Every Body Should Know This – by Dr. Federica Amati
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
This book is very much a primer on how to eat healthily. The science is high-quality (the author is the head nutritionist at ZOE) and well-explained, and the advice is reasonable.
Limitations: this book is not very deep, which we might expect from a book with this title. So, if you’ve been a long-time 10almonds reader, you might not learn a lot here, and this book might make a better gift for someone else.
In particular, the book may be well-suited for someone who is thinking of having children soon, as there is an unusual amount of focus on fertility and young motherhood—perhaps because the author herself has young children and so was preoccupied with this when writing. For those of us who are definitely not having any more children, the focus on young motherhood is a little superfluous.
The writing style is very readable pop-science, and nobody who is able to read English is likely to struggle with this one. It’s also quite conversational in parts, as the author discusses her own experiences with implementing the science at hand.
Bottom line: if you want a good, solid, primer of how to eat well for a lifetime of health, especially if you are (or are thinking of becoming) a young mother, then this is a very good book. Otherwise, it’s probably a better to give it as a gift.
Click here to check out Every Body Should Know This, and know the things!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
One in twenty people has no sense of smell – here’s how they might get it back
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
During the pandemic, a lost sense of smell was quickly identified as one of the key symptoms of COVID. Nearly four years later, one in five people in the UK is living with a decreased or distorted sense of smell, and one in twenty have anosmia – the total loss of the ability to perceive any odours at all. Smell training is one of the few treatment options for recovering a lost sense of smell – but can we make it more effective?
Smell training is a therapy that is recommended by experts for recovering a lost sense of smell. It is a simple process that involves sniffing a set of different odours – usually essential oils, or herbs and spices – every day.
The olfactory system has a unique ability to regenerate sensory neurons (nerve cells). So, just like physiotherapy where exercise helps to restore movement and function following an injury, repeated exposure to odours helps to recover the sense of smell following an infection, or other cause of smell loss (for example, traumatic head injury).
Several studies have demonstrated the effectiveness of smell training under laboratory conditions. But recent findings have suggested that the real-world results might be disappointing.
One reason for this is that smell training is a long-term therapy. It can take months before patients detect anything, and some people may not get any benefit at all.
In one study, researchers found that after three months of smell training, participation dropped to 88%, and further declined to 56% after six months. The reason given was that these people did not feel as though they noticed any improvement in their ability to smell.
Cross-modal associations
To remedy this, researchers are now investigating how smell training can be improved. One interesting idea is that information from our other senses, or “cross-modal associations”, can be applied to smell training to promote odour perception and improve the results.
Cross-modal associations are described as the tendency for sensory cues from different sensory systems to be matched. For example, brightness tends to be associated with loudness. Pitch is related to size. Colours are linked to temperature, and softness is matched with round shapes, while spiky shapes feel more rough. In previous studies, these associations have been shown to have a considerable influence on how sensory information is processed. Especially when it comes to olfaction.
Recent research has shown that the sense of smell is influenced by a combination of different sensory inputs – not just odours. Sensory cues such as colour, shape, and pitch are believed to play a role in the ability to correctly identify and name odours, and can influence perceptions of odour pleasantness and intensity.
In one study, participants were asked to complete a test that measured their ability to discriminate between different odours while they were presented with the colour red or yellow, an outline drawing of a strawberry or a lemon, or a combination of these colours and shapes. The results suggested that corresponding odour and colour associations (for example, the colour red and strawberry) were linked to increased olfactory performance compared with odours and colours that were not associated (for example, the colour yellow and strawberry).
People who associated strawberries with the colour red performed better on smell tests. GCapture/Shutterstock While projects focusing on harnessing these cross-modal associations to improve treatments for smell loss are underway, research has already started to deliver some promising results.
In a recent study that aimed to investigate whether the effects of smell training could be improved with the addition of cross-modal associations, participants watched a guidance video containing sounds that matched the odours that they were training with. The results suggest that cross-modal interactions plus smell training improved olfactory function compared to smell training alone.
The results reported in recent studies have been promising and offer new insights into the field of olfactory science. It is hoped that this will soon lead to the development of more effective treatment options for smell recovery.
In the meantime, smell training is one of the best things you can do for a lost sense of smell, so patients are encouraged to stick with it so that they give themselves the best chance at recovery.
Emily Spencer, PhD Candidate, Olfaction, Edinburgh Napier University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Is thirst a good predictor of dehydration?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Water is essential for daily functioning and health, and we can only survive a few days without it. Yet we constantly lose water through sweat, urination and even evaporation when we breathe.
This is why we have evolved a way to regulate and maintain water in our bodies. Like other animals, our survival relies on a strong biological drive that tells us to find and drink water to balance fluid loss.
This is thirst – a sensation of dryness in the mouth signalling we need to have a drink. This basic physiological mechanism is controlled mainly by part of the brain’s “control centre”, called the hypothalamus. The hypothalamus receives signals from various regions of the body and in return, releases hormones that act as a messenger to signal the thirst sensation.
KieferPix/Shutterstock What is dehydration?
Staying hydrated (having enough water in our bodies) is important for several reasons, including:
- regulating body temperature through sweat and respiration
- lubricating joints and eyes
- preventing infections
- digesting and absorbing nutrients
- flushing out waste (via the kidneys)
- preventing constipation
- brain function (including memory and concentration)
- mood and energy levels
- physical performance and recovery from exercise
- skin health.
Dehydration occurs when our body doesn’t have enough water. Even slight drops in fluid levels have noticeable consequences, such as headaches, feeling dizzy, lethargy and struggling to concentrate.
Chronic dehydration can pose more serious health risks, including urinary tract infections, constipation and kidney stones.
What does the evidence say?
Despite thirst being one of the most basic biological drivers for good hydration, science suggests our feelings of thirst and subsequent fluid intake don’t always correlate with hydration levels.
For example, a recent study explored the impact of thirst on fluid intake and hydration status. Participants attended a lab in the morning and then later in the afternoon to provide markers of hydration status (such as urine, blood samples and body weight). The relationship between levels of thirst in the morning and afternoon hydration status was negligible.
Further, thirst may be driven by environmental factors, such as access to water. For example, one study looked at whether ample access to water in a lab influenced how much people drank and how hydrated they were. The link between how thirsty they felt and how hydrated they were was weak, suggesting the availability of water influenced their fluid intake more than thirst.
Exercise can also change our thirst mechanism, though studies are limited at this stage.
Being thirsty doesn’t necessarily mean we’re dehydrated. puhhha/Shutterstock Interestingly, research shows women experience thirst more strongly than men, regardless of hydration status. To understand gender differences in thirst, researchers infused men and women with fluids and then measured their thirst and how hydrated they were. They found women generally reported thirst at a lower level of fluid loss. Women have also been found to respond more to feeling thirsty by drinking more water.
Other ways to tell if you need to drink some water
While acknowledging some people will need to drink more or less, for many people, eight cups (or two litres) a day is a good amount of water to aim for.
But beyond thirst, there are many other ways to tell whether you might need to drink more water.
1. urine colour: pale yellow urine typically indicates good hydration, while darker, concentrated urine suggests dehydration
2. frequency of going to the toilet: urinating regularly (around four to six times a day) indicates good hydration. Infrequent urination can signal dehydration
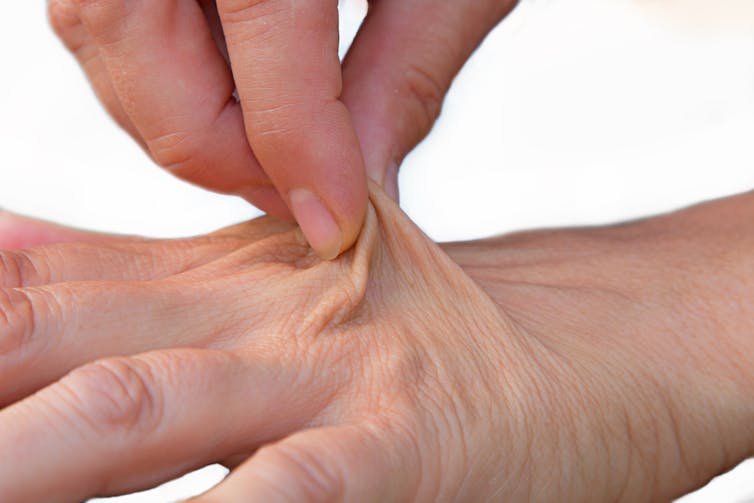
3. skin turgor test: gently pinching the skin (for example, on the back of the hand) and observing how quickly the skin returns to its normal position can help assess hydration. Slow return may indicate dehydration
If skin stays elevated after pinching it may be a sign of dehydration. SusaZoom/Shutterstock 4. mouth and lips: a dry mouth or cracked lips can be early signs of dehydration
5. headaches and fatigue: frequent headaches, dizziness, or unexplained fatigue can be signs of inadequate hydration
6. sweating: in physically active people, monitoring how much they sweat during activity can help estimate fluid loss and hydration needs. Higher levels of sweat may predispose a person to dehydration if they are unable to replace the fluid lost through water intake
These indicators, used together, provide a more comprehensive picture of hydration without solely depending on the sensation of thirst.
Of course, if you do feel thirsty, it’s still a good idea to drink some water.
Lauren Ball, Professor of Community Health and Wellbeing, The University of Queensland and Kiara Too, PhD candidate, School of Human Movement and Nutrition Sciences, The University of Queensland
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Share This Post
-
Are You Taking PIMs?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Getting Off The Overmedication Train
The older we get, the more likely we are to be on more medications. It’s easy to assume that this is because, much like the ailments they treat, we accumulate them over time. And superficially at least, that’s what happens.
And yet, almost half of people over 65 in Canada are taking “potentially inappropriate medications”, or PIMs—in other words, medications that are not needed and perhaps harmful. This categorization includes medications where the iatrogenic harms (side effects, risks) outweigh the benefits, and/or there’s a safer more effective medication available to do the job.
You may be wondering: what does this mean for the US?
Well, we don’t have the figures for the US because we’re working from Canadian research today, but given the differences between the two country’s healthcare systems (mostly socialized in Canada and mostly private in the US), it seems a fair hypothesis that if it’s almost half in Canada, it’s probably more than half in the US. Socialized healthcare systems are generally quite thrifty and seek to spend less on healthcare, while private healthcare systems are generally keen to upsell to new products/services.
The three top categories of PIMs according to the above study:
- Gabapentinoids (anticonvulsants also used to treat neuropathic pain)
- Proton pump inhibitors (PPIs)
- Antipsychotics (especially, to people without psychosis)
…but those are just the top of the list; there are many many more.
The list continues: opioids, anticholinergics, sulfonlyurea, NSAIDs, benzodiazepines and related rugs, and cholinesterase inhibitors. That’s where the Canadian study cuts off (although it also includes “others” just before NSAIDs), but still, you guessed it, there are more (we’re willing to bet statins weigh heavily in the “others” section, for a start).
There are two likely main causes of overmedication:
The side effect train
This is where a patient has a condition and is prescribed drug A, which has some undesired side effects, so the patient is prescribed drug B to treat those. However, that drug also has some unwanted side effects of its own, so the patient is prescribed drug C to treat those. And so on.
For a real-life rundown of how this can play out, check out the case study in:
The Hidden Complexities of Statins and Cardiovascular Disease (CVD)
The convenience factor
No, not convenient for you. Convenient for others. Convenient for the doctor if it gets you out of their office (socialized healthcare) or because it was easy to sell (private healthcare). Convenient for the staff in a hospital or other care facility.
This latter is what happens when, for example, a patient is being too much trouble, so the staff give them promazine “to help them settle down”, notwithstanding that promazine is, besides being a sedative, also an antipsychotic whose common side effects include amenorrhea, arrhythmias, constipation, drowsiness and dizziness, dry mouth, impotence, tiredness, galactorrhoea, gynecomastia, hyperglycemia, insomnia, hypotension, seizures, tremor, vomiting and weight gain.
This kind of thing (and worse) happens more often towards the end of a patient’s life; indeed, sometimes precipitating that end, whether you want it or not:
Mortality, Palliative Care, & Euthanasia
How to avoid it
Good practice is to be “open-mindedly skeptical” about any medication. By this we mean, don’t reject it out of hand, but do ask questions about it.
Ask your prescriber not only what it’s for and what it’ll do, but also what the side effects and risks are, and an important question that many people don’t think to ask, and for which doctors thus don’t often have a well-prepared smooth-selling reply, “what will happen if I don’t take this?”
And look up unbiased neutral information about it, from reliable sources (Drugs.com and The BNF are good reference guides for this—and if it’s important to you, check both, in case of any disagreement, as they function under completely different regulatory bodies, the former being American and the latter being British. So if they both agree, it’s surely accurate, according to best current science).
Also: when you are on a medication, keep a journal of your symptoms, as well as a log of your vitals (heart rate, blood pressure, weight, sleep etc) so you know what the medication seems to be helping or harming, and be sure to have a regular meds review with your doctor to check everything’s still right for you. And don’t be afraid to seek a second opinion if you still have doubts.
Want to know more?
For a more in-depth exploration than we have room for here, check out this book that we reviewed not long back:
To Medicate or Not? That is the Question! – by Dr. Asha Bohannon
Take care!
Share This Post
Related Posts
-
If You’re Poor, Fertility Treatment Can Be Out of Reach
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Mary Delgado’s first pregnancy went according to plan, but when she tried to get pregnant again seven years later, nothing happened. After 10 months, Delgado, now 34, and her partner, Joaquin Rodriguez, went to see an OB-GYN. Tests showed she had endometriosis, which was interfering with conception. Delgado’s only option, the doctor said, was in vitro fertilization.
“When she told me that, she broke me inside,” Delgado said, “because I knew it was so expensive.”
Delgado, who lives in New York City, is enrolled in Medicaid, the federal-state health program for low-income and disabled people. The roughly $20,000 price tag for a round of IVF would be a financial stretch for lots of people, but for someone on Medicaid — for which the maximum annual income for a two-person household in New York is just over $26,000 — the treatment can be unattainable.
Expansions of work-based insurance plans to cover fertility treatments, including free egg freezing and unlimited IVF cycles, are often touted by large companies as a boon for their employees. But people with lower incomes, often minorities, are more likely to be covered by Medicaid or skimpier commercial plans with no such coverage. That raises the question of whether medical assistance to create a family is only for the well-to-do or people with generous benefit packages.
“In American health care, they don’t want the poor people to reproduce,” Delgado said. She was caring full-time for their son, who was born with a rare genetic disorder that required several surgeries before he was 5. Her partner, who works for a company that maintains the city’s yellow cabs, has an individual plan through the state insurance marketplace, but it does not include fertility coverage.
Some medical experts whose patients have faced these issues say they can understand why people in Delgado’s situation think the system is stacked against them.
“It feels a little like that,” said Elizabeth Ginsburg, a professor of obstetrics and gynecology at Harvard Medical School who is president-elect of the American Society for Reproductive Medicine, a research and advocacy group.
Whether or not it’s intended, many say the inequity reflects poorly on the U.S.
“This is really sort of standing out as a sore thumb in a nation that would like to claim that it cares for the less fortunate and it seeks to do anything it can for them,” said Eli Adashi, a professor of medical science at Brown University and former president of the Society for Reproductive Endocrinologists.
Yet efforts to add coverage for fertility care to Medicaid face a lot of pushback, Ginsburg said.
Over the years, Barbara Collura, president and CEO of the advocacy group Resolve: The National Infertility Association, has heard many explanations for why it doesn’t make sense to cover fertility treatment for Medicaid recipients. Legislators have asked, “If they can’t pay for fertility treatment, do they have any idea how much it costs to raise a child?” she said.
“So right there, as a country we’re making judgments about who gets to have children,” Collura said.
The legacy of the eugenics movement of the early 20th century, when states passed laws that permitted poor, nonwhite, and disabled people to be sterilized against their will, lingers as well.
“As a reproductive justice person, I believe it’s a human right to have a child, and it’s a larger ethical issue to provide support,” said Regina Davis Moss, president and CEO of In Our Own Voice: National Black Women’s Reproductive Justice Agenda, an advocacy group.
But such coverage decisions — especially when the health care safety net is involved — sometimes require difficult choices, because resources are limited.
Even if state Medicaid programs wanted to cover fertility treatment, for instance, they would have to weigh the benefit against investing in other types of care, including maternity care, said Kate McEvoy, executive director of the National Association of Medicaid Directors. “There is a recognition about the primacy and urgency of maternity care,” she said.
Medicaid pays for about 40% of births in the United States. And since 2022, 46 states and the District of Columbia have elected to extend Medicaid postpartum coverage to 12 months, up from 60 days.
Fertility problems are relatively common, affecting roughly 10% of women and men of childbearing age, according to the National Institute of Child Health and Human Development.
Traditionally, a couple is considered infertile if they’ve been trying to get pregnant unsuccessfully for 12 months. Last year, the ASRM broadened the definition of infertility to incorporate would-be parents beyond heterosexual couples, including people who can’t get pregnant for medical, sexual, or other reasons, as well as those who need medical interventions such as donor eggs or sperm to get pregnant.
The World Health Organization defined infertility as a disease of the reproductive system characterized by failing to get pregnant after a year of unprotected intercourse. It terms the high cost of fertility treatment a major equity issue and has called for better policies and public financing to improve access.
No matter how the condition is defined, private health plans often decline to cover fertility treatments because they don’t consider them “medically necessary.” Twenty states and Washington, D.C., have laws requiring health plans to provide some fertility coverage, but those laws vary greatly and apply only to companies whose plans are regulated by the state.
In recent years, many companies have begun offering fertility treatment in a bid to recruit and retain top-notch talent. In 2023, 45% of companies with 500 or more workers covered IVF and/or drug therapy, according to the benefits consultant Mercer.
But that doesn’t help people on Medicaid. Only two states’ Medicaid programs provide any fertility treatment: New York covers some oral ovulation-enhancing medications, and Illinois covers costs for fertility preservation, to freeze the eggs or sperm of people who need medical treatment that will likely make them infertile, such as for cancer. Several other states also are considering adding fertility preservation services.
In Delgado’s case, Medicaid covered the tests to diagnose her endometriosis, but nothing more. She was searching the internet for fertility treatment options when she came upon a clinic group called CNY Fertility that seemed significantly less expensive than other clinics, and also offered in-house financing. Based in Syracuse, New York, the company has a handful of clinics in upstate New York cities and four other U.S. locations.
Though Delgado and her partner had to travel more than 300 miles round trip to Albany for the procedures, the savings made it worthwhile. They were able do an entire IVF cycle, including medications, egg retrieval, genetic testing, and transferring the egg to her uterus, for $14,000. To pay for it, they took $7,000 of the cash they’d been saving to buy a home and financed the other half through the fertility clinic.
She got pregnant on the first try, and their daughter, Emiliana, is now almost a year old.
Delgado doesn’t resent people with more resources or better insurance coverage, but she wishes the system were more equitable.
“I have a medical problem,” she said. “It’s not like I did IVF because I wanted to choose the gender.”
One reason CNY is less expensive than other clinics is simply that the privately owned company chooses to charge less, said William Kiltz, its vice president of marketing and business development. Since the company’s beginning in 1997, it has become a large practice with a large volume of IVF cycles, which helps keep prices low.
At this point, more than half its clients come from out of state, and many earn significantly less than a typical patient at another clinic. Twenty percent earn less than $50,000, and “we treat a good number who are on Medicaid,” Kiltz said.
Now that their son, Joaquin, is settled in a good school, Delgado has started working for an agency that provides home health services. After putting in 30 hours a week for 90 days, she’ll be eligible for health insurance.
One of the benefits: fertility coverage.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
Subscribe to KFF Health News’ free Morning Briefing.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
It’s Not Hysteria – by Dr. Karen Tan
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Firstly, who this book is aimed at: in case it wasn’t clear, this book assumes you have, or at least have had, a uterus. If that’s not you, then well, it’ll still be an interesting read but it won’t be about your reproductive health.
Secondly, about that “reproductive health”: it’s mostly not actually about reproductive health literally, but rather, the health of one’s reproductive organs and the things that they affect—which is a lot more than the ability to reproduce!
Dr. Tang takes us on a (respectably in-depth) tour of the relevant anatomy, before moving on to physiology, before continuing to pathology (i.e. things that can go wrong, and often do), and finally various treatment options, including elective procedures, and the pros and cons thereof.
She also talks the reader through talking about things with gynecologists and other healthcare providers, and making sure concerns are not dismissed out-of-hand (something that happens a lot, of course).
The style throughout is quite detailed prose, but without being difficult at all to read, and (assuming one is interested in the topic) it’s very engaging.
Bottom line: if you would like to know more about uteri and everything that is (or commonly/unfortunately) can be attached to them, the effects they have on the rest of the body and health, and what can be done about things not being quite right, then this is a good book for that.
Click here to check out It’s Not Hysteria, and understand more of what’s going on down there!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
What Your Doctor Wants You to Know to Crush Medical Debt – by Dr. Virgie Ellington
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
First things first: this one’s really only of relevance to people living in the US. That’s most of our readership, but if it’s not you, then apologies, this one won’t be of interest.
For the US Americans, though, Dr. Ellington starts strong with “you got a bill—now get the right bill”, and then gives a step-by-step process for finding the mistakes in your medical bills, fixing them, dealing with insurers who do not want to live up to their part of the bargain, and how to minimize what you need to pay, when you actually arrive at your final bill.
The biggest strength of this book is the wealth of insider knowledge (the author has worked as a primary care physician as well as as a health insurance executive), and while this information won’t stay current forever, its relatively recent publication date (2022) means that little has changed since then, and once you’re up to speed with how things are now, it’ll be easy to roll with whatever changes may come in the future.
Bottom line: if you’re living in the US and would like to not be ripped off as badly as possible when it comes to healthcare costs, this book is a very small, very powerful, investment.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: