Unlimited Memory – by Kevin Horsley
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Premise: there are easily learnable techniques to rapidly (and greatly) improve one’s memory. We’ve touched on some of these methods before at 10almonds, but being a newsletter rather than a book, we’ve not been able to go as deeply into it as Horsley!
Your memory is far, far, far more powerful than you might realize, and this book will help unlock that. To illustrate…
Some of the book is given over to what are for most purposes “party tricks”, such as remembering pi to 10,000 places. Those things are fun, even if not as practical in today’s world of rarely needing to even know the actual digits of a phone number. However, they do also serve as a good example of just how much of “super memory” isn’t a matter of hard work, so much as being better organized about it.
Most of the book is focused on practical methods to improve the useful aspects of memory—including common mistakes!
If the book has any flaw it’s that the first chapter or so is spent persuading the reader of things we presumably already believe, given that we bought the book. For example, that remembering things is a learnable skill and that memory is functionally limitless. However, we still advise to not skip those chapters as they do contain some useful reframes as well.
Bottom line: if you read this book you will be astonished by how much you just learned—because you’ll be able to recall whole sections in detail! And then you can go apply that whatever areas of your life you wanted to when you bought the book.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Recommended
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Veg in One Bed New Edition – by Huw Richards
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
We all know that growing our own veg is ultimately not only healthier on the plate, but also a very healthy activity. Cheaper too. So why don’t more of us do it?
For many of us, it’s a matter of not having the skills or knowledge to do so. This book bridges that knowledge-gap.
Richards gives, as promised, a month-by-month well-illustrated guide to growing a wide variety of vegetables. He does, by the way, assume that we are in a temperate climate in the Northern Hemisphere. So if you’re not, you may need to make some adjustments.
The book doesn’t assume prior knowledge, and does give the reader everything we need from an initial basic shopping list onwards.
A particular strength of this book is that it’s about growing veg in a single raised bed—this ensures keeping everything very manageable.
Bottom line: if you have ever thought it would be good to grow your own veg, but didn’t know where to start and want something practical for a beginner, this is an excellent guide that will get you going!
Share This Post
-
Do We Need Sunscreen In Winter, Really?
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
It’s Q&A Day at 10almonds!
Have a question or a request? We love to hear from you!
In cases where we’ve already covered something, we might link to what we wrote before, but will always be happy to revisit any of our topics again in the future too—there’s always more to say!
As ever: if the question/request can be answered briefly, we’ll do it here in our Q&A Thursday edition. If not, we’ll make a main feature of it shortly afterwards!
So, no question/request too big or small 😎
❝I keep seeing advice that we shoudl wear sunscreen out in winter even if it’s not hot or sunny, but is there actually any real benefit to this?❞
Short answer: yes (but it’s indeed not as critical as it is during summer’s hot/sunny days)
Longer answer: first, let’s examine the physics of summer vs winter when it comes to the sun…
In summer (assuming we live far enough from the equator to have this kind of seasonal variation), the part of the planet where we live is tilted more towards the sun. This makes it closer, and more importantly, it’s more directly overhead during the day. The difference in distance through space isn’t as big a deal as the difference in distance through the atmosphere. When the sun is more directly overhead, its rays have a shorter path through our atmosphere, and thus less chance of being blocked by cloud cover / refracted elsewhere / bounced back off into space before it even gets that far.
In winter, the opposite of all that is true.
Morning/evening also somewhat replicate this compared to midday, because the sun being lower in the sky has a similar effect to seasonal variation causing it to be less directly overhead.
For this reason, even though visually the sun may be just as bright on a winter morning as it is on a summer midday, the rays have been filtered very differently by the time they get to us.
This is one reason why you’re much less likely to get sunburned in the winter, compared to the summer (others include the actual temperature difference, your likely better hydration, and your likely more modest attire protecting you).
However…
The reason it is advisable to wear sunscreen in winter is not generally about sunburn, and is rather more about long-term cumulative skin damage (ranging from accelerated aging to cancer) caused by the UV rays—specifically, mostly UVA rays, since UVB rays (with their higher energy but shorter wavelength) have nearly all been blocked by the atmosphere.
Here’s a good explainer of that from the American Cancer Society:
UV (Ultraviolet) Radiation and Cancer Risk
👆 this may seem like a no-brainer, but there’s a lot explained here that demystifies a lot of things, covering ionizing vs non-ionizing radiation, x-rays and gamma-rays, the very different kinds of cancer caused by different things, and what things are dangerous vs which there’s no need to worry about (so far as best current science can say, at least).
Consequently: yes, if you value your skin health and avoidance of cancer, wearing sunscreen when out even in the winter is a good idea. Especially if your phone’s weather app says the UV index is “moderate” or above, but even if it’s “low”, it doesn’t hurt to include it as part of your skincare routine.
But what if sunscreens are dangerous?
Firstly, not all sunscreens are created equal:
Learn more: Who Screens The Sunscreens?
Secondly: consider putting on a protective layer of moisturizer first, and then the sunscreen on top. Bear in mind, this is winter we’re talking about, so you’re probably not going out in a bikini, so this is likely a face-neck-hands job and you’re done.
What about vitamin D?
Humans evolved to have more or less melanin in our skin depending on where we lived, and white people evolved to wring the most vitamin D possible out of the meagre sun far from the equator. Black people’s greater melanin, on the other hand, offers some initial protection against the sun (but any resultant skin cancer is then more dangerous than it would be for white people if it does occur, so please do use sunscreen whatever your skintone).
Nowadays many people live in many places which may or may not be the places we evolved for, and so we have to take that into account when it comes to sun exposure.
Here’s a deeper dive into that, for those who want to learn:
Take care!
Share This Post
-
How stigma perpetuates substance use
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
In 2022, 54.6 million people 12 and older in the United States needed substance use disorder (SUD) treatment. Of those, only 24 percent received treatment, according to the most recent National Survey on Drug Use and Health.
SUD is a treatable, chronic medical condition that causes people to have difficulty controlling their use of legal or illegal substances, such as alcohol, tobacco, prescription opioids, heroin, methamphetamine, or cocaine. Using these substances may impact people’s health and ability to function in their daily life.
While help is available for people with SUD, the stigma they face—negative attitudes, stereotypes, and discrimination—often leads to shame, worsens their condition, and keeps them from seeking help.
Read on to find out more about how stigma perpetuates substance use.
Stigma can keep people from seeking treatment
Suzan M. Walters, assistant professor at New York University’s Grossman School of Medicine, has seen this firsthand in her research on stigma and health disparities.
She explains that people with SUD may be treated differently at a hospital or another health care setting because of their drug use, appearance (including track marks on their arms), or housing situation, which may discourage them from seeking care.
“And this is not just one case; this is a trend that I’m seeing with people who use drugs,” Walters tells PGN. “Someone said, ‘If I overdose, I’m not even going to the [emergency room] to get help because of this, because of the way I’m treated. Because I know I’m going to be treated differently.’”
People experience stigma not only because of their addiction, but also because of other aspects of their identities, Walters says, including “immigration or race and ethnicity. Hispanic folks, brown folks, Black folks [are] being treated differently and experiencing different outcomes.”
And despite the effective harm reduction tools and treatment options available for SUD, research has shown that stigma creates barriers to access.
Syringe services programs, for example, provide infectious disease testing, Narcan, and fentanyl test strips. These programs have been proven to save lives and reduce the spread of HIV and hepatitis C. SSPs don’t increase crime, but they’re often mistakenly “viewed by communities as potential settings of drug-related crime;” this myth persists despite decades of research proving that SSPs make communities safer.
To improve this bias, Walters says it’s helpful for people to take a step back and recognize how we use substances, like alcohol, in our own lives, while also humanizing those with addiction. She says, “There’s a lack of understanding that these are human beings and people … [who] are living lives, and many times very functional lives.”
Misconceptions lead to stigma
SUD results from changes in the brain that make it difficult for a person to stop using a substance. But research has shown that a big misconception that leads to stigma is that addiction is a choice and reflects a person’s willpower.
Michelle Maloney, executive clinical director of mental health and addiction recovery services for Rogers Behavioral Health, tells PGN that statements such as “you should be able to stop” can keep a patient from seeking treatment. This belief goes back to the 1980s and the War on Drugs, she adds.
“We think about public service announcements that occurred during that time: ‘Just say no to drugs,’” Maloney says. “People who have struggled, whether that be with nicotine, alcohol, or opioids, [know] it’s not as easy as just saying no.”
Stigma can worsen addiction
Stigma can also lead people with SUD to feel guilt and shame and blame themselves for their medical condition. These feelings, according to the National Institute on Drug Abuse, may “reinforce drug-seeking behavior.”
In a 2020 article, Dr. Nora D. Volkow, the director of NIDA, said that “when internalized, stigma and the painful isolation it produces encourage further drug taking, directly exacerbating the disease.”
Overall, research agrees that stigma harms people experiencing addiction and can make the condition worse. Experts also agree that debunking myths about the condition and using non-stigmatizing language (like saying someone is a person with a substance use disorder, not an addict) can go a long way toward reducing stigma.
Resources to mitigate stigma:
- CDC: Stigma Reduction
- National Harm Reduction Coalition: Respect To Connect: Undoing Stigma
- NIDA:
- Shatterproof: Addiction language guide (Disclosure: The Public Good Projects, PGN’s parent company, is a Shatterproof partner)
This article first appeared on Public Good News and is republished here under a Creative Commons license.
Share This Post
Related Posts
-
Debate over tongue tie procedures in babies continues. Here’s why it can be beneficial for some infants
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
There is increasing media interest about surgical procedures on new babies for tongue tie. Some hail it as a miracle cure, others view it as barbaric treatment, though adverse outcomes are rare.
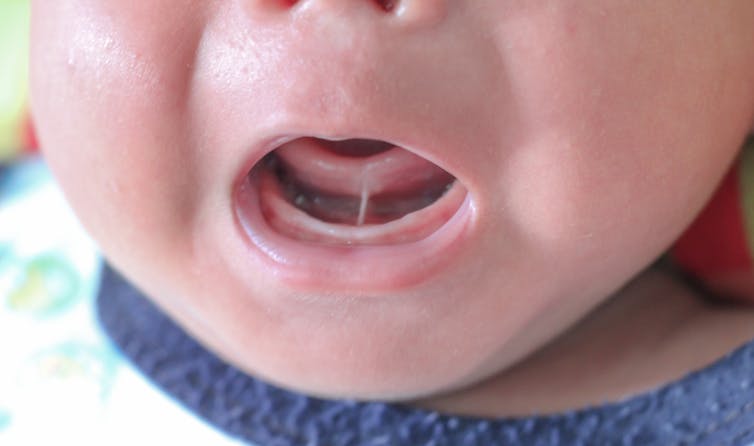
Tongue tie occurs when the tissue under the tongue is attached to the lower gum or floor of the mouth in a way that can restrict the movement or range of the tongue. This can impact early breastfeeding in babies. It affects an estimated 8% of children under one year of age.
While there has been an increase in tongue tie releases (also called division or frenotomy), it’s important to keep this in perspective relative to the increase in breastfeeding rates.
The World Health Organization recommends exclusive breastfeeding for the first six months of life, with breastfeeding recommended into the second year of life and beyond for the health of mother and baby as well as optimal growth. Global rates of breastfeeding infants for the first six months have increased from 38% to 48% over the past decade. So, it is not surprising there is also an increase in the number of babies being referred globally with breastfeeding challenges and potential tongue tie.
An Australian study published in 2023 showed that despite a 25% increase in referrals for tongue tie division between 2014 and 2018, there was no increase in the number of tongue tie divisions performed. Tongue tie surgery rates increased in Australia in the decade from 2006 to 2016 (from 1.22 per 1,000 population to 6.35) for 0 to 4 year olds. There is no data on surgery rates in Australia over the last eight years.
Tongue tie division isn’t always appropriate but it can make a big difference to the babies who need it. More referrals doesn’t necessarily mean more procedures are performed.
chomplearn/Shutterstock How tongue tie can affect babies
When tongue tie (ankyloglossia) restricts the movement of the tongue, it can make it more difficult for a baby to latch onto the mother’s breast and painlessly breastfeed.
Earlier this month, the International Consortium of oral Ankylofrenula Professionals released a tongue tie position statement and practice guideline. Written by a range of health professionals, the guidelines define tongue tie as a functional diagnosis that can impact breastfeeding, eating, drinking and speech. The guidelines provide health professionals and families with information on the assessment and management of tongue tie.
Tongue tie release has been shown to improve latch during breastfeeding, reduce nipple pain and improve breast and bottle feeding. Early assessment and treatment are important to help mothers breastfeed for longer and address any potential functional problems.
The frenulum is a band of tissue under the tongue that is attached to the gumline base of the mouth. Akkalak Aiempradit/Shutterstock Where to get advice
If feeding isn’t going well, it may cause pain for the mother or there may be signs the baby isn’t attaching properly to the breast or not getting enough milk. Parents can seek skilled help and assessment from a certified lactation consultant or International Board-Certified Lactation Consultant who can be found via online registry.
Alternatively, a health professional with training and skills in tongue tie assessment and division can assist families. This may include a doctor, midwife, speech pathologist or dentist with extended skills, training and experience in treating babies with tongue tie.
When access to advice or treatment is delayed, it can lead to unnecessary supplementation with bottle feeds, early weaning from breastfeeding and increased parental anxiety.
Getting a tongue tie assessment
During assessment, a qualified health professional will collect a thorough case history, including pregnancy and birth details, do a structural and functional assessment, and conduct a comprehensive breastfeeding or feeding assessment.
They will view and thoroughly examine the mouth, including the tongue’s movement and lift. The appearance of where the tissue attaches to the underside of the tongue, the ability of the tongue to move and how the baby can suck also needs to be properly assessed.
Treatment decisions should focus on the concerns of the mother and baby and the impact of current feeding issues. Tongue tie division as a baby is not recommended for the sole purpose of avoiding speech problems in later life if there are no feeding concerns for the baby.
A properly qualified lactation consultant can help with positioning and attachment. HarryKiiM Stock/Shutterstock Treatment options
The Australian Dental Association’s 2020 guidelines provide a management pathway for babies diagnosed with tongue tie.
Once feeding issues are identified and if a tongue tie is diagnosed, non-surgical management to optimise positioning, latch and education for parents should be the first-line approach.
If feeding issues persist during follow-up assessment after non-surgical management, a tongue tie division may be considered. Tongue tie release may be one option to address functional challenges associated with breastfeeding problems in babies.
There are risks associated with any procedure, including tongue tie release, such as bleeding. These risks should be discussed with the treating practitioner before conducting any laser, scissor or scalpel tongue tie procedure.
Post-release support by a certified lactation consultant or feeding specialist is necessary after a tongue tie division. A post-release treatment plan should be developed by a team of health professionals including advice and support for breastfeeding to address both the mother and baby’s individual needs.
We would like to acknowledge the contribution of Raymond J. Tseng, DDS, PhD, (Paediatric Dentist) to the writing of this article.
Sharon Smart, Lecturer and Researcher (Speech Pathology) – School of Allied Health, Curtin University; David Todd, Associate Professor, Neonatology, ANU Medical School, Australian National University, and Monica J. Hogan, PhD student, ANU School of Medicine and Psychology, Australian National University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
Palliative care as a true art form
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
How do you ease the pain from an ailment amidst lost words? How can you serve the afflicted when lines start to blur? When the foundation of communication begins to crumble, what will be the pillar health-care professionals can lean on to support patients afflicted with dementia during their final days?
The practice of medicine is both highly analytical and evidence based in nature. However, it is considered a “practice” because at the highest level, it resembles a musician navigating an instrument. It resembles art. Between lab values, imaging techniques and treatment options, the nuances for individualized patient care so often become threatened.
Dementia, a non-malignant terminal illness, involves the progressive cognitive and social decline in those afflicted. Though there is no cure, dementia is commonly met in the setting of end-of-life care. During this final stage of life, the importance of comfort via symptomatic management and communication usually is a priority in patient care. But what about the care of a patient suffering from dementia? While communication serves as the vehicle to deliver care at a high level, medical professionals are suddenly met with a roadblock. And there … behind the pieces of shattered communication and a dampened map of ethical guidelines, health-care providers are at a standstill.
It’s 4:37 a.m. You receive a text message from the overnight nurse at a care facility regarding a current seizure. After lorazepam is ordered and administered, Mr. H, a quick-witted 76-year-old, stabilizes. Phenobarbital 15mg SC qhs was also added to prevent future similar events. You exhale a sigh of relief.
Mr. H. has been admitted to the floor 36 hours earlier after having a seizure while playing poker with colleagues. Since he became your patient, he’s shared many stories from professional and family life with you, along with as many jokes as he could fit in between. However, over the course of the next seven days, Mr. H. would develop aspiration pneumonia, progressing to ventilator dependency and, ultimately, multi-organ failure with rapid cognitive decline.
What strategies and tools would you use to maximize the well-being of your patient during his decline? How would you bridge the gap of understanding between the patient’s family and health-care team to provide the standard of care that all patients are owed?
To give Mr. H. the type of care he would have wanted, upon his hospital admission, he should have been questioned about his understanding of illness along with the goals of care of the medical team. The patient should have been informed that it is imperative to adhere to the medical regimen implemented by his team along with the risks of not doing so. In the event disease-related complications arose, advanced directives should have been documented to avoid any unnecessary measures.
It is important to note, that with each change in status of the patient’s health status, the goal of treatment must be reassessed. The patient or surrogate decision-maker’s understanding of these goals is paramount in maintaining the patient’s autonomy. It is often said that effective communication is the bedrock of a healthy relationship. This is true regardless of type of relationship.
This is why I and Megan Vierhout wrote Integrated End of Life Care in Dementia: A Comprehensive Guide, a book targeted at providing a much-needed road map to navigate the many challenges involved in end-of-life care for individuals with dementia. Ultimately, our aim is to provide a compass for both health-care professionals and the families of those affected by the progressive effects of dementia. We provide practical advice on optimizing communication with individuals with dementia while taking their cognitive limitations, preferences and needs into account.
I invite you to explore the unpredictable terrain of end-of-life care for patients with dementia. Together, we can pave a smoother, sturdier path toward the practice of medicine as a true art form.
This article is republished from healthydebate under a Creative Commons license. Read the original article.
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails:
-
More Mediterranean – by American’s Test Kitchen
10almonds is reader-supported. We may, at no cost to you, receive a portion of sales if you purchase a product through a link in this article.
Regular 10almonds readers will know that we talk about the Mediterranean diet often, and with good reason; it’s been for quite a while now the “Gold Standard” when it comes to scientific consensus on what constitutes a good diet for healthy longevity.
However, it’s easy to get stuck in a rut of cooking the same three meals and thinking “I must do something different, but not today, because I have these ingredients and don’t know what to cook” and then when one is grocery-shopping, it’s “I should have researched a new thing to cook, but since I haven’t, I’ll just get the ingredients for what I usually cook, since we need to eat”, and so the cycle continues.
This book will help break you out of that cycle! With (as the subtitle promises) hundreds of recipes, there’s no shortage of good ideas. The recipes are “plant-forward” rather than plant-based per se (i.e. there are some animal products in them), though for the vegetarians and vegans, it’s nothing that’s any challenge to substitute.
Bottom line: if you’re looking for “delicious and nutritious”, this book is sure to put a rainbow on your plate and a smile on your face.
Click here to check out More Mediterranean, and inspire your kitchen!
Don’t Forget…
Did you arrive here from our newsletter? Don’t forget to return to the email to continue learning!
Learn to Age Gracefully
Join the 98k+ American women taking control of their health & aging with our 100% free (and fun!) daily emails: