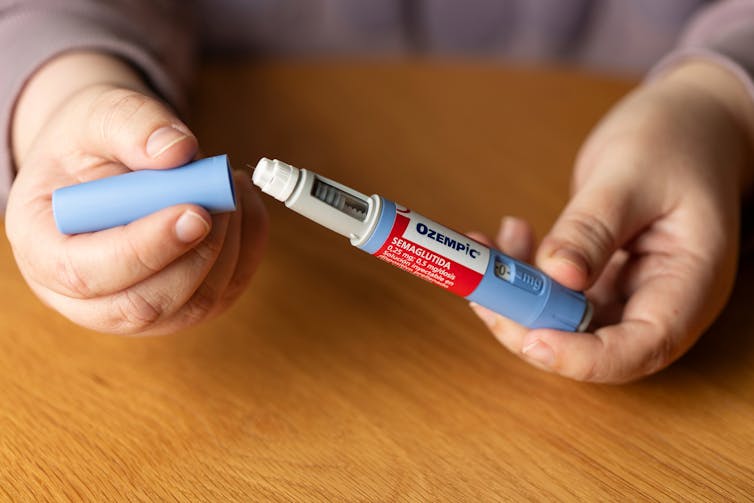
No, taking drugs like Ozempic isn’t ‘cheating’ at weight loss or the ‘easy way out’
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Hundreds of thousands of people worldwide are taking drugs like Ozempic to lose weight. But what do we actually know about them? This month, The Conversation’s experts explore their rise, impact and potential consequences.
Obesity medication that is effective has been a long time coming. Enter semaglutide (sold as Ozempic and Wegovy), which is helping people improve weight-related health, including lowering the risk of a having a heart attack or stroke, while also silencing “food noise”.
As demand for semaglutide increases, so are claims that taking it is “cheating” at weight loss or the “easy way out”.
We don’t tell people who need statin medication to treat high cholesterol or drugs to manage high blood pressure they’re cheating or taking the easy way out.
Nor should we shame people taking semaglutide. It’s a drug used to treat diabetes and obesity which needs to be taken long term and comes with risks and side effects, as well as benefits. When prescribed for obesity, it’s given alongside advice about diet and exercise.
How does it work?
Semaglutide is a glucagon-like peptide-1 receptor agonist (GLP-1RA). This means it makes your body’s own glucagon-like peptide-1 hormone, called GLP-1 for short, work better.
GLP-1 gets secreted by cells in your gut when it detects increased nutrient levels after eating. This stimulates insulin production, which lowers blood sugars.
GLP-1 also slows gastric emptying, which makes you feel full, and reduces hunger and feelings of reward after eating.
GLP-1 receptor agonist (GLP-1RA) medications like Ozempic help the body’s own GLP-1 work better by mimicking and extending its action.
Some studies have found less GLP-1 gets released after meals in adults with obesity or type 2 diabetes mellitus compared to adults with normal glucose tolerance. So having less GLP-1 circulating in your blood means you don’t feel as full after eating and get hungry again sooner compared to people who produce more.
GLP-1 has a very short half-life of about two minutes. So GLP-1RA medications were designed to have a very long half-life of about seven days. That’s why semaglutide is given as a weekly injection.
What can users expect? What does the research say?
Higher doses of semaglutide are prescribed to treat obesity compared to type 2 diabetes management (up to 2.4mg versus 2.0mg weekly).
A large group of randomised controlled trials, called STEP trials, all tested weekly 2.4mg semaglutide injections versus different interventions or placebo drugs.
Trials lasting 1.3–2 years consistently found weekly 2.4 mg semaglutide injections led to 6–12% greater weight loss compared to placebo or alternative interventions. The average weight change depended on how long medication treatment lasted and length of follow-up.
Higher doses of semaglutide are prescribed for obesity than for type 2 diabetes. fcm82/Shutterstock Weight reduction due to semaglutide also leads to a reduction in systolic and diastolic blood pressure of about 4.8 mmHg and 2.5 mmHg respectively, a reduction in triglyceride levels (a type of blood fat) and improved physical function.
Another recent trial in adults with pre-existing heart disease and obesity, but without type 2 diabetes, found adults receiving weekly 2.4mg semaglutide injections had a 20% lower risk of specific cardiovascular events, including having a non-fatal heart attack, a stroke or dying from cardiovascular disease, after three years follow-up.
Who is eligible for semaglutide?
Australia’s regulator, the Therapeutic Goods Administration (TGA), has approved semaglutide, sold as Ozempic, for treating type 2 diabetes.
However, due to shortages, the TGA had advised doctors not to start new Ozempic prescriptions for “off-label use” such as obesity treatment and the Pharmaceutical Benefits Scheme doesn’t currently subsidise off-label use.
The TGA has approved Wegovy to treat obesity but it’s not currently available in Australia.
When it’s available, doctors will be able to prescribe semaglutide to treat obesity in conjunction with lifestyle interventions (including diet, physical activity and psychological support) in adults with obesity (a BMI of 30 or above) or those with a BMI of 27 or above who also have weight-related medical complications.
What else do you need to do during Ozempic treatment?
Checking details of the STEP trial intervention components, it’s clear participants invested a lot of time and effort. In addition to taking medication, people had brief lifestyle counselling sessions with dietitians or other health professionals every four weeks as a minimum in most trials.
Support sessions were designed to help people stick with consuming 2,000 kilojoules (500 calories) less daily compared to their energy needs, and performing 150 minutes of moderate-to-vigorous physical activity, like brisk walking, dancing and gardening each week.
STEP trials varied in other components, with follow-up time periods varying from 68 to 104 weeks. The aim of these trials was to show the effect of adding the medication on top of other lifestyle counselling.
Trial participants also exercised for 150 minutes a week. Elena Nichizhenova/Shutterstock A review of obesity medication trials found people reported they needed less cognitive behaviour training to help them stick with the reduced energy intake. This is one aspect where drug treatment may make adherence a little easier. Not feeling as hungry and having environmental food cues “switched off” may mean less support is required for goal-setting, self-monitoring food intake and avoiding things that trigger eating.
But what are the side effects?
Semaglutide’s side-effects include nausea, diarrhoea, vomiting, constipation, indigestion and abdominal pain.
In one study these led to discontinuation of medication in 6% of people, but interestingly also in 3% of people taking placebos.
More severe side-effects included gallbladder disease, acute pancreatitis, hypoglycaemia, acute kidney disease and injection site reactions.
To reduce risk or severity of side-effects, medication doses are increased very slowly over months. Once the full dose and response are achieved, research indicates you need to take it long term.
Given this long-term commitment, and associated high out-of-pocket cost of medication, when it comes to taking semaglutide to treat obesity, there is no way it can be considered “cheating”.
Read the other articles in The Conversation’s Ozempic series here.
Clare Collins, Laureate Professor in Nutrition and Dietetics, University of Newcastle
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Hardcore Self Help: F**k Anxiety – by Dr. Robert Duff
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We’ve reviewed other anxiety books before, so what makes this one different? Mostly, it’s the style.
Aside from swearing approximately once every two lines (so you might want to skip this one if that would bother you), Dr. Duff’s writing is very down-to-earth in other ways too, making it unpretentiously comfortable and accessible without failing to draw upon the wealth of good-practice, evidence-based advice he has to offer.
To that end, he talks about what anxiety is and isn’t, and goes over various approaches, explaining them in a “about” fashion, and also a “how to” fashion, covering areas such as CBT, somatic therapies, social support, when talk therapy is most likely to help.
The book is a quick read (a modest 74 pages), and it’s refreshing that it hasn’t been padded unnecessarily, unlike a lot of books that could have been a fraction of the size without losing value.
Bottom line: if you (or perhaps someone you care about) would benefit from a straight-to-the-point, no-BS approach to dealing with anxiety (that’s actually evidence-based, not just a “get over it” dismissal), then this is the book for you.
Click here to check out Hardcore Self Help: F**k Anxiety, and indeed do just that!
Share This Post
-
Why We Sleep – by Dr Matthew Walker
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
- We all know sleep is important.
- We all know that without it, we’ll suffer rapid cognitive decline.
- We all know approximately what we’re supposed to do to get good sleep.
So what does this book bring to the table? Mostly, deep understanding (written from the perspective of a career in sleep science) presented in such a way as to be applicable, by you, in your life. Stop sabotaging yourself before you even get out of your bed in the morning!
Hustle culture champions early mornings and late nights, and either or both of those might be difficult to avoid. But to make what you’re doing sustainable, you’re going to have to make some informed decisions about looking after your #1 asset—you!
Dr. Walker writes in a clear and accessible fashion, without skimping on the hard science, and always with practical application in mind. All in all, we can’t recommend this one enough.
Share This Post
Related Posts
-
Lettuce vs Arugula – Which is Healthier?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Our Verdict
When comparing lettuce to arugula, we picked the arugula.
Why?
These two salad leaves that often fulfil quite similar culinary roles (base of a green salad) are actually of different families, and it shows…
In terms of macros, arugula is lower in carbs, and much higher in protein and fiber—to the point that the protein content in arugula is almost equal to the carb content, which for leaves, is not that common a thing to see.
When it comes to vitamins, things are more even: lettuce has more of vitamins A, B1, B3, B6, and K, while arugula has more of vitamins B5, B9, C, E, and choline. All in all, we can comfortably call it a tie on the vitamin front.
In the category of minerals, things are once again more decided: arugula has more calcium, copper, iron, magnesium, manganese, phosphorus, potassium, and zinc. In contrast, lettuce boasts only more selenium. An easy win for arugula.
Both of these plants have plenty of health-giving phytochemicals, including flavonoids and carotenoids along with other less talked-about things, and while the profiles are quite different for each of them, they stack up about the same in terms of overall benefits in this category.
Taking the various categories into account, this of course adds up to an easy win for arugula, but do enjoy both, especially as lettuce brings benefits that arugula doesn’t in the two categories where they tied!
Want to learn more?
You might like to read:
- How To Avoid Age-Related Macular Degeneration
- Brain Food? The Eyes Have It!
- Spinach vs Kale – Which is Healthier?
Take care!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
I Will Make You Passionate About Exercise – by Bevan Eyles
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
What this isn’t: a “just do it!” motivational pep-talk.
What this is:a compassionate and thoughtful approach to help non-exercisers become regular exercisers, by looking at the real life factors of what holds people back (learning from his own early failures as a coach, by paying attention now to things he inadvertently neglected back then), both in the material/practical and in the psychological/emotional.
Further, he gives a 10-step method, for those who would like to be walked through it by the hand, making the transition to exercising regularly (and as a leisure habit, rather than as a chore) as frictionless as possible.
The style is friendly and energetic, and very easy-reading throughout.
Bottom line: if you are someone who finds exercising to be a chore, this book can definitely help you “get from here to there” in terms of finding joy in it, and finding exercise even easier than not exercising. Yes, really.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Rehab Science – by Dr. Tom Walters
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Many books of this kind deal with the injury but not the pain; some source talk about pain but not the injury; this one does both, and more.
Dr. Walters discusses in detail the nature of pain, various different kinds of pain, the factors that influence pain, and, of course, how to overcome pain.
He also takes us on a tour of various different categories of injury, because some require very different treatment than others, and while there are some catch-all “this is good/bad for healing” advices, sometimes what will help with one injury with hinder healing another. So, this information alone would make the book a worthwhile read already.
After this two-part theory-heavy introduction, the largest part of the book is given over to rehab itself, in a practical fashion.
We learn about how to make an appropriate rehab plan, get the material things we need for it (if indeed we need material things), and specific protocols to follow for various different body parts and injuries.
The style is very much that of a textbook, well-formatted and with plenty of illustrations throughout (color is sometimes relevant, so we recommend a print edition over Kindle for this one).
Bottom line: if you have an injury to heal, or even just believe in being prepared, this book is an excellent guide.
Click here to check out Rehab Science, to overcome pain and heal from injury!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: